Common Knees Injuries We Treat

Rehabilitation After Ankle Sprain
Ankle Sprain The Injury
Ankle sprains are very common ankle injuries, usually the result of the ankle turning inward.
An ankle sprain occurs when a ligament connecting the ankle bones is stretched or torn. If treated quickly and properly, most ankle sprains heal completely, allowing a safe and early return to activity. Recurrent sprains are
common, so it is important to strengthen the muscles that stabilize the ankle.
Contributing Factors to Ankle Sprains
• Muscle weakness or imbalance
• Inappropriate footwear
• Overweight
• Family tendency
• High-arch foot
• Previous injury
DEGREES OF SEVERITY OF ANKLE SPRAINS. Ankle sprains are graded as mild,
moderate and severe. The more severe the sprain, the longer the time to recover.
First Degree (Mild). This injury is the most common and usually the most minor. Ligaments connecting the bones of the ankle are “stretched”, causing a small amount of injury to the ankle ligaments. There is slight swelling but no instability. With a first-degree injury, you can expect to be back to sports within 1 to 3 weeks.
Second Degree (Moderate). When this injury occurs, the ankle ligaments are more deeply torn, resulting more pain and swelling. There is bruising of the skin and pain with walking. There can be looseness and minor instability. A second-degree sprain may require the use of a protective brace and 3 to 6 weeks of rest and recovery before you can return to full activity.
Third Degree (Severe). This injury results in a full tearing or rupture of an ankle ligament(s) usually on the inner and outer side of the ankle. The ankle can be very swollen and weight- bearing is painful. Crutches are often necessary and sometimes the ankle will be placed in a cast or cast-boot to allow the injury time to rest and heal. Surgery is rarely necessary, but the third-
degree ankle sprain can take many months to fully heal and may result in residual looseness of the ankle joint.
Treatment of Ankle Sprains
Treatment is divided into four stages. The rate of progress from one stage to the next depends upon the amount of pain and swelling present, and whether an elastic bandage, tape, a brace or a cast was used to stabilize your ankle.
Stage 1 (up to 72 hours)
To reduce pain and swelling, apply ice to the ankle for 20 minutes every hour while awake. Crushed Ice application in a plastic bag with a towel between the ice and your skin is a safe method to use. Compression of the ankle with an elastic bandage will help to limit swelling. The ankle should be elevated, as much as possible, to a position higher than your heart to reduce swelling. Tape, a splint, a brace or a cast may be applied to support or immobilize the ankle.
Stage 2 (first week)
You can walk and bear weight on the ankle as soon as it is comfortable. Crutches can be used as partial support when you begin to walk. Continue using taping, bracing or a cast. Let pain be your guide as to how much activity is enough. After an injury your ankle will get stiff. It is important to maintain the full range of motion your ankle. As an exercise to increase the ankle motion, rest your heel on the floor and write the alphabet in the air with your big toe, making the letters as large as you can.
Stage 3 (second week and after)
After the pain and swelling have subsided, you should try to walk normally with a brace or elastic support. Maintain ankle motion and strengthen the supporting muscles using theraband elastic bands.
Stage 4 (variable)
Your ankle should be strong when you return to full daily activity or sports. Returning too early to full activity may lead to re-injury and a chronic problem.
Criteria for return to sports activity: When you can stand on the toes of the injured ankle for 20 seconds and hop on your toes 10 times you can begin to run. Initially you should jog in a straight line until you jog pain-free. As you become stronger, you can progress to running a large figure-of-eight. You can return to sports practice when you can run a zigzag pattern without pain or instability.
Your ankle should be protected with a lace-up or other ankle support for a minimum of 6 months after injury.
Shoes. Athletic shoes that fit well and stabilize your foot will help prevent re-injury. You should not wear running shoes or sandals to play sports such as basketball, volleyball or tennis.
Exercises The following exercises will strengthen the ankle muscles and re-develop the reflexes of the ankle. Following the prescribed exercise program will restore normal ankle function and prevent re-injury and chronic problems.
Ankle Eversion With tubing anchored around uninvolved foot, slowly turn injured foot outward. Repeat 30 times.
Ankle Plantar Flexion With tubing around foot, press foot down. Repeat 30 times.
Ankle Dorsiflexion With tubing anchored on solid object, pull foot toward you knee. Repeat 30 times.
Ankle Inversion Cross legs with injured ankle underneath.
With tubing anchored around uninvolved foot, slowly turn injured foot inward. Repeat 30 times.
Calf Stretch Keeping back leg (injured) straight, with the heel and foot flat on the floor, lean into wall until a stretch is felt in the calf. Hold 15 to 20 seconds. Repeat 3 to 5 times.
Dorsiflexion Stretch Standing with both knees bent and the injured foot forward, gently lean forward, bending the injured knee over the ankle while keeping the heel and foot flat on the floor. This stretch will be felt in the ankle close to the heel or in the front of the ankle. Hold 15 to 20 seconds, Repeat 3 to 5 times.
Toe Raises Stand facing a wall, hands on the wall for support and balance, keep the knees extended fully. Tighten the quadricep to hold the knee fully straight. Raise up on ‘tip-toes’ while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 to 30 times. As you become stronger, you can raise up on both legs, and lower down on just the injured side. Gradually build so that you can raise up and down on just the injured leg.
Single -Leg Balancing Attempt to balance on the injured leg while holding the uninjured foot in the air. When you can balance easily, you can attempt to balance with eyes closed, or while someone throws you a ball. Practice this exercise for 5 minutes.
Calf Strain
ANATOMY
The calf muscles consist of the Gastrocnemius, which is the big muscle at the back of the lower leg, and the Soleus muscle, which is a smaller muscle lower down in the leg and under the Gastrocnemius. Either of these two muscles can be strained (torn).
INJURY
A calf strain is caused by a tearing of part of the gastrocnemius or soleus muscle from the top of the Achilles tendon. A sudden sharp pain at the back of the leg when running, sprinting or lunging is how the injury presents and occurs. Usually there is tenderness on the calf muscle; especially on the inner side. You may think you've just been hit in the leg.
Often, there is an audible "pop," and you may turn around to see what has just hit you. There is a sudden pain at the back of the leg, you may have difficulty in contracting the muscle or standing on tiptoe, and there may be pain, swelling or bruising in the calf muscle. This injury is common in running sports that require quick acceleration of changes in direction. Calf strain is also referred to as "Tennis Leg," because it is so common among tennis players. It usually occurs in people between the ages of 30 – 45.
Severity of Muscle Strains. Muscle strains are graded as mild, moderate and severe. The more severe the strain, the longer the time to recover.
First Degree (Mild). This injury is the most common and usually the most minor. This injury is a ‘pulled muscle’ with a structural disruption of less than 5 percent. With a first-degree injury, you can expect to be back to sports within 1 to 3 weeks.
Second Degree (Moderate). This injury consists of a more significant, but still incomplete muscle tear. This a partial muscle tear and requires 3 to 6 weeks of rest and recovery before you can return to full activity.
Third Degree (Severe). This injury results in complete tearing of the muscle–tendon unit. A third-degree muscle strain can take many weeks or months to fully heal.
TREATMENT
Rest from the activity that caused the muscle strain allows for healing to occur. Immediately following the muscle strain, ice should be applied over the painful area for 20 min. Periodic icing (2-3 times per day) will help to control swelling and reduce pain. Heat should not be applied to the area during the first 7-10 days since this may increase swelling and bleeding within the muscle. A compressive walking boot can permit pain free walking, and expedite healing. An elastic wrap or compressive stocking may be applied to the area to assist with swelling control. If the compressive device causes increased discomfort or "pins and needles" in any part of your leg, it is probably too tight. Lying down periodically with your leg elevated allows gravity to assist with your effort to control the swelling.
Though some experts believe early stretching to be valuable, caution should be taken to avoid aggressive stretching (stretching beyond the point of mild discomfort) which may disrupt healing. NO stretching or resistive exercise should be done during the first 3 weeks. As a general rule of thumb, any activity that elicits pain at or near the injured site may be causing
further injury and will only hamper your recovery effort.
A gradual conditioning program, specific to your sport, will prepare the calf muscles for the high demands placed upon them during athletics. Don't forget to incorporate a proper warm-up and stretching session into your conditioning program and athletic competition.
Rehabilitation Program
Exercises outlined in the rehabilitation program are described and illustrated in the back of the handout. The ‘time line’ that is illustrated in the following rehabilitation program is typical after grade 2 and 3 injuries. After a grade 1 injury, rehabilitation can usually begin at phase three.
Phase one - The first week after injury
• Rest from painful activities
• Ice 20 minutes, three times a day
• Compression wrap or neoprene sleeve
Phase two – the second and third week after injury
• Ice once a day, 20 minutes, after exercises
• Start active ROM exercises, 1-2 times a day, 10 to 20 repetitions
• Ankle ROM exercises: move the foot up and down 20 times and make circles with the foot,
left and right, 20 times, three times a day.
• Stationary bicycle, 10 minutes, no resistance, if pain free
• NO stretching
Phase three – the 4th, 5th and 6th week after injury
•Theraband Strengthening exercises, pain free
•Stationary cycle, add 1 minute per session up to 30 to 40 minutes
•Slow treadmill walking, pain free, start 5 minutes and add one minute per session to 20
minutes or start “Return to Walk\Run Program” (see below).
•Gentle pain-free stretching, two times a day (see stretching illustrations and instructions
in the back of the handout).
Phase four – 7 to 12 weeks after injury
• Follow ‘Toe Raising Progression’ strengthening supplement
• Stationary cycle
• Continue gentle calf stretching
• Start ‘Return to Full Speed Running Program’
Phase five – from 12 weeks onward
• Continue above program
• Start return to sports training
Return to Walk/ Run Program after Calf strain
General Instructions
1. Walking/jogging should be done no more than every other day.
2. The program should be performed step by step. Do not advance your program until you can successfully complete the initial step. Let pain and swelling be your guide. If the activity creates pain, swelling, or causes you to limp, go back to the previous step. 3. Before starting the program and after completion of the program allow 15 minutes to perform warm-up and gentle stretching exercises.
4. Cool down by gently stretching all muscle groups
5. Ice for 20 minutes after cool down stretching.
Phase 1:
Day #1 Walk 1/4 mile -- easy pace (1/2 speed)
Day #2 Walk 1/4 mile -- (3/4 speed)
Day #3 Walk 1/4 mile -- full speed - briskly
Phase 2:
Day #1 Walk 1/2 mile -- easy pace (1/2 speed)
Day #2 Walk 1/2 mile (3/4 speed)
Day #3 Walk 1/2 mile -- full speed - briskly
Phase 3:
Day #1 Walk 3/4 mile-- (3/4 speed)
Day #2 Walk 3/4 mile -- (full speed — briskly)
Day #3 Walk 1 mile -- (comfortable pace — 3/4—full speed)
Phase 4:
Day #1 Jog 1⁄4 mile, Walk 3⁄4 mile, comfortable pace
Day #2 Jog 1⁄2 mile, Walk 1⁄2 mile, comfortable pace
Day #3 Jog 3⁄4 mile, Walk 1⁄4 mile, comfortable pace
Phase 5:
Day #1 Jog 3⁄4 mile, Walk 1⁄4 mile, comfortable pace
Day #2 Jog 1 mile
Day #3 Jog 1 mile
You can continue to increase distance by 1⁄4 mile per session until you reach your desired distance. When you have reached your training distance without causing any pain or swelling, and have a normal running form, you can gradually start to increase your running speed or progress to the “Return to sprint program”.
Toe Raising Progression for Achilles Tendon Repair
Phase 1
Frequency: Daily
Times per Day: 3
Repetitions: 20
Technique: Up and down on both legs together
Duration: 2-4 weeks
Phase 2
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1-2
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 3
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1-2
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times, 2 sets
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 4
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 5
Frequency: 4 days a week, 2 days on, 2 days off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times, 2 sets
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 6
Frequency: 3-4 days a week, 1 day on, one day off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times, 3 sets
-Up and down on both legs together, 10 times
Duration: 1 month
Phase 7
Gradual Return to sports activity
ACHILLES TENDON RUPTURE
The Achilles tendon is a strong tendon that connects the calf muscles to the heel. The calf is formed by two muscles: the underlying soleus muscle and the thick outer gastrocnemius muscle. When they contract, they pull on the Achilles tendon causing your foot to point down (plantar flexion)and helping you raise up on your toes. This powerful muscle group helps when you sprint, jump, or climb.
With aging and overuse, the Achilles tendon is subject to degeneration within the substance of the tendon. The term degeneration means that wear and tear occurs in the tendon over time and leads to a weakening of the tendon. Degeneration in a tendon usually shows up as a loss of the normal arrangement of the fibers of the tendon. Tendons are made up of strands of a material called collagen (think of a tendon as similar to a nylon rope with the strands of collagen being the nylon strands). Some of the individual strands of the tendon become jumbled due to the degeneration, other fibers break, and the tendon loses strength. The healing process in the tendon can cause the tendon to become thickened as scar tissue tries to repair the tendon. This process can continue to the extent that a nodule forms within the tendon. This condition is called tendinosis. The area of tendinosis in the tendon is weaker than normal tendon and is usually painful.
Spontaneous rupture of the Achilles tendon can occur in patients in their third to fifth decade. Rupture is more common in men than women and most injuries occur during sporting activities. The most common mechanism of injury is pushing off forcefully such as in
tennis, squash, racquetball and basketball.
When the Achilles tendon ruptures, the person often hears a "pop" or "snap" at the time of injury and feels a sudden pain in the region of the Achilles tendon. However, the pain subsidesmquickly. There is weakness when trying to stand on tip-toes. A defect or gap in the Achillesmtendon can usually be felt.
DIAGNOSTIC IMAGING
X-rays are useful to rule out fractures, but are of limited value to diagnose Achilles tendon ruptures. Although MRI will show the ruptured tendon, it is usually not necessary to obtain an MRI because the diagnosis is obvious to examination.
TREATMENT OPTIONS Non- surgical Treatment
If the foot and ankle are immobilized in a cast with the toes pointing down for at least 8 weeks the torn Achilles tendon can heal. Non-surgical treatment avoids potential complications associated with surgery, such as infections and wound breakdown. However, currently controversial in the literature there may a higher re-rupture rate with non-operative treatment, there is less pushing-off strength and less endurance when compared to tendons that have been surgically repaired.
Surgical Treatment
Surgical repair of Achilles tendon ruptures consists of sewing together the torn ends. Sometimes, if the injury is chronic or the tissue is poor, local tissue such as tendon grafts or fascia can be used to reinforce the repair.
A major advantage of early repair is that early range of motion out of cast can be allowed. Surgical repair of the Achilles tendon offers a lower re-rupture rate (0-4%), a greater chance of returning to sports, greater strength, and more endurance. However wound complcations such as wound breakdown or infection can occur and can be very serious.
Post operative rehabilitation consists of a cast for two weeks, then a removable cast-boot for about 12 weeks after surgery. It usually takes six months after surgery before sports activities can be resumed.
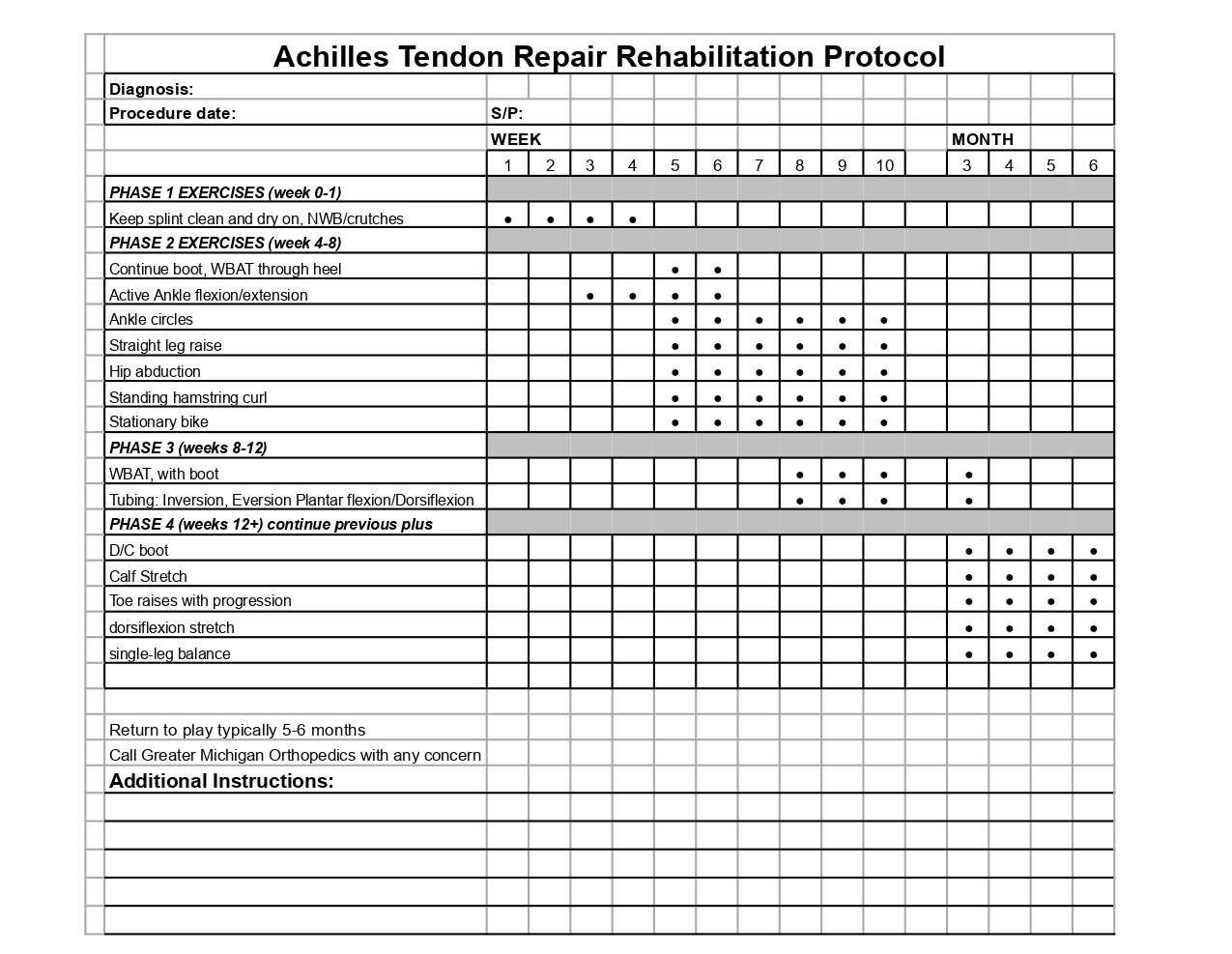
ACHILLES TENDON REPAIR SURGERY REHABILITATION PROTOCOL
PHASE ONE: The first week after surgery
SURGERY:
After anesthesia has been given, your leg will be cleaned and sterile drapes will be placed. A small incision will be made over the Achilles tendon. The ruptured tendon is identified and exposed. The ruptured ends of the tendon are brought together with sutures to achieve a secure repair. Sometimes a small tendon in the leg is also used to reinforce the Achilles tendon repair. The skin is closed with sutures and the foot is immobilized in a cast or splint.
AFTER SURGERY:
You will be given a prescription for pain medication to take home with you (usually Percocet, Vicodin). The pain medication has a tendency to make you constipated and occasionally can cause nausea.
In addition to this medication you should take one aspirin a day to help prevent blood clots (phlebitis).
CAST/CRUTCHES
You will go home with a cast on your leg and foot. As much as possible, keep you foot elevated higher than your heart and move the toes up and down often to help control swelling. Use the crutches when you walk, but do not bear weight on your operated leg.
OFFICE VISIT
Please make an appointment to see your surgeon in the office one week after surgery. At that time your cast and sutures will be examined. Your surgeon will give you further instructions at that time.
ACHILLES TENDON REPAIR SURGERY REHABILITATION PROTOCOL
PHASE 2: Weeks 4 through 8 after surgery
Goals
1. Protect the repaired tendon
2. Decrease swelling
3. Start early gentle range of motion exercises
4. Begin weight bearing with the cast-boot when walking
ACTIVITIES
1. Achilles Boot (brace)
You will be fitted with a removable ankle brace / boot that has rubber wedges under the heel to elevate your heel. This keeps your foot in a toe-down position. You can bear full weight on the operated leg as long as you are wearing the brace and feel pressure on your heel when you walk. Your weight should be borne through the heel and not the toes. You can remove the boot to
shower or bathe and to move the foot and ankle.
2. Crutches
You can discontinue using the crutches over the next one to two weeks. Progress from using two crutches to using one crutch on the side opposite your surgery. If you feel comfortable doing so, you can progress to walking with only the support of the brace if you are pain free and you are bearing weight through your heel.
3. Swelling
As often as you can, elevate your leg higher than your heart to control swelling in you foot and leg. If the foot and toes are swollen, you must elevate for longer periods of time. Use elastic stockings to lessen leg swelling.
4. Exercises
You may do exercises for your upper body and uninvolved leg. Exercises can be done for the operated leg as directed in the following section. When doing the ankle motion exercises with the brace removed, move the ankle and foot gently to avoid excessive stress at the surgery site. Gentle motion can promote healing, but aggressive motion can disrupt the surgical repair.
Exercise Program
Ankle flexion-extension - Remove the brace. Gently move the foot in an up and down motion. Do not try to force motion through pain, but move the foot up and down through the range of motion that is pain free. Repeat 20 times, three times a day.
Ankle circles - Remove the brace.
Move the foot so that you are making a circular motion. Make 10 circles to the left and 10 circles to the right, three times a day.
Straight leg lift - With the brace on, tighten the quadriceps muscles so that the knee is flat, straight and fully extended. Try to raise the entire leg up off the floor or bed. If you are able to do so keeping the knee straight, raise the leg to about 45 degrees, pause one second and then lower slowly. Repeat 20 times, twice a day.
Hip Abduction - With the brace on, lie on your unoperated side. Keeping theknee fully extended, raise the operated limb upward to a 45 degree angle as illustrated. Hold one second, then lower slowly. Repeat 20 times, twice a day
Standing Hamstring Curl - With the brace on, stand facing a table which you will use for balance and support. While standing on the unoperated leg bend the knee of the operated side and raise the heel toward the buttock. Hold this flexed position for one second. Slowly lower the foot back to the floor. Keep the thighs aligned as illustrated. Repeat 20 times.
Stationary Cycle - With the brace on, you may ride a stationary bicycle for 10 to 20 minutes a day if you wish.
ACHILLES TENDON REPAIR SURGERY REHABILITATION PROTOCOL
PHASE THREE: Weeks 8 through 12 after surgery Goals
1. Protect the repaired tendon
2. Decrease swelling
3. Start strengthening exercises
4. Continue full weight bearing using the brace when walking
ACTIVITIES
1. Achilles boot (brace)
Continue to wear the brace, but the heel lift that keeps your foot in a toe-down position can be lowered. You can bear full weight on the operated leg as long as you are wearing the brace. You should feel that your weight is being borne through the heel and not the toes. You can remove the cast-boot to shower or bathe and to practice range of motion exercises.
2. Swelling
If the leg is swollen, continue to elevate your leg higher than your heart. Use elastic stockings to lessen swelling.
3. Exercises
You may do exercises for your upper body and uninvolved leg. Continue to do the exercises outlined in earlier phases on a daily basis. All exercises should be done without pain or excessive stretch at the surgery site. The following Theraband exercises can be added, once a day, as instructed by your doctor or the physical therapist.
Theraband Exercise Program (start using yellow theraband and progress to red in 2 weeks)
Ankle Eversion
With tubing anchored around uninvolved foot, slowly turn injured foot outward. Repeat 30 times.
Ankle Plantar Flexion
With tubing around foot, press foot down. Repeat 30 times. This is the most important of the exercises.
Ankle Dorsiflexion
With tubing anchored on solid object, pull foot toward you knee. Repeat 30 times.
Ankle Inversion
Cross legs with the operated foot underneath. With tubing anchored around uninvolved foot, slowly turn injured foot inward. Repeat 30 times.
ACHILLES TENDON REPAIR SURGERY REHABILITATION PROTOCOL
PHASE FOUR: Weeks 12 through 24 after surgery
Goals
1. Protect the repaired tendon
2. Add strengthening exercises
3. Use a heel lift when walking
4. Begin walking normally
ACTIVITIES
1. Discontinue Achilles Boot (brace)
Insert one of the rubber wedges from inside the brace into your shoe to elevate the heel. After using the heel lift in your shoe for approximately one month, you may remove the lift from your shoe if you are walking normally (without a limp).
2. Exercises
You may do exercises for your upper body and uninvolved leg. The theraband exercises should be done every other day. You can progress to red theraband for one month, then progress to blue theraband after that. The exercises from Phase One can be done every other day and ankle weights can be added to increase resistance. The following exercises can be added, every other day, as instructed by your doctor or the physical therapist.
Calf Stretch
Keeping the rear (injured) leg straight, with the heel and foot flat on the floor, lean into wall until a stretch is felt in the calf. Do not stretch excessively. Hold 15 to 20 seconds. Repeat 3 to 5 times.
Toe Raises
Stand facing a table, holding the table for support and balance. Keep the knees extended straight. While holding the knees fully straight, raise up on ‘tip-toes’ while maintaining the knees in full extension. Hold for one second, then lower slowly to the starting position. Repeat 20 to 30 times. After one month, you can raise up on both legs, and lower down on only the operated side. At five or six months after surgery, build strength so that you can raise up and down on just the injured leg. See the Achilles Toe Raising Progression on the next page.
Dorsiflexion Stretch
Standing with both knees bent and the injured foot forward, gently lean forward, bending the injured knee over the ankle while keeping the heel and foot flat on the floor. This stretch will be felt in the ankle close to the heel or in the front of the ankle. Do not over-stretch! Hold 15 to 20 seconds, Repeat
3 to 5 times.
Single -Leg Balancing
Attempt to balance on the operated leg while holding the unoperated foot in the air. When you can balance easily, you can attempt to balance with eyes closed, or while someone throws you a ball. Practice this exercise for 5 minutes.
Toe Raising Progression for Achilles Tendon Repair
Phase 1
Frequency: Daily
Times per Day: 3
Repetitions: 20
Technique: Up and down on both legs together
Duration: 2-4 weeks
Phase 2
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1-2
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 3
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1-2
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times, 2 sets
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 4
Frequency: 5 days a week, 2 days on, one day off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 5
Frequency: 4 days a week, 2 days on, 2 days off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times, 2 sets
-Up and down on both legs together, 10 times
Duration: 2 weeks
Phase 6
Frequency: 3-4 days a week, 1 day on, one day off
Times per Day: 1
Repetitions and Technique: -Up and down on both legs together, 10 times
-Up on both legs and down on the affected leg, 10 times
-Up and down the affected leg only, 10 times, 3 sets
-Up and down on both legs together, 10 times
Duration: 1 month
Phase 7
Gradual Return to sports activity
Schedule Your Consultation With Our Specialists
Schedule your next appointment quickly and conveniently with our team.
