Common Knees Injuries We Treat
- Anterior Cruciate Ligament Injury
- ACL Post-Op BTB
- ACL Post-op Hamstring
- ACL pre-op protocol
- High Tibial Osteotomy Surgery
- Iliotibial Band Tendinitis
- Arthroscopic Knee Surgery
- Sports Conditioning for the Knee
- The Medial Collateral Ligament (MCL) of the Knee
- Knee Meniscus Repair
- Meniscal Allograft Transplant
- Arthroscopic Microfracture Surgery
- Oats Protocol
- Osteochrondritis dissecans
- Osteochrondritis dissecans
- Patellar and Quadriceps Tendon
- Patellofemoral Instability
- Patellofemoral Syndrome
- The Posterior Cruciate Ligament
- Total Knee Arthroplasty Protocol
- Uni-Compartment Knee Replacement

Anterior Cruciate Ligament Injury
What is the Anterior Cruciate Ligament?
The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band of fibrous tissue, similar to a rope, which connects the bones together at a joint. There are two ligaments on the sides of the knee (collateral ligaments) that give stability to sideways motions: the medial collateral ligament (MCL) on the inner side and the lateral collateral ligament (LCL) on the outer side of the knee. Two ligaments cross each other (therefore, called "cruciate") in the center of the knee joint: The crossed ligament toward the front (anterior) is the ACL and the one toward the back of the knee (posterior) is the posterior cruciate ligament (PCL). The ACL prevents the lower bone (tibia) from sliding forward too much and stabilizes the knee to allow cutting, twisting and jumping sports. The PCL stops the tibia from moving backwards.
How Can the ACL Tear?
The most common mechanism that tears the ACL is the combination of a sudden stopping motion on the leg while quickly twisting on the knee. This can happen in a sport such as basketball, for example, when a player lands on the leg when coming down from a rebound or is running down the court and makes an abrupt stop to pivot. In football, soccer, or lacrosse, the cleats on the shoes do not allow the foot to slip when excess force is applied. In skiing, the ACL is commonly injured when the skier sits back while falling. The modern ski boot is stiff, high, and is tilted forward. The boot thus holds the tibia forward and the weight of the body quickly shifts backwards. Thus, too much force is suddenly applied to the knee. The excess force causes the ACL to "pop".
A contact injury, such as when the player is clipped in football, forces the knee into an abnormal position. This may tear the ACL, MCL and other structures.
What Are the Signs That an ACL is Torn?
When the ACL tears, the person feels the knee go out of joint and often hears or feels a "pop". If he or she tries to stand on the leg, the knee may feel unstable and give out. The knee usually swells a great deal immediately (within two hours). Over the next several hours, pain often increases and it becomes difficult to walk.
What Other Knee Structures Can Be Injured When the ACL Tears?
The meniscus is a crescent shaped cartilage that acts as a shock absorber between the femur and tibia. Each knee has two menisci: medial (inner) and lateral (outer). The menisci are attached to the tibia. When the tibia suddenly moves forward and the ACL tears, the meniscus can become compressed between the femur and tibia tearing the meniscus. The abnormal motion of the joint can also bruise the bones.
There is a second type of cartilage in the knee joint called articular cartilage. This is a smooth, white glistening surface that covers the ends of the bones. The articular cartilage provides lubrication and as a result, there is very little friction when the joint moves. This joint cartilage can get damaged when the ACL tears and the joint is compressed in an abnormal way.
If this articular cartilage is injured, the joint no longer moves smoothly. Stiffness, pain, swelling and grinding can occur. Eventually, arthritis can develop. The MCL and other ligaments in the joint can also be disrupted when the ACL tears. This is more common if an external blow to the knee caused the injury (such as if the knee was clipped while playing football) or when skiing.
What is the Initial Treatment for a Knee That May Have a Torn ACL?
The initial treatment of the injured joint is to apply ice and gentle compression to control swelling. A knee splint and crutches are typically used. The knee should be evaluated by a doctor to see which ligaments are torn and to be sure other structures such as tendons, arteries, nerves, etc. have not been injured. X-rays are taken to rule out a fracture. Sometimes an MRI is needed, but usually the diagnosis can be made by physical examination.
How Will the Knee Function if the ACL is Torn?
If no structure other than the ACL is injured, the knee usually regains its range of motion and is painless after six or eight weeks. The knee may feel "normal". However, it can be a "trick knee". If a knee has a torn ACL, the knee can give way or be unstable when the person pivots or changes direction. The athlete can usually run straight ahead without a problem but when he or she makes a quick turning motion, the knee tends to give way and collapse. This abnormal motion can damage the menisci or articular cartilage and cause further knee problems.
If a person does not do sports and is relatively inactive, the knee can feel quite normal even if the ACL is torn. Thus, in some older or less active patients, the ACL may not need to be reconstructed. In young, athletic patients, however, the knee will tend to reinjure frequently and give way during activities in which the person quickly changes direction. Therefore, it is usually recommended to reconstruct the torn ACL.
When Should Surgery Be Performed for a Torn ACL?
It is best to wait for the pain and swelling to subside and to allow associated injuries to heal before performing surgery for the ACL. If surgery is done soon after injury, rehabilitation may be difficult, the knee may get stiff, and there could be permanent loss of motion. The athlete will usually get back to sports much more quickly if the knee is allowed to recover from initial injury and to regain its full painless range of motion (usually about six weeks) before performing surgery. At Boston Sports Medicine and Research Institute, we typically prefer that our patients have restored about 130-135 degrees of motion with minimal swelling and good quadriceps control prior to proceeding with surgical reconstruction. The final decision for timing of surgery is made on an individual basis, but these are general guidelines. By delaying surgery to attain these pre-operative goals, then an accelerated rehabilitation program can be used after surgery. With accelerated rehabilitation, continuous passive range of motion (CPM) is used for the first two weeks following surgery. The knee heals much more quickly and better joint function results.
The best treatment following acute ACL injury is to usually protect the joint and apply ice and use crutches for several weeks. As the swelling and pain subside, and the patient can put weight on the leg; then the immobilizer and crutches are discontinued. The emphasis is on regaining knee motion. Resistive exercises to build up strength should not be done during this time to prevent damaging the knee cap and causing chondromalacia patella.
If the knee also has an injured medial collateral ligament (MCL), it is best to allow the MCL to heal completely (usually six to eight weeks) before reconstructing the ACL. Then an arthroscopic procedure can be performed to reconstruct the ACL. The torn MCL typically does not need to be repaired surgically unless incomplete healing occurs. There may be instances when immediate surgery is indicated following injury. Examples include some knee dislocation when multiple ligaments are torn. Tears of the outer knee ligaments (lateral collateral ligament) often do require timely surgical repair. Individual decisions need to be made on whether or not to reconstruct the ACL soon after injury in these instances where immediate surgery may be required.
Do All ACL Tears Need Surgery?
No — some knees function reasonably well despite having a torn ACL. Good knee function is more common in patients who are over forty years old and who are relatively inactive in sports. Patients who are less than thirty years old, regardless of activity level, tend to have problems with instability and frequent episodes of giving way. Therefore, surgical reconstruction of a torn ACL is often recommended in these patients.
Treatment Options for a Torn ACL
I. Non-Operative
Some patients can function reasonably well even if the ACL is torn. However, it may be necessary to modify activities and avoid high risk sports (such as basketball, soccer and football). The key to prevent the knee that has a torn ACL from giving out is to avoid quick pivoting motions. Wearing a knee brace can help to prevent re-injury. The main effect of a knee brace is to be a constant reminder to be careful. However, a brace will not completely stabilize a knee that has a torn ACL. Exercises that restore the muscle strength, power, coordination, and endurance will also improve knee function and help to stabilize the knee. However, a fully rehabilitated knee that has a torn ACL can still give way if a quick change in direction occurs.
II. Limited Arthroscopic Surgery
Many knees in which the ACL is torn have additional injuries such as torn menisci or fragments of articular cartilage that are knocked loose (creating a loose body and a defect in the articular cartilage). These associated injuries can cause symptoms of pain, swelling, and locking (in addition to symptoms of giving way due to a torn ACL). Arthroscopic surgery to remove torn menisci or to remove loose bodies can improve pain and eliminate locking. However, it would usually not eliminate symptoms of instability, i.e. giving way.
III. ACL Reconstruction
Surgical reconstruction of a torn ACL involves replacing the torn ACL with tissue (called a "graft", usually a ligament or tendon) from another part of the knee and putting it into a position to take the place of the torn ACL.
The most commonly used graft is taken from the middle third of the patellar tendon (the tendon connecting the knee cap to the tibial bone). Hamstring tendon grafts taken from the inner thigh on the back of the knee are also used. Occasionally, tendon grafts are taken from donor cadavers (referred to as "allograft"). For most of these procedures, the operation is done arthroscopically instead of making big incisions. The knee is examined arthroscopically and associated injuries such as torn menisci, loose bodies, etc are treated. If the middle third of the patellar tendon is used, a small incision is made on the inner side of the leg just below the knee to take the graft (this results in numbness on the front of the knee). While viewing the inside of the joint through the arthroscope, guides are used to create bone tunnels in the exact positions to allow proper reconstruction of the ACL. The graft is then pulled into the bony tunnels. Absorbable screws are placed in the tunnels to wedge the bone graft against the wall of the tunnel to give immediate stability and allow healing of the bone graft. Thus, the bone plug on one end of the graft is secured to the tunnel in the femur and the bone plug on the other end of the graft is secured to the tunnel in the tibia. The piece of patellar tendon graft between the two bone plugs becomes the new ACL.
Postoperatively, an accelerated rehabilitation program allows the optimal return of function. Two weeks after surgery, the sutures are removed and the patient can walk bearing full weight on the leg. A knee brace and crutches are used for the first week or two until the leg regains enough strength to allow unaided walking without a limp.
When Can I Expect to Return to Sports Following Surgery?
Within two weeks after surgery, the patient is usually walking on level surfaces without difficulty. At about five or six weeks, he or she can usually go up and down stairs without support. For the next several months, exercises are done to regain motion and strength in the knee. When the knee has full range of motion (usually at six to eight weeks), muscle-strengthening exercises are done. At four months, the patient is usually running and at six to eight months, participating in sports.
When Can I Expect to Return to Activities After Surgery?
Most people can get back to desk work or sedentary activity one or two weeks after surgery. If the right knee has been reconstructed, it may be several weeks before the knee is strong enough to drive safely. For heavy work, it may take 3 to six months before the leg is strong enough to allow working.
| Work Return | |
|---|---|
| Sedentary/desk | 1-2 weeks |
| General office | 2-3 weeks |
| Light | 6-8 weeks |
| Medium | 3 months |
| Heavy | 4-6 months |
| Sport Return | |
|---|---|
| Normal walking/stairs | 1 month |
| Light individual sports | 3-4 months |
| Running | 4 months |
| Jumping | 6 months |
| Contact/high performance | 9-12 months |
What Are the Risks and Benefits of ACL Treatment?
Non-Operative
Risks
- Repetitive injuries may cause further permanent damage and eventually lead to arthritis.
- Inability to participate in sports or daily activities that require pivoting.
Benefits
- Small percentage of people manage well without surgery.
Operative Risks
Benefits
- Return to work and sports with a stable knee
- Hopefully prevent further injury to the knee
| Complications | % |
|---|---|
| Permanent numbness in front of knee near incision | 100 |
| Other nerve injury | 0.5 |
| Patello-femoral pain (kneecap) | 5 |
| Flexion contracture | 10 |
| Reinjury | 5-10 |
| Swelling | 1 |
| Superficial infection | 1 |
| Deep infection | 0.5 |
| DVT (blood clots) | 0.5 |
| Delay in regaining motion | 5-10 |
| Vascular (damage to blood vessels) | 0.01 |
| Death | <0.01 |
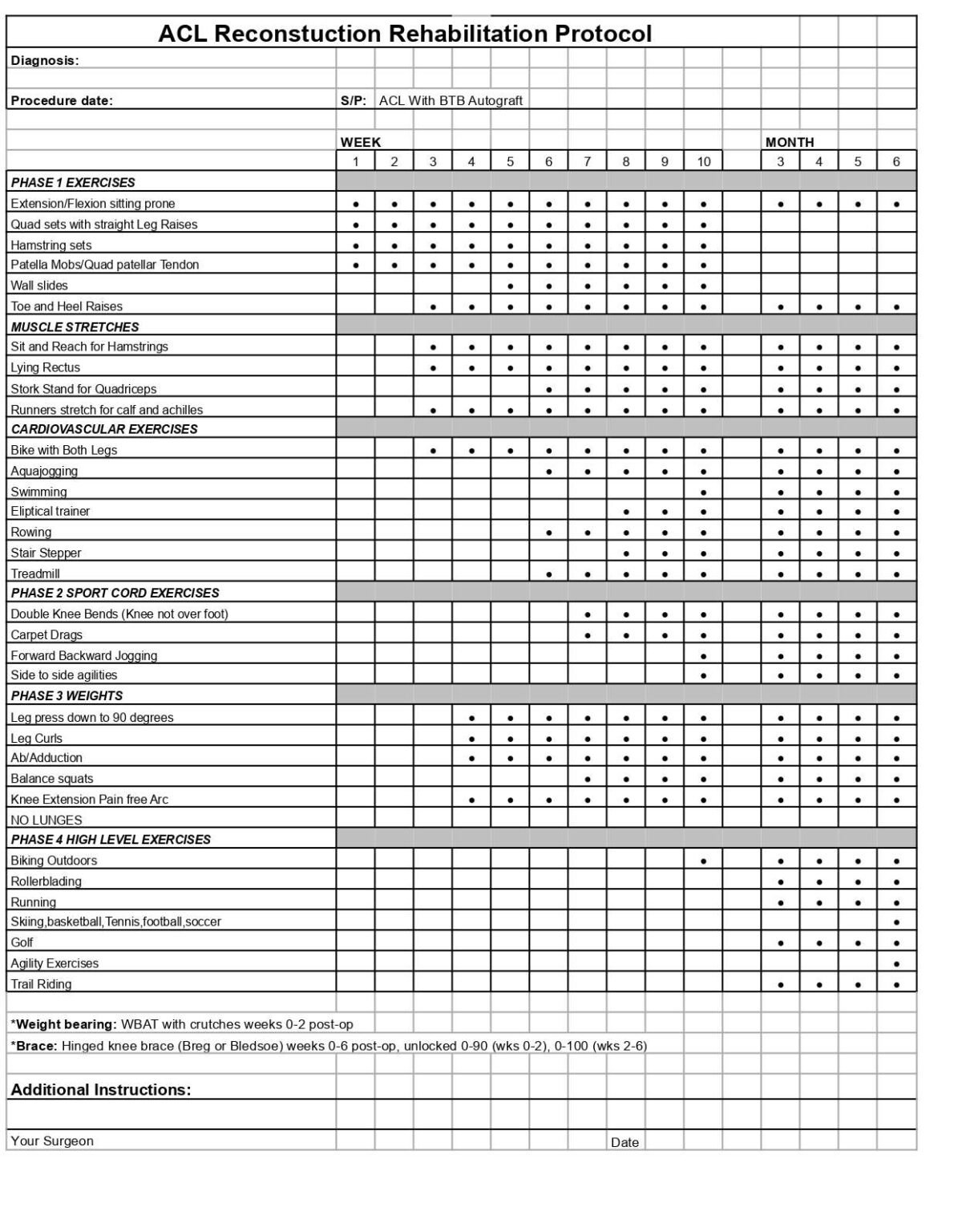
ACL Post-Op BTB
Anterior Cruciate Ligament Reconstruction Surgery
Here are guidelines that will help you to prepare for ACL reconstruction surgery:
PREOPERATIVE INSTRUCTIONS
BEFORE SURGERY:
Your Surgeon will see you in the office. He will do a preoperative history and physical examination and complete the necessary paperwork. He will write preoperative hospital orders and schedule an appointment with the pre-operative test center if needed. You will have an opportunity to speak with anesthesia and physical therapy. It is recommended that you utilize a stationary cycle to maintain your knee range of motion and improve the overall function of the knee prior to surgery. Continue to perform the ACL-preoperative exercises.
SEVERAL DAYS PRIOR TO SURGERY:
Wash the knee with soap or Hibiclens several times per day to get the skin as clean as you can. This decreases the risk of infection. Be careful not to get any scratches, cuts, sunburn, poison ivy, etc. The skin has to be in very good shape to prevent problems. You do not need to shave.
THE DAY BEFORE SURGERY:
You can have nothing to eat or drink after midnight on the day before surgery. It is very important to have a completely empty stomach prior to surgery for anesthesia safety reasons. This included no chewing gum or drinking coffee. If you have to take medication, you can do so with a sip of water early in the morning prior to surgery (but later tell the anesthesiologist you have done so).
DAY OF SURGERY:
Please bring any crutches, brace, ice machine or imaging studies that you have received.
SURGERY:
The operation to replace the torn anterior cruciate ligament will be done arthroscopically. A small incision will be made on the inner side of the knee to take the graft from the middle of the patellar tendon together with a small piece of bone from the bottom of the kneecap and the upper part of the tibia (mid-third patellar tendon graft, "bone-tendon-bone"). The incision leaves a small area of numbness on the outer side of the upper leg. Most of this numbness clears but it takes a year or two and is not usually bothersome. In certain circumstances, the graft is a hamstring tendon or a donor graft from a cadaver (allograft).
AFTER SURGERY:
- The most important aspect is to get the knee out completely straight.
You will be given a prescription for pain medication to take home with you. In addition to this medication, you should take one aspirin per day to help prevent blood clots (phlebitis) for 14 days. The pain medication has a tendency to make you constipated and over the counter medication for constipation should be taken on an as needed basis.
The dressing can be removed at two days. The wound is sealed with steri-strips (small pieces of tape on the skin). You can shower on the second day following surgery, but be careful standing in the shower so that you do not fall. It is better to have a small stool to be able to sit on. However, you can get the leg wet and wash it, but do not scrub the wound or pick off steri-strips as they will fall off on their own. Do not submerge the knee under water in a bath, hot tub or swimming pool.
To help control swelling in the lower leg, you should elevate the extremity, if excessive wear compression stockings after surgery until your first post-operative visit. If you develop calf pain or excessive swelling in the leg, call Greater Michigan Orthopedics.
A cryocuff is a blue wrap that is put on the knee to keep it cold. You can use this as often as you want to cool down the knee to reduce swelling and pain. Check your skin every time that you remove the wrap to make sure that it is intact. Be sure to stock up on extra ice in your freezer. These can be bought through the office. Ice bags work just as well.
ACL Reconstruction Rehabilitation Guidelines
PHASE 1: 0-2 weeks after surgery
This handout is to use as a guideline for your rehabilitation after anterior cruciate reconstruction. You may vary in your ability to do these exercises and to progress from one phase to the other. Please call your Surgeon's office if you are having a problem with your knee or if you need clarification of these instructions.
GOALS
- Protect the reconstruction – avoid falling
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
Do not place a pillow under the knee for comfort. This can lead to knee stiffness.
BRACE/CRUTCHES
Your knee brace is set to allow your knee to bend and straighten from 0 to 90 degrees. Use it when walking. In some cases, you may be sent home with the brace locked at 0 degrees (fully straight). After you arrive home, and the anesthetic nerve block has worn off, unlock the brace to allow 0 to 90 degrees of motion.
Weight bear as tolerated with crutches beginning the day of the surgery. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you. In some cases, crutches and restricted weight bearing may be necessary for longer periods, such as, if a meniscal repair was performed. Then you must remain partial weight bearing for 4 weeks. Your Surgeon or the physical therapist will give special instructions in these cases. Wean the crutches and advance to full motion at 4-6 weeks in these cases.
Criteria to discontinue crutches is when you attain a normal gait pattern.
CRYOCUFF (COLD APPLICATION)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15-20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
WOUND CARE
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
FREE/MACHINE WEIGHTS (Upper Body/Trunk Only)
We suggest that you do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15-20 repetitions. Do not place yourself in a compromising position with your recently operated knee.
EXERCISE PROGRAM
Days per week: 7 Times per day: 3-4
Cardiopulmonary
UBE or similar exercise is recommended
Criteria for phase 2
- No lag SLR
- Normal gait
- Crutch D/c
- ROM: no greater than 5 degree active extension lag, 110 active flexion
| Quadriceps sets | 1-2 sets of 15-20 reps |
| Hamstring sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Heel slides with towel assist | 1 set of 5-15 minutes |
| Sitting heel slides | 1-2 sets of 15-20 reps |
| Straight leg raises (emphasize no lag) (may e-stim) | 1-2 sets of 15-20 reps |
| Patellar Mobilization (IMPORTANT) | 1 set for 1-3 minutes |
| Hip abduction | 3 sets of 10 |
| Ankle pumps | 1 set of 2-3 minutes |
| Prone hang | 5 minutes |
PHASE 2: 2 – 6 weeks after surgery
Goals
- Protect the reconstruction, avoid falling
- Ensure wound healing
- Full ROM
- Begin quadriceps muscle strengthening
- Decrease knee and leg swelling
CRYOCUFF
Use the cryocuff or ice bags to decrease swelling for 20 minutes three times a day after each exercise session.
BRACE/CRUTCHES
In cases where the patellar tendon autograft is used, you can begin placing all of your weight on the operated leg when you walk unless otherwise instructed by your Surgeon. Discontinue using your crutches when you are comfortable doing so. Continue using your brace when walking outside of the home. Within one or two weeks, you can usually discontinue use of the crutches if you have good control of the leg and are sure that you will not fall or get injured. Concentrate walking normally, in a heel-strike to toe-off pattern, without a limp. Occasionally (every one or two hours) practice standing on your operated leg, with your knee fully straight, for 10 to 20 seconds.
In cases where a meniscus repair is done along with the ACL reconstruction, the brace should be locked fully straight when walking for the first 6 weeks after surgery.
EXERCISE PROGRAM – Stationary Bicycle
Days per week: 5-7 Times per day: 1-2
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for up to 10-15 minutes, 1 to 2 times a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
Water Workout (optional)
Days per week: 3 Times per day: 1
Aqua-jogger exercise or Flutter kick swimming 20-30 minutes
RANGE OF MOTION AND STRENGTHENING EXERCISES (brace off)
Days per week: 5-7 Times per day: 1-2
ROM:
- Low load, long duration (assisted PRN)
- Heel slides/wall slides
- Heel prop/prone hang (minimize co-contraction/nociceptor response)
- Bike (rocking-for-range → Ride with low seat height)
- Flexibility stretching all major groups
Strengthening:
- Quads: Quad sets, Mini Squats/Wall Squats, Steps-ups, Knee extension from 90-40, Leg press
- Hamstrings: Hamstring curls closed chain, resistive SLR with sports cord
Other musculature:
- Hip adduction/abduction: SLR or with equipment
- Standing Heel raises: progress from double to single leg support
- Seated calf press against resistance
- Multi-hip machine in all directions with proximal pad placement
Neuromuscular:
- Wobble board, Rocker board, Single-leg stance with or without equipment
Cardiopulmonary:
Bike, Elliptical
If you did not have a meniscus repair, you can start the Leg Press during this phase under supervision of a physical therapist if you have achieved: 1. Full passive knee extension. 2. Full extension while quadriceps setting. 3. Flexion of 125 degrees. 4. Minimal swelling.
Criteria for progression to phase 3
- Full ROM
- Minimal effusion
- Functional strength and control in daily activities
- IKDC Question #10 (global rating of function) score 7 or higher
PHASE 3: 7-12 weeks after surgery
GOALS
- Protect the reconstruction; avoid falling
- Maintain full ROM
- Walk with a normal heel-toe gait with no limp
- Muscle strength and conditioning improvements
BRACE
The brace is discontinued after you see your surgeon at your 6-week post-operative office visit. Concentrate on walking with a heel-toe gait without a limp. In some cases, use of the brace will continue if the knee requires a longer period of protection.
CRYOCUFF/ICE
Continue to use the cryocuff for 20 minutes after each workout.
EXERCISE PROGRAM
Strengthening:
- Squats, Leg press, Hamstring curl, Knee extension 90 to 0, Step-ups/down, Shuttle, Sports cord, Wall squats
Neuromuscular training:
- Wobble board/ rocker board / roller board, Perturbation training, instrumented testing systems, varied surfaces
Cardiopulmonary:
Continue Bike and Elliptical
Precautions When Exercising
- Avoid pain at the patellar tendon site
- Avoid pain and/or crepitus at the patella
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
PHASE 4: 12-16 weeks after surgery
GOALS
- Regain full muscle strength.
- Work on cardiovascular conditioning.
- Sports-specific training.
EXERCISE PROGRAM
Muscle Strengthening Exercises
You should continue muscle-strengthening exercises from Phase 2 and 3 on a three times a week basis. At this time, you can decrease the number of repetitions per set from 15 to 10. This will allow you to work with more resistance. Remember to do all exercises slowly, with good form. You may begin to hold dumbbells when doing the chair squat, single-leg 1/3 knee bends and single-leg wall slides. Weights can be increased when you can do a particular weight easily, for 3 sets of 10 repetitions, for 3 consecutive workouts. At all times, be cautious of pain or crunching at the kneecap or patellar tendon while exercising. You may use resistance machines at your gym, but do not use the knee extension machine and do not do lunging or high impact drills.
Cardiovascular Conditioning
You can use the elliptical trainer, stationary bicycle, rowing machine or swimming workouts to build cardiovascular fitness. Three to five times per week for 20 to 30 minutes is sufficient for improvement in this area. Please note that excessive long duration cardiovascular exercise can retard or delay muscular strength development when strength improvement and gains in muscle size are the programs' primary goal.
At this time, light running on a soft level surface with a sports brace can begin if your surgeon advises. You need to have full range of motion, good strength and no swelling to run safely. If you run, 3 times per week for 10 minutes is advisable for the first 2 weeks. If there is no pain or swelling, you can increase your running time by 1 minute per session for a maximum of 30 minutes. Walking and hiking on gentle trails can also be used for conditioning activity.
Jump and Plyometric training
With the approval of the doctor and physical therapist, you can begin the Jump and Plyometric Training Progression that is included in this packet.
Progressive Resistance Exercise (PRE) Principle
- To build muscle strength and size, the amount of resistance used must be gradually increased.
- The exercises should be specific to the target muscles
- The amount of resistance should be measurable and gradually increased over a longer period of time
- To avoid excess overload and injury, the weight or resistance must be gradually increased in increments of 5 to 10%
- Resistance can be increased gradually every 10 to 14 days when following a regular and consistent program.
- Adequate rest and muscle recovery between workout is necessary to maximize the benefit of the exercise
- If the PRE principle is followed too strictly, the weights potentially will go higher and higher.
- At a certain point, the joints and muscles will become overloaded and injury will occur.
- This eventuality can be avoided by refraining from using excessive weight during strength training.
Basic Knee Strengthening Program
Days per week: 2-3 Times per day: 1 3 sets of 10-15 repetitions
- Emphasis is to build muscle strength using BOTH legs
- Progress according to the PRE principle
Basic Program Exercises
- Leg Press
- Hamstring Curl
- Wall Slides (hold dumbbells for resistance)
- Roman Chair (strengthens hamstrings)
- Chair Squat (hold dumbbells for resistance)
- Calf Raises or calf raise machine
- Hip Abductor/Adductor machine
- Hip flexor machine
- Single leg strengthening progression
PRECAUTIONS
The following exercises can cause injury to the knee and are usually not recommended at this time:
- Leg extension machine (quadriceps extensions)
- Stairmaster or stair climber machines
- Lunges
- Squats past 90 degrees of knee flexion
- High Impact and plyometric exercises
PHASE 5: 16-24 weeks after surgery
Cardiovascular Conditioning
Continue with the program outlined in phase 4.
Muscle Strengthening Exercises
Continue with the program outlined in phase 4.
Speed and Agility Training
Refer to Speed and Agility Progression.
Sports-Specific Training
To reach your ultimate goal of returning to sports participation, you must follow an orderly sequence of drills that are designed to re-train the muscle-to-joint coordination that is necessary to provide the proper control of your knee. The following time-table illustrates an ideal progression sequence:
Return to sport eval recommendations:
- Hop tests (single leg, triple hop, crossover hop, 6 meter timed hop)
- Isokinetic strength test (60 degree/second)
- Vertical jump
- Deceleration shuttle test
Returning to Sports
You should discuss the exact timing of return to sports activities and brace use with your surgeon.
| Activity | Weeks post-surgery |
|---|---|
| Running slowly | 12-16 |
| Golf | 16-20 |
| Roller blading | 18 |
| Tennis | 20-24 |
| Return to sport practice | 24-32 |
| Full return to sport | 32-36 |
Speed and Agility Progression
GOALS
- Safely recondition the knee for the demands of sports activity
- Provide a logical sequence of progressive drills for pre-sports conditioning
- Provide objective criteria for safe return to sports
Phases of Training
- Straight ahead running phase
- Direction change running phase
- Unrestricted direction change and impact phase
Prerequisites
- Full Range of Motion
- Strength at least 80% of uninjured limb
- Thigh girth within 1/2 inch of unaffected limb
- No tenderness at the graft harvest site
- Symmetrical quadriceps and hamstring flexibility
- Perform and pass functional tests
- Obtain clearance from your doctor or physical therapist
Functional Tests
Before starting the running sequence you must be able to:
- Hop forward on both legs at least 2 feet
- Hop to either side at least 1 foot
- Hop up and down on both feet 10 times
- Jog with no limp for 100 yards
Warm-up, Stretch and Ice
Be sure that you warm-up and stretch before and after workouts. Generally, you should do some walking, cycling or elliptical so that you break a sweat before starting the running program. You can then stretch before beginning the running drills. Ice your knee for 20 minutes following workouts and stretch all muscle groups as you are cooling down.
Recommended Frequency: 2-3 times per week
Criteria to Progress
Do not progress to the next step in the phase until the present step is pain free, and you can perform with proper technique and without difficulty (muscle soreness or fatigue). Add only one new step in the progression per workout.
I. Straight Ahead Running (16-20 weeks)
- Run 1/2 speed 100 yards, 10 repetitions
- Run 3/4 speed 100 yards, 10 reps
- Run 1/2 speed 100 yards, 3 reps; 3/4 speed 100 yards, 3 reps; full-speed 50 yards, 4 reps
- Continue 1/2 and 3/4 speed 100-yard runs, for 3 reps each and add one 50-yard run each workout until you can do (10) 50-yard full speed runs.
II. Basic Change of Direction Running (20-24 weeks)
Intensity: Progress drills from walking → 1/2 speed → 3/4 speed → full speed. Continue current workout from above (Step 4): Run 1/2 and 3/4 speed 100 yd runs for 3 reps each. Run full speed 50-yard run for 5 reps.
Progressively add each step below:
- Zig-Zag run, round corners, 50 yards, 5 reps
- Backward run 25 yards to gradual stop, then forward run 25 yards to gradual stop, 5 reps
- Circle run 20 feet or greater diameter circle, 3 reps to left and 3 reps to right
- Figure '8' run 20 feet or greater length, 5 reps
- Carioca 50 yards, 5 reps left, 5 reps right
III. Advanced Speed and Agility Running (24 weeks onward)
Intensity: Progress drill from walking → 1/2 speed → 3/4 speed → full speed. Continue current workout above and progress with below:
- Run forward to plant-and-cut off of the unoperated limb, 1/2 speed, 5 reps
- Run forward to plant-and-cut off of the operated limb, 1/2 speed, 5 reps
- Zig-Zag drill with alternate limb plant-and-cut, 6 reps
- Box drill 20 yards square, 6 reps, alternate sides
- Shuttle run 50 yards with direction change every 10 yards, 5 reps
- Agility run, 5 reps, alternate starting sides
IV: Begin Sports Practice
Shuttle drill Box drill Agility drill
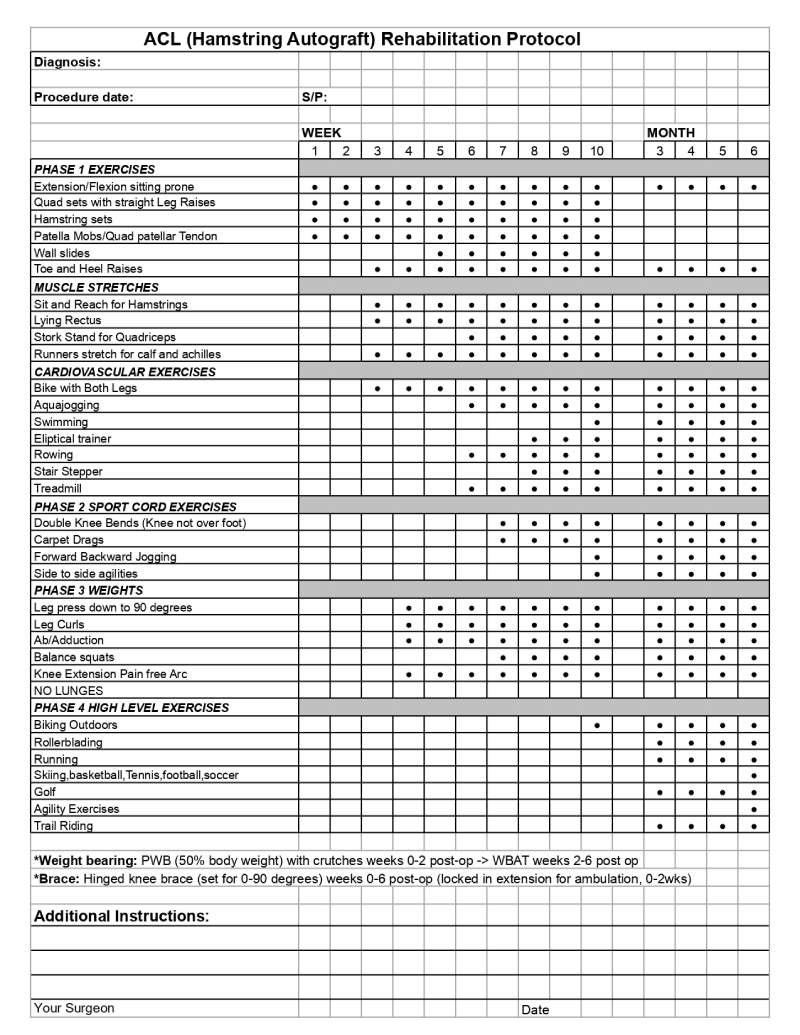
ACL Post-op Hamstring
Here are guidelines that will help you to prepare for ACL reconstruction surgery:
Preoperative Instructions
Before Surgery
Your Surgeon will see you in the office. He will do a preoperative history and physical examination and complete the necessary paperwork. He will write preoperative hospital orders and schedule an appointment with the pre-operative test center if needed. You will have an opportunity to speak with anesthesia and physical therapy. It is recommended that you utilize a stationary cycle to maintain your knee range of motion and improve the overall function of the knee prior to surgery. Continue to perform the ACL-preoperative exercises.
Several Days Prior to Surgery
Wash the knee with soap or Hibiclens several times per day to get the skin as clean as you can. This decreases the risk of infection. Be careful not to get any scratches, cuts, sunburn, poison ivy, etc. The skin has to be in very good shape to prevent problems. You do not need to shave.
The Day Before Surgery
You can have nothing to eat or drink after midnight on the day before surgery. It is very important to have a completely empty stomach prior to surgery for anesthesia safety reasons. This included no chewing gum or drinking coffee. If you have to take medication, you can do so with a sip of water early in the morning prior to surgery (but later tell the anesthesiologist you have done so).
Day of Surgery
Please bring any crutches, brace, ice machine or imaging studies that you have received.
Surgery
The operation to replace the torn anterior cruciate ligament will be done arthroscopically. A small incision will be made on the inner side of the knee to take the graft from the middle of the patellar tendon together with a small piece of bone from the bottom of the kneecap and the upper part of the tibia (mid-third patellar tendon graft, “bone-tendon-bone”). The incision leaves a small area of numbness on the outer side of the upper leg. Most of this numbness clears but it takes a year or two and is not usually bothersome. In certain circumstances, the graft is a hamstring tendon or a donor graft from a cadaver (allograft).
After Surgery
- The most important aspect is to get the knee out completely straight.
You will be given a prescription for pain medication to take home with you. In addition to this medication, you should take one aspirin per day to help prevent blood clots (phlebitis) for 14 days. The pain medication has a tendency to make you constipated and over the counter medication for constipation should be taken on an as needed basis.
The dressing can be removed at two days. The wound is sealed with steri-strips (small pieces of tape on the skin). You can shower on the second day following surgery, but be careful standing in the shower so that you do not fall. It is better to have a small stool to be able to sit on. However, you can get the leg wet and wash it, but do not scrub the wound or pick off steri-strips as they will fall off on their own. Do not submerge the knee under water in a bath, hot tub or swimming pool.
To help control swelling in the lower leg, you should elevate the extremity. If excessive swelling occurs, wear compression stockings after surgery until your first post-operative visit. If you develop calf pain or excessive swelling in the leg, call Greater Michigan Orthopedics.
A cryocuff is a blue wrap that is put on the knee to keep it cold. You can use this as often as you want to cool down the knee to reduce swelling and pain. Check your skin every time that you remove the wrap to make sure that it is intact. Be sure to stock up on extra ice in your freezer. These can be bought through the office. Ice bags work just as well.
ACL Reconstruction Rehabilitation Guidelines
Phase 1: 0–2 Weeks After Surgery
This handout is to use as a guideline for your rehabilitation after anterior cruciate reconstruction. You may vary in your ability to do these exercises and to progress from one phase to the other. Please call Greater Michigan Orthopedics if you are having a problem with your knee or if you need clarification of these instructions.
Goals
- Protect the reconstruction – avoid falling
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
Do not place a pillow under the knee for comfort. This can lead to knee stiffness.
Brace / Crutches
Your knee brace is set to allow your knee to bend and straighten from 0 to 90 degrees. Use it when walking. In some cases, you may be sent home with the brace locked at 0 degrees (fully straight). After you arrive home, and the anesthetic nerve block has worn off, unlock the brace to allow 0 to 90 degrees of motion.
You had an ACL reconstruction with Hamstring Autograft. Weight bearing is 50% for the first two weeks. Weight bear as tolerated with crutches beginning 3 weeks post operative. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you. In some cases, crutches and restricted weight bearing may be necessary for longer periods, such as if a meniscal repair was performed. Then you must remain partial weight bearing for 4 weeks. Your Surgeon or the physical therapist will give special instructions in these cases. Wean the crutches and advance to full motion at 4–6 weeks in these cases.
Criteria to discontinue crutches is when you attain a normal gait pattern.
Cryocuff (Cold Application)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15–20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
Wound Care
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
Free / Machine Weights (Upper Body / Trunk Only)
We suggest that you do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15–20 repetitions. Do not place yourself in a compromising position with your recently operated knee.
Exercise Program

Cardiopulmonary
UBE or similar exercise is recommended
Criteria for Phase 2
No lag SLR
Normal gait
Crutch D/c
ROM: no greater than 5 degree active extension lag, 110 active flexion
Phase 2: 2–6 Weeks After Surgery
Goals
- Protect the reconstruction, avoid falling
- Ensure wound healing
- Full ROM
- Begin quadriceps muscle strengthening
- Decrease knee and leg swelling
Cryocuff
Use the cryocuff or ice bags to decrease swelling for 20 minutes three times a day after each exercise session.
Brace/Crutches
In cases where the patellar tendon autograft is used, you can begin placing all of your weight on the operated leg when you walk unless otherwise instructed by your Surgeon. Discontinue using your crutches when you are comfortable doing so. Continue using your brace when walking outside of the home. Within one or two weeks, you can usually discontinue use of the crutches if you have good control of the leg and are sure that you will not fall or get injured. Concentrate walking normally, in a heel-strike to toe-off pattern, without a limp. Occasionally (every one or two hours) practice standing on your operated leg, with your knee fully straight, for 10 to 20 seconds.
In cases where a meniscus repair is done along with the ACL reconstruction, the brace should be locked fully straight when walking for the first 6 weeks after surgery.
Exercise Program – Stationary Bicycle
Days per week: 5-7 Times per day: 1-2
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for up to 10-15 minutes, 1 to 2 times a day.
Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
Water Workout (Optional)
Days per week: 3 Times per day: 1
Aqua-jogger exercise or Flutter kick swimming 20-30 minutes
Range of Motion and Strengthening Exercises (Brace Off)
Days per week: 5-7 Times per day: 1-2
ROM
- Low load, long duration (assisted PRN)
- Heel slides/wall slides
- Heel prop/prone hang (minimize co-contraction/nociceptor response)
- Bike (rocking-for-range → Ride with low seat height)
- Flexibility stretching all major groups
Strengthening
- Quads: Quad sets, Mini Squats/Wall Squats, Steps-ups, Knee extension from 90-40, Leg press
- Hamstrings: Hamstring curls closed chain, resistive SLR with sports cord
Other Musculature
- Hip adduction/abduction: SLR or with equipment
- Standing Heel raises: progress from double to single leg support
- Seated calf press against resistance
- Multi-hip machine in all directions with proximal pad placement
Neuromuscular
- Wobble board
- Rocker board
- Single-leg stance with or without equipment
Cardiopulmonary
Bike, Elliptical
Criteria for Progression to Phase 3
- Full ROM
- Minimal effusion
- Functional strength and control in daily activities
- IKDC Question #10 (global rating of function) score 7 or higher
Phase 3: 7–12 Weeks After Surgery
Goals
- Protect the reconstruction; avoid falling
- Maintain full ROM
- Walk with a normal heel-toe gait with no limp
- Muscle strength and conditioning improvements
Brace
The brace is discontinued after you see your surgeon at your 6-week post-operative office visit. Concentrate on walking with a heel-toe gait without a limp. In some cases, use of the brace will continue if the knee requires a longer period of protection.
Cryocuff / Ice
Continue to use the cryocuff for 20 minutes after each workout.
Exercise Program
Strengthening:
- Squats
- Leg press
- Hamstring curl
- Knee extension 90 to 0
- Step-ups/down
- Shuttle
- Sports cord
- Wall squats
Neuromuscular Training:
- Wobble board
- Rocker board
- Roller board
- Perturbation training
- Instrumented testing systems
- Varied surfaces
Cardiopulmonary: Continue Bike and Elliptical
Precautions When Exercising
- Avoid pain at the patellar tendon site
- Avoid pain and/or crepitus at the patella
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are “warmed –up” when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
Phase 4: 12-16 Weeks After Surgery
Goals
- Regain full muscle strength.
- Work on cardiovascular conditioning.
- Sports-specific training.
Exercise Program
Muscle Strengthening Exercises
You should continue muscle-strengthening exercises from Phase 2 and 3 on a three times a week basis. At this time, you can decrease the number of repetitions per set from 15 to 10. This will allow you to work with more resistance. Remember to do all exercises slowly, with good form. You may begin to hold dumbbells when doing the chair squat, single-leg 1/3 knee bends and single-leg wall slides. Weights can be increased when you can do a particular weight easily, for 3 sets of 10 repetitions, for 3 consecutive workouts. At all times, be cautious of pain or crunching at the kneecap or patellar tendon while exercising. You may use resistance machines at your gym, but do not use the knee extension machine and do not do lunging or high impact drills.
Cardiovascular Conditioning
You can use the elliptical trainer, stationary bicycle, rowing machine or swimming workouts to build cardiovascular fitness. Three to five times per week for 20 to 30 minutes is sufficient for improvement in this area. Please note that excessive long duration cardiovascular exercise can retard or delay muscular strength development when strength improvement and gains in muscle size are the programs’ primary goal.
At this time, light running on a soft level surface with a sports brace can begin if your surgeon advises. You need to have full range of motion, good strength and no swelling to run safely. If you run, 3 times per week for 10 minutes is advisable for the first 2 weeks. If there is no pain or swelling, you can increase your running time by 1 minute per session for a maximum of 30 minutes. Walking and hiking on gentle trails can also be used for conditioning activity.
Jump and Plyometric Training
With the approval of the doctor and physical therapist, you can begin the Jump and Plyometric Training Progression that is included in this packet.
Progressive Resistance Exercise (PRE) Principle
- To build muscle strength and size, the amount of resistance used must be gradually increased.
- The exercises should be specific to the target muscles
- The amount of resistance should be measurable and gradually increased over a longer period of time
- To avoid excess overload and injury, the weight or resistance must be gradually increased in increments of 5 to 10 %
- Resistance can be increased gradually every 10 to 14 days when following a regular and consistent program.
- Adequate rest and muscle recovery between workout is necessary to maximize the benefit of the exercise
- If the PRE principle is followed too strictly, the weights potentially will go higher and higher.
- At a certain point, the joints and muscles will become overloaded and injury will occur.
- This eventuality can be avoided by refraining from using excessive weight during strength training.
Basic Knee Strengthening Program
Days per week: 2-3 Times per day: 1 3 sets of 10-15 repetitions
- Emphasis is to build muscle strength using BOTH legs
- Progress according to the PRE principle
Basic Program Exercises
- Leg Press
- Hamstring Curl
- Wall Slides (hold dumbbells for resistance)
- Roman Chair (strengthens hamstrings)
- Chair Squat (hold dumbbells for resistance)
- Calf Raises or calf raise machine
- Hip Abductor/Adductor machine
- Hip flexor machine
- Single leg strengthening progression
Precautions
The following exercises can cause injury to the knee and are usually not recommended at this time:
- Leg extension machine (quadriceps extensions)
- Stairmaster or stair climber machines
- Lunges
- Squats past 90 degrees of knee flexion
- High Impact and plyometric exercises
Phase 5: 16-24 Weeks After Surgery
Cardiovascular Conditioning
Continue with the program outlined in phase 4
Muscle Strengthening Exercises
Continue with the program outlined in phase 4
Speed and Agility Training
Refer to Speed and Agility Progression
Sports-Specific Training
To reach your ultimate goal of returning to sports participation, you must follow an orderly sequence of drills that are designed to re-train the muscle-to-joint coordination that is necessary to provide the proper control of your knee. The following time-table illustrates an ideal progression sequence:

Return to Sport Eval Recommendations
- Hop tests (single leg, triple hop, crossover hop, 6 meter timed hop)
- Isokinetic strength test (60degree/second)
- Vertical jump
- Deceleration shuttle test
Returning to Sports
You should discuss the exact timing of return to sports activities and brace use with your Surgeon.
Speed and Agility Progression
Goals
- Safely recondition the knee for the demands of sports activity
- Provide a logical sequence of progressive drills for pre-sports conditioning
- Provide objective criteria for safe return to sports
Phases of Training
- Straight ahead running phase
- Direction change running phase
- Unrestricted direction change and impact phase
Prerequisites
- Full Range of Motion
- Strength at least 80 % of uninjured limb
- Thigh girth within 1⁄2 inch of unaffected limb
- No tenderness at the graft harvest site
- Symmetrical quadriceps and hamstring flexibility
- Perform and pass functional tests
- Obtain clearance from your doctor or physical therapist
Functional Tests
Before starting the running sequence you must be able to:
- Hop forward on both legs at least 2 feet
- Hop to either side at least 1 foot
- Hop up and down on both feet 10 times
- Jog with no limp for 100 yards
Warm-up, Stretch and Ice
Be sure that you warm-up and stretch before and after workouts. Generally, you should do some walking, cycling or elliptical so that you break a sweat before starting the running program. You can then stretch before beginning the running drills. Ice your knee for 20 minutes following workouts and stretch all muscle groups as you are cooling down.
Recommended Frequency
2-3 times per week
Criteria to Progress
Do not progress to the next step in the phase until the present step is pain free, and you can perform with proper technique and without difficulty (muscle soreness or fatigue). Add only one new step in the progression per workout.
I. Straight Ahead Running (16-20 weeks)
- Run 1⁄2 speed 100 yards, 10 repetitions
- Run 3⁄4 speed 100 yards, 10 reps
- Run 1⁄2 speed 100 yards, 3 reps; 3⁄4 speed 100 yards, 3 reps; full-speed 50 yards, 4 reps
- Continue 1⁄2 and 3⁄4 speed 100-yard runs for 3 reps each and add one 50-yard run each workout until you can do (10) 50-yard full speed runs.
II. Basic Change of Direction Running (20-24 weeks)
Intensity: Progress drills from walking → 1⁄2 speed → 3⁄4 speed → full speed.
Continue current workout from above (Step 4): Run 1⁄2 and 3⁄4 speed 100 yd runs for 3 reps each. Run full speed 50-yard run for 5 reps.
Progressively add each step below:
- Zig-Zag run, round corners, 50 yards, 5 reps
- Backward run 25 yards to gradual stop, then forward run 25 yards to gradual stop, 5 reps
- Circle run 20 feet or greater diameter circle, 3 reps to left and 3 reps to right
- Figure ‘8’ run 20 feet or greater length, 5 reps
- Carioca 50 yards, 5 reps left, 5 reps right
III. Advanced Speed and Agility Running (24 weeks onward)
Intensity: Progress drill from walking → 1⁄2 speed → 3⁄4 speed → full speed.
Continue current workout above and progress with below:
- Run forward to plant-and-cut off of the unoperated limb, 1⁄2 speed, 5 reps
- Run forward to plant-and-cut off of the operated limb, 1⁄2 speed, 5 reps
- Zig-Zag drill with alternate limb plant-and-cut, 6 reps
- Box drill 20 yards square, 6 reps, alternate sides
- Shuttle run 50 yards with direction change every 10 yards, 5 reps
- Agility run, 5 reps, alternate starting sides
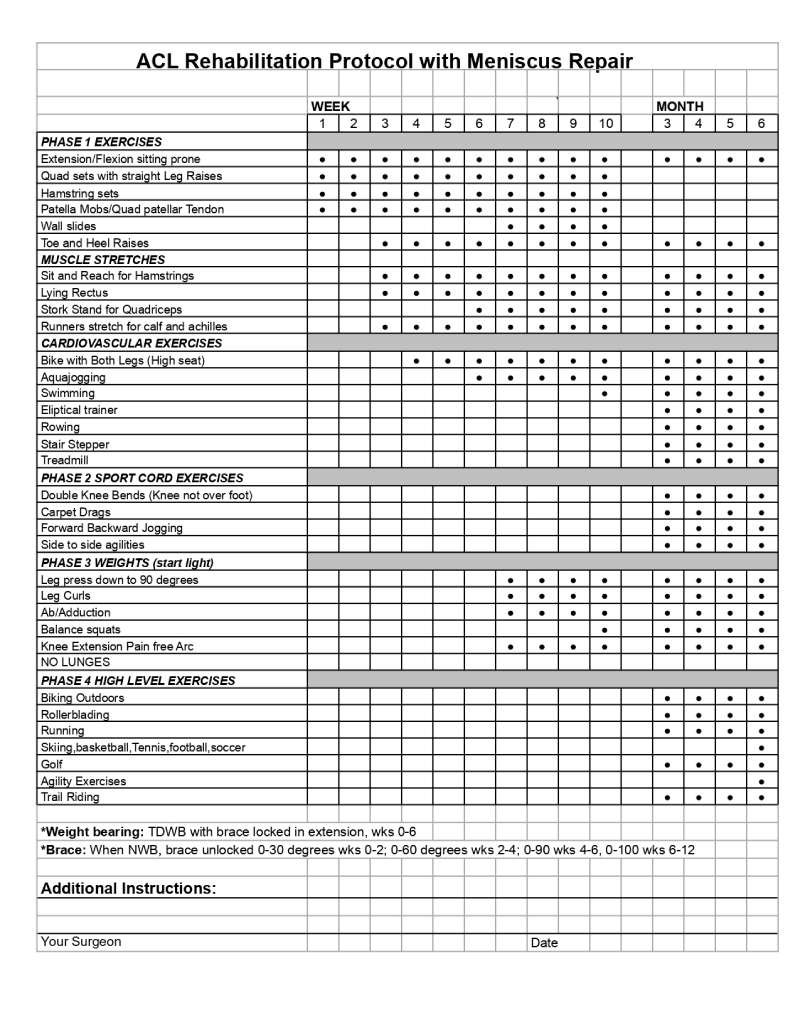
ACL pre-op protocol
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee
Phase One: The First Six Weeks After Injury
Initially, the knee needs to be protected-use the knee immobilizer and/or crutches and avoid full weight bearing. Apply ice and an elastic wrap to control swelling. Elevate the leg and use elastic stockings if the leg is swollen. As the pain lessens and the swelling decreases, try to gradually regain knee motion. Avoid pivoting or twisting the knee because it might be unstable and give out.
Do not place a pillow under the knee for comfort. This can lead to knee stiffness. When walking, bear weight according to the doctor’s instructions. Use crutches to assist when walking. You may gradually wean from 2 crutches to 1 crutch, held on the side opposite the injured knee. Progress to no crutch(es) or brace when you can walk without a limp and there is no pain. Ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury. Ice for 20 minutes, three times a day.
At about three weeks following injury, the pain is usually subsiding and the swelling is lessened. You can now try to stretch the knee to regain motion. Stationary cycle, swimming (flutter kick only) and the following exercise program are recommended.
Quadriceps Setting – To Maintain Muscle Tone in the Thigh (Quadriceps) Muscles and Straighten the Knee
Lie on your back with the knee extended fully straight as in the figure. Contract and hold the front thigh muscles (quadriceps) making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscles. The tightening action of the quadriceps muscles should make your knee straighten and be pushed flat against the bed or floor. Hold five seconds for each contraction.
Do at least 20 repetitions three or four times a day until you can fully straighten your knee equal to the uninjured side.
Heel Prop – To Straighten (Extend) the Knee
Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
Heel Slides – To Regain the Bend (Flexion) of the Knee
While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for five seconds and then slowly relieve the stretch and straighten the knee.
While the knee is straight, you may repeat the quadriceps setting exercise. Continue this exercise until you can fully bend your knee equal to the uninjured side. As you start to gain flexion, you can assist your efforts to gain flexion by assisting the heel slide with a towel. Repeat 20 times, three times a day.
Straight Leg Lift
The quality of the muscle contraction in this exercise is what counts the most, not just the ability to lift the leg!
- Tighten the quadriceps (quadriceps setting) as much as you can, push the back of the knee against the floor.
- Tighten this muscle harder.
- Lift your heel 4 to 6 inches off the floor.
- Tighten the quadriceps harder again.
- Lower your leg and heel back to the floor. Keep the quadriceps as tight as possible.
- Tighten this muscle harder again.
- Relax and repeat.
If the knee bends when you attempt to lift the limb off of the bed, do not do this exercise. Keep trying to do the quadriceps setting exercise until you can lift the limb without letting the knee bend.
You can advance to the following exercise program to help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds.
Do the exercises daily for the first week, then decrease to every other day when using ankle weights. You may ride the stationary bicycle daily for 10 to 20 minutes.
Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
Stationary Bicycle
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal and pedal back and forth until your knee will bend far enough to allow a full cycle.
Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 10 to 20 minutes a day.
Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then ride the bicycle with your forefoot resting on the pedal.
Standing Hamstring Curl
Stand facing the wall, using the wall for balance and support. While standing on the uninjured limb bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated. Repeat 20 times.
Standing Toe Raise
Stand facing a table, hands on the table for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on tip-toes while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 times.
Hip Abduction
Lie on your uninjured side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, then lower slowly. Repeat 20 times.
Wall Slides
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees. Pause five seconds and then slowly slide back up to the upright starting position. Do 3 sets of 10 to 15 repetitions.
High Tibial Osteotomy Surgery
Here are guidelines that will help you in preparing for high tibial osteotomy surgery.
PREOPERATIVE INSTRUCTIONS WITHIN A FEW WEEKS BEFORE SURGERY:
Your Surgeon will see you in the office. He will do a preoperative history and physical examination and complete the necessary paperwork. It is recommended that you utilize a stationary cycle to maintain your knee range of motion and improve the overall function of the knee prior to surgery.
SEVERAL DAYS PRIOR TO SURGERY:
Wash the knee with soap or Hibiclens solution to get it as clean as you can. This decreases the risk of infection. Be careful not to get any scratches, cuts, sunburn, poison ivy, etc. The skin has to be in very good shape to prevent problems. You do not need to shave.
THE DAY BEFORE SURGERY:
You can have nothing to eat or drink after midnight on the day before surgery. It is very important to have a completely empty stomach prior to surgery for anesthesia safety reasons. If you have to take medication, you can do so with a sip of water early in the morning prior to surgery (but later tell the anesthesiologist you have done so).
DAY OF SURGERY:
Bring any crutches, brace, ice machine or imaging studies that you have received.
SURGERY:
HIGH TIBIAL OSTEOTOMY (HTO) is a surgical procedure aimed repositioning the knee joint, realigning the mechanical axis of the limb so that less pressure/body weight goes through the worn area of your knee. This distributes your weight more evenly through both sides of the knee. The surgical technique involves making an incision over the tibia, below the knee joint. A wedge of bone is removed, based on the surgeon's calculations, to allow the angle of the knee to be adjusted. The space created in the tibia is filled with a bone graft taken from the crest of your pelvis or hip-bone and a metal plate and screws is used to hold the tibia in position while it heals. In some cases, the doctor will perform microfracture surgery in combination with the HTO.
Appropriate rehabilitation of the knee after surgery is critical to the success of the operation.
Any other indicated procedures that will be done may change your therapy protocol and rehabilitation. Your Surgeon will provide you with more rehab information if this is the case.
Dressing
The dressing should be changed the day following surgery and can be removed at two days. The wound is sealed with steri-strips (small pieces of tape on the skin). You can shower on the second day following surgery, but be careful standing in the shower so that you do not fall. It is better to have a small stool to be able to sit on. However, you can get the leg wet and wash it. Do not submerge the knee under water in a bath, hot tub or swimming pool.
Cold Therapy
You may also receive a cryocuff. The cryocuff is a closed loop cuff that circulates cold water and provides compression around your knee to help minimize swelling and pain. You can use this as often as you want to cool down the knee to reduce swelling and pain. Check your skin every time that you remove the wrap to make sure that it is intact.
Physical Therapy
You should make arrangements to start physical therapy between 3-5 days following your surgery. Your therapist will help make sure you understand the program we want you to follow and assist you in making sure all exercises are performed correctly. If you will be seeking rehab services elsewhere, contact your physical therapist directly.
***If you develop calf pain or excessive swelling in the leg, call Greater Michigan Orthopedics or present to your local ER.***
HTO Rehabilitation Protocol
This protocol is a guideline for your rehabilitation after high tibial osteotomy surgery. Please call our office if you are having a problem with your knee or if you need clarification of these instructions.
PHASE I: 0 – 2 weeks after surgery
You will go home with crutches, cryocuff cold therapy unit.
GOALS:
- Protect the osteotomy – avoid weight bearing.
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
ACTIVITIES:
BRACE/CRUTCHES
Unless otherwise instructed by your Surgeon, use crutches when walking and do not bear weight on the operated leg.
CRYOCUFF (COLD APPLICATION)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15-20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
WOUND CARE
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
5. ASPIRIN / ELASTIC STOCKINGS
Take an aspirin each morning for one month, wear an elastic stocking (TED) that extends above the knee, and do at least 10 ankle pump exercises each hour to help prevent phlebitis (blood clots in the veins).
6. FREE/MACHINE WEIGHTS
Upper Body/Trunk Only
Do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15-20 repetitions. Do not place yourself in a compromising position with your recently operated knee.
EXERCISE PROGRAM
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles and straighten the knee.
Sit or lie on your back with the knee extended fully straight as shown in the figure. Tighten and hold the front thigh muscle making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscle. The tightening action of the quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold 5 seconds for each contraction. Do 20 repetitions or more, three times a day.
HEEL PROP- to straighten (extend) the knee.
Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
HEEL SLIDES - to regain the bend (flexion) of the knee.
While lying on your back, actively slide your heel backward to bend the knee as shown in the figure. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise. Repeat 20 times, three times a day.
SITTING HEEL SLIDES - to regain the bend (flexion of the knee).
When sitting in a chair or on the edge of a bed, slide the heel backward as if trying to get the foot underneath the chair. Hold 5 seconds and slowly relieve the stretch by sliding the foot forward. You can help in both directions with the opposite foot. Repeat 20 times, three times a day.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to see your Surgeon approximately ten to fourteen days after your surgery. At this time, your sutures will be removed and your progress will be checked.
HTO Rehabilitation Protocol
Phase Two: 2 to 6 weeks after surgery
Goals:
- Protect the knee from overstress and allow healing
- Regain full motion
- Begin muscle strengthening
Brace and Crutches:
Unless otherwise instructed by the doctor, use crutches when walking and do not bear weight on the operated leg. When walking with the crutches follow the instructions below:
Walking ('toe-touch' non-weight bearing):
- Put the crutches forward about one step's length.
- Put the injured leg forward; level with the crutch tips.
- Touch the toe of the involved leg to the floor to help you balance but do not bear weight on the leg.
- While bearing all of your weight on the crutches, take a step through with the uninjured leg.
Exercise Program
The following exercise program should be followed as directed by the doctor or the physical therapist. Do the exercises daily unless otherwise noted.
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 20 to 30 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
WATER WORKOUT (optional)
Utilize an Aqua jogger floatation vest to run in deep water with no foot contact to the pool floor or swim flutter kick only for up to 20 minutes 2 or 3 times a week.
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles and straighten the knee.
Lie on your back with the knee extended fully straight. Tighten and hold the front thigh muscle making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscle. The tightening action of the quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold 5 seconds for each contraction. Do 20 repetitions three times a day until you can fully straighten your knee equal to the non operative side.
HEEL PROP - to straighten (extend) the knee.
Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
HEEL SLIDES - to regain the bend (flexion) of the knee.
While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise. Continue this exercise until you can fully bend your knee equal to the non operative side. Repeat 20 times, three times a day.
STRAIGHT LEG LIFT
The quality of the muscle contraction in this exercise is what counts the most, not just the ability to lift the leg!
- Tighten the quadriceps (quadriceps setting) as much as you can, push the back of the knee against the floor.
- Tighten this muscle harder!
- Lift your heel 4 to 6 inches off the floor
- Tighten the quadriceps harder again.
- Lower your leg and heel back to the floor. Keep the quadriceps as tight as possible.
- Tighten this muscle harder again. 7. Relax and repeat.
If the knee bends when you attempt to lift the limb off of the bed, do not do this exercise. Keep trying to do the quadriceps setting exercise until you can lift the limb without letting the knee bend.
SHORT ARC LIFT
With the knee bent over a rolled up towel or blanket of a height of 4-5 inches (the knee should be bent only 20-25 degrees), lift the foot so that the knee fully straightens. Hold the knee locked in extension for 5 seconds, then slowly lower. Repeat 20 times.
STANDING HAMSTRING CURL
Stand facing the wall, using the wall for balance and support. While standing on the unoperated limb bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated. Repeat 20 times.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
HIP ABDUCTION
Lie on your unoperated side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, and then lower slowly. Repeat 20 times.
OFFICE VISIT
Please make an appointment with your Surgeon at 6-8 weeks after surgery.
HTO Rehabilitation Protocol
Phase Three: 7 to 12 weeks after surgery
Goals:
- Begin partial weight bearing
- Regain full motion
- Regain full muscle strength
Brace and Crutches:
Unless otherwise instructed by the doctor, continue to use crutches when walking and you can begin bearing up to 50% of your weight on the operated leg. When walking with the crutches follow the instructions below:
Walking (50% partial-weight bearing):
- Put the crutches forward about one step's length.
- Put the injured leg forward; level with the crutch tips.
- Touch the foot of the involved leg to the floor and bear 50% of the weight of a normal step.
- While bearing half weight on the crutches and half of your weight on the involved leg, take a step through with the uninjured leg.
Exercise Program
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds. Do the exercises daily for the first week, then decrease to every other day when using ankle weights. You may ride the stationary bicycle daily for 10 to 20 minutes. Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 10 to 20 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then ride the bicycle with your forefoot resting on the pedal.
WATER WORKOUT (optional)
The water workout can continue as described in phase 2.
EXERCISE PROGRAM (see phase 2 for descriptions and illustrations)
- QUADRICEPS SETTING
- HEEL SLIDES
- STRAIGHT LEG LIFT
- SHORT ARC LIFT
- STANDING HAMSTRING CURL
- STANDING TOE RAISES
- HIP ABDUCTION
Do the above exercises every other day for 3 sets of 10 repetitions. Follow the outline on the first page of phase three where the ankle weight program is described.
Add the wall slide exercise (every other day) as described below. Do not do the wall slide if there is pain or grinding at the kneecap.
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees. Pause five seconds and then slowly slide back up to the upright starting position. When doing a wall slide, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe. Do 3 sets of 10 to 15 repetitions.
STANDING TOE RAISE
Stand facing a wall, hands on the wall for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 times.
SEATED LEG PRESS
If you are using a leg press machine for strengthening, use an amount of weight that feels easy enough to perform 20 repetitions as the starting weight for this exercise. Use this weight for the first week before raising the weight. The weight may be increased by about 5 pounds every 7 to 10 days thereafter, as long as you can perform 20 repetitions per set for 3 sets, and as long as the weight used does not exceed body-weight when using both legs, or 1/2 body weight when using the one leg. In this exercise, avoid letting the knees snap or drop suddenly into extension when reaching the fully straightened position. Avoid starting the exercise with the knees bent past 45 degrees. Adjust the seat position to limit the excursion of the machine.
STRETCHING EXERCISES
Times per week: 5-7 Times per day: 1-2
| Quadriceps Stretch | 3-5 reps holding 15-30 seconds |
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Calf stretch | 3-5 reps holding 15-30 seconds |
Quadriceps Stretch prone
This stretch is performed in the position illustrated at the right. Bend your knee, grasping your toes, foot or ankle. If you are too tight to do this, loop a belt or towel around your ankle and grasp that. Pull the heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold 15 to 20 seconds for 3 to 5 repetitions.
Hamstring Stretch
Perform this stretch in the position illustrated at the right. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for 15 to 20 seconds and repeat 3 to 5 times.
Calf/Achilles Stretch
In the position illustrated, keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for 15 to 20 seconds, 3 to 5 repetitions.
OFFICE VISIT
Please set up an appointment to see your Surgeon in 6 weeks (12 weeks after surgery).
HTO Rehabilitation Protocol
Phase Four: Twelve weeks after surgery onward
- Walk normally
- Regain full motion
- Regain full muscle strength
Weight bearing instructions
If instructed by your Surgeon, you may begin to progressively bear full weight and walk on the leg. Try to avoid limping and walk slowly but normally. Start by walking with 50-75% weight and both crutches for 7 days. If pain free, then wean to one crutch on the opposite side of surgery for 7 days. Discontinue the crutch after that when you can walk normally with no pain or limp.
Exercise Program
Continue to follow the exercise program outlined in phase 2 and 3 on a three times a week basis. Ankle weights can be built up gradually, but not so much that you overload the knee. The step-up progression, chair squats, and the following stretches can be added to the exercise program at this time as long as they do not cause any pain or swelling.
Exercises
Cycling (road or mountain or stationary) — Stay on flat ground and on the seat. Progress the resistance as tolerated. Perform for 30-45 minutes.
STRETCHING EXERCISES
Times per week: 5-7 Times per day: 1-2
Range of Motion and Strengthening Exercises
Days per Week: 3 Times per Day: 1
- Straight Leg Lift
- Side Abduction Leg Lift
- Short Arc Lift (30 degrees or less)
- Standing Hamstring Curls
- Add 1 lb. per week to reach 5 lbs. 3 sets of 15 repetitions
| Quadriceps Stretch | 3-5 reps holding 15-30 seconds |
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Calf stretch | 3-5 reps holding 15-30 seconds |
Squat to chair
In the chair squat exercise, you lower your buttocks toward the chair until your buttocks touch the chair. Do not sit or rest at the chair, but instead immediately and slowly return to the standing and starting position. Remember to keep your head over your feet and bend at the waist as you descend. When doing a squat, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe.
For patellar/trochlear microfracture patients, do only a partial squat about 1/3 way to the chair. The angle at the knee should not exceed 30 degrees to avoid excess stress on the healing cartilage. Do not do this exercise if there is pain or grinding at the kneecap. After the first week, you may hold dumbbells while performing this exercise and the wall slide. Start with 3 to 5 pounds each hand. You may add 2 to 3 pounds per week until you reach 10 pounds in each hand. 3 sets of 10 to 15 repetitions.
Wall Slides
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 30 degrees (illustration). Do not slide down deeper than 45 degrees at the knee to avoid kneecap problems (this instruction is especially important for patellar and trochlear microfractures). Pause for five seconds and then slowly slide back up to the upright starting position. When doing a wall slide, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe. Do 3 sets of 10 to 15 repetitions.
Step Up- Down Exercise
Place the foot of the operated limb on a stool or step. Maintain balance, if necessary, by holding onto the wall or a chair (illustration). Standing sideways to the step, slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and then step up onto the stool by straightening the knee using the quadriceps muscles. Try to keep an upright posture and avoid bending forward during the exercise. When doing a step up-down, you should position your thigh so that your kneecap is in line with the tip of your shoe, or your second toe. Do 3 sets of 10 to 15 repetitions.
Progression for Step Up-Down Exercise
Start with a step of 3 inches in height. Start with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 6 inches in height. Repeat the above progression starting with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 9 inches in height (the height of a standard stair). Repeat this process of progression from 3 sets of 5, to 3 sets of 10 (about 2 weeks).
OFFICE VISIT
Please make an appointment to see your Surgeon in 12 weeks (6 months after surgery).
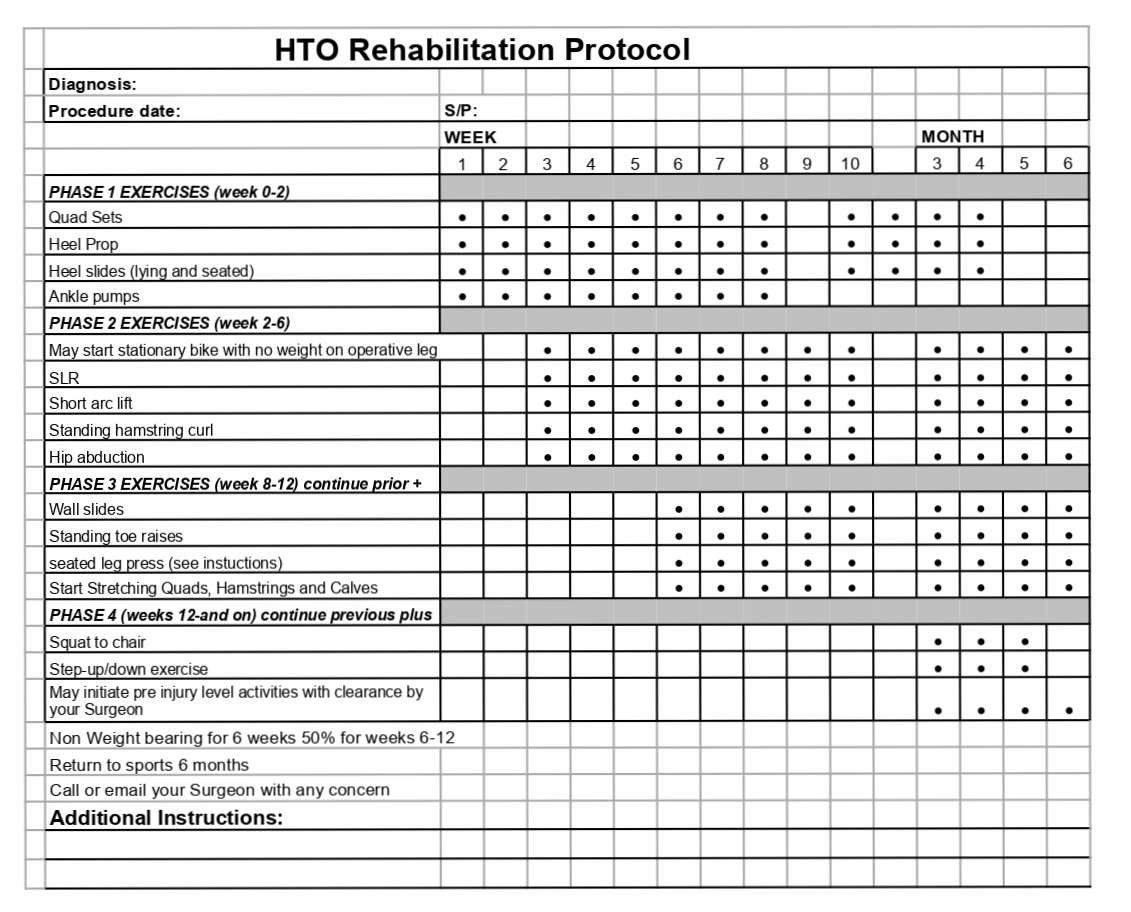
Iliotibial Band Tendinitis
Anatomy
The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches to the outer tibia. When the knee moves the iliotibial band slides over a bony prominence on the outer knee (lateral femoral epicondyle). Iliotibial band friction syndrome or iliotibial band tendinitis is a painful condition on the outer (lateral) aspect of the knee that is common in long distance runners.
Injury
The iliotibial band friction syndrome is an overuse injury caused by repetitive friction of the iliotibial band crossing the lateral femoral epicondyle. It is a well recognized cause of knee pain in runners, so it is commonly called "runner's knee”. It can also occur in other athletes.
The average jogger strikes the foot against the ground 3,000 times per mile. This adds up to 60,000 foot impacts for every twenty miles. While running you only have one foot on the ground at a time. When walking, 30 percent of the time, both feet are on the ground. When running, the force of landing has been estimated to be about three times your body weight. This means that if you weigh 150 pounds, the force in your leg when you land is around 450 pounds. Shoe mileage should also be considered. After 500 miles most shoes retain less than 60% of their initial shock absorption capacity.
When cycling, with each pedaling stroke, the iliotibial band slides over the lateral femoral epicondyle. Knee flexion and extension occur approximately 4800 times an hour (at an average cadence of 80 revolutions per minute), so the iliotibial band is susceptible to repetitive irritation.
Treatment
The injury is the result of too much running. In the simplest terms, if you stop running, the injury will eventually heal. There are ways, however to continue to run if you modify your training schedule and technique.
Initial treatment has two objectives: to reduce the inflammation and to allow the iliotibial band to heal. When the knee is painful and swollen, you must rest it. Avoid activities that aggravate the pain. Reduce your activity to a pain free level. Keep your knee straight while sitting, and avoid repetitive squatting. Let pain be your guide. Mild discomfort or ache is not a problem but do not do activities that cause definite pain.
Ice your knee for 20 minutes, two or three times a day and after any sporting activities—apply a bag of crushed ice over a towel. This reduces swelling, inflammation and pain. Aspirin, Aleve or Advil sometimes helps to relieve pain and reduce inflammation.
A physical therapist or your Surgeon can recommend exercises to strengthen the muscles. Exercises can also be used to stretch and balance the thigh muscles. In rare cases surgery may be indicated.
Sports
Use your judgement. When your knees hurt, avoid sports that may aggravate your knee problems. Total elimination of running may be required for a while. When your knee is better, you should be able to return to most sports.
Sports that aggravate iliotibial band syndrome:: Distance running, Cycling, Volleyball, Basketball, Soccer, Racquetball, Squash, Football, Weightlifting (squats)
Sports that may or may not cause symptoms: Baseball, Hockey, Skiing, Tennis
Sports that are easiest on the knees: Swimming (especially with a flutter kick), Walking (avoid up and down hills), Cross-country skiing
Although many sports can cause or aggravate the iliotibial band, running is the main culprit. It is better to vary your running schedule and use interval training: run sprints three days a week, intermediate distance two days a week and long distance once a week.
Exercises
The following exercise program should be followed as instructed by your Surgeon or physical therapist. For the straight leg lift and short arc lift, ankle weights can be added to increase resistance and strength of the quadriceps. Generally, after one or two weeks, ankle weights can be added (starting at one pound) and increased by one pound per week until you build to five pounds.
The exercises should be done daily until ankle weights are added. At this time, the straight-leg lift, short-arc lift and wall slides should be done every other day and the stretches should continue daily. When you have built up to five pounds on the straight-leg and short-arc lifts, continue the exercises two times per week for maintenance.
Exercise Program
- Straight Leg Raise – Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 10-15 pounds.
- Side laying Hip adduction – Lay on side that is affected. Keep your ankle, knee, hip and shoulder in a straight line. Raise the affected leg so that your foot is just past midline. Hold for a count of 6 and repeat 3 sets of 15 reps. Add weight just like #1 until you reach the goal weight of 10-15 pounds.
- 1/4 Squats – Stand with your feet shoulder width apart. Toes pointing straight ahead. Look down at your feet, lean with your butt first and squat down slowly until your knees pass over your toes then stand back up to start position. Perform 3 sets of 15 repetitions. You may hold dumbbells to add resistance.
- Short Arc Knee Extension – Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 15 repetitions. Add weight just like #1 until the goal weight is reached of 10-30 pounds.
- Quad Sets – Isometric exercise. This can be done where ever the knee is straight (laying in bed, standing, or reclined in the lax-y-boy). Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 15 repetitions.
- Wall Squats – Put your back flat against the wall. Stand with your feet shoulder width apart. Heel approximately 18 inches from the wall. Toes point straight ahead. Slide down the wall until your knee is at a 60 degree angle. Stay in this position for a count of 30. Return to start position. Repeat 3 sets of 15.
- Standing Hamstring Curl – Stand facing a table, using the table for balance and support. While standing on the uninjured limb bend the injured knee up toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as shown in the illustration. Repeat twenty times.
- Standing Toe Raises – Stand facing a table, hands on the table for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on tip-toes while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat twenty times.
- Hamstring Stretch – Perform this stretch in the position illustrated at the right. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for fifteen to twenty seconds and repeat three to five times.
- Quadriceps Stretching – This stretch is performed in the position illustrated at the right. Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold fifteen to twenty seconds for three to five repetitions.
- Calf Stretch – In the position illustrated, keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for fifteen to twenty seconds, three to five repetitions.
- Lateral Hip and Thigh Stretch (for the Iliotibial Band) – Cross your left (right) leg over in front of the other. Lean to the left (right), bending at the waist and letting your right (left) hip jut out. When you feel a gentle stretch in the outside of hip, hold fifteen to twenty seconds, three to five repetitions.
Knee Surgery
Rehabilitation After Arthroscopic Knee Surgery
This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to full resumption of your previous activity. Please call Greater Michigan Orthopedics or your physical therapist if you are having a problem with your knee or need clarification of the exercises.
Guidelines and Activities:
- The novocaine that is put in your knee at the time of surgery lasts six to eight hours. Begin taking the pain medication when you start feeling sensation return. The knee will be painful for several days after the arthroscopy.
- You can bear full weight and walk on the leg unless otherwise instructed by your Surgeon. In some instances, crutches can be used for a period of time if walking is uncomfortable.
- Gently move the knee (flexion and extension) as much as you can to prevent stiffness.
- Apply cold to reduce pain and swelling. Use ice on the knee 20 minutes/on and 20 minutes/off for the first day when awake. Then apply cold as often as needed for 15 to 20 minutes at a time for the next several days. Place a towel or cloth between the skin and the ice to prevent skin injury.
- You may shower and get your incision wet. Do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
- Take an aspirin each morning for 14 days unless there is a medical contraindication to do so (such as a history of ulcers or aspirin allergy), or you are taking other blood thinners.
- You can elect to wear an elastic stocking (TED) below the knee to prevent leg swelling, and do at least 10 ankle pump exercises each hour to control swelling and to help prevent phlebitis (blood clots in the veins).
OFFICE VISIT
Please return to your Surgeon approximately 10-14 days after your surgery. At this time, your progress will be checked.
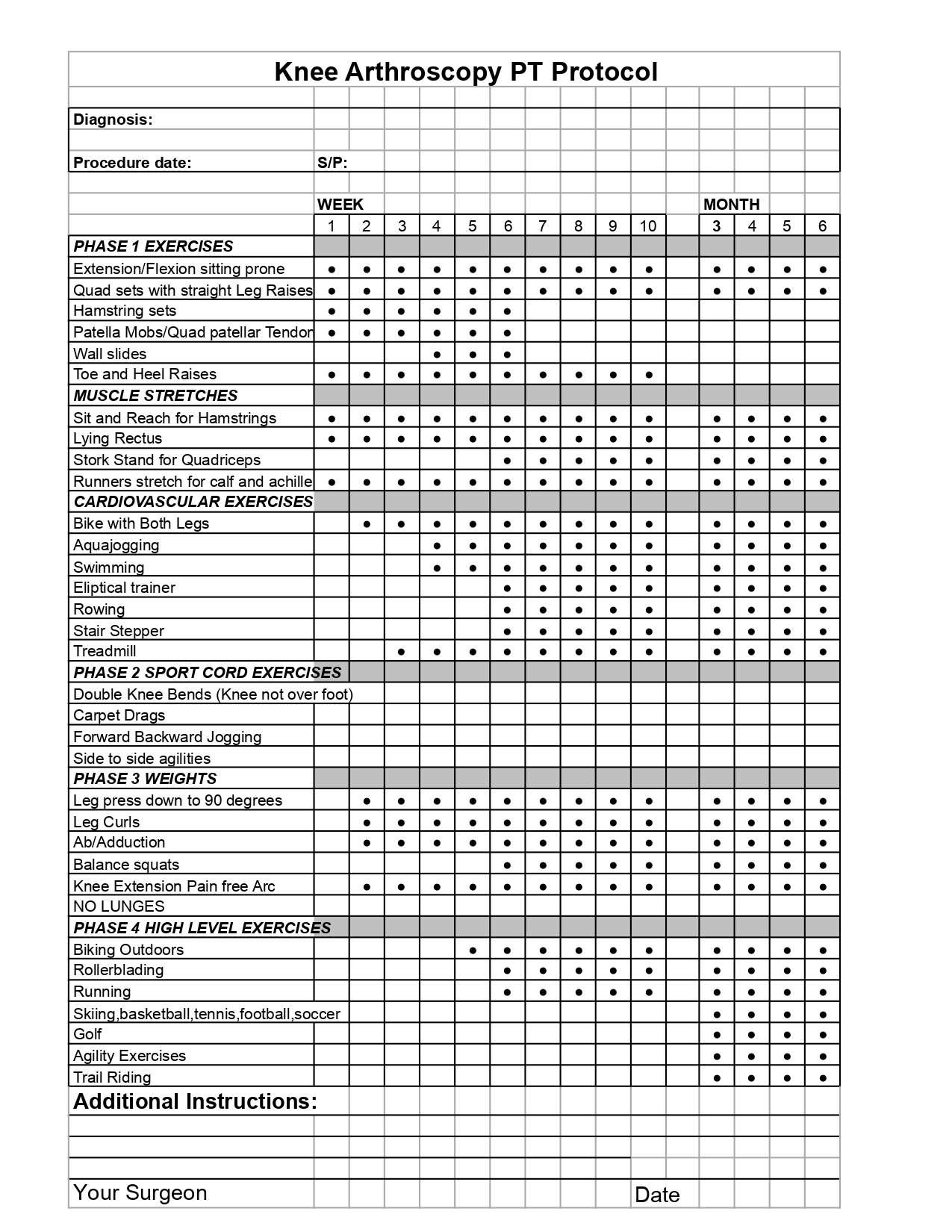
Sports Conditioning for the Knee
A guide to conditioning and knee injury prevention
This program has been developed to provide a comprehensive guide to the conditioning of the knee for sports participation. Following a specific program of exercises for the knee, on a year round basis, will help to reduce the risk of injury to the knee joint.
Since 2/3 of knee injuries in sports are non-contact in nature, most knee injuries occur as a result of situations where there is a sudden knee imbalance caused by cutting, turning, twisting, stopping, jumping, landing from a jump or other high-speed, high-force athletic maneuver.
An effective knee-conditioning program should be focused on providing exercises and drills to develop coordination, balance, strength, speed, power and quick reactions in the knee and knee joint muscles. In addition to the development of strength in the knee muscles, drills to enhance and train controlled knee joint actions at high speed and force need to be specifically trained for the mechanics of cutting, turning and stopping, as well as jumping, landing and run/jump transitions.
Five components of the knee training program:
- Warm-up
- Flexibility and stretching
- Strength training
- Speed/ Agility training
- Jump/ Plyometric training
Keys to success in training:
- Focused effort and concentration when training
- Always use proper form and technique
- Quality workouts on a consistent basis
- Avoid over-training
Warm-up and Stretch
- Always be sure that you warm-up well and stretch lightly before workouts, and stretch well again after workouts.
- Generally, you should do some walking, cycling, jump-rope or jogging before starting the exercise program.
- You should warm-up until you break a sweat to assure that your whole body is ready to exercise.
- You should then stretch before beginning the exercise program.
- Always allow time to stretch during the cool-down period after finishing the exercise program.
- 3 to 5 repetitions of each stretching exercise should be done, statically holding the stretch for 15 to 20 seconds.
- There should be no bouncing or oscillations of the body during stretching exercises.
- You should slowly assume the stretching position until a comfortable feeling of stretch is felt in the muscle and then held, without further movement, for the 15 to 20 second period.
- Stretching should NOT BE PAINFUL or cause soreness after being done.
- Stretching exercises for the knee and lower body are illustrated and described in the back of the guide.
Strength Training
- Strength training should generally be done 2 to 3 times per week, on an every other day basis, in order to realize progressive strength gains.
- Off- Season strength programs, which are followed when the sport that you play is not in session should be done 2 to 3 times per week.
- During the In-Season period, when you are regularly playing your sport, strength training should continue 1 to 2 times per week.
- During the off-season you should try to maintain the weights or resistance being used when the maintenance regime is begun.
- The weights used in the maintenance regime remain the same for each workout and should not be increased (sometimes weights need to be adjusted lower due to injury or fatigue).
- The goal of the maintenance regime is to use the same weight each workout, to prevent strength loss of the strength gained during a previous strength improvement program.
Precautions when strength training:
- Avoid pain at the patellar tendon
- Avoid pain and/or crepitus (grinding) at the patella (kneecap)
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Be consistent and regular with the exercise schedule
Before Staring Your Workout
- Warm-up prior to exercising by stationary cycling, elliptical machine, jogging or jump rope for 15 to 20 minutes. You are “warmed –up” when you have started sweating
- Gently stretch all muscle groups next (see attachment for recommended stretches)
- Do exercises involving multiple muscle groups first and individual muscle groups last.
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
Progressive Resistance Exercise (PRE) Principle
- To build muscle strength and size, the amount of resistance used must be gradually increased.
- The exercises should be specific to the target muscles
- The amount of resistance should be measurable and gradually increased over a longer period of time
- To avoid excess overload and injury, the weight or resistance must be gradually increased in increments of 5 to 10 %
- Resistance can be increased gradually every 10 to 14 days when following a regular and consistent program
- Adequate rest and muscle recovery between workout is necessary to maximize the benefit of the exercise
- If the PRE principle is followed too strictly, the weights potentially will go higher and higher.
- At a certain point, the joints and muscles will become overloaded and injury will occur.
- This eventuality can be avoided by refraining from using excessive weight during strength training.
Repetition-Maximum Principle
Knowing when to increase the weight you are using in a strength-training program is based upon the ‘repetition-maximum ‘(RM) principle.
For example, a 10 RM for the leg press exercise is the amount of weight that can be lifted "just 10 times", and No More, before fatigue or failure sets in. That is, the particular weight being lifted is so heavy that an 11th repetition is not possible.
In a typical strength improvement program, the workout might look like this:
Exercise
Leg press
Intensity
10 RM
10 RM Weight
Determined by trial = 100 pounds
Workout Sets
- Set 1 – 1/2 10 RM (50 lb.) – 10 repetitions
- Set 2 – 3/4 10 RM (75 lb.) – 10 repetitions
- Set 3 – 10 RM (100 lb.) – up to 10 repetitions
- Set 4 – 10 RM
- Set 5 – 10 RM
- If 10 repetitions of 100 lb is achieved on the third set, then the 10 RM can be raised by 5 lb for the next set/exercise session.
- If 10 repetitions are not achieved on the third set, then the 10 RM weight remains the same (100 lb) for the next workout or any subsequent sets.
- If you reached the 10 RM on the third set, and wished to do a 4th and 5th set, then the weight can be raised to the new 10 RM.
- If you did not reach the 10 RM on the 3rd set, then the 4th and 5th sets would remain at the original 10 RM.
- The 1/2 and 3/4 RM set should always be done to gradually ramp-up the weight to the 10 RM set(s).
- The 3rd, 4th and 5th sets are considered the ‘working sets’.
- The number of repetitions you choose for your RM will depend upon the goals of your strength training program:
- 15 to 20 RM – Builds muscle size and definition
- 8 to 10 RM – Builds muscle size and force capability (pure strength)
- 3 to 5 RM – Builds maximal force capability, minimal size gains (high power)
Basic Knee Strengthening Program
- Frequency: 3 Times per week
- Sets: 3 to 5
- Repetitions per set: 15
- Emphasis is to build muscle strength using BOTH legs
- Progress according to the PRE and RM principles
Basic Program Exercises - see illustrations at the back of the handout.
- Leg Press
- Hamstring Curl
- Knee extension machine (short-arc 30 degrees)
- Roman Chair
- Partial Squat (hold dumbbells or barbell for resistance)
- Calf Raises
- Hip Abductor/Adductor machine (or hip pulleys or multi-hip machine)
- Hip flexor pulls
- Step Up/Down on 9 inch step (see below for progression)
The step-up exercise is the first drill to provide training for single-leg strength and balance. After you are able to perform the step-up exercise for 3 sets of 15 repetitions, without holding anything for balance, you can progress to the following advanced program.
If you have difficulty performing the step-up exercise, use the following progression as a guide:
- Start with a step of 3 inches in height
- Start with 3 sets of 5 repetitions
- Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks)
- If pain free, progress to a step of 6 inches in height
- Repeat progression starting with 3 sets of 5 repetitions
- Add one repetition per set until you can do 3 set of 10 (about 2 weeks)
- If pain free, progress to a step of 9 inches in height (the height of a standard stair)
- Repeat process of progression from 3 sets of 5, to 3 sets of 10 (about 2 weeks)
Advanced Knee Strengthening Program
- Frequency: 3 Times per week
- Sets: 3
- Repetitions per set: 10
- Emphasis is to continue to build muscle strength using both legs and progress to Advanced Exercises using the Single leg.
- Advanced Single leg exercises are integrated with the exercises from the Basic Knee Strengthening Program.
Single Leg Drills (Rotating Basis)
- Single Leg Wall Slide
- Single Leg Squat (see below for single leg drills)
Advanced Program Exercises
- Leg Press
- Hamstring Curl
- Knee extension machine (short-arc 30 degrees)
- Roman Chair
- Chair Squat (with barbell or hold dumbbells for resistance)
- Calf Raises
- Hip Abductor/Adductor machine (or hip pulleys or multi-hip machine)
- Hip flexor pulls
- Step up/down (hold dumbbells for resistance with balance)
- Alternate workouts with single leg wall slide and single leg squat
- When starting the new single leg drills, start with 3 sets of 5, and add one repetition per set, per workout until you can do 3 sets of 10.
- When you can do 3 sets of 10 without holding anything for balance, then you can hold dumbbells to increase resistance and strength on all single-leg drills.
Instructions for Single Leg Exercises
Step Up-Down Exercise
Standing sideways to a step or stool, place the foot of the single limb on a step or stool. Standing on the single-leg, maintain balance if necessary, by lightly holding onto something. Keeping an upright posture and bending only at the knee and controlling with the quadriceps muscle, slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and repeat the step up motion, maintaining constant muscle activity in the quadriceps. Keep the back straight and do not let your hips go backward.
Single Leg Wall Slide Exercise
Stand on the single leg with your back and buttocks touching a wall. Place the foot about 6 inches from the wall. While maintaining balance, slowly lower your body by bending the knee and slide down the wall until the knee is flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position. Keep the hips level and be sure you are using your knee muscles to perform the exercise.
Single Leg Squat Exercise
In the single leg squat exercise, while maintaining balance, you stand on the single leg and then lower your buttocks toward a chair or bench. Slowly return to the standing and starting position. As you begin the squatting motion, keep your head over your feet and bend at the waist and hips as you descend. You do not have to squat all the way to the chair or bench, instead, try to stay in a comfortable range of motion where there is no knee pain or excessive strain. As you gain strength, try to do the exercise without holding on to anything, and eventually, balancing while holding dumbbells.
Some Final Precautions
When using the leg extension machine (quadriceps extensions), limit the lifting of the weight through the upper 30 degrees and hold for 5 seconds with the knee fully straight (see illustration in back of guide).
Due to their potential to cause knee injury, the following exercises are not recommended:
- Stairmaster or stair climber machines
- Lunges with weights
- Squats past 90 degrees of knee flexion
- High impact exercises
Speed / Agility Training
Goals:
- Safely condition the knee and lower limb for the demands of sports activity.
- Provide a logical sequence of progressive drills for pre-sports conditioning.
- Provide objective criteria for safe progression from training to sports participation.
Sports Specific Speed and Agility Training
Phases of Training
- Straight-ahead running phase
- Direction change running phase
- Unrestricted direction change
Warm-up and Stretch
Generally, you should cycle, jog, jump rope or use an elliptical trainer, rower or other device for 15 to 20 minutes so that you break a sweat before starting the running program.
You should then stretch before beginning the running drills.
After completing the running drills, cool down by stretching for 15 to 20 minutes.
The Criteria to Progress
Do not progress to the next step in the progression until the present step is pain free, without any difficulty (muscle soreness, joint pain or fatigue).
Frequency
2 times per week.
Notes
Each ‘step’ is considered one workout.
The program adds the steps together as you progress through the outlined sequence. Repeats should not be skipped to avoid overuse injuries due to too rapid progression.
Phase 1 Straight Ahead Running
- STEP 1 Run 1/2 speed 100 yards, 10 repetitions
- 2 Repeat previous step
- 3 Run 3/4 speed 100 yards, 10 repetitions
- 4 Repeat previous step
- 5 Run 1/2 speed, 100 yards, 3 repetitions; Run 3/4 speed, 100 yards, 3 repetitions; Run full-speed, 50 yards, 4 repetitions
- 6–10 Continue workout from Step 5, adding one 50 yard run each workout until you can do (10) 50 yard full speed runs.
Phase 2 Basic Direction Change Running
- STEP 11 100 yard run 1/2 speed, 3 repetitions; 3/4 speed, 3 repetitions; full speed, 3 repetitions. Start zig-zag run, round corners, 50 yards, 5 repetitions, 1/2 to 3/4 speed.
- 12 Repeat previous step
- 13 Repeat previous step, add backward run 25 yards to gradual stop, then forward run 25 yards to gradual stop, 5 repetitions, 1/2 to 3/4 speed.
- 14 Repeat previous step
- 15 Repeat previous step, add circle run, 20 foot or greater diameter circle, 3 repetitions to left and 3 repetitions to right, 1/2 to 3/4 speed.
- 16 Repeat previous step
- 17 Repeat previous step, add figure of eight run, 20 foot or greater length, 5 repetitions, 1/2 to 3/4 speed.
- 18 Carioca, 50 yards, 5 repetitions left, 5 repetitions right, 1/2 to 3/4 speed.
Phase 3 Unrestricted Direction Change Running
Current Workout
- 100 yd 1/2 speed, 3/4 speed and full speed each distance, 2 repetitions
- Zig-zag run, 5 repetitions
- Forward backward run, 5 repetitions
- Circle run, 6 repetitions
- Figure 8 runs, 5 repetitions
- Carioca, 5 repetitions each way
Progression
- STEP 19–24 Continue current workout increasing all drills to full speed.
- STEP 25 Continue current workout and add at 3/4 speed: Shuttle run, 50 yards, direction change every 10 yards, 5 repetitions, alternate hand touching.
- 26 Repeat previous step
- 27 Repeat previous step
- 28 Repeat previous step and add Box drill, 20 yards square, 6 repetitions, alternate starting side.
- 29 Repeat previous step
- 30 Repeat previous step
- 31 Repeat previous step and add agility run, 5 repetitions, alternate starting side.
- 32 Repeat previous step
- 33 Repeat previous step
- 34–39 Repeat previous step working all drills full speed.
Final Workout
- 100 yd 1/2 speed, 3/4 speed and full speed each distance, 2 repetitions
- Zig-zag run, 6 repetitions
- Forward backward run, 6 repetitions
- Circle run, 6 repetitions
- Figure ‘8’ runs, 6 repetitions
- Carioca, 6 repetitions each way
- Shuttle run, 50 yards, direction change every 10 yards, 6 repetitions, alternate hands touching
- Box drill, 20 yards square, 6 repetitions, alternate starting side
- Agility run, 6 repetitions, alternate starting side
When practicing the final workout, for each drill, do the first 2 repetitions at 1/2 speed, 2 repetitions at 3/4 speed and the last 2 repetitions at full speed.
Jump / Plyometric Training
Goals:
- Safely condition the knee and lower limb for the demands of jumping and landing during sports activity.
- Provide a logical sequence of progressive drills for pre-sports conditioning.
- Provide objective criteria for safe progression from training to jumping-sports participation.
Sports Specific Jump / Plyometric Training
Phases of Training
- Double-leg training
- Double-leg complex training
- Single-leg training
Warm-up and Stretch
Generally, you should cycle, jog or use an elliptical trainer, rower or other device for 15 to 20 minutes so that you break a sweat before starting the running program.
You should then stretch before beginning the jumping drills.
Jump Rope Warm-up Routine
- Jump rope 50 turns, double-leg hops
- Jump rope 50 turns, alternating single-hops, 2 sets
- Jump rope 50 turns, double single leg hops, alternating
- Jump rope 50 turns, double single leg hops, alternating, followed by 3 double leg hops
After completing the jumping drills, cool down by stretching for 15 to 20 minutes.
The Criteria to Progress
Do not progress to the next step in the progression until the present step is pain free, without any difficulty (muscle soreness or fatigue).
Frequency
2 times per week.
Notes
Each ‘step’ is considered one workout.
The program adds the steps together as you progress through the outlined sequence. Repeats should not be skipped to avoid overuse injuries due to too rapid progression.
Technical Essentials
Each hop or jump should be performed with concentration on good technique. Each jump landing should be a ‘stick’ landing, i.e. you should land and hold balance momentarily before proceeding to the next jump. Keep the feet apart and do not let the knees move or rotate inward when taking off and especially landing.
Phase 1 – Double-Leg Training
- STEP 1 Power skip, warm-up, 100 feet distance, 5 reps.
- Double leg, hop-hop-stick, 5 reps.
- Wall jumps, 10 reps.
- 2. Repeat previous step
Phase 2
- 3. Add Triple-broad-Vertical jumps, 5 reps. 180 degree jumps, 5 reps.
- 4. Repeat previous step
- 5. Add Triple broad jump to Vertical jump to 180 degree jump, 5 reps.
- Forward-Backward jumps (over 6” hurdle), 5 reps each way.
- Side-to-Side jumps (over 6” hurdle), 5 reps each way.
- 6. Repeat previous step
Phase 3
- 7. Add Single-leg Forward Hopping, 3 hops then stick, 5 reps each leg.
- 8. Repeat previous step
- 9. Add Single-leg Forward-Backward hopping (over 6” hurdle), 5 times each leg.
- 10. Repeat previous step
- 11. Add Single-leg Side-Side hopping (over 6” hurdle), 5 times each leg.
Final Workout
- Power skip, warm-up, 100 feet distance, 5 reps.
- Double leg, hop-hop-stick, 5 reps.
- Wall jumps, 10 reps.
- Triple-broad-Vertical jumps, 5 reps.
- 180 degree jumps, 5 reps.
- Triple broad jump to Vertical jump to 180 degree jump, 5 reps.
- Forward-Backward jumps (over 6” hurdle), 5 reps each way.
- Side-to-Side jumps (over 6” hurdle), 5 reps each way.
- Single-leg Forward Hopping, 3 hops then stick, 5 reps each leg.
- Single-leg Forward-Backward hopping (over 6” hurdle), 5 times each leg.
- Single-leg Side-Side hopping (over 6” hurdle), 5 times each leg.
Looking at the Whole Training Program
- The following is suggested schedule of off-season workouts incorporating the strength, speed/agility and jump/plyometric programs.
- The workout-week is 7 days.
- The workout weeks are recycled every 5 weeks.
- Aerobic workouts can be done on training days, after strength, speed or jump training.
- To allow adequate rest and recovery from workouts, rest days should be observed.
- Rest days can be active, participating in non-athletic activities and stretching, but avoiding exercise intensities that would require further rest and recovery.
Workout Week 1
- Day 1 – Strength training
- Day 2 – Speed/Agility training
- Day 3 – Rest day
- Day 4 – Strength training
- Day 5 – Jump/Plyometric training
- Day 6 – Rest day
- Day 7 – Strength training
Workout Week 2
- Day 1 – Speed/Agility training
- Day 2 – Rest day
- Day 3 – Strength training
- Day 4 – Jump/Plyometric training
- Day 5 – Rest day
- Day 6 – Speed/Agility training
- Day 7 – Strength training
Workout Week 3
- Day 1 – Rest day
- Day 2 – Jump/Plyometric training
- Day 3 – Strength training
- Day 4 – Speed/Agility training
- Day 5 – Rest day
- Day 6 – Jump/Plyometric training
- Day 7 – Strength training
Workout Week 4
- Day 1 – Speed/Agility
- Day 2 – Rest day
- Day 3 – Strength training
- Day 4 – Jump/Plyometric training
- Day 5 – Speed/Agility training
- Day 6 – Strength training
- Day 7 – Rest day
Workout Week 5
- Day 1 – Rest day
- Day 2 – Rest day
- Day 3 – Strength training
- Day 4 – Speed/Agility training
- Day 5 – Strength training
- Day 6 – Rest day
- Day 7 – Jump/Plyometric training
In-Season Conditioning
Warm-up and Stretch
Always continue the advice on warm-up and stretching before and after practice and games.
Strength Training
- Frequency: Ideally 2 times a week (one time a week better than none)
- Intensity: 85 to 95 % of your 10 RM weights achieved during the off-season. Weights will vary due to fatigue, injury or illness.
- Sets: 2 to 3
- Repetitions: 6 to 8
- When: After practice or on an off day
Speed/Agility and Jump/Plyometric Training
The exercises and drills that comprise the speed and jump training programs can be easily incorporated into pre-practice warm-up and in-practice conditioning routines.
The Medial Collateral Ligament (MCL) of the Knee
Activities and Exercises After Injury to the Medial Collateral Ligament (MCL) of the Knee
PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1)
The knee should be to be protected with a hinged brace for 3 to 6 weeks, depending upon the severity of the injury. Crutches and restricted weight bearing may be needed, as instructed by your Surgeon. Apply ice and elevate the leg to control swelling. As the pain lessens and the swelling decreases, try to gradually regain knee motion. Avoid pivoting or twisting the knee because it might be unstable and give out. Be careful getting out of cars, or catching your toe on a rug. When walking, bear weight according to Dr. Gill's instructions. Progress to no crutch(es) or brace when you can walk without a limp and there is no pain (per doctor instructions). Ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury. Ice for 20 minutes, three times a day. At about two or three weeks following injury, the pain is usually subsiding and the swelling is lessened. You can now try to stretch the knee to regain motion. Stationary cycle, swimming (flutter kick only) and the following exercise program are recommended.
STATIONARY BICYCLE
Times per week: 5-7 Duration: 30 minutes 1-2 times a day
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 20 to 30 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then ride the bicycle with your forefoot resting on the pedal.
Range of Motion and Strengthening Exercises (brace off)
Days per Week: 5-7
Times per Day: 1-2
| Quadriceps sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Heel slides with towel assist | 1 set of 15 reps |
| Straight leg raises | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing Hamstring Curl | 3 sets of 10 reps |
| Standing toe raises | 3 sets of 10 reps |
| Hip Abduction | 3 sets of 10 reps |
| 1/4 Squats | 3 sets of 15 reps |
| Wall slides | 3 sets of 15 reps |
Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lax-y-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 15 repetitions.
Heel Prop- Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
Heel slides- While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for five seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise. Continue this exercise until you can fully bend your knee equal to the uninjured side. Also, as you start to gain flexion, you can assist your efforts to gain flexion by assisting the heel slide with a towel. Repeat 20 times, three times a day.
Straight Leg Raise- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 10-15 pounds.
Short Arc Knee Extension- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Add weight just like #1 until the goal weight is reached of 10-30 pounds.
Standing Hamstring Curl- Stand facing a table, using the table for balance and support. While standing on the unaffected limb bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated.
Standing Toe Raise- Stand facing a table, hands on the table for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position.
Hip Abduction- Lie on your uninjured side. Keep the knees fully extended. Raise the operated limb upward to a 45-degree angle as illustrated. Hold one second, and then lower slowly.
1/4 Squats- Stand with your feet shoulder width apart. Toes pointing straight ahead. Look down at your feet, Lean with your butt first and squat down slowly until your knees pass over your toes then stand back up to start position. You may hold dumbbells to add resistance.
Wall Slides- Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE
PHASE 2: SIX WEEKS AFTER INJURY ONWARD (grade 2 and 3) THREE WEEKS AFTER INJURY ONWARD (grade 1)
This handout is to help you rebuild the strength of the knee muscles after injury to the MCL of the knee. It is intended as a guideline to help you organize a structured approach to strengthen the knee.
Precautions When Exercising:
- Avoid pain at the patellar tendon
- Avoid pain and/or crepitus (grinding) at the patella (kneecap)
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Before Starting Your Workout:
- Warm-up prior to exercising by stationary cycling, elliptical machine or treadmill walking uphill
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next (see attachment for recommended stretches)
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
EXERCISE PROGRAM
ROM and Strengthening
Days per week: 3 Times per Day: 1
Stretching
Days per week: 5-7 Times per day: 1-2
Optional weight training
- It is ok to start slow weight training at this time using low weights and high reps, it is also advised if you have pain refrain from doing lower body weight training.
Cardiovascular
- Start to perform cardiovascular training 2 times per week for 30 minutes. Include stationary bicycle, walking, rowing, elliptical or water workout. Refrain from impact exercises.
Return to play
- Full Range of Motion
- Strength at least 80% of uninjured limb
- Thigh girth within 1/2 inch of unaffected limb
- Symmetrical quadriceps and hamstring flexibility
- Perform and pass functional tests
| Quadriceps sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Prone Hang | 5 minutes |
| Heel slides | 1 set of 15 reps |
| Straight leg raises | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing Hamstring Curl | 3 sets of 10 reps |
| Standing toe raises | 3 sets of 10 reps |
| Hip Abduction | 3 sets of 10 reps |
| Squat to Chair | 3 sets of 15 reps |
| Wall slides | 3 sets of 15 reps |
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Quadriceps stretch | 3-5 reps holding 15-30 seconds |
| Calf Stretch | 3-5 reps holding 15-30 seconds |
Functional test
Before starting the running sequence you must be able to:
- Hop forward on both legs at least 2 feet
- Hop to either side at least 1 foot
- Hop up and down on both feet 10 times
- Jog with no limp for 100 feet
Before starting unrestricted direction change and impact training you must be able to:
- Hop forward on the affected limb for at least 80% of the distance of the unaffected side.
- Hop to either side for 80% of the distance of the unaffected limb.
- Hop up and down on the operated limb 10 times with no pain.
Once these have been completed you may return to sport.
Warm-up and Stretch and Ice
Be careful to be sure that you warm-up well and stretch lightly before workouts, and stretch well again after workouts. Generally, you should do some walking, cycling or jogging so that you break a sweat before starting the running program. You should then stretch before beginning the running drills. Ice your knee for 20 minutes following workouts after stretching again as you are cooling down.
Any questions call Greater Michigan Orthopedics
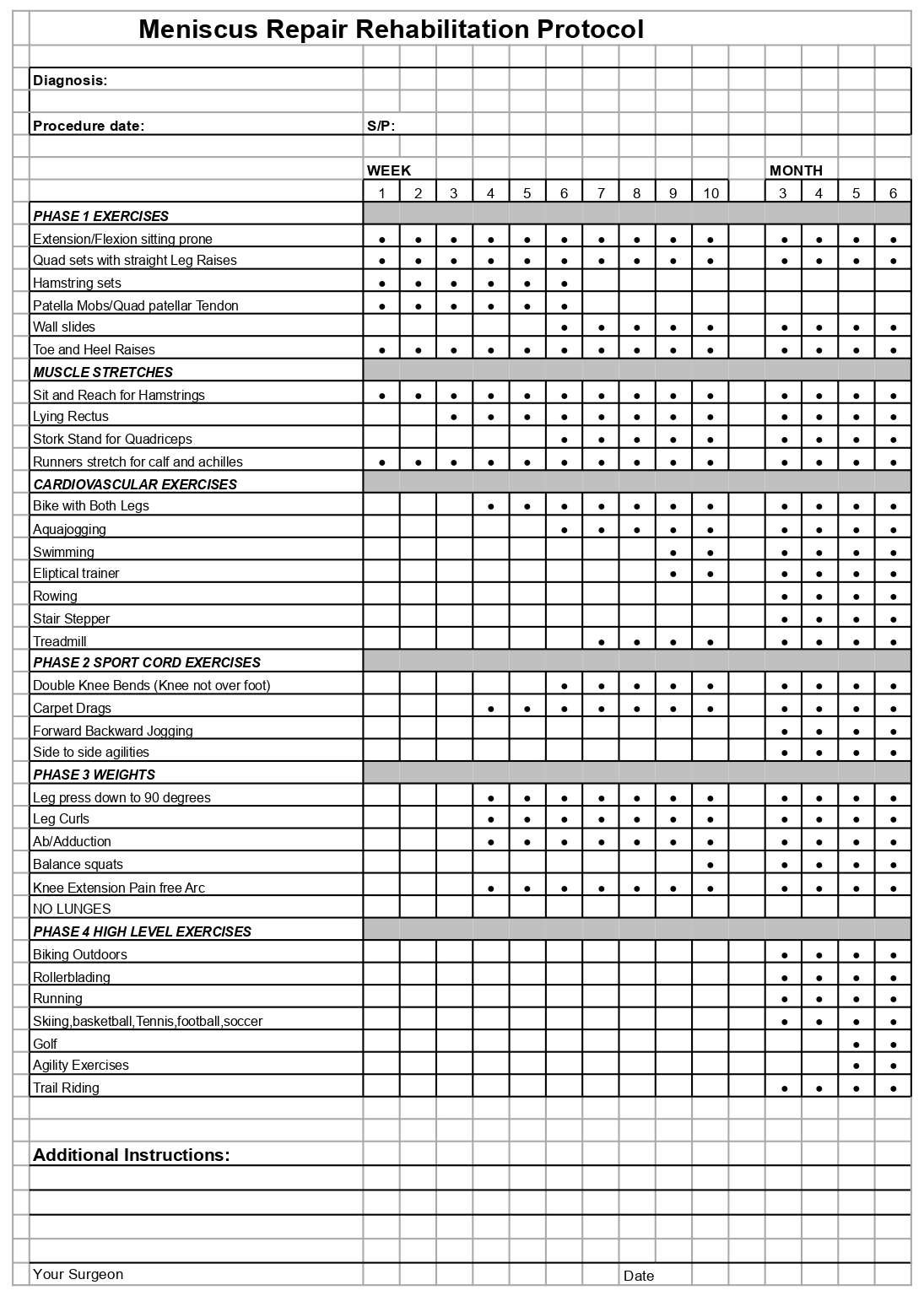
Knee Meniscus Repair
REHABILITATION AFTER KNEE MENISCUS REPAIR
Phase One: The first week after surgery
Goals:
- Control pain and swelling
- Initiate knee motion
- Activate the quadriceps muscles
Guidelines and Activities:
Knee Range of Motion:
You can fully extend (straighten the knee). To avoid placing stress on the meniscus repair, do not bend your knee beyond 90 degrees (bent to a right angle).
Brace and Crutches:
You will go home with crutches and a knee brace locked in full extension (straight).
Unless otherwise instructed by your Surgeon, use crutches when walking and bear weight as tolerated on the operated leg. That is, you can bear as much weight as you can, even full weight, as long as there is no knee pain when you put your weight on the limb. Wear the post-operative brace for walking. Lock the brace when walking to protect the knee in case of a fall. You can unlock the brace to sit or move the knee when not walking. When walking with the crutches, follow the instructions below:
Walking (weight bearing as tolerated):
- Put the crutches forward about one step's length.
- Put the injured leg forward; level with the crutch tips.
- Touch the foot of the involved leg to the floor and bear weight as tolerated.
- While bearing weight (on the crutches if there is pain in the knee) on the involved leg, take a step through with the uninjured leg.
Exercise Program:
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles and straighten the knee.
Lie or sit with the knee extended fully straight as in figure. Tighten and hold the front thigh muscle making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscle. The tightening action of the quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold 5 seconds for each contraction. Do 20 repetitions three times a day.
HEEL PROP- to straighten (extend) the knee.
Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
SITTING HEEL SLIDES - to regain the bend (flexion of the knee).
While sitting in a chair or over the edge of your bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the unoperated leg controlling it. Allow the knee to bend but DO NOT exceed 90 degrees of bend at the knee. Hold five seconds and slowly relieve the stretch by lifting the foot upward, helping with the uninvolved leg, to the straight position (passive assist). Repeat exercise 20 times, three times a day.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to Dr. Nelson's office approximately 10-14 days after your surgery.
Rehabilitation after knee meniscus repair
Phase Two: 2 to 6 weeks after surgery
Goals:
- Protect the knee from overstress and allow healing
- Regain knee motion, limiting knee flexion to 90 degrees
- Begin muscle strengthening
Knee Range of Motion:
You can fully extend (straighten the knee). To avoid placing stress on the meniscus repair, do not bend your knee beyond 90 degrees (bent to a right angle).
Brace and Crutches:
Unless otherwise instructed by Dr. Nelson, use crutches when walking and bear weight as tolerated on the operated leg. Wear the post-operative brace for walking. Lock the brace with the knee fully straight when walking to protect the knee in case of a fall. You can unlock the brace to sit or move the knee when not walking.
Exercise Program
Days per week: 5-7 Times per day: 1
| Quadriceps sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Seated Heel slides | 1 set of 15 reps |
| Straight leg raises | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing toe raises | 3 sets of 10 reps |
| Hip Abduction | 3 sets of 10 reps |
| Wall slides | 3 sets of 15 reps |
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles and straighten the knee.
Lie on your back with the knee extended fully straight. Tighten and hold the front thigh muscle making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscle. The tightening action of the quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold 5 seconds for each contraction.
HEEL PROP - to straighten (extend) the knee.
Lie on your back with a rolled up towel under your heel or sit in a chair with the heel stool as shown in. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. While maintaining this extended position, practice quadriceps setting.
SITTING HEEL SLIDES - to regain the bend (flexion of the knee). See figure in phase 1.
While sitting in a chair or over the edge of your bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the nonoperative leg controlling, allowing the knee to bend but DO NOT exceed 90 degrees of bend at the knee. Hold five seconds and slowly relieve the stretch by lifting the foot upward, helping with the uninvolved leg, to the straight position (passive assist).
STRAIGHT LEG LIFT
The quality of the muscle contraction in this exercise is what counts the most, not just the ability to lift the leg!
- Tighten the quadriceps (quadriceps setting) as much as you can, push the back of the knee against the floor.
- Tighten this muscle harder!
- Lift your heel 4 to 6 inches off the floor
- Tighten the quadriceps harder again.
- Lower your leg and heel back to the floor. Keep the quadriceps as tight as possible.
- Tighten this muscle harder again.
- Relax and repeat.
If the knee bends when you attempt to lift the limb off of the bed, do not do this exercise. Keep trying to do the quadriceps setting exercise until you can lift the limb without letting the knee bend.
SHORT ARC LIFT
With the knee bent over a rolled up towel or blanket of a height of 4-5 inches (the knee should be bent only 20-25 degrees), lift the foot so that the knee fully straightens. Hold the knee locked in extension for 5 seconds, then slowly lower.
HIP ABDUCTION
Lie on your unoperated side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, and then lower slowly. Repeat 20 times. If the straight leg lift, short arc lift and side leg lift can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds.
STANDING TOE RAISE
Stand facing a wall, hands on the wall for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position.
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. You will be bearing 50% of your weight (or less on the affected side) on each leg. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position. When doing a wall slide, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe, and try to keep equal weight on both feet.
Office visit
Call to schedule a 6 week follow up with your Surgeon.
Rehabilitation after knee meniscus repair
Phase Three: Six to twelve weeks after surgery
Goals:
- Begin partial weight bearing
- Regain full motion
- Regain full muscle strength
Knee Range of Motion:
You can now begin to gradually regain normal range of motion of the knee.
Brace and Crutches:
If instructed by your Surgeon, you may discontinue the brace and begin to progressively walk normally on the leg. Try to avoid limping and walk slowly but normally. Avoid squatting or pivoting on the operated knee.
Exercise Program
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds. Do the exercises daily for the first week, then decrease to every other day when using ankle weights. You may ride the stationary bicycle daily for 10 to 20 minutes (see below). Avoid using stair-stepper machines, doing deep knee bends and squats. Avoid any exercise that causes crunching, clicking or pain at the kneecap. Do not pivot or twist on the knee.
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 10 to 20 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then ride the bicycle with your forefoot resting on the pedal.
EXERCISE PROGRAM (see phase 2 for descriptions and illustrations)
Days per week 5-7 Times per day 1
| Quadriceps sets | 1-2 sets of 15-20 reps |
| Seated or supine Heel slides | 1 set of 15 reps |
| Straight leg raises | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing toe raises | 3 sets of 10 reps |
| Hip Abduction | 3 sets of 10 reps |
| Standing hamstring curl | 3 sets of 10 reps |
| Wall slides | 3 sets of 15 reps |
| Squat to Chair | 3 sets of 10 reps |
| Seated leg press | 3 sets of 20 reps |
| Step up Down | see below |
STANDING HAMSTRING CURL
Stand facing the wall, using the wall for balance and support. While standing on the unoperated limb bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position with the leg parallel to the floor for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated.
SQUAT TO CHAIR
In the chair squat exercise, you lower your buttocks toward the chair until your buttocks touch the chair. Do not sit or rest at the chair, but instead immediately and slowly return to the standing and starting position. Remember to keep your head over your feet and bend at the waist as you descend. When doing a squat, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe. After the first week, you may hold dumbbells while performing this exercise and the wall slide. Start with 3 to 5 pounds each hand. You may add 2 to 3 pounds per week until you reach 10 pounds in each hand.
SEATED LEG PRESS
If you are using a leg press machine for strengthening, use an amount of weight that feels easy enough to perform 20 repetitions as the starting weight for this exercise. Use this weight for the first week before raising the weight. The weight may be increased by about 5 pounds every 7 to 10 days thereafter, as long as you can perform 20 repetitions per set for 3 sets, and as long as the weight used does not exceed body-weight when using both legs, or 1/2 body weight when using the one leg. In this exercise, avoid letting the knees snap or drop suddenly into extension when reaching the fully straightened position. Avoid starting the exercise with the knees bent past 90 degrees. Adjust the seat position to limit the excursion of the machine.
Step Up- Down Exercise
Place the foot of the operated limb on a stool or step. Maintain balance, if necessary, by holding onto the wall or a chair (illustration). Standing sideways to the step, slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and then step up onto the stool by straightening the knee using the quadriceps muscles. Try to keep an upright posture and avoid bending forward during the exercise. When doing a step up-down, you should position your thigh so that your kneecap is in line with the tip of your shoe, or your second toe. Do 3 sets of 10 to 15 repetitions.
Progression for Step Up-Down Exercise
Start with a step of 3 inches in height. Start with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 6 inches in height. Repeat the above progression starting with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 9 inches in height (the height of a standard stair). Repeat this process of progression from 3 sets of 5, to 3 sets of 10 (about 2 weeks).
STRETCHING EXERCISES
Times per day: 1-2 Days per week: 5-7
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Quadriceps stretch | 3-5 reps holding 15-30 seconds |
| Calf Stretch | 3-5 reps holding 15-30 seconds |
OFFICE VISIT
Please set up an appointment to see your Surgeon in 8 weeks (3-4 months after surgery).
Rehabilitation after knee meniscus repair
Phase Four: Twelve weeks after surgery onward
Goals:
- Regain full muscle strength.
- Work on cardiovascular conditioning.
- Do sports-specific training.
ACTIVITIES – Muscle-Strengthening Exercises
You should continue muscle-strengthening exercises from phase 2 and 3 on a three times a week basis. At this time, you can decrease the number of repetitions per set from 15 to 10. This will allow you to work with more resistance. Remember to do all exercises slowly, with good form. Weights can be increased when you can do a particular weight easily, for 3 sets of 10 repetitions, for 3 consecutive workouts. At all times, be cautious of pain or crunching at the kneecap or patellar tendon while exercising. You may use resistance machines at your gym, DO NOT do lunging or high impact drills or exercises or drills where you pivot on the fixed foot. Also avoid doing squats or leg press where the knee is allowed to bend past 90 degrees.
Cardiovascular Conditioning
You can use Nordic track, stationary bicycle, elliptical trainer or swimming workouts to build cardiovascular fitness. Three to five times per week for 20 to 30 minutes is sufficient for improvement in this area. Please note that excessive long duration cardiovascular exercise can retard or delay muscular strength development when strength improvement and gains in muscle size are the program's primary goal.
Phase Five: 16 Weeks after surgery onward
At this time, light running on a soft level surface can begin if Dr. Nelson advises. You need to have full range of motion, good strength and no swelling to run safely. If you run, 3 times per week for 10 minutes is advisable for the first 2 weeks. If there is no pain or swelling, you can increase your running time by 1 minute per session for a maximum of 30 minutes. Walking and hiking on gentle trails can also be used for conditioning activity.
20 weeks after surgery
Speed and agility running program for Return to Sports

Meniscal Allograft Transplant
Introduction:
- This rehabilitation protocol has been developed for the patient with a meniscal allograft or collagen meniscal implant (CMI) procedure. It is extremely important to protect this patient against excessive weight bearing forces during the early postoperative period to avoid shearing or disruption of the graft tissues. Early passive range of motion is highly beneficial to enhance the cartilage and the remodeling process.
Goals:
- Control joint pain, swelling, hemarthrosis
- Regain normal knee range of motion
- Regain a normal gait pattern
- Regain normal lower extremity strength
- Regain normal proprioception, balance, and coordination
The physical therapy is to begin post-op day #3-5. It is extremely important for the supervised rehabilitation to be supplemented by a home fitness program.
Important post-op signs to monitor:
- Swelling of the knee or surrounding soft tissue
- Abnormal pain response, hypersensitive
- Abnormal gait pattern, with or without assistive device
- Limited range of motion
- Weakness in the lower extremity musculature
Return to activity:
- It requires both time and regular clinic evaluation to safely and efficiently return to functional activity.
- Adequate strength, flexibility, and endurance are all necessary to return to high level function, all of which are addressed in this program.
- Isokinetic testing and functional evaluation are required to assess a patient's readiness to return to sport.
- Return to intense activities following a meniscal transplant may increase the risk of repeat injury or the potential of compounding the original injury. Symptoms such as pain, swelling, or instability should be closely monitored by the patient.
- Typical return to sport is 9 to 12 months and modification of sport is highly recommended. This will be discussed with your Surgeon in the office and is dependent on the sport you are trying to achieve.
Phase 1: Week 1-3
Range of Motion:
- Passive, 0-90°
- Patella mobs
- Ankle pumps
- Gastoc/Soleus/Hamstring gentle stretch (no stretch if osteotomy was performed)
- Heel/Wall slides to reach goal
Strength:
- Quad sets with e-stim/biofeedback
- SLR in (flex, abd, add) as tolerated
- Multi-angle isometrics (0-60°)
- Hamstring/Gluteal isometric sets
- Knee extension (90-30°) (active assisted)
Weight Bearing:
- TDWB (for osteotomy patients)
Crutches post-op Brace:
- Bracing with 0-90° range of motion
- Removed during range of motion exercise
Modalities:
- E-stim/biofeedback as needed
- Ice 15-20 minutes
Goals for Phase 1:
- ROM 0-90°
- Adequate quad/VMO contraction
- Independent in HEP
- Control pain, inflammation, and effusion
- TDWB as noted by Dr. Nelson
Patient to make appointment with your Surgeon 10-14 days post op.
Phase 2: Week 4-12
Range of Motion:
- Passive, 0-135°
- Patella mobs
- Gastoc/Soleus/Hamstring stretch
- ITB/Quad stretch
- Heel/Wall slides to reach goal
- Prone hang to reach goal
Strength:
- Progression of isometric exercises
- SLR in 4 planes with ankle wt/tubing
- Knee extension (90-30°) with light weight
- Hamstring curl with light weight
- Leg press (0-60°)/Total Gym
- Heel raise/Toe raise
- Multi-hip in 4 directions
- Mini-squats (0-30°)
- Initiate 3-6" lateral/forward step-up/down
Balance Training:
- Weight shift (side-to-side, fwd/bkwd)
- Initiate single leg balance work
- 1/2 Foam roller work
- Wobble board work
- Sportscord balance/agility work
Weight Bearing:
- PWB to FWB with quad control
Brace:
- Bicycle when flexion is 110°
- Swimming 9 weeks
Modalities:
- Ice 15-20 minutes
Goals for Phase 2:
- PWB to FWB
- ROM 0-135°
- Control pain, inflammation, and effusion
- Increase lower extremity strength
- Enhance proprioception, balance, and coordination
Patients to return to office to see your Surgeon 6 weeks post operative. Call with any concerns.
Phase 3: Week 12-16
Range of Motion:
- Gastroc/Soleus/Hamstring stretch
- ITB/Quad stretch
Strength:
- Continue all strengthening exercises from previous phases
- Progress with all single leg activity
Balance Training:
- Advanced proprioception/balance activity
- Single leg work with plyotoss
- Dynamic balance work on advanced surfaces
Running Program:
- Initiate jump rope for endurance and impact
- Initiate running on minitramp, progress to treadmill as tolerated
Functional Training:
- Lateral movements (slide board, shuffles)
- Initiate light plyometric training
Modalities:
- Ice 15-20 minutes as needed
Goals for Phase 3:
- Maintain full range of motion
- Increase lower extremity strength and endurance
- Initiate functional activity
- Initiate sport specific activity
Phase 4: Week 16-24
Range of Motion:
- Continue with all stretching activities
Strength:
- Continue with all strengthening activities from previous phases increasing weight and repetition
Running/ Conditioning Program:
- Bicycle with resistance for endurance
- EFX/StairMaster for endurance
- Increase running program
- Increase walking program
- Swimming for endurance
- Backward running
Cutting/ Agility Program:
- Lateral shuffle/slide board
- Carioca
- Figure 8's
Functional Training:
- Advance plyometric program
- Advance sport specific drills
Modalities:
- Ice 15-20 minutes as needed
Goals for Phase 4:
- Enhance lower extremity strength and endurance
- Return to previous activity level
- Return to sport specific functional level
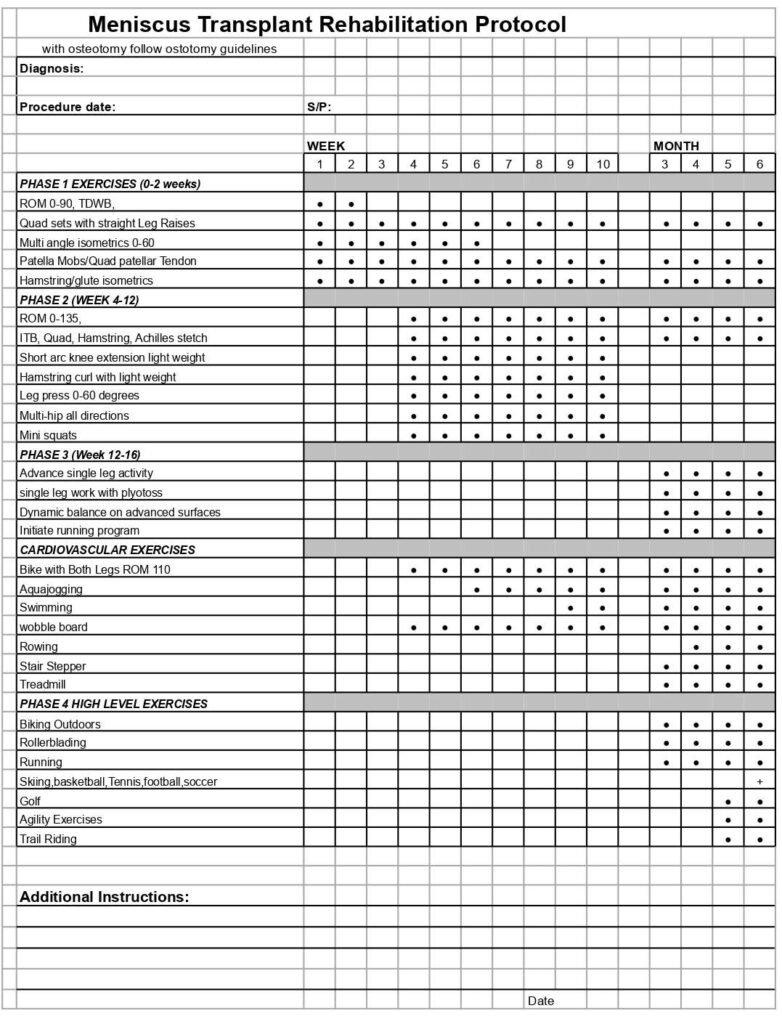
Arthroscopic Microfracture Surgery
Here are guidelines that will help you in preparing for arthroscopic microfracture surgery.
PREOPERATIVE INSTRUCTIONS WITHIN A FEW WEEKS BEFORE SURGERY:
Your Surgeon will see you in the office. He will do a preoperative history and physical examination and complete the necessary paperwork. It is recommended that you utilize a stationary cycle to maintain your knee range of motion and improve the overall function of the knee prior to surgery.
SEVERAL DAYS PRIOR TO SURGERY:
Wash the knee several times a day to get it as clean as you can. This decreases the risk of infection. Be careful not to get any scratches, cuts, sunburn, poison ivy, etc. The skin has to be in very good shape to prevent problems. You do not need to shave.
THE DAY BEFORE SURGERY:
You can have nothing to eat or drink after midnight on the day before surgery. It is very important to have a completely empty stomach prior to surgery for anesthesia safety reasons. If you have to take medication, you can do so with a sip of water early in the morning prior to surgery (but later tell the anesthesiologist you have done so).
DAY OF SURGERY:
Bring any brace, ice machine, or imaging studies that you may have received.
SURGERY:
Microfracture is a surgical procedure aimed at cartilage regeneration. The arthroscopic technique involves clearing damaged tissue from the knee joint and creating tiny holes ("microfractures") in the bone area where the cartilage is defective. The underlying bone marrow seeps out through the holes and becomes part of a blood clot that forms over the area. The marrow contains stem cells, which have the ability to form replacement cartilage between the bare-bone surfaces of the knee. Appropriate rehabilitation of the knee after surgery is critical to the success of the operation. Strict adherence to an aggressive physical therapy program following surgery all appear to enhance the success of the procedure.
AFTER SURGERY:
The dressing can be removed at two days. The wound is sealed with steri-strips (small pieces of tape on the skin). You can shower on the second day following surgery, but be careful standing in the shower so that you do not fall. It is better to have a small stool to be able to sit on. However, you can get the leg wet and wash it. Do not submerge the knee under water in a bath, hot tub or swimming pool.
If you develop calf pain or excessive swelling in the leg, call Greater Michigan Orthopedics.
Arthroscopic Microfracture Rehabilitation Protocol
PHASE 1: 0 – 2 weeks after surgery
You will go home with crutches and cryocuff cold therapy unit.
GOALS:
- Protect the cartilage transfer – avoid weight bearing if instructed to do so
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
ACTIVITIES:
1. ROM
Continue to move the leg after surgery. It is important for the gliding function of the knee to maintain smooth surfaces. You do not have to wear the brace to perform range of motion exercises. It is very important that you straighten the knee completely!
2. CRUTCHES
For patellar and trochlear groove lesions, you will wear a knee brace, which is set to allow your knee to bend only 30 degrees and straighten fully. Use it when walking and put as much weight on your operated leg as possible (without pain) when walking. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you.
For femoral condyle defects, you may have a brace (0-90), but crutches and restricted weight bearing will be necessary for longer periods. Dr. Nelson will give special instructions in these cases.
3. CRYOCUFF (COLD APPLICATION)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15-20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
4. WOUND CARE
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
5. ASPIRIN / ELASTIC STOCKINGS
Avoid aspirin for the first week so that the blood can "clot" in the cartilage defect. Wear an elastic stocking (TED) below the knee, and do at least 10 ankle pump exercises each hour to help prevent phlebitis (blood clots in the veins).
6. FREE/MACHINE WEIGHTS (Upper Body/Trunk Only)
We suggest that you do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15-20 repetitions. Do not place yourself in a compromising position with your recently operated knee.
EXERCISE PROGRAM
Perform daily
| Quadriceps sets | 3 sets of 10 reps |
| Heel Prop | 5 minutes |
| Heel slides | 20 reps |
| Ankle pumps | 10 times an hour |
Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lax-y-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 10 repetitions.
HEEL PROP- to straighten (extend) the knee. Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
HEEL SLIDES - to regain the bend (flexion) of the knee. While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to your Surgeon office approximately ten to fourteen days after your surgery.
Rehabilitation after Arthroscopic Microfracture Surgery
Phase Two: 2 to 6 weeks after surgery
Goals:
- Protect the knee from over stress and allow healing
- Regain full motion
- Begin muscle strengthening
Brace and Crutches:
For patellar and trochlear groove lesions, you will wear a knee brace, which is set to allow your knee to bend only 30 degrees and straighten fully. Use it when walking and put as much weight on your operated leg as possible (without pain) when walking. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you.
Exercise Program
The following exercise program should be followed as directed by your Surgeon or the physical therapist. Do the exercises daily unless otherwise noted.
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 20 to 30 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
| Days per week | 5-7 | Times per day: | 1 |
| Quadriceps set | 3 sets of 10 reps | ||
| Heel prop | 5 minutes | ||
| Heel slides | 3 sets of 10 reps | ||
| Straight leg raise | 3 sets of 10 reps | ||
| Short arc lift | 3 sets of 10 reps | ||
| Standing hamstring curl | 3 sets of 10 reps | ||
| Standing toe raise | 3 sets of 10 reps | ||
| Hip abduction | 3 sets of 10 reps |
Straight Leg Raise- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 5-10 pounds.
Short Arc Knee Extension- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 15 repetitions. Add weight just like #1 until the goal weight is reached of 10-12 pounds.
Standing Hamstring Curl- Stand facing the wall, using the wall for balance and support. While standing on the non operative limb, bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated. Repeat 20 times.
Standing toe raise- Stand facing a wall, hands on the wall for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 times.
Hip Abduction- Lie on your non operative side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, and then lower slowly. Repeat 20 times.
OFFICE VISIT
Please make an appointment with your Surgeon at 6 weeks after surgery.
Phase three: Eight to Twelve weeks after surgery
Goals:
- Walk normally
- Regain full motion
- Regain full muscle strength
Activities:
- You may discontinue the knee brace (patellar/trochlear patients) at this time.
- Progressively bear full weight and walk on the leg. Try to avoid limping and walk slowly but normally. Start by walking with full weight and both crutches for 3 to 5 days. If pain free, then wean to one crutch on the opposite side of surgery for 3 to 5 days. Discontinue the crutch after that when you can walk normally with no pain or limp.
- Continue to ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury.
Exercise Program
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds.
You may ride the stationary bicycle daily for 10 to 20 minutes.
Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
EXERCISE PROGRAM (see phase 2 for descriptions and illustrations)
| Days per week | 5-7 | Times per day | 1 |
| Quadriceps set | 3 sets of 10 reps | ||
| Heel prop | 5 minutes | ||
| Heel slides | 3 sets of 10 reps | ||
| Straight leg raise | 3 sets of 10 reps | ||
| Short arc lift | 3 sets of 10 reps | ||
| Standing hamstring curl | 3 sets of 10 reps | ||
| Standing toe raise | 3 sets of 10 reps | ||
| Hip abduction | 3 sets of 10 reps | ||
| Wall slides | 3 sets of 10 reps |
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
OFFICE VISIT
Please make an appointment with your Surgeon at 12 weeks after surgery.
Rehabilitation after Arthroscopic Microfracture surgery
Phase four: Twelve weeks after Surgery onward
Goals:
- Regain full muscle strength
- Gradual return to full activity
Cycling
Days per week: 3-4 Times per day: 1 Duration: 30-45 minutes
Stationary or outdoor (mountain or road bikes) (Stay on flat terrain and remain on seat)
Indoors- Brace off
Outdoors- Brace ON
Stretching Exercises
Times per day: 1-2 Days per week: 5-7
Hamstring Stretch
Perform this stretch against a table or chair. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for 15 to 20 seconds and repeat 3 to 5 times.
Quadriceps Stretch
This stretch is performed on your stomach or standing. Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold 15 to 20 seconds for 3 to 5 repetitions.
Calf/Achilles Stretch
Keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for 15 to 20 seconds, 3 to 5 repetitions.
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Quadriceps stretch | 3-5 reps holding 15-30 seconds |
| Calf Stretch | 3-5 reps holding 15-30 seconds |
Exercises – Range of Motion and Strengthening Exercises
Days per Week: 3 Times per Day: 1
| Straight leg raise | 3 sets of 10 reps |
| Hip abduction | 5 minutes |
| Short arc lift | 3 sets of 10 reps |
| Squat to chair | 3 sets of 10 reps |
| Wall slides | 3 sets of 10 reps |
| Leg press | 3 sets of 10 reps |
| Hamstring curls | 3 sets of 10 reps |
| Step up down exercise | 3 sets of 10 reps |
Squat to Chair
In the chair squat exercise, you lower your buttocks toward the chair until your buttocks touch the chair. Do not sit or rest at the chair, but instead immediately and slowly return to the standing and starting position. Remember to keep your head over your feet and bend at the waist as you descend. For patellar/trochlear patients, do only a partial squat about 1/3 way to the chair. The angle at the knee should not exceed 30 degrees to avoid excess stress on the healing cartilage. Do not do this exercise if there is pain or grinding at the kneecap. After the first week, you may hold dumbbells while performing this exercise and the wall slide. Start with 3 to 5 pounds each hand. You may add 2 to 3 pounds per week until you reach 10 pounds in each hand. 3 sets of 10 to 15 repetitions.
Seated Leg Press (patellar and trochlear patient DO NOT do this exercise)
Use an amount of weight that feels easy enough to perform 20 repetitions as the starting weight for this exercise. Use this weight for the first week before raising the weight. The weight may be increased by about 5 pounds every 7 to 10 days thereafter, as long as you can perform 20 repetitions per set for 3 sets. In this exercise, avoid letting the knees snap or drop suddenly into extension when reaching the fully straightened position. Avoid starting the exercise with the knees excessively bent. Do not bend the knee so far that your calves and back of thighs touch. Adjust the seat position to limit the excursion of the machine.
Resisted Hamstring Curls
If you have access to a hamstring curl machine (illustration), you may start using it. As with the leg press, start with a reasonable weight and use that weight for the first week. You may increase the weight by 3 to 5 pounds every 10 days as long as you can perform 3 sets of 20 repetitions slowly, with good form. If you do not have access to a hamstring machine, continue doing the standing hamstring curl adding an ankle weight for resistance. Start with 3 to 5 pounds and add 1 pound per week until you build to 10 pounds for 3 sets of 15 repetitions.
Step Up- Down Exercise
Place the foot of the operated limb on a stool or step. Maintain balance, if necessary, by holding onto the wall or a chair (illustration). Standing sideways to the step, slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and then step up onto the stool by straightening the knee using the quadriceps muscles. Try to keep an upright posture and avoid bending forward during the exercise. When doing a step up-down, you should position your thigh so that your kneecap is in line with the tip of your shoe, or your second toe. Do 3 sets of 10 to 15 repetitions.
Progression for Step Up-Down Exercise
Start with a step of 3 inches in height. Start with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 6 inches in height. Repeat the above progression starting with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 9 inches in height (the height of a standard stair). Repeat this process of progression from 3 sets of 5, to 3 sets of 10 (about 2 weeks).
Additional Weight Training
Hip Abductor/Adductor machine Roman Chair Calf Raise Machine
Precautions When Exercising
- Avoid pain at the patellar tendon site
- Avoid pain and/or crepitus at the patella
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
Avoid the following exercises unless your therapist has deemed you:
- Knee extension weight lifting machine
- Running
- Jumping
- Pivoting or cutting
- Lunges
- Stairmaster
- Step exercises with impact
OFFICE VISIT
Please make an appointment to see your Surgeon in 12 weeks (6 months after surgery).
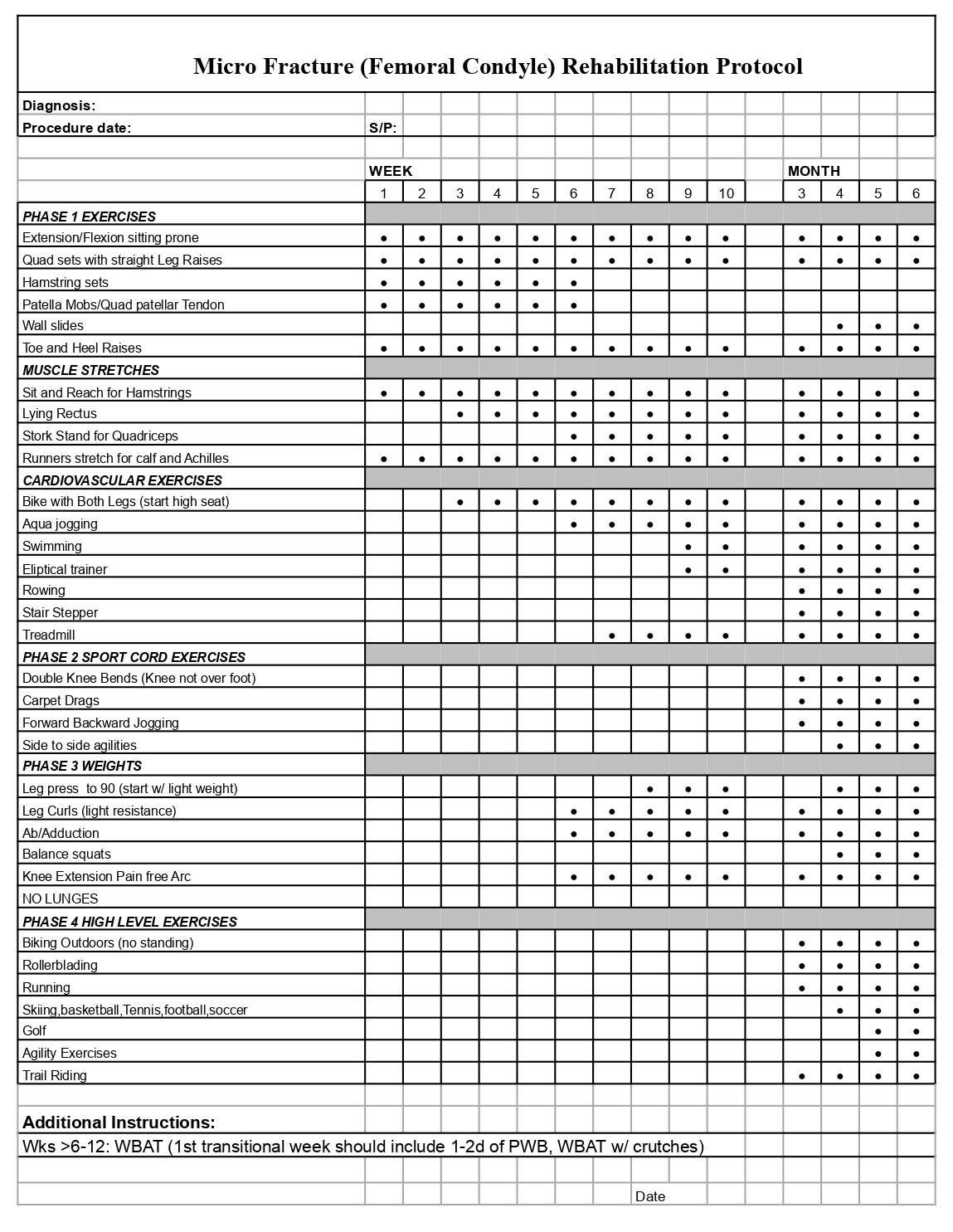
Oats Protocol
Mosaicplasty and OATS Rehabilitation Protocol
PHASE 1: 0 – 2 weeks after surgery
You will go home with crutches and possibly a cryocuff cold therapy unit.
GOALS:
- Protect the cartilage transfer – avoid weight bearing if instructed to do so
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
ACTIVITIES:
Extension (knee straight) It is very important that you straighten the knee completely!
BRACE/CRUTCHES
You will wear a knee brace, which is set to allow your knee to bend only 30 degrees for patellar and trochlear lesions and 90 for all other lesions and straighten fully. Use it when walking and put as much weight on your operated leg as possible (without pain) when walking. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you.
CRYOCUFF (COLD APPLICATION)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15-20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
WOUND CARE
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri-strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
ASPIRIN / ELASTIC STOCKINGS
Take an aspirin each morning, you may also wear an elastic stocking (TED) below the knee, and do at least 10 ankle pump exercises each hour to help prevent phlebitis (blood clots in the veins).
FREE / MACHINE WEIGHTS
Upper Body/Trunk Only
We suggest that you do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15-20 repetitions. Do not place yourself in a compromising position with your recently operated knee.
EXERCISE PROGRAM
Perform 2x daily
| Quadriceps sets | 3 sets of 10 reps |
| Heel Prop | 5 minutes |
| Heel slides | 20 reps |
| Sitting Heel Slides | 20 reps |
| Ankle pumps | 10 times an hour |
Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lazy-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 10 repetitions.
HEEL PROP- to straighten (extend) the knee. Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes. While maintaining this extended position, practice quadriceps setting.
HEEL SLIDES - to regain the bend (flexion) of the knee. While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise.
SITTING HEEL SLIDES - to regain the bend (flexion of the knee). When sitting in a chair, slide the heel backward as if trying to get the foot underneath the chair. Hold 5 seconds and slowly relieve the stretch by sliding the foot forward. You can help with the opposite foot if necessary.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to see your Surgeon approximately 10-14 after your surgery. At this time, your sutures will be removed and your progress will be checked.
Mosaicplasty and OATS Rehabilitation Protocol
Phase Two: 2 to 6 weeks after surgery
Goals:
- Protect the knee from overstress and allow healing
- Regain full motion
- Begin muscle strengthening
Brace and Crutches:
You will wear a knee brace, which is set to allow your knee to bend only 30 degrees for patellar and trochlear lesions and 90 for all other lesions and straighten fully. Use it when walking and put as much weight on your operated leg as possible (without pain) when walking. You should use the crutches in the beginning, but can discontinue the crutches when you have confidence in the knee to support you.
Exercise Program
The following exercise program should be followed as directed by your Surgeon or the physical therapist. Do the exercises daily unless otherwise noted.
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. You may ride the cycle with no resistance for 20 to 30 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
Days per week 5-7 Times per day: 1
| Quadriceps set | 3 sets of 10 reps |
| Heel prop | 5 minutes |
| Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing hamstring curl | 3 sets of 10 reps |
| Standing toe raise | 3 sets of 10 reps |
| Hip abduction | 3 sets of 10 reps |
Straight Leg Raise- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 5-10 pounds.
Short Arc Knee Extension- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 15 repetitions. Add weight just like #1 until the goal weight is reached of 10-12 pounds.
Standing Hamstring Curl- Stand facing the wall, using the wall for balance and support. While standing on the non operative limb, bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated. Repeat 20 times.
Standing toe raise- Stand facing a wall, hands on the wall for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 times.
Hip Abduction- Lie on your non operative side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, and then lower slowly. Repeat 20 times.
OFFICE VISIT
Please make an appointment with your Surgeon at 6 weeks after surgery.
Mosaicplasty and OATS Rehabilitation Protocol
Phase three: 6-12 weeks after surgery
Goals:
- Walk normally
- Regain full motion
- Regain full muscle strength
Activities:
- You may discontinue the knee brace (patellar/trochlear patients) at this time.
- Progressively bear full weight and walk on the leg. Try to avoid limping and walk slowly but normally. Start by walking with full weight and both crutches for 3 to 5 days. If pain free, then wean to one crutch on the opposite side of surgery for 3 to 5 days. Discontinue the crutch after that when you can walk normally with no pain or limp.
- Continue to ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury.
Exercise Program
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds.
You may ride the stationary bicycle daily for 10 to 20 minutes.
Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
EXERCISE PROGRAM (see phase 2 for descriptions and illustrations)
Days per week- 5-7 Times per day 1
| Quadriceps set | 3 sets of 10 reps |
| Heel prop | 5 minutes |
| Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing hamstring curl | 3 sets of 10 reps |
| Standing toe raise | 3 sets of 10 reps |
| Hip abduction | 3 sets of 10 reps |
| Wall slides | 3 sets of 10 reps |
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
OFFICE VISIT
Please make an appointment with your Surgeon at 12 weeks after surgery.
Mosaicplasty and OATS Rehabilitation Protocol
Phase four: Twelve weeks after Surgery onward
Goals:
- Regain full muscle strength
- Gradual return to full activity
Cycling
Days per week: 3-4 Times per day: 1 Duration 30-45 minutes
Stationary or outdoor (mountain or road bikes) (Stay on flat terrain and remain on seat)
Indoors- Brace off
Outdoors- Brace ON
Stretching Exercises
Times per day: 1-2 Days per week: 5-7
Hamstring Stretch
Perform this stretch against a table or chair. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for 15 to 20 seconds and repeat 3 to 5 times.
Quadriceps Stretch
This stretch is performed on your stomach or standing. Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold 15 to 20 seconds for 3 to 5 repetitions.
Calf/Achilles Stretch
Keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for 15 to 20 seconds, 3 to 5 repetitions.
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Quadriceps stretch | 3-5 reps holding 15-30 seconds |
| Calf Stretch | 3-5 reps holding 15-30 seconds |
Exercises
Range of Motion and Strengthening Exercises
Days per Week: 3 Times per Day: 1
| Straight leg raise | 3 sets of 10 reps |
| Hip abduction | 5 minutes |
| Short arc lift | 3 sets of 10 reps |
| Squat to chair | 3 sets of 10 reps |
| Wall slides | 3 sets of 10 reps |
| Leg press | 3 sets of 10 reps |
| Hamstring curls | 3 sets of 10 reps |
| Step up down exercise | 3 sets of 10 reps |
Squat to Chair
In the chair squat exercise, you lower your buttocks toward the chair until your buttocks touch the chair. Do not sit or rest at the chair, but instead immediately and slowly return to the standing and starting position. Remember to keep your head over your feet and bend at the waist as you descend. For patellar/trochlear patients, do only a partial squat about 1/3 way to the chair. The angle at the knee should not exceed 30 degrees to avoid excess stress on the healing cartilage. Do not do this exercise if there is pain or grinding at the kneecap. After the first week, you may hold dumbbells while performing this exercise and the wall slide. Start with 3 to 5 pounds each hand. You may add 2 to 3 pounds per week until you reach 10 pounds in each hand. 3 sets of 10 to 15 repetitions.
Seated Leg Press (patellar and trochlear patient DO NOT do this exercise)
Use an amount of weight that feels easy enough to perform 20 repetitions as the starting weight for this exercise. Use this weight for the first week before raising the weight. The weight may be increased by about 5 pounds every 7 to 10 days thereafter, as long as you can perform 20 repetitions per set for 3 sets. In this exercise, avoid letting the knees snap or drop suddenly into extension when reaching the fully straightened position. Avoid starting the exercise with the knees excessively bent. Do not bend the knee so far that your calves and back of thighs touch. Adjust the seat position to limit the excursion of the machine.
Resisted Hamstring Curls
If you have access to a hamstring curl machine (illustration), you may start using it. As with the leg press, start with a reasonable weight and use that weight for the first week. You may increase the weight by 3 to 5 pounds every 10 days as long as you can perform 3 sets of 20 repetitions slowly, with good form. If you do not have access to a hamstring machine, continue doing the standing hamstring curl adding an ankle weight for resistance. Start with 3 to 5 pounds and add 1 pound per week until you build to 10 pounds for 3 sets of 15 repetitions.
Step Up- Down Exercise
Place the foot of the operated limb on a stool or step. Maintain balance, if necessary, by holding onto the wall or a chair (illustration). Standing sideways to the step, slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and then step up onto the stool by straightening the knee using the quadriceps muscles. Try to keep an upright posture and avoid bending forward during the exercise. When doing a step up-down, you should position your thigh so that your kneecap is in line with the tip of your shoe, or your second toe. Do 3 sets of 10 to 15 repetitions.
Progression for Step Up-Down Exercise
Start with a step of 3 inches in height. Start with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 6 inches in height. Repeat the above progression starting with 3 sets of 5 repetitions. Add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 9 inches in height (the height of a standard stair). Repeat this process of progression from 3 sets of 5, to 3 sets of 10 (about 2 weeks).
Additional Weight Training
Hip Abductor/Adductor machine Roman Chair Calf Raise Machine
Precautions When Exercising
- Avoid pain at the patellar tendon site
- Avoid pain and/or crepitus at the patella
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
Avoid the following exercises:
- Knee extension weight lifting machine
- Running
- Jumping
- Pivoting or cutting
- Lunges
- Stairmaster
- Step exercises with impact
OFFICE VISIT
Please make an appointment to see your Surgeon in 12 weeks (6 months after surgery).
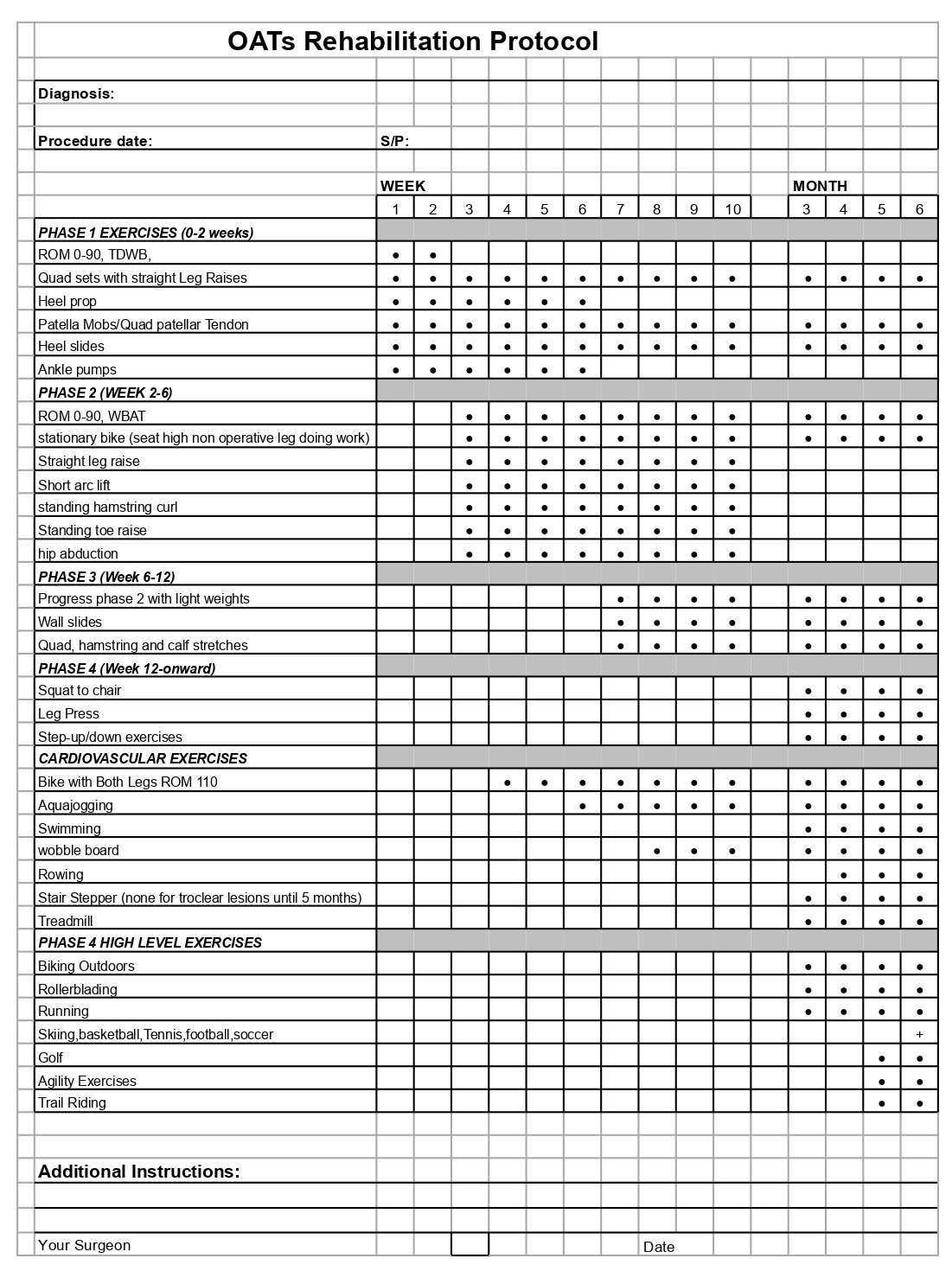
Osteochrondritis dissecans
Osteochrondritis dissecans (aka "OCD")
OCD is a relatively rare problem, likely affecting far less than 1 percent of the population, in which the bone that supports the cartilage inside a joint undergoes softening. This softening is caused by an interruption in the blood flow to that portion of bone. Over time, if left untreated, this can lead to damage to the overlying cartilage of the joint. Loose pieces of bone and cartilage can even break off into joint. Long term ramifications may even include arthritis.
Etiology/ Pathoanatomy
The causes of OCD are unknown, however repetitive trauma, inflammation, accessory centers of ossification, ischemia, and genetic factors show causative correlation. Some familial tendencies exist, but non-familial OCD is most prevalent. Repetitive trauma caused by year round sports, early sports specialization, multiple sports in a singe season or multiple teams in a single sport and increased training intensity are some of the causative factor associated with OCD. Chronic repetitive microtrauma has been suggested to lead to a stress reaction within the subchondral bone and in more severe cases subchondral bone necrosis where fragment dissection and separation may ensue.
Evaluation
Patients with OCD of knee initially have nonspecific complaints, with anterior knee pain and variable amounts of intermittent swelling. With progression of the disease, patients may complain of more persistent swelling or effusion, catching, locking, and/or giving way. Unfortunately, pain and swelling are not good indicators of dissection. Physical findings may include a positive Wilson test, which reproduces the pain by internally rotating the tibia during extension of the knee between 90 and 30 degrees, then relieving the pain with tibial external rotation. The premise for this test is that the tibial eminence impinges on the OCD lesion in internal rotation and extension; whereas, external rotation moves the eminence away from the lesion.
Standard weight-bearing radiographs of both knees are helpful for initially characterizing the lesion type and status of the growth plate. The lateral view helps identify anterior-posterior lesion location and normal, benign accessory ossification centers in the skeletally immature knee. An axial view is helpful if a lesion of the patella or trochlea is suspected, and a "notch view" in 30 to 50 degrees of knee flexion may help identify the lesions of the posterior femoral condyle.
Studies have been performed to attempt to identify specific MRI findings that link the ability of OCD lesions to heal following non-operative treatment.
Non-Operative Treatment
The goal of non-operative intervention is to promote healing in the subchondral bone and prevent chondral collapse, subsequent fracture, and crater formation. The treatment depends on skeletal maturity of the patient, as well as the size, stability, and location of the lesion as the more skeletally mature a patient, the worse the prognosis. Non-surgical treatment is the treatment of choice for small stable lesions in skeletally immature patients with wide open physes and no signs of instability on MRI. Nonsurgical management focuses on significant activity modification by limiting high impact activities. Short-term immobilization and protected weight bearing may be helpful. Alternatively, bracing and range-of-motion knee exercises may be beneficial. Typically a period of three to nine months of non-operative treatment is initiated. Surgical treatment to promote healing is suggested when non-surgical methods fail and for skeletally mature patients with large lesions.
Operative Treatment
Surgical management begins with arthroscopy. Operative treatment should be considered for patients with unstable or detached lesions, failed non-operative treatment, and for patients approaching skeletal maturity. The goals of operative treatment are to promote healing of subchondral bone, to maintain joint congruity, to fix rigidly unstable fragments, and to replace osteochondral defects with cells that can replace and grow cartilage. (53) Optimal surgical treatment provides a stable construct of subchondral bone, calcified tidemark, and repair cartilage with viability and biomechanical properties equivalent to or similar to native hyaline cartilage.
Surgical treatment for stable lesions with intact articular cartilage involves drilling the subchondral bone with the intention of stimulating vascular ingrowth and subchondral bone healing. If the lesion is unstable and hinged, fixation is indicated. For patients with a hinged lesion without subchondral support, bone grafting is indicated to restore articular congruency. The goal is to fix the osseous portion of the fragment to allow healing and stabilization of the overlying articular surface. Arthroscopic or open reduction and internal fixation can be performed with hardware using Kirschner wires, cannulated screws, or Herbert screws. Associated complications include implant migration, adjacent cartilage damage, and hardware fracture. Osteochondral plugs have recently been presented as a biologic alternative to the use of hardware. The plugs provide bone graft as well as fixation of the lesion.
If fixation is not possible, there are several salvage techniques for full-thickness defects, including marrow stimulation techniques such as microfracture as well as autologous chondrocyte implantation, and osteochondral autograft transplantation. However, these techniques have limited clinical outcome data in adolescents.
When strength grade is 70% of unaffected limb, patient can begin to run after clearance from M.D. When 90% strength of unaffected limb is attained and patient can run 10 minutes without pain or swelling, patient can return to agility type sports after being cleared by M.D. Patient must complete Return to Sport Agility Protocol without pain or swelling.
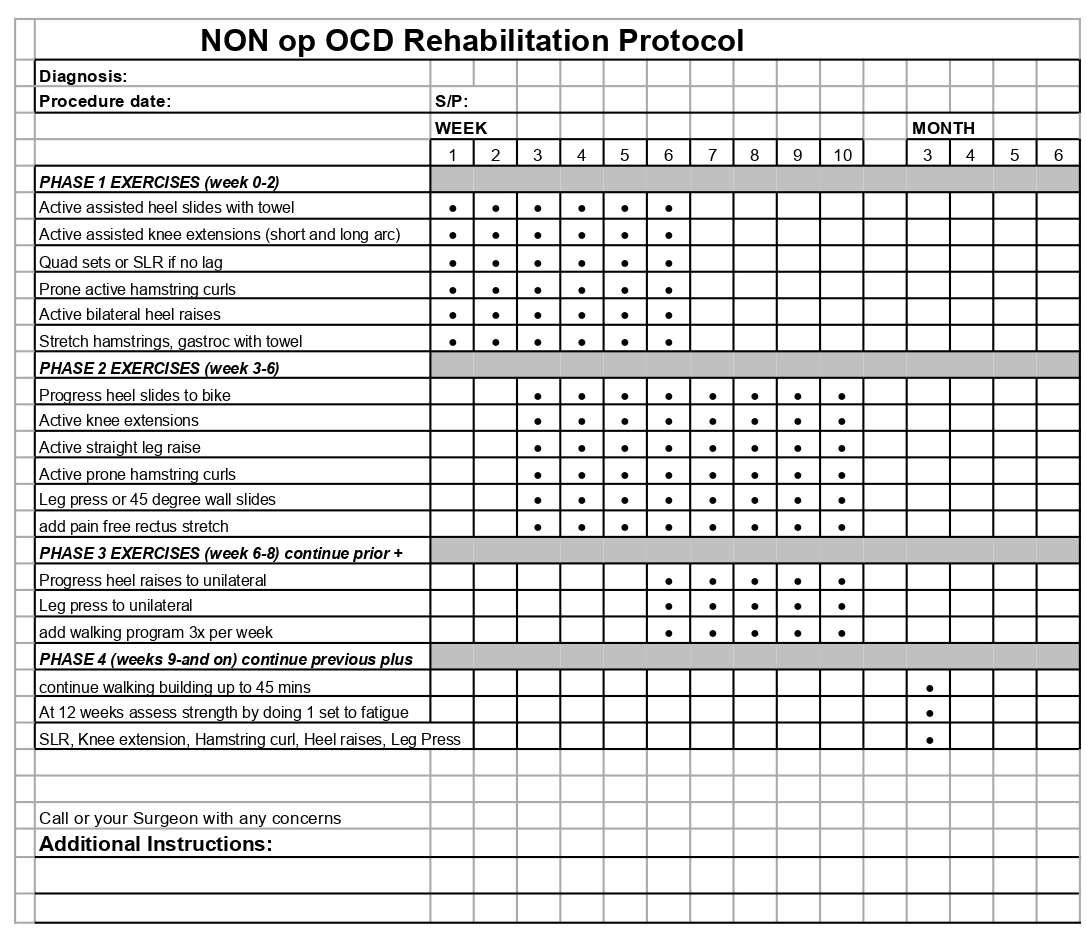
Osteochrondritis dissecans
Osteochrondritis dissecans (aka "OCD")
OCD is a relatively rare problem, likely affecting far less than 1 percent of the population, in which the bone that supports the cartilage inside a joint undergoes softening. This softening is caused by an interruption in the blood flow to that portion of bone. Over time, if left untreated, this can lead to damage to the overlying cartilage of the joint. Loose pieces of bone and cartilage can even break off into joint. Long term ramifications may even include arthritis.
Etiology/ Pathoanatomy
The causes of OCD are unknown, however repetitive trauma, inflammation, accessory centers of ossification, ischemia, and genetic factors show causative correlation. Some familial tendencies exist, but non-familial OCD is most prevalent. Repetitive trauma caused by year round sports, early sports specialization, multiple sports in a singe season or multiple teams in a single sport and increased training intensity are some of the causative factor associated with OCD. Chronic repetitive microtrauma has been suggested to lead to a stress reaction within the subchondral bone and in more severe cases subchondral bone necrosis where fragment dissection and separation may ensue.
Evaluation
Patients with OCD of knee initially have nonspecific complaints, with anterior knee pain and variable amounts of intermittent swelling. With progression of the disease, patients may complain of more persistent swelling or effusion, catching, locking, and/or giving way. Unfortunately, pain and swelling are not good indicators of dissection. Physical findings may include a positive Wilson test, which reproduces the pain by internally rotating the tibia during extension of the knee between 90 and 30 degrees, then relieving the pain with tibial external rotation. The premise for this test is that the tibial eminence impinges on the OCD lesion in internal rotation and extension; whereas, external rotation moves the eminence away from the lesion.
Standard weight-bearing radiographs of both knees are helpful for initially characterizing the lesion type and status of the growth plate. The lateral view helps identify anterior-posterior lesion location and normal, benign accessory ossification centers in the skeletally immature knee. An axial view is helpful if a lesion of the patella or trochlea is suspected, and a "notch view" in 30 to 50 degrees of knee flexion may help identify the lesions of the posterior femoral condyle.
Studies have been performed to attempt to identify specific MRI findings that link the ability of OCD lesions to heal following non-operative treatment.
Non-Operative Treatment
The goal of non-operative intervention is to promote healing in the subchondral bone and prevent chondral collapse, subsequent fracture, and crater formation. The treatment depends on skeletal maturity of the patient, as well as the size, stability, and location of the lesion as the more skeletally mature a patient, the worse the prognosis. Non-surgical treatment is the treatment of choice for small stable lesions in skeletally immature patients with wide open physes and no signs of instability on MRI. Nonsurgical management focuses on significant activity modification by limiting high impact activities. Short-term immobilization and protected weight bearing may be helpful. Alternatively, bracing and range-of-motion knee exercises may be beneficial. Typically a period of three to nine months of non-operative treatment is initiated. Surgical treatment to promote healing is suggested when non-surgical methods fail and for skeletally mature patients with large lesions.
Operative Treatment
Surgical management begins with arthroscopy. Operative treatment should be considered for patients with unstable or detached lesions, failed non-operative treatment, and for patients approaching skeletal maturity. The goals of operative treatment are to promote healing of subchondral bone, to maintain joint congruity, to fix rigidly unstable fragments, and to replace osteochondral defects with cells that can replace and grow cartilage. (53) Optimal surgical treatment provides a stable construct of subchondral bone, calcified tidemark, and repair cartilage with viability and biomechanical properties equivalent to or similar to native hyaline cartilage.
Surgical treatment for stable lesions with intact articular cartilage involves drilling the subchondral bone with the intention of stimulating vascular ingrowth and subchondral bone healing. If the lesion is unstable and hinged, fixation is indicated. For patients with a hinged lesion without subchondral support, bone grafting is indicated to restore articular congruency. The goal is to fix the osseous portion of the fragment to allow healing and stabilization of the overlying articular surface. Arthroscopic or open reduction and internal fixation can be performed with hardware using Kirschner wires, cannulated screws, or Herbert screws. Associated complications include implant migration, adjacent cartilage damage, and hardware fracture. Osteochondral plugs have recently been presented as a biologic alternative to the use of hardware. The plugs provide bone graft as well as fixation of the lesion.
If fixation is not possible, there are several salvage techniques for full-thickness defects, including marrow stimulation techniques such as microfracture as well as autologous chondrocyte implantation, and osteochondral autograft transplantation. However, these techniques have limited clinical outcome data in adolescents.
OCD of knee - post op
These are general guidelines. Treatment varies for individual patients.
Immediately post op
- Dressing: Dressing, cryocuff applied in OR
- Brace: Bledsoe in OR (ROM 0-40°). Wear for 6 weeks total.
- Crutches: Partial weight bearing x 6 weeks.
- Pain control: Rx for Tylenol #3/vicodin/percoset given on day of surgery.
- Follow up: Return to clinic for 2 week post op visit.
2 weeks post op
- Clinic visit: Remove sutures.
- Brace: Continue Bledsoe for additional 4 weeks.
- Crutches: Continue partial weight bearing for additional 4 weeks.
- Physical therapy: start PT for ROM, SLR, no PT at 2 weeks if screw used.
- Follow up: Return to clinic for 6 week post op visit.
6 weeks post op
- Clinic visit: Ensure patient progressing. Check ROM, strength, x-ray to check healing.
- Brace: Discontinue Bledsoe.
- Crutches: Discontinue.
- Activities: Continue physical therapy. Avoid cutting/pivoting for additional 6 weeks.
- Follow up: Return to clinic for 12 week post op check.
12 weeks post op
- Clinic visit: Ensure patient progressing. Check ROM, strength.
- Activity: Gradual return to activities/sports.
- Follow up: Return to clinic in 3 months if ongoing issues, or PRN.
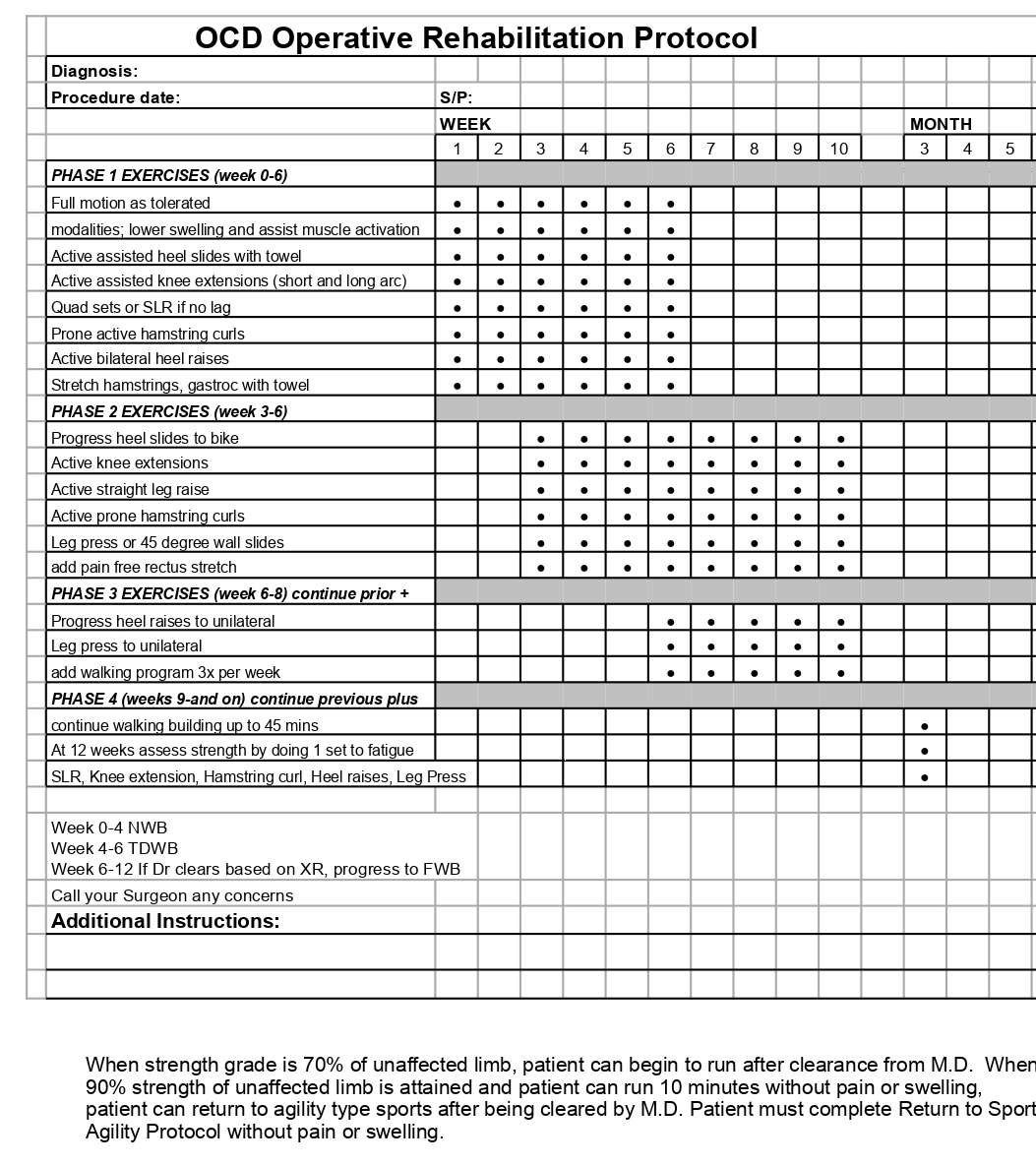

Patellar and Quadriceps Tendon
Rehabilitation After Repair of the Patellar and Quadriceps Tendon
The patellar tendon attaches to the tibial tubercle on the front of the tibia (shin bone) just below the front of the knee. It also is attached to the bottom of the patella (kneecap). At the top of the patella, the quadriceps tendon is attached. Attaching to the quadriceps tendon is the quadriceps muscle. The quadriceps muscle is the large muscle on the front of the thigh. As the quadriceps muscle contracts (shortens), it pulls on the quadriceps tendon, the patella, the patellar tendon, and the tibia to move the knee from a flexed (bent) position to an extended (straight) position. Conversely, when the quadriceps muscle relaxes, it lengthens. This allows the knee to move from a position of extension (straight) to a position of flexion (bent).
When the patellar tendon ruptures, the patella loses its anchoring support to the tibia. Without this anchoring effect of the intact patellar tendon, the patella tends to move upward (towards the hip) as the quadriceps muscle contracts. Without the intact patellar tendon, the patient is unable to straighten the knee. If a rupture of the patellar tendon occurs, and the patient tries to stand up, the knee will usually buckle and give way because the quadriceps muscle is no longer able to hold the knee in a position of extension (straight).
When the quadriceps tendon ruptures, the patella loses its anchoring support in the thigh. Without this anchoring effect of the intact quadriceps tendon, the patella tends to move inferiorly (towards the foot). Without the intact quadriceps tendon, the patient is unable to straighten the knee. If a rupture of the quadriceps tendon occurs, and the patient tries to stand up, the knee will also usually buckle and give way, again, because the quadriceps muscle is no longer able to hold the knee in a position of extension (straight).
The office examination consists of palpating the quadriceps and patellar tendons and the patella. Usually, when these tendons rupture, the patella moves upwards on the thigh for patellar tendon ruptures and slips downward for quadriceps tendon ruptures. At the same time, the gap between the ends of the ruptured tendon is palpable on the front of the knee. X-rays of the knee usually reveal the abnormal position of the patella, indicating a rupture of the patellar/quadriceps tendon.
This is an injury that must be treated surgically. Since the tendon is outside of the joint, it cannot be repaired arthroscopically. Usually, the repair is done as an outpatient surgery. An incision is made on the front of the knee, over the tendon. The site of the tendon rupture is identified. The tendon ends are identified and then sewn together. Afterwards, a knee immobilizer or hinged brace is often used to protect the repair. The length of time required for bracing is usually a minimum of 6 weeks followed by several weeks of rehabilitation. The usual risks of surgery are involved including: infection, stiffness, suture reaction, failure of satisfactory healing, risks of anesthesia, phlebitis, pulmonary embolus (blood clot in the lungs), and persistent pain or weakness after the injury and repair.
Rehabilitation after Repair of the Quadriceps and Patellar Tendons
Phase One: 0-14 days
Goals:
- Control pain and swelling
- Initiate knee motion
- Activate the quadriceps muscles
Knee Range of Motion:
There are no knee range-of-motion exercises at this time. Keep the knee in the post-op brace, locked in full extension (fully straight).
Brace and Crutches:
You will go home with crutches and a knee brace locked in full extension (straight). Unless otherwise instructed by the doctor, use crutches when walking and bear weight as tolerated (with brace-on and your knee locked straight) on the operated leg. When walking with the crutches, follow the instructions below:
Walking (weight bearing as tolerated):
- Put the crutches forward about one step's length.
- Put the injured leg forward; level with the crutch tips.
- Touch the foot of the involved leg to the floor and bear weight as tolerated (brace-on).
- While bearing weight (on the crutches if there is pain in the knee) on the involved leg, take a step through with the uninjured leg.
Exercise Program:
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles and straighten the knee. Lie or sit with the knee extended fully straight as in figure. Tighten and hold the front thigh muscle making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscle. The tightening action of the Quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold 5 seconds for each contraction. Do 20 repetitions three times a day.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to see your Surgeon approximately 10-14 days after your surgery. At this time, your sutures will be removed and your progress will be checked.
Rehabilitation after Repair of the Patellar and Quadriceps Tendon
Phase Two: 2 to 6 weeks after surgery
Goals:
- Protect the tendon repair from overstress and allow healing
- Regain knee motion, limiting knee flexion to 90 degrees
- Begin muscle strengthening
Knee Range of Motion:
You can fully extend (straighten the knee). To avoid placing excess stress on the tendon repair, do not bend your knee beyond 90 degrees (bent to a right angle). Your doctor will give you instructions if this limit will be different than outlined here.
Brace and Crutches:
Unless otherwise instructed by your Surgeon, use crutches when walking and bear weight as tolerated on the operated leg. Wear the post-operative brace for walking. Lock the brace with the knee fully straight when walking to protect the knee in case of a fall. You can unlock the brace to sit or move the knee when not walking if the doctor allows you to. When walking with the crutches, follow the instructions below:
Walking (Weight bearing as tolerated), brace locked in full extension:
- Put the crutches forward about one step's length.
- Put the injured leg forward; level with the crutch tips.
- Touch the foot of the involved leg to the floor and bear as much weight as you can without pain.
- If you cannot bear full weight without pain, place some of your weight on the crutches so that there is no pain with weight bearing.
- If you are able to bear full weight without pain, you can taper to one crutch, held on the opposite side of your affected knee.
- If you continue to have no pain with weight bearing, you can discontinue the crutch and walk with the brace only locked in full extension.
EXERCISE PROGRAM
Perform daily
| Quadriceps sets | 3 sets of 10 reps |
| Heel Prop | 5 minutes |
| Heel slides | 20 reps |
| Sitting knee flexion | 20 reps |
| Hip abduction | 20 reps |
| Standing toe raises | 20 reps |
| Ankle pumps | 10 times an hour |
Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lazy-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 10 repetitions.
HEEL PROP- to straighten (extend) the knee. Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
HEEL SLIDES - to regain the bend (flexion) of the knee. While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise.
SITTING KNEE FLEXION - to regain the bend (flexion of the knee). While sitting in a chair or over the edge of your bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the unoperated leg controlling, allowing the knee to bend to a limit or maximum of 90°. Hold five seconds and slowly relieve the stretch by lifting the foot upward, with the uninvolved leg, to the straight position (passive assist). Repeat exercise 20 times, three times a day.
HIP ABDUCTION - lie on your unoperated side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, then lower slowly. Repeat 20 times, once or twice a day.
STANDING TOE RAISES - With the knee brace on, use a table for support and balance. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position.
ANKLE PUMPS - move your foot up and down at the ankle to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please make an appointment with your Surgeon at 6 weeks after surgery.
Rehabilitation after Repair of the Patellar and Quadriceps Tendon
Phase Three: 6 to 12 weeks after Surgery
Goals:
- Walk normally
- Regain and improve range of motion
- Start muscle strengthening exercises
Activities:
- The repaired tendon is still weak and subject to injury if you overload it. You should be careful walking up and down steps or inclined surfaces.
- You may begin to wean from the knee immobilizer as instructed by your doctor. It is recommended that if walking without the immobilizer, you use one crutch on the side opposite your injured knee, in case you slip or stumble.
- Avoid squatting, deep knee bends, and lunging movements and do not try to step up or down stairs.
- Bear full weight on level surfaces and try to avoid limping, and walk slowly but normally.
- Continue to ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury.
Brace and Crutches:
Unless otherwise instructed by the doctor, you can gradually discontinue crutches when walking and bear full weight on the operated leg. Wear the post-operative brace for walking. Your doctor may make an adjustment to the brace so that you can bend your knee when you walk. Be sure that you get specific instructions from the doctor before making any changes to your support when walking.
Exercise Program:
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds. Do the exercises daily for the first week, then decrease to every other day when using ankle weights.
You may also ride the stationary bicycle daily for 10 to 20 minutes. Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
(see phase 2 for descriptions and illustrations)
Days per week- 5-7 Times per day 1
| Quadriceps set | 3 sets of 10 reps |
| Heel prop | 5 minutes |
| Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing toe raise | 3 sets of 10 reps |
| Hip abduction | 3 sets of 10 reps |
| Wall slides | 3 sets of 10 reps |
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
OFFICE VISIT
Please make an appointment with your Surgeon at 12 weeks after surgery.
Rehabilitation after Patellar Tendon and Quadriceps Tendon Repair
Phase 4: Twelve weeks after surgery onward
ACTIVITIES
1. Walking/Stairs
You should be walking without the aid of a brace or crutches. If you feel confident walking on the operated limb and have good strength and knee motion, you can begin attempting to walk up-stairs on the operated limb. It is not recommended that you lower yourself down-stairs on the operated limb until you complete the enclosed 'Step up-down progression'.
2. Knee Support – for excess activities
Buy an elastic knee sleeve (made of neoprene rubber) at a sporting goods store. It should have an opening for the kneecap and velcro straps but does not need hinges on the sides. Use this support if you are on your feet for a prolonged period of time.
3. Stationary Bicycle – good exercise
Utilize a stationary bicycle to both strengthen the thigh muscles and increase knee flexion. If you cannot yet pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. You may ride the cycle with mild resistance for up to 10 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
4. Swimming – good exercise
Swimming is good exercise at this time, if available.
5. Exercises
You should add the following exercises, every other day, as instructed by the physical therapist:
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees. Pause five seconds and then slowly slide back up to the upright starting position. When doing a wall slide, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe. This exercise is illustrated in phase 2.
SQUAT TO CHAIR
In the chair squat exercise, you lower your buttocks toward the chair until your buttocks touch the chair. Do not sit or rest at the chair, but instead immediately and slowly return to the standing and starting position. Remember to keep your head over your feet and bend at the waist as you descend. When doing a squat, you should position your thighs so that your kneecaps are in line with the tips of your shoes, or your second toe. After the first week, you may hold dumbbells while performing this exercise and the wall slide. Start with 3 to 5 pounds each hand. You may add 2 to 3 pounds per week until you reach 10 pounds in each hand.
STEP-UP-DOWN EXERCISE
At this time, it is important to begin the development of single-leg strength. Begin to follow the "Step-up-down Strengthening progression" outlined below, if you are able to do the exercises without pain. The instructions estimate a time period of 6 to 8 weeks for you to progress through the whole program. This time line will vary for different people and knees, depending upon the presence of other knee problems. Place the foot of the operated limb on the stool. Maintain balance, if necessary, by holding onto the wall or chair. Standing sideways to the step, slowly step up onto the stool and slowly straighten the knee using the quadriceps muscles. Slowly lower the opposite foot to touch the floor. Do not land on the floor, just touch gently and repeat the step up.
Step Up-Down exercise Progression (12-20 weeks after surgery)
Start with a step of 3 inches in height. Start with 3 sets of 5 repetitions for the first 2 weeks. If pain free, add one repetition per set, per workout, until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 6 inches in height. Repeat progression starting with 3 sets of 5 repetitions for 2 weeks. After that, if pain free, add one repetition per set until you can do 3 sets of 10 (about 2 weeks). If pain free, progress to a step of 9 inches in height (the height of a standard stair). Repeat progression starting with 3 sets of 5 repetitions for 2 weeks. After that, if pain free, add one repetition per set until you can do 3 sets of 10 (about 2 weeks). Do not continue to raise the height of the step if there is pain or crepitus at the kneecap.
ONE LEGGED TOE RAISES
Continue the toe-raises from phase 2, but now try to raise up and down slowly on just the operated side. Hold the unoperated foot off the floor and hold the wall or a chair or table for balance and support. Build to 3 sets of 15 repetitions.
HAMSTRING STRETCH
Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for 15 to 20 seconds and repeat 3 to 5 times.
QUADRICEPS STRETCH
Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold 15 to 20 seconds for 3 to 5 repetitions.
CALF STRETCH
Keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for 15 to 20 seconds for 3 to 5 repetitions.
OPTIONAL ADDITIONAL EXERCISES
The following exercises may be added to your exercise program at 16 weeks after surgery:
SEATED LEG PRESS
If you are using a leg press machine for strengthening, use an amount of weight that feels easy enough to perform 20 repetitions as the starting weight for this exercise. Use this weight for the first week before raising the weight. The weight may be increased by about 5 pounds every 7 to 10 days thereafter, as long as you can perform 20 repetitions per set for 3 sets, and as long as the weight used does not exceed body-weight when using both legs, or 1/2 body weight when using the one leg. In this exercise, avoid letting the knees snap or drop suddenly into extension when reaching the fully straightened position. Avoid starting the exercise with the knees bent past 90 degrees. Adjust the seat position to limit the excursion of the machine.
RESISTED HAMSTRING CURLS
If you have access to a hamstring curl machine, you may start using it. As with the leg press, start with a reasonable weight and use that weight for the first week. You may increase the weight by 3 to 5 pounds every 10 days as long as you can perform 3 sets of 20 repetitions slowly, with good form. If you do not have access to a hamstring machine, continue doing the standing hamstring curl adding an ankle weight for resistance. Start with 3 to 5 pounds and add 1 pound per week until you build to 10 pounds for 3 sets of 15 repetitions.
Additional Weight Training
Hip Abductor/Adductor machine Roman Chair Calf Raise Machine
Precautions When Exercising
- Avoid pain at the tendon repair site
- Avoid pain and/or crepitus at the patella
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
The following exercises are not recommended until full knee strength recovered because they may overload the patella and the tendon repair:
- Knee extension using a weight lifting machine
- Lunges
- Stairmaster
- Step exercises with impact
- Running
- Jumping
- Pivoting or cutting
OFFICE VISIT
Please make an appointment to see your Surgeon in 12 weeks (6 months after surgery).
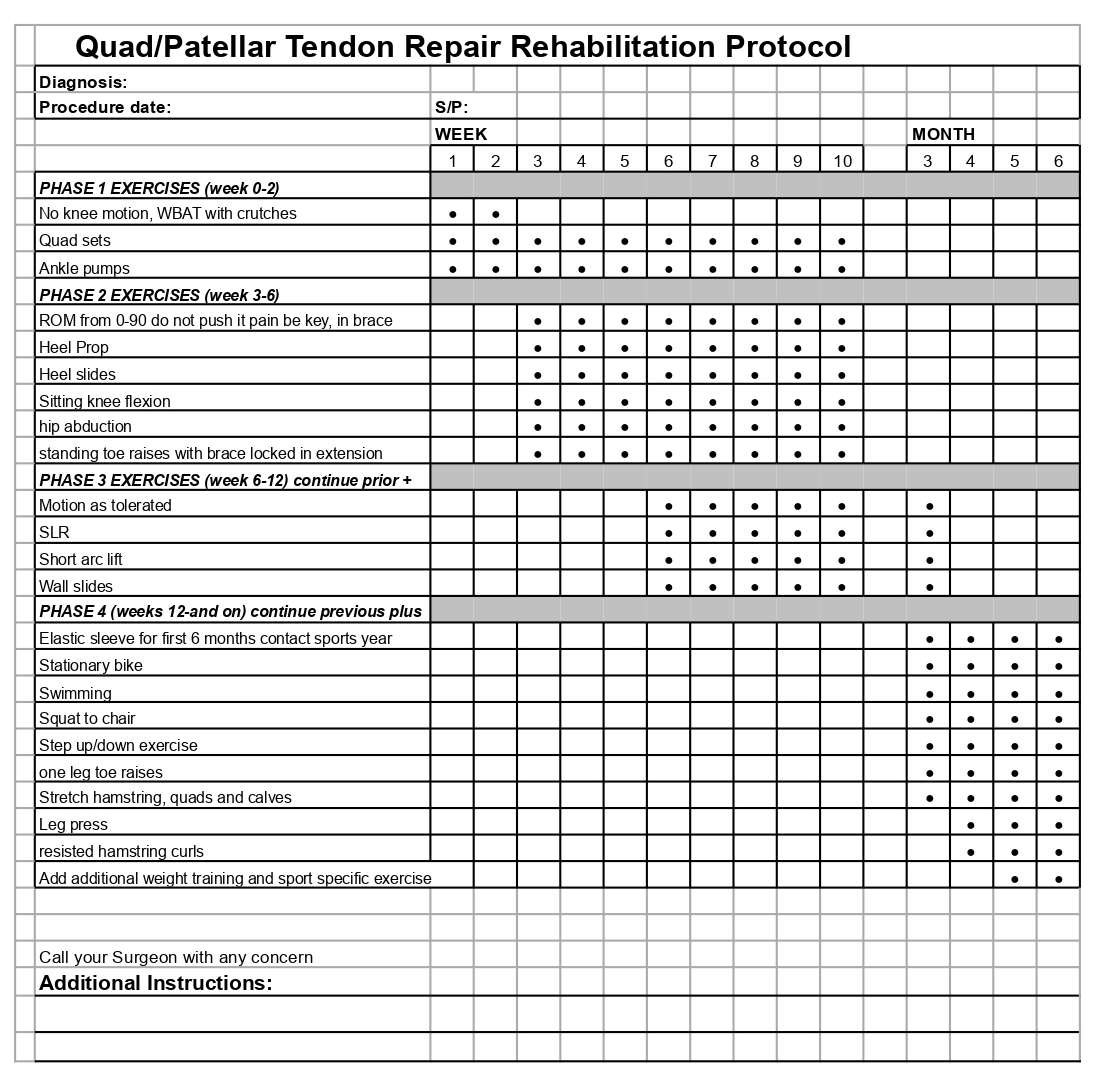
Patellofemoral Instability
Patellofemoral Instability (Subluxation and Dislocation)
Anatomy and Function
The knee joint is composed of two distinctly separate articulations. The tibiofemoral joint is formed by the thigh bone (femur) meeting the shin bone (tibia). The patellofemoral joint is formed by the kneecap (patella) gliding along a groove (trochlea) of the femur. The quadriceps muscles in the front of the thigh attach to the patella and continue via the patellar tendon to insert into the tibia. When the quadriceps muscles contract, the knee straightens (extends). The patella protects the knee from a direct blow and, more importantly, creates a fulcrum that increases the mechanical efficiency of the action of the quadriceps muscles.
Patellofemoral Alignment
Multiple aspects go into patellar instability including: the q-angle (quadriceps angle), alta or baja, trochlear dysplasia, TT-TG distance, rotation of the femur as well as the tibia, dynamic muscular forces. With abnormalities of the aforementioned structures the patella can partially dislocate (subluxate) or completely dislocate from a direct sideways blow to the knee or if the Q-angle temporarily increases too much due to outward rotation of the leg and foot (such as when pivoting).
Diagnosis of Patellofemoral Instability
Pain in the front of the knee and a sensation of "looseness" of the kneecap are common complaints. If the patella partially dislocates (subluxates) the knee will "give-way" or buckle. If this condition is suspected, Dr. Nelson may order x-rays of your knee that will show the position of the patella in the trochlear groove. Patellar tracking can be tested during the physical examination.
Non-operative Treatment
Non-operative treatment consists of the following:
- Bracing and lateral knee supports to help hold the patella in place.
- Exercises to strengthen the quadriceps muscles
- Activity modification - avoiding excess pivoting sports
Operative Treatment
Operative treatment for patellofemoral instability consists of surgery to re-align the patella and to decrease the Q-angle. Surgical treatment can be divided into two basic types:
Proximal re-alignment procedures
- Proximal re-alignment consists of making a small incision at the knee and lengthening the restraining structures on the outside of the patella and/or shortening the ligaments on the inside of the patella. This procedure is usually used in young patients in whom the growth plates are still open. Proximal re-alignment is often done in combination with a distal re-alignment procedure.
- Another option to proximal re-alignment consists of making small incisions along the inside of the knee to reconstruct the medial patellofemoral ligament (MPFL). This procedure is utilized on patients who have normal alignment and have incompetent medial soft tissue structures.
Distal re-alignment procedures
- Distal re-alignment consist of making a small incision over the upper tibia. The surgeon then uses a bone-cutting instrument to cut the tibial tubercle (to which the patellar tendon attaches) so that the bone and patellar tendon can be moved medially or toward the inside of the knee. The piece of bone is reattached to the tibia using two screws. This procedure re-aligns the pull of the quadriceps muscles across the knee by decreasing the Q-angle. After surgery a knee brace is worn to protect the knee for about six weeks until the bone is healed. You may bear partial weight on the leg when using the immobilizer and crutches when you are comfortable doing so. The two screws can be removed when the bone is completely healed (after about six months) if they are tender.
Results of Surgery and Risks
Results of both proximal and distal patellar re-alignment procedures are good when performed on appropriately selected patients. In patients who have pre-existing injury to the joint surfaces (such as chondromalacia), knee pain and crepitus (joint noise) can persist. In most instances, however, knee function improves after surgery due to better knee mechanics.
Risks of surgery:
- wound infection
- continued pain
- delayed bone healing
- loss of motion
Patellar Re-Alignment Surgery Preoperative Instructions
Here are guidelines that will help you prepare for surgery that will re-align your patella.
Within One Month Before Surgery:
Your Surgeon will see you in the office. A preoperative history and physical examination will be completed. He will write preoperative hospital orders and order laboratory tests. These tests usually include a complete blood count (and also electrocardiogram for patients over 40 years old.)
The Day Before Surgery:
You can have nothing to eat or drink after midnight on the evening before surgery. It is very important to have a completely empty stomach prior to surgery for anesthesia safety reasons. If you have to take medication, you can take the medication with a sip of water early in the morning prior to surgery (but later tell the anesthesiologist you have done so).
The Day of Surgery:
Please bring any crutches, brace, ice machine, or imaging studies that you have received.
Surgery:
If a problem inside of the knee is suspected (such as chondromalacia), arthroscopy may be done in addition to open surgery to re-align the patella. After anesthesia has been given, your knee will be cleaned and sterile drapes will be placed. To perform the patella realignment, a small incision will be made below the knee joint on the outer side of the upper tibia. The doctor will divide the tibial tubercle (where the patellar tendon inserts into bone) and move the tibial tubercle medially about one-half inch. The bone will be fixed in its new position using two screws.
After Surgery:
You will be given a prescription for pain medication to take home with you. The pain medication has a tendency to make you constipated while you are taking it and occasionally can cause nausea. In addition to pain medication you should take one aspirin a day to help prevent blood clots (phlebitis) unless there is a reason to avoid aspirin. You will have a knee brace applied to protect the knee. The brace can be removed for washing and sleeping, but should be used when you are up and walking for about six weeks. You can use crutches for the first week or two to take excess pressure off of the knee. The dressing will be changed the day following surgery and can be removed at two days. The wound is sealed with steri-strips (small pieces of tape on the skin). You can shower on the second day following surgery, but be careful standing in the shower so you do not fall. It is better to have a small stool to be able to sit on. You can get the incision wet and wash the knee. If the lower leg swells, elevate the leg or use below-knee elastic stockings to control swelling. If you develop calf pain or excessive swelling in the leg, call the doctors office. The cryocuff is a blue wrap that is sometimes put on the knee to make it easier to keep it cold. You can use the cryocuff or ice packs as often as you want to cool down the knee to reduce swelling and pain.
OFFICE VISIT
Please arrange an office visit approximately one week after surgery for suture removal and further instructions.
Rehabilitation After Patellar Realignment Surgery
Phase One: the first week after surgery
Goals:
- Control pain and swelling
- Initiate knee motion
- Activate the quadriceps muscles
Guidelines and Activities:
- You will go home with crutches and a knee immobilizer. You can bear full weight and walk on the leg with the immobilizer and your crutches unless otherwise instructed by your Surgeon.
- Apply cold to reduce pain and swelling. Use ice on the knee 20 minutes/on and 20 minutes/off for the first day when awake. Then apply cold as often as needed for 15 to 20 minutes at a time for the next several days. Place a towel or cloth between the skin and the ice to prevent skin injury.
- Wrap an elastic bandage (ace) around the knee at other times to control swelling.
- You may shower and get your incision wet. Do not soak the incision in a bath tub or Jacuzzi until the stitches have been removed.
- Take an aspirin each morning, unless there is a reason not to take aspirin.
Exercise Program:
QUADRICEPS SETTING - to maintain muscle tone in the thigh muscles (quadriceps) and straighten the knee. Lie on your back with your knee extended fully straight as in figure. Tighten and hold the front thigh muscles making the knee flat and straight. If done correctly, the kneecap will slide slightly upward toward the thigh muscles as the muscles contract. The tightening action of the quadriceps should make your knee straighten and be pushed flat against the bed or floor. Hold for five seconds for each contraction. Do 20 repetitions whenever you think about it (many times a day).
STRAIGHT LEG RAISE- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 5-10 pounds.
ANKLE PUMPS - move the foot up and down to stimulate circulation in the leg. Do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to see your Surgeon approximately 10-14 days after your surgery. At this time, your sutures will be removed and your progress will be checked. You will see the physical therapist for exercise instruction.
Rehabilitation After Patellar Realignment Surgery
Phase Two: Two to six weeks after surgery
This protocol is a guideline for your rehabilitation after patellar re-alignment surgery. You may vary in your ability to do these exercises and to progress from one phase to the other. Please call your doctor if you are having a problem with your knee or if you need clarification of these instructions.
GOALS:
- Protect the patellar re-alignment – avoid falling
- Ensure wound healing
- Maintain full knee extension (knee straight)
- Initiate passive knee flexion exercises
- Decrease swelling in the knee and leg
- Promote activation of the quadriceps muscle
- Avoid blood pooling in the leg
ACTIVITIES:
BRACE/CRUTCHES
Use the knee brace (immobilizer) when you get out of bed and walk. The brace is set for full extension (straight). You can put your full weight on your operated leg while wearing the immobilizer. You should use the crutches if you need extra support when you are walking. After one or two weeks, you can begin to using one crutch on the side opposite of your surgery if you are comfortable and gradually stop using the crutch when the knee feels strong enough to do so (but continue to use the knee immobilizer).
COLD APPLICATION (CRYOCUFF OPTIONAL)
Fill the blue cryocuff by putting ice water in the container and elevating the container above the knee so the cold water runs into the cryocuff. Use the cryocuff for 20 minutes at a time whenever you want to, but especially after exercising. If you do not have a cryocuff, put ice into a plastic bag. Put a thin towel over the knee and apply the ice pack.
Exercise Program
Perform daily
| Quadriceps set | 3 sets of 10 reps |
| Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing toe raise | 3 sets of 10 reps |
| Hip abduction | 3 sets of 10 reps |
| Ankle pumps | 10 times an hour |
HEEL SLIDES - to regain the bend (flexion) of your knee. Keep brace on 0-30 degrees of flexion for TTO, 0-90 for MPFL. While lying on your back, use your muscles to slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for five seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise.
SHORT ARC LIFT- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 10 repetitions.
STANDING TOE RAISES - With the knee brace on, use a table for support and balance. Tighten the quadricep to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position.
HIP ABDUCTION - lie on your unoperated side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, then lower slowly. Repeat 20 times, once or twice a day.
ANKLE PUMPS - move your foot up and down at the ankle to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to see your Surgeon approximately six weeks after your surgery.
Rehabilitation After Patellar Realignment Surgery
Phase Three: 6 to 12 weeks after surgery
Goals:
- Walk normally
- Regain full motion
- Regain full muscle strength
Activities:
- Continue the brace opened from 0-120 degrees of motion.
- Bear full weight and walk on the leg. Try to avoid limping and walk slowly but normally.
- Continue to ice the knee if there is pain and swelling. Place a towel or cloth between the skin and the ice to prevent skin injury.
Exercise Program
The following exercise program will help you regain knee motion and strength. If the exercises can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and to build strength. Start with one pound and add one pound per week until you reach five pounds.
Do the exercises daily for the first week, then decrease to every other day when using ankle weights.
You may ride the stationary bicycle daily for 10 to 20 minutes.
Avoid using stair-stepper machines, doing deep knee bends and squats or any exercise that causes crunching, clicking or pain at the kneecap.
| Quadriceps set | 3 sets of 10 reps |
| Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Short arc lift | 3 sets of 10 reps |
| Standing hamstring curl | 3 sets of 10 reps |
| Standing toe raise | 3 sets of 10 reps |
| Hip abduction | 3 sets of 10 reps |
| Wall slides | 3 sets of 10 reps |
STATIONARY BICYCLE
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for 10 to 20 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then ride the bicycle with your forefoot resting on the pedal.
STANDING HAMSTRING CURL
Stand facing the wall, using the wall for balance and support. While standing on the non operative limb, bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated.
WALL SLIDES
Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
OFFICE VISIT
Please make an appointment with your Surgeon's office at 12 weeks after surgery.
Rehabilitation after Patellar Realignment
Phase Four: twelve weeks after surgery onward
ACTIVITIES
1. Walking/Stairs
You should be walking without the aid of a brace or crutches. If you feel confident walking on the operated limb and have good strength and knee motion, you can begin attempting to walk upstairs on the operated limb. It is not recommended that you lower yourself down-stairs on the operated limb until you have regained your strength in the operative leg.
2. Knee Support – for excess activities
Buy an elastic knee sleeve (made of neoprene rubber) at a sporting goods store. It should have an opening for the kneecap and velcro straps but does not need hinges on the sides. Use this support if you are on your feet for a prolonged period of time.
3. Stationary Bicycle – good exercise
Utilize a stationary bicycle to both strengthen the thigh muscles and increase knee flexion. If you cannot yet pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. You may ride the cycle with mild resistance for up to 10 minutes a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
4. Swimming – good exercise
Swimming is good exercise at this time, if available.
5. Exercises
You should add strength training exercises, every other day, as instructed by the physical therapist. In addition, in line running may be added.
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
Avoid the following exercises unless your therapist has deemed you ready:
- Knee extension weight lifting machine
- Running
- Jumping
- Pivoting or cutting
- Lunges
- Stairmaster
- Step exercises with impact
OFFICE VISIT
Please make an appointment to see your Surgeon in 12 weeks (6 months after surgery).
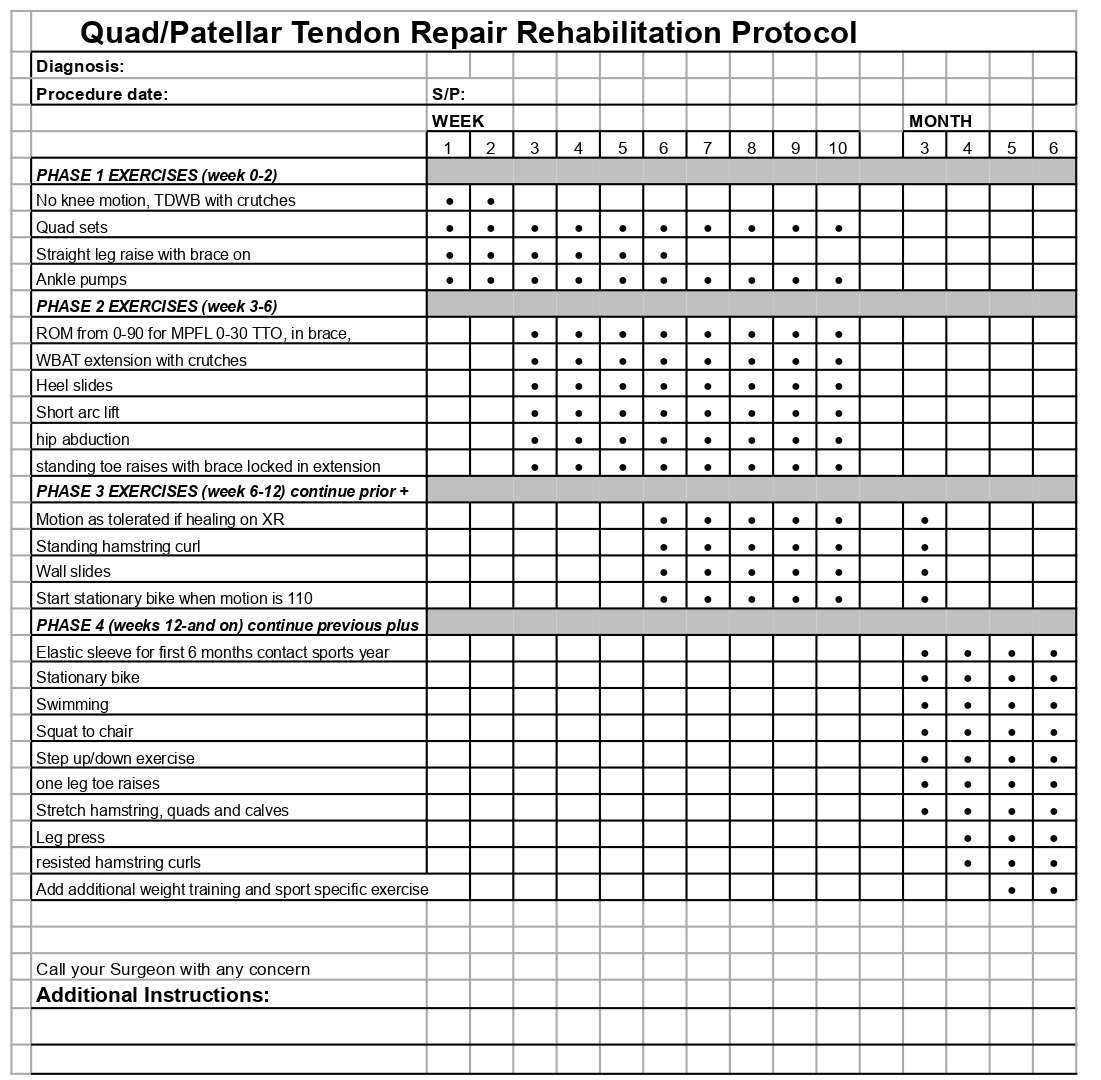
Patellofemoral Syndrome
Rehabilitation for Patellofemoral Syndrome ('chondromalacia patella')
When the knee moves, the kneecap (patella) slides to remain in contact with the lower end of the thigh bone (trochlear groove of the femur). Normally, this motion has almost no friction: the friction between these two joint surfaces is approximately 20% the friction of ice sliding against ice. If the patella and/or femur joint surface (articular cartilage) becomes softened or irregular, the friction increases. Grinding or crepitus that can be heard or felt when the knee moves is the result. This condition in which there is patellofemoral crepitus is called chondromalacia patella or patellofemoral syndrome.
The force, or pressure, with which the patella pushes against the femur is 1.8 times body weight with each step when walking on a level surface. When climbing up stairs, the force is 3.5 times body weight and when going down stairs it is 5 times body weight. When running or landing from a jump the patellofemoral force can exceed 10 or 12 times body weight.
The symptoms of chondromalacia patella are usually pain in the front of the knee that is aggravated by going up and down stairs, sitting for long periods of time with the knees bent (such as in a movie) and when doing deep knee bends.
Pressure between the patella and femur is minimized when the knee is straight or only slightly bent. Exercises and activities that require deep knee bending, jumping and landing, pushing or pulling heavy loads and stopping and starting will place very high stresses on the patellofemoral joint and the patellar tendon.
Treatment
The best treatment for patellofemoral syndrome is to avoid activities that compress the patella against the femur with force. This means avoiding going up and down stairs and hills, deep knee bends, kneeling, step-aerobics and high impact aerobics. Do not wear high heeled shoes. Do not do exercises sitting on the edge of a table lifting leg weights (knee extension).
An elastic knee support that has a central opening cut out for the kneecap sometimes helps. Applying ice packs for 20 minutes after exercising helps. Aspirin, Aleve or Advil sometimes helps.
Sports that aggravate patellar tendinitis and chondromalacia patella: volleyball, basketball, soccer, distance running, racquetball, squash, football, weightlifting (squats).
Sports that may or may not cause symptoms: cycling (it is best to keep the seat high and avoid hills), baseball, hockey, skiing and tennis.
Sports that are easiest on the knees: Swimming (especially with a flutter kick), walking (avoid up and down hills), and cross-country skiing.
Do not do the following exercises:
- lunges
- squats
- stair-stepper machines
- leg extension machine
The following exercises are OK to do if they cause no pain, grinding or swelling:
- straight-leg lifting exercises
- stationary cycle (seat high, resistance low)
- leg press (do not let the knees bend past 90 degrees)
- hamstring curl machine
The following exercise program should be followed as instructed by your Surgeon or your physical therapist. For the straight leg lift and short arc lift, ankle weights can be added to increase resistance and strength of the quadriceps. Generally, after 1 to 2 weeks, ankle weights can be added (starting at 1 pound) and increased by 1 pound per week until you build to 5 pounds. The exercises should be done daily until ankle weights are added. At this time, the straight-leg lift, short-arc lift and wall slides should be done every other day and the stretches should continue daily. When you have built up to 5 pounds on the straight-leg and short-arc lifts, continue the exercises 2 times per week for maintenance.
- Straight Leg Raise- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 15 reps. Add 1-2 pounds to your ankle until you can reach your goal weight of 10-15 pounds.
- Side laying Hip adduction- Lay on side that is affected. Keep your ankle, knee, hip and shoulder in a straight line. Raise the affected leg so that your foot is just past midline. Hold for a count of 6 and repeat 3 sets of 15 reps. Add weight just like #1 until you reach the goal weight of 10-15 pounds.
- 1/4 Squats- Stand with your feet shoulder width apart. Toes pointing straight ahead. Look down at your feet, Lean with your butt first and squat down slowly until your knees pass over your toes then stand back up to start position. Perform 3 sets of 15 repetitions. You may hold dumbbells to add resistance.
- Short Arc Knee Extension- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 15 repetitions. Add weight just like #1 until the goal weight is reached of 10-30 pounds.
- Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lazy-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 15 repetitions.
- Wall Squats- Put your back flat against the wall. Stand with your feet shoulder width apart. Heel approximately 18 inches from the wall. Toes point straight ahead. Slide down the wall until your knee is at a 60 degree angle. Stay in this position for a count of 30. Return to start position. Repeat 3 sets of 15.
- Hamstring Stretch- Perform this stretch in the position illustrated at the right. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for fifteen to twenty seconds and repeat three to five times.
- Quadriceps Stretch- This stretch is performed in the position illustrated at the right. Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold fifteen to twenty seconds for three to five repetitions.
The Posterior Cruciate Ligament
The Posterior Cruciate Ligament (PCL) is the strongest ligament in the knee (2 times as strong as the ACL) and provides a significant amount of knee stability. PCL deficient knees are susceptible to degeneration at the medial femoral compartment and the patello-femoral joint due to the increased translation at these joint surfaces. The PCL is approximately 38mm in length and 13mm wide. It runs from the medial femoral condyle to the posterior tibia. It is composed of two distinct bands (anterolateral and posteromedial) and is closely connected to the menisco-femoral ligament. The bands are named with respect to their anatomic location with the femoral insertion specified first followed by the tibial insertion. The anterolateral band is twice as large as the posteromedial band and 1.5 times stronger. It becomes taut with knee flexion whereas the posteromedial band tightens with knee extension.
The PCL provides 95% restraint to posterior tibial translation and acts as a secondary restraint to tibial external rotation, varus, and hyperextension. With PCL rupture, there is an increased posterior translation when a posterior load is applied to the tibia and this translation increases as knee flexes with maximum translation from 70-90°, where the ACL is on full slack. Isolated PCL tears are uncommon due to the strength of the PCL.
There is much debate as to whether one should reconstruct a ruptured PCL or opt for conservative treatment. Many studies have shown that isolated PCL tears do well with conservative treatment. Conservative treatment of the PCL should focus on quadriceps rehab and protective weight bearing. Hamstring activity should be restricted due to the posterior pull the hamstrings elicit on the tibia. Quad activity helps counteract this posterior pull and should be addressed aggressively. Open kinetic chain activities are advised from 60-0° and closed chain activities from 0-60°. The therapist must watch for patellar pain due to the increased tibial drop back present with a ruptured PCL. The therapist must also be aware that the lateral structures of the knee act as secondary stabilizers to posterior translation and need to be guarded initially.
Overview
The Posterior Cruciate Ligament or PCL, and the Anterior Cruciate Ligament (ACL), limit the motion of the tibia backward and forward, respectively.
The lateral collateral ligament (on the outside of the knee) and the medial collateral ligament (on the inside of the knee) limit side-to-side knee motion. Fifty percent of PCL injuries occur in conjunction with other knee ligament injuries, while the other 50 percent occur alone and are referred to as isolated PCL injuries. PCL tears usually result from high force impacts, generally vehicular accidents or contact sports such as football, soccer, or hockey. PCL injuries also can occur in non-contact sports, such as gymnastics or skiing, but are much less common.
A PCL injury usually occurs during a direct hit below the knee while the leg is bent. In other cases, you may land directly on a bent knee, driving the tibia up and behind the knee and tearing the PCL. Extreme hyperextension of the leg (straightening beyond the normal limit) is a third type of trauma that may result in tears to the PCL and other knee ligaments.
If untreated, a torn PCL can change knee mechanics, resulting in abnormal motion and subsequent pain and instability. Over years, this wear and tear can lead to progressive degenerative arthritis.
Diagnosis
Symptoms of PCL injuries include:
- Marked, immediate swelling (within three hours of injury)
- Difficulty in walking after the injury
- Pain when moving the knee
- An occasional feeling of instability or the knee "giving way"
Unlike the "pop" and severe pain that may occur with a torn ACL, an isolated PCL injury may manifest itself simply as swelling in the knee that subsides over a few days or weeks. In many cases, patients may overlook the initial injury and fail to visit a doctor or specialist for evaluation. Unlike ACL injuries, isolated PCL injuries may not initially limit knee function, allowing you to return to normal activities.
Diagnosis of a PCL injury begins with an extensive history to learn how the injury occurred. The doctor must determine what position the leg was in at the time of injury and whether the injury involved contact or a noncontact mechanism (for example, twisting). In an acute, isolated PCL injury, there is usually a history of mild pain and swelling. If the PCL and other knee ligaments are torn, the knee is severely swollen and the person is completely disabled.
Once a thorough history is obtained, the examiner performs a physical exam of the knee to assess the stability of the ligaments. Using specific tests, the physician can diagnose PCL injuries by applying forces to the knee and feeling for abnormal motion.
The examiner also must assess other knee ligaments to rule out combined ligament injuries. In severe, multiple ligament injuries, nerves and blood vessels also may be damaged. These injuries must be evaluated immediately by a doctor.
It is difficult at times to completely assess all the damage that may have occurred in conjunction with a PCL injury. In this case, obtaining additional studies such as magnetic resonance imaging (MRI) exams can be very helpful. Magnetic resonance can show the ligaments, cartilage, and bone to give an accurate picture of the extent of the injury.
Posterior Cruciate Ligament Reconstruction
This protocol is a guideline for your rehabilitation after posterior cruciate ligament reconstruction. You may vary in your ability to do these exercises and to progress from one phase to the other. Please call Greater Michigan Orthopedics if you are having a problem with your knee or if you need clarification of these instructions.
PHASE I: 0 – 2 weeks after surgery
You will go home with a knee brace, crutches, possibly a cryocuff cold therapy unit machine.
GOALS:
- Protect the reconstruction – avoid falling
- Ensure wound healing
- Attain and maintain full knee extension
- Gain knee flexion (knee bending) to 90 degrees
- Decrease knee and leg swelling
- Promote quadriceps muscle strength
- Avoid blood pooling in the leg veins
ACTIVITIES:
BRACE/CRUTCHES
For the first two weeks after surgery, your knee brace will be locked in extension (straight). Use the brace when walking. You will be asked to use crutches to walk after surgery. You will be instructed in partial weight bearing with the crutches for at least the first 6 weeks after surgery. Your doctor will give special instructions in some cases. Remove the brace for exercises.
CRYOCUFF (COLD APPLICATION)
If you are experiencing pain, swelling, or discomfort, we suggest icing for 15-20 minutes with at least a 60-minute break in between. Use your cryocuff or place ice in a zip lock bag and/or in a towel and apply to the injured area. Never place ice directly on the skin.
WOUND CARE
Remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri strips) across the incision. You can wrap an elastic bandage (ace) around the knee at other times to control swelling. You may now shower and get your incision wet, but do not soak the incision in a bathtub or Jacuzzi until the stitches have been removed.
ASPIRIN / ELASTIC STOCKINGS
Take an aspirin each morning; optional to wear elastic stocking (TED) below the knee for 2 weeks, to help prevent phlebitis (blood clots in the veins).
FREE/MACHINE WEIGHTS — Upper Body/Trunk Only
We suggest that you do not use any lower extremity free or machine weights. If you are doing free or machine weights for the upper body and trunk, we suggest a very light resistance of 3 sets of 15-20 repetitions. Do not place yourself in a compromising position with your recently operated knee. Do not do exercises while standing. Use a bench or chair to support your body weight.
EXERCISE PROGRAM
- You can start formal physical therapy about 3 to 5 days after the operation.
- We ask that your PT follow our written protocol.
- If your PT has questions, please ask them to call us to discuss them.
Days per week: 5-7 Times per day: 1-2
| Quadriceps set | 3 sets of 10 reps |
| Heel prop | 5 minutes |
| Sitting Heel slides | 3 sets of 10 reps |
| Straight leg raise | 3 sets of 10 reps |
| Patellar mobilization | 1-3 sets of 3 minutes |
| Hip abduction | 3 sets of 10 reps |
| Ankle pumps | 10 pumps per hour |
Quad Sets- Isometric exercise. This can be done where ever the knee is straight. (laying in bed, standing, or reclined in the lazy-boy) Tighten up your thigh muscle as tight as you can make it. Hold for a count of 10. Relax and repeat 3 sets of 10 repetitions.
HEEL PROP- to straighten (extend) the knee. Lie on your back with a rolled up towel under your heel or sit in a chair with the heel on a stool as shown in the figure. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a weight (2 to 5 pounds) on the thigh, just above the kneecap. Try to hold this position for 5 minutes, three times a day. While maintaining this extended position, practice quadriceps setting.
SITTING HEEL SLIDES - to regain the bend (flexion of the knee). See figure in phase 1. While sitting in a chair or over the edge of your bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the nonoperative leg controlling, allowing the knee to bend but DO NOT exceed 90 degrees of bend at the knee. Hold five seconds and slowly relieve the stretch by lifting the foot upward, helping with the uninvolved leg, to the straight position (passive assist).
STRAIGHT LEG RAISE- Lay flat on back, unaffected knee bent to 90 degrees. Keep involved leg straight and raise it so that your thighs are equal. Hold for count of 6. Perform 3 sets of 10 reps.
PATELLAR MOBILIZATION
Inferior Glide - With thumbs on upper border of kneecap, gently push your knee cap towards your foot. Hold 5 sec.
Superior Glide - With thumbs on lower border of kneecap, gently pull kneecap towards your body. Hold 5 sec.
Medial Glide - Utilizing a pincer grip, grab the inside and outside edges of your kneecap and gently push your kneecap in towards your other leg. Hold 5 sec.
Lateral Glide - Utilizing a pincer grip, grab the inside and outside edges of your kneecap and gently push your kneecap out. Hold 5 sec.
HIP ABDUCTION- Lie on your non operative side. Keep the knees fully extended. Raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, and then lower slowly.
ANKLE PUMPS - to stimulate circulation in the leg. You should do at least 10 ankle pump exercises each hour.
OFFICE VISIT
Please return to your Surgeon approximately two weeks after your surgery. At this time, your sutures will be removed and your progress will be checked.
Posterior Cruciate Ligament Reconstruction
PHASE 2: 2 – 6 weeks after surgery
Goals:
- Protect the reconstruction, avoid falling
- Ensure wound healing
- Maintain full knee extension (straighten knee fully)
- Begin quadriceps muscle strengthening
- Attain knee flexion of 90 degrees or more
- Decrease knee and leg swelling
- Protected gait with crutches and partial weight bearing
ACTIVITIES
Motion- It is important to work on regaining your motion by simply moving your knee. It is very important to regain full extension during this time period.
Cryocuff - Use the cryocuff or ice bags to decrease swelling for 20 minutes three times a day after each exercise session.
Brace / Crutches - Always wear the post-operative brace when walking in extension. (the brace should be set to allow full extension and 60 degrees of flexion for weeks 2-4 and 90 degrees of flexion at 6 weeks). Always use your crutches and bear only partial weight on the operated leg. Follow these instructions until you return for your follow-up with your doctor at six weeks after surgery.
Swelling - You may continue using the elastic stockings (TED) for the lower leg and wrapping the knee with an elastic bandage (ACE) to control swelling.
Exercise Program
Stationary Bicycle
Utilize a stationary bicycle to move the knee joint and increase knee flexion. If you cannot pedal all the way around, then keep the foot of your operated leg on the pedal, and pedal back and forth until your knee will bend far enough to allow a full cycle. Use the non-operated ('good') leg to move the pedals while your operated (PCL) leg just travels around as a 'passenger'. Most people are able to achieve a full cycle revolution backwards first, followed by forward. You may ride the cycle with no resistance for up to 10-15 minutes, 1 to 2 times a day. Set the seat height so that when you are sitting on the bicycle seat, your knee is fully extended with the heel resting on the pedal in the fully bottom position. You should then actually ride the bicycle with your forefoot resting on the pedal.
RANGE OF MOTION AND STRENGTHENING EXERCISES (brace off)
Days per Week: 5-7 Times per Day: 1-2
| Quadriceps Sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Heel slides with towel assist | 1 set of 5 to 15 minutes |
| Straight leg raises | 1-2 sets of 15-20 reps |
| Short arc lift | 3 sets of 10 |
| Standing toe-raises | 3 sets of 10 |
| Prone hip extension | 3 sets of 15 |
| Hip abduction | 3 sets of 10 |
HEEL SLIDES - to regain the bend (flexion) of the knee. While lying on your back, actively slide your heel backward to bend the knee. Keep bending the knee until you feel a stretch in the front of the knee. Hold this bent position for 5 seconds and then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise.
SHORT ARC LIFT- Place 2-3 towels rolled up under the knee to the affected knee. This will have the knee bent to 30 degrees. Bring the leg up into full extension. Hold for a count of 6 and repeat 3 sets of 10 repetitions.
STANDING TOE RAISES- Stand facing a wall, hands on the wall for support and balance. Keep the knees extended fully. Tighten the quadriceps to hold the knee fully straight. Raise up on 'tip-toes' while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position.
PRONE HIP EXTENSION- Lie face down as shown in the illustration. Keep the knee fully extended. Tighten up your glutes and lift your leg off the ground.
OFFICE VISIT
Please return to Dr. Nelson's office approximately 6 weeks after your surgery.
Posterior Cruciate Ligament Reconstruction
PHASE 3: 6-12 weeks after surgery
Goals
- Protect the reconstruction, avoid falling
- Ensure wound healing
- Maintain full knee extension (straighten knee fully)
- Begin quadriceps muscle strengthening
- Attain knee flexion of 90 degrees or more
- Decrease knee and leg swelling
- Return to normal walking without crutches
ACTIVITIES
Cryocuff - Use the cryocuff or ice bags as needed to decrease swelling for 20 minutes.
Brace / Crutches - You can discontinue use of the brace and crutches according to Dr. Nelson's instructions.
Exercise Program
Stationary Bicycle- Continue to use daily for 20-30 minutes.
Range of Motion and Strengthening Exercises (brace off)
For the straight leg raise, hip abduction and prone hip extension, if the exercise can be performed easily after the first week, then an ankle weight may be used to increase the resistance of the exercise and build strength. Start with 1 pound and add 1 pound per week until you reach 5 pounds. Do the exercises daily for the first week, and then decrease to every other day when using ankle weights.
Days per week: 5 Times per day: 1-2
| Quadriceps Sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Heel slides with towel assist | 1 set of 5 to 15 minutes |
| Straight leg raises | 1-2 sets of 15-20 reps |
| Short arc lift | 3 sets of 10 |
| Standing Hamstring Curl to 45 degrees | 3 sets of 10 |
| Standing toe-raises | 3 sets of 10 |
| Prone hip extension | 3 sets of 15 |
| Hip abduction | 3 sets of 10 |
| Wall Slides | 3 sets of 10 |
STANDING HAMSTRING CURLS- Stand facing the wall, using the wall for balance and support. While standing on the non operative limb, bend the knee of the operated side and raise the heel toward the buttock only to 45 degrees. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated.
WALL SLIDES - Stand upright with your back and buttocks touching a wall. Place the feet about 12 inches apart and about 6 inches from the wall. Slowly lower your hips by bending the knees and slide down the wall until the knees are flexed about 45 degrees (illustration). Pause five seconds and then slowly slide back up to the upright starting position.
OFFICE VISIT
Please return to your Surgeon approximately 12 weeks after your surgery.
Posterior Cruciate Ligament Rehabilitation Protocol
PHASE 4: 12 to 16 weeks after surgery
Goals:
- Protect the reconstruction; avoid falling.
- Maintain full knee extension.
- Attain full knee flexion.
- Walk with a normal heel-toe gait with no limp.
- Muscle strength and conditioning improvements.
Activity
Brace / Crutches- The brace and crutches are usually discontinued after you see the doctor at your 6-week post-operative office visit. Concentrate on walking with a heel-toe gait without a limp.
Cryocuff- Continue to use the cryocuff or ice bags, as needed, for 20 minutes after each workout.
Knee Support - Buy an elastic knee sleeve (made of neoprene rubber) at a sporting goods store. It should have an opening for the kneecap and velcro straps but does not need hinges on the sides. Use this support if you are on your feet for a prolonged period of time.
Stationary Bicycle - Continue to use daily for 20-30 minutes.
Swimming - You may begin swimming at this time, if available, using only the flutter kick and doing the freestyle and backstroke. Do not swim breast-stroke, butterfly or side-stroke yet. Swimming with a kick-board is safe as long as the flutter-kick is used. You can swim up to 15 to 20 minutes, 3 to 4 times per week.
Exercises
Days per week: 3 to 5 Times per day: 1
| Quadriceps Sets | 1-2 sets of 15-20 reps |
| Heel prop | 5 minutes |
| Heel slides | 1 set of 5 to 15 minutes |
| Straight leg raises | 1-2 sets of 15-20 reps |
| Short arc lift | 3 sets of 10 |
| Standing Hamstring Curl to 45 degrees | 3 sets of 10 |
| Standing toe-raises single leg | 3 sets of 10 |
| Prone hip extension | 3 sets of 15 |
| Hip abduction | 3 sets of 10 |
| Wall Slides | 3 sets of 10 |
Stretching Exercises
Days per week 5-7 Time per day 1
| Hamstring stretch | 3-5 reps holding 15-30 seconds |
| Quadriceps stretch | 3-5 reps holding 15-30 seconds |
| Calf Stretch | 3-5 reps holding 15-30 seconds |
Hamstring Stretch - Perform this stretch against a table or chair. Bend slowly forward at the hips, keeping the knee fully extended until you feel gentle stretch in the back of your thigh and knee. Hold the stretch for 15 to 20 seconds and repeat 3 to 5 times.
Quadriceps Stretch - This stretch is performed on your stomach or standing. Lean gently backward as if bringing your heel toward the buttock. When a stretch is felt in the front of the thigh and knee, hold 15 to 20 seconds for 3 to 5 repetitions.
Calf/Achilles Stretch - Keep the heel flat on the floor and the knee fully extended. Lean forward at the hips with the arms supporting your weight. When you feel a gentle stretch in the back of your calf and knee, hold for 15 to 20 seconds, 3 to 5 repetitions.
Optional Additional Weight Training
Days per week: 2-3 Times per day: 1 3 sets of 20 reps
- Seated leg press
- Hamstring curl
- Hip abductor/adductor machine
- Roman chair
- Calf raise machine
- Hip flexor machine
SINGLE LEG STRENGTHENING PROGRESSION
At this time, it is important to begin the development of single-leg strength. Begin to follow the "Progression for Single Leg Strengthening" included in this packet if you are able to do the exercises without pain. The instructions estimate a time period of 10 to 12 weeks for you to progress through the whole program. This time line will vary for different people and knees, depending upon the presence of other knee problems. Again, limit flexion of the knee to 60 degrees or less during these exercises.
Precautions When Exercising
- Avoid pain at the surgical incision site
- Avoid pain and/or crepitus at the patella
- When using a leg press machine, squatting or doing wall slides, limit the flexion of the knee to 60 degrees or less to avoid over stressing the PCL graft.
- Build up resistance and repetitions gradually
- Perform exercises slowly avoiding quick direction change and impact loading
- Exercise frequency should be 2 to 3 times a week for strength building
- Be consistent and regular with the exercise schedule
Principles of Strength Training
- Warm-up prior to exercising by stationary cycling or other means
- You are "warmed-up" when you have started sweating
- Gently stretch all muscle groups next
- Do exercises involving multiple muscle groups first and individual muscle groups last
- Do aerobic workouts after strength workouts
- Cool-down by stretching after finishing exercise
DO NOT do any of the following exercises:
- Knee extension using a weight lifting machine
- Resisted Hamstring curls or hamstring weight machine
- Lunges
- Step exercises with impact
- Running sprint until progressed
- Jumping
- Pivoting or cutting
OFFICE VISIT
Please make an appointment to see your Surgeon at six months after surgery.
Posterior Cruciate Ligament Rehabilitation Protocol
Phase 5: from the 16th week onward
Goals:
- Regain full muscle strength.
- Work on cardiovascular conditioning.
- Do sports-specific training.
ACTIVITIES
Muscle-Strengthening Exercises
You should continue muscle-strengthening exercises from Phases 2 and 3 three times a week. You can now decrease the number of repetitions per set from 15 to 10. This will allow you to work with heavier weights. Remember to do all exercises slowly with good form. Weights can be increased when you can do a particular weight easily for 3 sets of ten repetitions for 3 consecutive workouts.
Cardiovascular Conditioning
Use Nordic track, stationary bicycle, rowing machine or swimming workouts to build cardiovascular fitness. Three to five times per week for 20 to 30 minutes is sufficient for improvement in conditioning. Excessively long duration cardiovascular exercise can retard or delay muscular strength development. Strength improvement and gains in muscle size are your primary goals at this time.
Sports-Specific Training
To reach your ultimate goal of returning to sports participation, you must follow an orderly sequence of drills which are designed to re-train coordination that is necessary to provide the proper control of your knee. The following time-table gives an approximate sequence for returning to activities:
| Sport | Months Post-Operative |
|---|---|
| Golf | 4-5 |
| Running | 5 |
| Tennis | 6 |
| Sprinting | 6 |
| Running with quick starts and stops | 7 |
| Backward running | 7 |
| Circle running | 7 |
| Carioca | 7-8 |
| Hopping and jump training | 8-9 |
| Quick pivoting and cutting | 8-9 |
| Full return to sport | 9 |
Progressive Resistance Exercise (PRE) Principle
- To build muscle strength and size, the amount of resistance used must be gradually increased.
- The exercises should be specific to the target muscles.
- The amount of resistance should be measurable and gradually increased over a longer period of time.
- To avoid excess overload and injury, the weight or resistance must be gradually increased in increments of 5-10%.
- Resistance can be increased gradually every 10-14 days when following a regular and consistent program.
- Adequate rest and muscle recovery between workout is necessary to maximize the benefit of the exercise.
- If the PRE principle is followed too strictly, the weights potentially will go higher and higher.
- At a certain point, the joints and muscles will become overloaded and injury will occur.
- This eventuality can be avoided by refraining from using excessive weight during strength training.
Basic Knee Strengthening Program (weeks 18 to 24)
Frequency 2-3 times per week Sets: 3 Reps per set: 10-15
—Emphasis is to build muscle strength using BOTH legs
—Progress according to the PRE principle
Basic Program Exercises:
- Leg press
- Standing hamstring curl with ankle weights
- Wall slides (hold dumbbells for resistance)
- Roman Chair (strengthens hamstrings)
- Chair squats (hold dumbbells for resistance)
- Calf Raises
- Hip abductor/Adductor machine
- Step Up/Down Progression
In general, the basic knee program is good for most people who are active recreationally, but who do not participate in running and jumping sports. For people who will participate in running and jumping sports, the following Advanced knee strengthening program can be used to develop a higher level of knee strength.
Advanced Knee Strengthening Program (Week 24 onward)
Frequency 2-3 times per week Sets: 3 Reps per set: 10-15
—Emphasis is to continue to build muscle strength using both legs and progress to Advanced Exercises using the Single Leg.
—Advanced single leg exercises are integrated with the exercises from the Basic Knee Strengthening Program.
The following single leg drills are integrated into the workout on a rotating basis:
- Step Up/Down
- Single leg wall slide
- Single leg squat
So that the Advanced Knee Strengthening Program would be as follows:
- Leg Press
- Hamstring curl machine (limit knee flexion to 60 degrees)
- Wall slides (hold dumbbells for resistance)
- Roman Chair (strengthens hamstrings)
- Chair squats (hold dumbbells for resistance)
- Calf Raises
- Step Up/Down Progression
- Alternate workouts with single leg wall slide and single leg squat
—When starting the new single leg drills, start with 3 sets of 5 and add one rep per set, per workout until you can do 3 sets of 10.
—When 3 sets of 10 are achieved easy and pain free, then you can hold the dumbbells to increase resistance and strength.
Once these have been achieved, sports specific drills can be added at the discretion of the therapists or your Surgeon.
OFFICE VISIT
Please set up an appointment to see your Surgeon at 9 months post operative prior to clearance to return to sport.
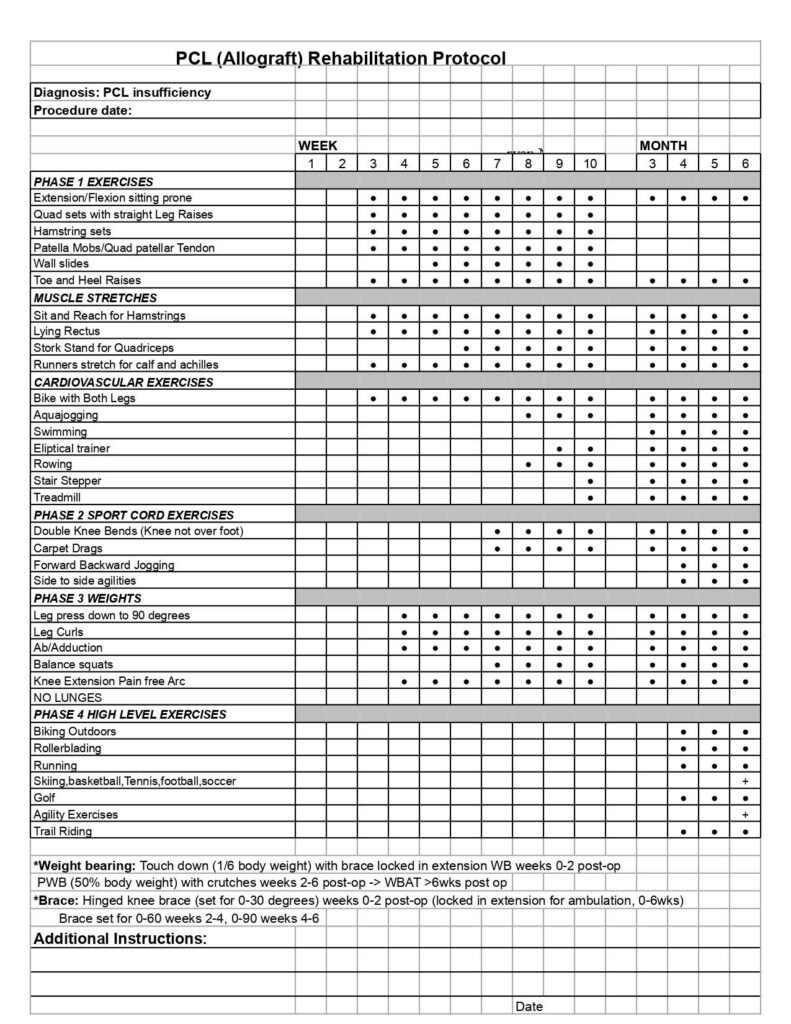
Total Knee Arthroplasty Protocol
Joint Replacement Discharge Instructions
PAIN/SWELLING/STIFFNESS MANAGEMENT
To decrease swelling and pain:
- Follow medication instructions and elevate extremity when resting to keep pain at tolerable level.
- Lay down in bed at least 2-3 times a day, elevating your affected leg for 30 minutes with 3 pillows, and alternate using cold therapy for at least 20 minutes.
- Expect bruising to appear within the first week.
DRESSING/INCISION CARE
Your dressing will help to keep your incision protected, even in the shower.
- Remove your Aquacell dressing on (POD7) Date: _______________.
- To remove, pull the edges to stretch before removing.
- AVOID INFECTION by washing your hands before touching your incision and using clean washcloths and towels.
- DO NOT put another dressing on.
- DO NOT submerge the incision in any type of water until your surgeon approves.
Call your surgeon's office FIRST if:
- Swelling and pain are NOT controlled by elevating your leg, using cold packs, and taking pain medication. Excessive swelling and calf tenderness, unrelieved by pain medication and elevation, may be signs of blood clot and need evaluation.
- Fluid/drainage or change in fluid/drainage from the incision site BEYOND 7 days after your surgery.
Go to the Ascension Genesys Emergency Room if:
- You have chills, sweating, or shivering, and your temperature is ABOVE 101 degrees F.
- If you are having a hard time breathing or you become confused. These are signs of infection or a blood clot and can be life threatening.
Surgeon's Name: _________________________ Phone #: ____________________________
Please reference your Joint Replacement Guidebook to review other important information regarding: After surgery exercise plan, Signs and symptoms of a blood clot and/or Pulmonary Embolus (PE).
Pain Management
Adequate pain control after TKA is important in expediting patient progress with mobility and range of motion after surgery. This in turn may result in a shorter hospital stay and improved patient satisfaction.
Pain management following TKA is multimodal and may include:
- Pre-operative dose of medications including Acetaminophen and/or Celebrex.
- Spinal or epidural analgesia – Administered as a one-time dose, lasting 6-8 hours. Intrathecal opioids may be added to the anesthetic cocktail. Side effects of epidural injection may include low blood pressure and decreased motor function.
- Peripheral nerve blocks – Adductor canal nerve blocks may be administered as a for a period following surgery, typically lasting 6-8 hours. Potential side-effects may include nerve damage and a lack of muscle control in the immediate post-operative period.
- IV or oral analgesics – See chart below to help.
- Local analgesics - intra-articular or periarticular injections during TKA surgery may be used for post-operative pain control and to improve range-of-motion (ROM).
| Check if ordered | Pain Medication Name & Dose | Next Dose Due | Day 1 after discharge | 2nd Day | 3rd Day | 4th Day | 5th Day | 6th Day | 7th Day | 8th Day |
|---|---|---|---|---|---|---|---|---|---|---|
| □ | Tylenol (acetaminophen): Take two 500 mg pills | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | □8am □2pm □8pm | |
| □ | Mobic: Take one 15mg pill | □With 1st meal | □With 1st meal | □With 1st meal | □With 1st meal | □With 1st meal | □With 1st meal | □With 1st meal | □With 1st meal | |
| □ | Oxycodone: 5mg | Take one pill every 4 to 6 hours, if needed for pain | ||||||||
Starting Day 9: Begin taking pain medications ONLY as needed.
Blood Clot Prevention: Take ASA 81mg as prescribed. (over the counter baby aspirin) Daily for one month.
Prevention of Constipation:
- Take 1 dose of Miralax x1 per day. Keep taking each day until you are no longer taking narcotic medications or if you start having frequent bowel movements.
- If no bowel movement for 3 days, take "over the counter" Docusate Sodium as per directions on the bottle or package insert.
- If no bowel movement the day after taking Docusate Sodium, take an "over the counter" stimulant laxative such as Dulcolax or Senokot, or Ex-Lax according to directions on the bottle or package insert.
Phase I – Immediate Post Surgical Phase (Day 0-3)
The goal of physical therapy intervention during the early post-operative phase is to decrease swelling, increase range of motion, enhance muscle control and strength in the involved lower extremity and maximize patients' mobility with a goal of functional independence. Physical therapy interventions are also directed towards identifying other sensomotor or systemic conditions that may influence a patients' rehabilitation potential.
Goals:
The patient will:
- Perform bed mobility and transfers with the least amount of assistance while maintaining appropriate precautions.
- Ambulate with an assistive device for 25-100 feet and ascend/descend stairs to allow for independence with household activities while maintaining appropriate WB.
- Regain at least 80 degrees of passive and active range of motion in the knee to perform sit to stand transfers with minimal compensatory activity.
- Gain knee extension less than or equal to -10 degrees.
- Independently perform operative extremity Straight Leg Raise (SLR) exercise.
- Verbalize understanding of post-operative activity recommendations/precautions including use of proper positioning of the lower extremity, range of motion and strengthening exercises.
- Patients will also be educated on superficial massage of the knee joint to minimize hypersensitivity following surgery.
Observation and Assessment:
- Observe for any signs of deep vein thrombosis (DVT): increased swelling, erythema, calf pain.
- If a large amount of drainage is present, or there is blistering or frail skin around the knee joint or the lower extremities, discuss with the nurse and decide if notifying the surgical team is indicated.
- Assess patients' pain using the visual analogue scale. Ensure that patients are premedicated with oral/IV pain medication 30-60 minutes prior to treatment. Cryotherapy is recommended following physical therapy treatment to reduce pain, discomfort and swelling in the knee joint.
Therapeutic exercise and functional mobility:
- Active/active assisted/passive (A/AA/PROM) exercises (seated and supine).
- Patella femoral and tibial femoral joint mobilization and soft tissue mobilization as indicated.
- Soft tissue massage not over incision ever! Sutures dissolve on their own and don't need help.
- Isometric quadriceps, hamstring, and gluteal isometric exercises.
- Straight leg raises (SLR).
- Lower extremity range of motion (ROM) and strengthening as indicated based on evaluation findings.
- Closed chain exercises (if patient demonstrates good pain control, muscle strength and balance). Close-chained exercises should be performed with bilateral upper extremity support while maintaining appropriate WB precautions.
- Gait training on flat surfaces and on stairs.
- Transfer training.
Modalities:
- Continuous Cryotherapy for 72 hours after surgery, or at least 5 times/day.
- Patients are encouraged to use cryotherapy for 20 minutes before and after their independent exercise program.
Precautions:
- Weight bearing as tolerated (WBAT) with assistive device (unless indicated otherwise by the surgeon) to full weight bearing.
- Monitor wound healing and consult your surgeon if signs and symptoms of excessive bleeding and poor incision integrity are present.
- Monitor for signs of DVT, pulmonary embolism (PE), and/or loss of peripheral nerve integrity. In these cases, notify your surgeon or his team immediately.
- No exercises with weights or resistance.
- Avoid torque or twisting forces across the knee joint especially when WB on involved limb.
Positioning:
- A trochanter roll may be used as needed to maintain neutral hip rotation and promote knee extension.
- A towel roll should be placed at the ankle to promote knee extension when patients are supine in bed. Extension is the most important at this stage!
- Nothing should be placed behind the operative knee, to promote maximal knee extension and prevent knee flexion contracture.
Criteria for progression to the next phase:
- Ability to demonstrate Quadriceps contraction and/or perform a straight leg raise (SLR).
- Active knee range of motion (AROM) 0°-80°.
- Minimal pain and inflammation.
- Independent transfers and ambulation at least 100 feet with appropriate assistive device.
Phase II – Motion Phase (Day 3 – Week 6)
Goals:
- Improve knee active range of motion (AROM) to >/= 0-110 degrees.
- Muscle strengthening of the entire operative extremity with emphasis on knee extensor and flexor muscle groups.
- Attention should also be directed toward any weakness present in the operative extremity as well as, any generalized weakness in the upper extremities, trunk or contralateral lower extremity.
- Proprioceptive training to improve body/spatial awareness of the operative extremity in functional activities.
- Endurance training to increase cardiovascular fitness.
- Functional training to promote independence in activities of daily living and mobility.
- Gait training: Assistive devices are discontinued when the patient demonstrates adequate lower extremity strength and balance during functional activities (usually 1-4 weeks).
- Decrease inflammation/swelling.
- Return to functional activities.
Therapeutic Exercises:
Weeks 1-4
- AA/A/PROM, stretching for flexion (>90 degrees) and extension.
- Stationary Bicycle for ROM, begin with partial revolutions then progress as tolerated to full revolutions (no resistance).
- Patella femoral and tibial femoral joint mobilization as indicated.
- Continue isometric quadriceps, hamstring, and gluteal isometric exercises.
- Supine heel slides and seated Long Arc Quad (LAQ).
- SLR in 4 planes (flexion, abduction, adduction, extension).
- Neuromuscular electrical stimulation (NMES) for quads if poor quad contraction is present. NMES parameters to be set based on goal of exercise/activity. See neuromuscular electrical stimulation procedural standard of care for specific details.
- Gait training to improve function and quality of involved limb performance during swing through and stance phase. Patients are encouraged to wean off their assistive device at the latest by the end of second week from surgery.
- Postural cues/reeducation during all functional activities as indicated.
Weeks 4-6
- Continue above exercises.
- Continue patella femoral and tibial femoral joint mobilization as indicated.
- Continue NMES of quads if poor muscular performance of quad is present. May progress NMES use from isometric quad activity to isotonic and functional activity.
- Front and lateral step up and step down.
- 1/4 front lunge.
- Use sit to stand and chair exercises to increase knee flexion during functional tasks.
- Continue stationary bicycle for ROM.
- Begin pool program if incision is completely healed if available.
*Note: Exercises with resistance may be initiated as tolerated for operative extremity after goals for the first phase have been met, and the patient has met criteria for progression to the next phase.
Modalities:
- Cryotherapy 1-3x/day for swelling and pain management.
- Other modalities at the discretion of the therapist based on clinical findings.
Precautions:
- WBAT with assistive device as needed to minimize compensatory gait. Patient may be encouraged to use a straight cane within one week of surgery if he/she is WBAT to FWB. Patients may be weaned from assistive device by 2 weeks if they did not use an assistive device preoperatively and post-operative muscle performance is adequate for weight acceptance.
- Monitor wound healing and consult with referring MD if signs and symptoms of infection are present.
- Monitor for increased edema and continue with cryotherapy as needed.
Criteria for progression to the next phase:
- AROM 0-110°.
- Good voluntary quadriceps control.
- Independent ambulation community distances (>/= 800 feet), without assistive device, deviations or antalgia.
- Minimal pain and inflammation.
Phase III – Intermediate phase (week 7-12)
Goals:
- Maximize post-operative ROM (0-115 degrees plus).
- Good patella femoral mobility.
- Good strength all lower extremity musculature.
- Return to most functional activities and begin light recreational activities (i.e. walking, pool program).
Therapeutic Exercises:
- Continue exercises listed in Phase II with progression including resistance and repetitions. It is recommended to assess hip/knee and trunk stability at this time and provide patients with open/closed chain activities that are appropriate for each patient's individual needs.
- Continue patella femoral and tibial femoral joint mobilization as indicated.
- Initiate endurance program, walking and/or pool.
- Initiate and progress age-appropriate balance and proprioception exercises.
- Discontinue NMES of quads when appropriate quad activity is present.
Criteria for progression to next phase:
- AROM without pain, or plateaued AROM based on preoperative ROM status.
- 4+/5 muscular performance based on MMT of all lower extremity musculature.
- Minimal to no pain or swelling.
Phase IV – Advanced strengthening and higher level function stage (week 12-16)
Goals:
- Return to appropriate recreational sports/activities as indicated.
- Enhance strength, endurance and proprioception as needed for activities of daily living and recreational activities.
Therapeutic Exercises:
- Continue previous exercises with progression of resistance and repetitions.
- Increased duration of endurance activities.
- Initiate return to specific recreational activity: golf, doubles tennis, progressive walking or biking program.
Criteria for Discharge:
(These are general guidelines as patients may progress differently depending on previous level of function and individual goals.)
- Non-antalgic, independent gait.
- Independent step over step stair climbing.
- Pain-free AROM.
- At least 4+/5 muscular performance based on MMT of all lower extremity musculature.
- Normal, age appropriate balance and proprioception.
- Patient is independent with home exercise program.
Ryan Nelson
861 Health Park Blvd.
Grand Blanc, MI 48439
(810) 953-0500
www.DrRNelson.com
ryan.Nelson@DrRNelson.com
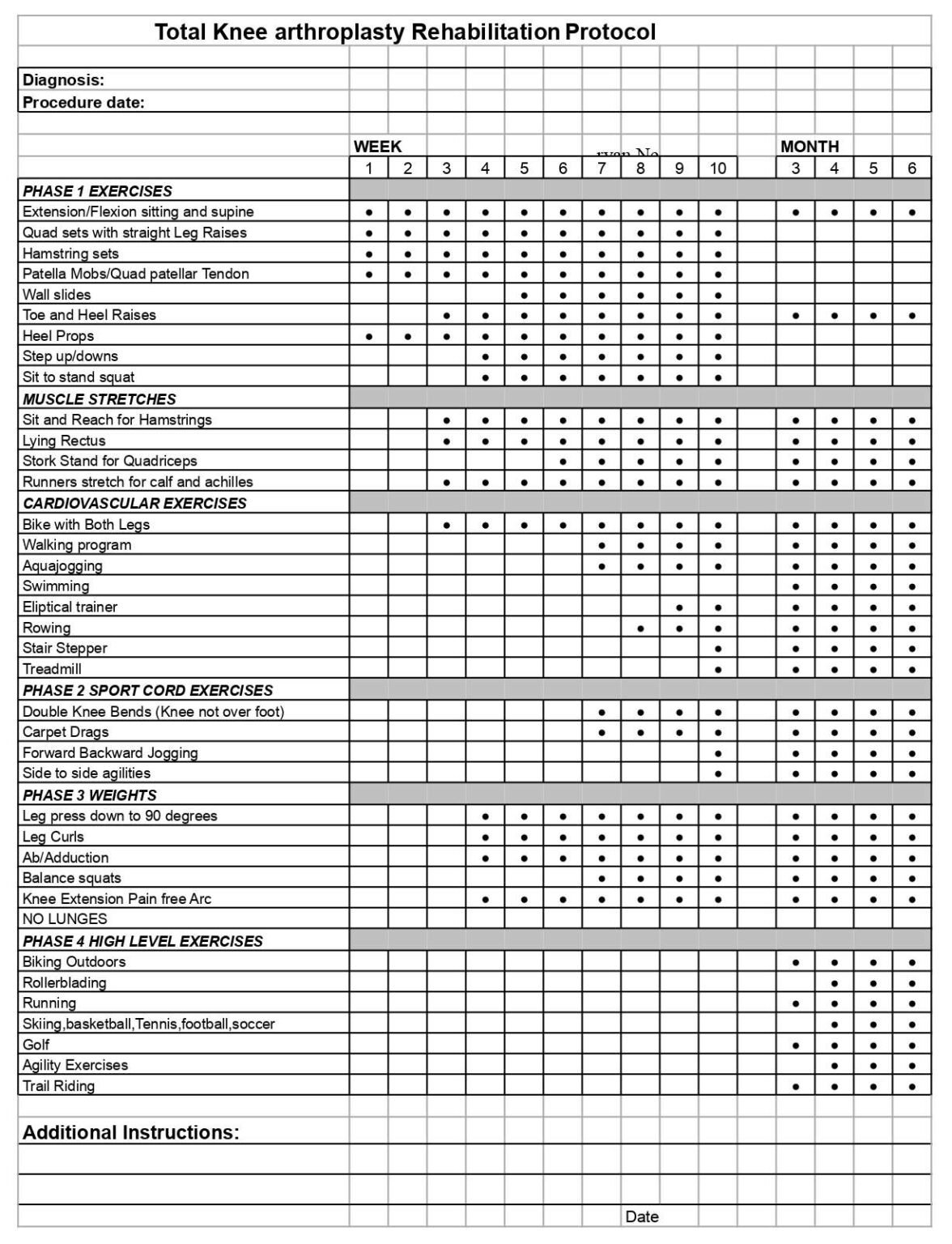
Phase IV – Advanced Strengthening and Higher Level Function Stage (week 12-16)
Goals:
- Return to appropriate recreational sports/activities as indicated.
- Enhance strength, endurance and proprioception as needed for activities of daily living and recreational activities.
Therapeutic Exercises:
- Continue previous exercises with progression of resistance and repetitions.
- Increased duration of endurance activities.
- Initiate return to specific recreational activity: golf, doubles tennis, progressive walking or biking program.
Criteria for Discharge:
(These are general guidelines as patients may progress differently depending on previous level of function and individual goals.)
- Non-antalgic, independent gait.
- Independent step over step stair climbing.
- Pain-free AROM.
- At least 4+/5 muscular performance based on MMT of all lower extremity musculature.
- Normal, age appropriate balance and proprioception.
- Patient is independent with home exercise program.
Uni-Compartment Knee Replacement
This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis (OA) is a degenerative disease of joints caused by a breakdown and eventual loss of articular cartilage. Articular cartilage lines the bony joint surfaces and allows the joint to move in a near frictionless environment. There are many reasons for cartilage loss including, wear, trauma and genetics. Once the knee joint cartilage is worn away, patients start to experience pain, stiffness and loss of function. The knee joint may assume an altered alignment such as a bowlegged or knock-kneed position.
The knee joint is made up of three compartments consisting of the outside (lateral), inside (medial) and the knee cap (patella femoral). Only one of the three compartments may experience ostoarthritic changes. The degenerative condition may spare the other knee areas leaving good working cartilage. A Unicondylar (one condyle) knee replacement is ideal when only 1 portion of the knee joint needs to be replaced. Often this surgery can relieve the pain of regional osteoarthritis and maintain a pain free knee for an extended period. In the event that the knee develops multiple compartment osteoarthritis a total knee replacement can be utilized even after undergoing unicondylar replacement surgery.
There are many advantages of a unicondylar replacement over a total knee replacement. See table one for a list of these benefits. Unicondylar replacement does not prevent osteoarthritis from forming in the remainder of the knee and a future knee replacement is often required.
Table 1. Benefits of unicondylar replacement over traditional knee replacement:
- Smaller incision
- Decreased blood loss (no blood donation needed)
- Quicker return to activity/work
- Reduced hospitalization (1-2 days)
- Less Post-op discomfort
As with any surgical procedure, there are risks to unicondylar knee replacement. These risks include but are not limited to infection, blood clot (DVT), bleeding, and nerve injury.
Pre-Surgery:
Before surgery, patients are instructed to continue to be as active as the knee permits. The following are specific instructions leading up to unicondylar knee replacement surgery.
- Anti-inflammatory such as ibuprofen or aspirin must be stopped 10 days prior to surgery. Utilize ice and elevation and Tylenol to control pain and swelling during this period.
- On the night before surgery, do not eat after midnight (no chewing gum or lozenges).
- On the morning of surgery you may take your daily pills with a sip of water.
- Your surgery time will be confirmed the day before.
Post-Surgery:
After the surgery is completed, you will awaken in the operating room and be moved to the recovery area. Once in recovery, you will meet a nurse who will take care of you prior to transfer to either home or the hospital unit (2 hours later). If you are staying overnight, expect to stay in the hospital for 1 day.
Pain Control:
—Femoral Nerve Block: Upon your consent, a femoral nerve block will be provided by an Anesthesiologist for pain control. This consists of an injection of Marcaine (like Novacaine) into the region around the femoral nerve and may decrease leg pain for up to 12 hours, many cases this is unnecessary but may help with your pain postoperatively.
—Oral pain medicine: Oral pain medicine will be provided to control your pain. A pain medication prescription will be provided to you prior to discharge. You may take the prescribed medication as directed. You should expect to experience minimal to moderate knee discomfort for several days and even weeks following the surgery. Patients often only need prescription narcotics for a few weeks following surgery and can then switch to over-the-counter medications such as Tylenol or Ibuprofen. Your Surgeon will not prescribe oral narcotics for more than 6 weeks following surgery. Ice should be used to reduce pain and swelling. In general apply ice for 20 minutes every 2-3 hours during the initial postoperative period.
Physical Therapy:
You will receive PT prior to discharge from the hospital. PT will work on ambulation, functional mobility and leg exercises. You should be comfortable walking independently with crutches before leaving the hospital. You will be able to put as much weight as tolerated on your knee. You should participate in the home exercise program provided in this packet and the program made by your hospital physical therapist until your post-op appointment where outpatient physical therapy will be initiated.
General information:
- If the bandage is draining, reinforce it with additional dressings for the first 48 hours. After 48 hours remove the bandage and leave the aquacel in place. Showering is acceptable at this time. Do not submerge or scrub the knee.
- Skin numbness often occurs around the incision (most common on outside of knee). This usually returns but may be permanent.
- You may shower on post op day one. Keep incision covered when showering for up to two days post-op. Do not wet wound until it is completely dry (non-draining).
- Take one 325 mg (full strength) aspirin in the morning and one at night daily for 6 weeks (unless otherwise instructed) to prevent blood clots.
- Eat a regular diet as tolerated and please drink plenty of fluids.
- First post-op appointment is 2 weeks after the surgery. Please call the office if you have any problems or questions.
- You may drive once you establish full control of your extremity (able to perform a straight leg raise, etc.). If your right knee was operated on, this may take several days or even weeks.
- Call office for Temperature >102 degrees, excessive swelling, pain or redness around the incision sites.
- Maximal improvement from surgery can be up to a year; typically patients are extremely mobile at 6-8 weeks.
- Golf and skiing can start after 8-10 weeks.
- Plan at least 2 weeks away from work (sedentary job) or school. Utilize this time to decrease swelling and participate in your home exercise program. You may resume work once the pain and swelling resolves (this varies based on job activity).
Phase I – Immediate Post Surgical Phase (Day 0-3)
The goal of physical therapy intervention during the early post-operative phase is to decrease swelling, increase range of motion, enhance muscle control and strength in the involved lower extremity and maximize patients' mobility with a goal of functional independence. Physical therapy interventions are also directed towards identifying other sensomotor or systemic conditions that may influence a patients' rehabilitation potential.
Goals:
The patient will:
- Perform bed mobility and transfers with the least amount of assistance while maintaining appropriate precautions.
- Ambulate with an assistive device for 25-100 feet and ascend/descend stairs to allow for independence with household activities while maintaining appropriate WB.
- Regain at least 80 degrees of passive and active range of motion in the knee to perform sit to stand transfers with minimal compensatory activity.
- Gain knee extension less than or equal to -10 degrees.
- Independently perform operative extremity Straight Leg Raise (SLR) exercise.
- Verbalize understanding of post-operative activity recommendations/precautions including use of proper positioning of the lower extremity, range of motion and strengthening exercises.
- Patients will also be educated on superficial massage of the knee joint to minimize hypersensitivity following surgery.
Observation and Assessment:
- Observe for any signs of deep vein thrombosis (DVT): increased swelling, erythema, calf pain.
- If a large amount of drainage is present, or there is blistering or frail skin around the knee joint or the lower extremities, discuss with the nurse and decide if notifying the surgical team is indicated.
- Assess patients' pain using the visual analogue scale. Ensure that patients are premedicated with oral/IV pain medication 30-60 minutes prior to treatment. Cryotherapy is recommended following physical therapy treatment to reduce pain, discomfort and swelling in the knee joint.
Therapeutic exercise and functional mobility:
- Active/active assisted/passive (A/AA/PROM) exercises (seated and supine).
- Patella femoral and tibial femoral joint mobilization and soft tissue mobilization as indicated.
- Soft tissue massage not over incision ever! Sutures dissolve on their own and don't need help.
- Isometric quadriceps, hamstring, and gluteal isometric exercises.
- Straight leg raises (SLR).
- Lower extremity range of motion (ROM) and strengthening as indicated based on evaluation findings.
- Closed chain exercises (if patient demonstrates good pain control, muscle strength and balance). Close-chained exercises should be performed with bilateral upper extremity support while maintaining appropriate WB precautions.
- Gait training on flat surfaces and on stairs.
- Transfer training.
Modalities:
- Continuous Cryotherapy for 72 hours after surgery, or at least 5 times/day.
- Patients are encouraged to use cryotherapy for 20 minutes before and after their independent exercise program.
Precautions:
- Weight bearing as tolerated (WBAT) with assistive device (unless indicated otherwise by the surgeon) to full weight bearing.
- Monitor wound healing and consult your Surgeon if signs and symptoms of excessive bleeding and poor incision integrity are present.
- Monitor for signs of DVT, pulmonary embolism (PE), and/or loss of peripheral nerve integrity. In these cases, notify your Surgeon or his team immediately.
- No exercises with weights or resistance.
- Avoid torque or twisting forces across the knee joint especially when WB on involved limb.
Positioning:
- A trochanter roll may be used as needed to maintain neutral hip rotation and promote knee extension.
- A towel roll should be placed at the ankle to promote knee extension when patients are supine in bed. Extension is the most important at this stage!
- Nothing should be placed behind the operative knee, to promote maximal knee extension and prevent knee flexion contracture.
Criteria for progression to the next phase:
- Ability to demonstrate Quadriceps contraction and/or perform a straight leg raise (SLR).
- Active knee range of motion (AROM) 0°-80°.
- Minimal pain and inflammation.
- Independent transfers and ambulation at least 100 feet with appropriate assistive device.
Phase II – Motion Phase (Day 3 – Week 6)
Goals:
- Improve knee active range of motion (AROM) to >/= 0-110 degrees.
- Muscle strengthening of the entire operative extremity with emphasis on knee extensor and flexor muscle groups.
- Attention should also be directed toward any weakness present in the operative extremity as well as, any generalized weakness in the upper extremities, trunk or contralateral lower extremity.
- Proprioceptive training to improve body/spatial awareness of the operative extremity in functional activities.
- Endurance training to increase cardiovascular fitness.
- Functional training to promote independence in activities of daily living and mobility.
- Gait training: Assistive devices are discontinued when the patient demonstrates adequate lower extremity strength and balance during functional activities (usually 1-4 weeks).
- Decrease inflammation/swelling.
- Return to functional activities.
Therapeutic Exercises:
Weeks 1-4
- AA/A/PROM, stretching for flexion (>90 degrees) and extension.
- Stationary Bicycle for ROM, begin with partial revolutions then progress as tolerated to full revolutions (no resistance).
- Patella femoral and tibial femoral joint mobilization as indicated.
- Continue isometric quadriceps, hamstring, and gluteal isometric exercises.
- Supine heel slides and seated Long Arc Quad (LAQ).
- SLR in 4 planes (flexion, abduction, adduction, extension).
- Neuromuscular electrical stimulation (NMES) for quads if poor quad contraction is present. NMES parameters to be set based on goal of exercise/activity. See neuromuscular electrical stimulation procedural standard of care for specific details.
- Gait training to improve function and quality of involved limb performance during swing through and stance phase. Patients are encouraged to wean off their assistive device at the latest by the end of second week from surgery.
- Postural cues/reeducation during all functional activities as indicated.
Weeks 4-6
- Continue above exercises.
- Continue patella femoral and tibial femoral joint mobilization as indicated.
- Continue NMES of quads if poor muscular performance of quad is present. May progress NMES use from isometric quad activity to isotonic and functional activity.
- Front and lateral step up and step down.
- 1/4 front lunge.
- Use sit to stand and chair exercises to increase knee flexion during functional tasks.
- Continue stationary bicycle for ROM.
- Begin pool program if incision is completely healed if available.
*Note: Exercises with resistance may be initiated as tolerated for operative extremity after goals for the first phase have been met, and the patient has met criteria for progression to the next phase.
Modalities:
- Cryotherapy 1-3x/day for swelling and pain management.
- Other modalities at the discretion of the therapist based on clinical findings.
Precautions:
- WBAT with assistive device as needed to minimize compensatory gait. Patient may be encouraged to use a straight cane within one week of surgery if he/she is WBAT to FWB. Patients may be weaned from assistive device by 2 weeks if they did not use an assistive device preoperatively and post-operative muscle performance is adequate for weight acceptance.
- Monitor wound healing and consult with referring MD if signs and symptoms of infection are present.
- Monitor for increased edema and continue with cryotherapy as needed.
Criteria for progression to the next phase:
- AROM 0-110°.
- Good voluntary quadriceps control.
- Independent ambulation community distances (>/= 800 feet), without assistive device, deviations or antalgia.
- Minimal pain and inflammation.
Phase III – Intermediate phase (week 6-8)
Goals:
- Maximize post-operative ROM (0-115 degrees plus).
- Good patella femoral mobility.
- Good strength all lower extremity musculature.
- Return to most functional activities and begin light recreational activities (i.e. walking, pool program).
Therapeutic Exercises:
- Continue exercises listed in Phase II with progression including resistance and repetitions. It is recommended to assess hip/knee and trunk stability at this time and provide patients with open/closed chain activities that are appropriate for each patient's individual needs.
- Continue patella femoral and tibial femoral joint mobilization as indicated.
- Initiate endurance program, walking and/or pool.
- Initiate and progress age-appropriate balance and proprioception exercises.
- Discontinue NMES of quads when appropriate quad activity is present.
Criteria for progression to next phase:
- AROM without pain, or plateaued AROM based on preoperative ROM status.
- 4+/5 muscular performance based on MMT of all lower extremity musculature.
- Minimal to no pain or swelling.
Phase IV – Advanced Strengthening and Higher Level Function Stage (week 8-12)
Goals:
- Return to appropriate recreational sports/activities as indicated.
- Enhance strength, endurance and proprioception as needed for activities of daily living and recreational activities.
Therapeutic Exercises:
- Continue previous exercises with progression of resistance and repetitions.
- Increased duration of endurance activities.
- Initiate return to specific recreational activity: golf, doubles tennis, progressive walking or biking program.
Criteria for Discharge:
(These are general guidelines as patients may progress differently depending on previous level of function and individual goals.)
- Non-antalgic, independent gait.
- Independent step over step stair climbing.
- Pain-free AROM.
- At least 4+/5 muscular performance based on MMT of all lower extremity musculature.
- Normal, age appropriate balance and proprioception.
- Patient is independent with home exercise program.
Dr. Ryan Nelson
861 Health Park Blvd.
Grand Blanc, MI 48439
(810) 953-0500
www.DrRNelson.com
ryan.Nelson@DrRNelson.com

Dr. Ryan Nelson
861 Health Park Blvd.
Grand Blanc, MI 48439
(810) 953-0500
www.DrRNelson.com
ryan.Nelson@DrRNelson.com
Schedule Your Consultation With Our Specialists
Schedule your next appointment quickly and conveniently with our team.
