AC arthritis
Acromioclavicular (AC) Joint Arthritis of the Shoulder
The AC joint is located at the tip of the shoulder where the shoulder blade (scapula) and collarbone (clavicle) come together at a point on the upper part of the shoulder blade called the acromion. These two bones are held together by ligaments. One group of ligaments envelope the joint to form a capsule that covers the joint; these ligaments are termed the acromioclavicular ligaments. Another set of ligaments stabilize the shoulder by holding the clavicle in place by attaching it to a bony projection on the surface of the shoulder blade called the coracoid process. These ligaments are called the coracoclavicular ligaments. There is a disk of cartilage in the joint between the two bones that helps the guide the joint movement. As you move the shoulder, the AC joint allows movement to occur between the clavicle and scapula.
What is AC arthritis?
AC joint arthrosis(arthritis) is most common in middle aged patients when the cartilage in the AC joint begins to wear out. With this condition there is typically pain that limits motion of the arm.
Causes of AC Arthritis of the Shoulder
The primary cause of AC arthritis is due to wear and tear. As a person does lifting of the arm stress is placed across this joint and over time this stress can cause the cartilage to wear over repetitive stress. Constant overhead lifting, such as weightlifters or construction workers, can increase the incidence of the disease. Traumatic causes from a fall onto the end of the shoulder can also contribute to the disease.
Symptoms of AC Arthritis of the Shoulder
One of the first signs is pain and tenderness at the top of the shoulder around the AC joint. Sleeping on the side that is painful may increase the pain. In addition, there may be decreased shoulder motion. Compression of the joint, such as bringing the arm across the chest may result in increased pain. There may be swelling at the AC joint. If the AC joint had ben injured in the past, there may be a snap or click as the shoulder is moved, and there may be a slight prominence of the AC joint.
Diagnosis
Usually the diagnosis of AC joint arthritis is made during physical exam. X-rays will also demonstrate narrowing of the joint and the presence of bone spurs.
Non-Surgical Treatment
The goal of treatment for AC joint arthritis is to eliminate pain and restore movement to the shoulder. Treatment, initially, may be conservative, consisting of rest and NSAIDs. Ice may be applied to decrease the pain and inflammation at the joint. Cortisone or other injections may be used if the pain persist. Physical therapy can help restore the motion and retrain muscles around the shoulder to help lessen the load across the AC joint
Surgical Treatment
Should rest, ice, medications and activity modification fail to reduce your pain and allow you to perform the activities you like to perform, surgery may be indicated for the next step. The most common procedure is AC joint resection (mumford procedure) This procedure is done under arthroscopic guidance to remove the arthritic portion of the end of the collar bone. The surgery can is often done in conjunction with other procedures such as rotator cuff repair. It is same day surgery and may begin motion of the shoulder immediately. Full recovery for an isolated AC resection can be expected to be three months.
Results and Risks of Surgery
May series of patients have been reported in the literature showing high levels of pain relief; nearly 95 percent of patients return to their normal activities and sports with few complications. As with any surgery there are potential risks, such as, infection (less than 0.5%) persistent pain, incomplete resolution of symptoms, damage to nerves and vessels and possible need for further surgeries.
Acromioclavicular Joint Injury (ACCR)
Shoulder Separation and Acromioclavicular Joint Injury Description
A shoulder separation is not truly an injury to the shoulder joint. The injury actually involves the acromioclavicular joint (also called the AC joint). The AC joint is where the collarbone (clavicle) meets the highest point of the shoulder blade (acromion).
Mechanism of Injury
The most common cause for a separation of the AC joint is from a fall directly onto the shoulder. The fall injures the ligaments that surround and stabilize the AC joint. If the force is severe enough, the ligaments attaching to the underside of the clavicle are torn. This causes the "separation" of the collarbone and shoulder blade. The shoulder blade actually moves downward from the weight of the arm. This creates a "bump" or bulge above the shoulder.
The injury can range from a little change in configuration with mild pain, to quite deforming and very painful. Good pain-free function often returns even with a lot of deformity. The greater the deformity, the longer it takes for pain-free function to return.
- A mild shoulder separation involves a sprain of the AC ligament that does not move the collarbone and looks normal on X-rays.
- A more serious injury tears the AC ligament and sprains or slightly tears the coracoclavicular (CC) ligament, putting the collarbone out of alignment to some extent.
- The most severe shoulder separation completely tears both the AC and CC ligaments and puts the AC joint noticeably out of position.
Diagnosis
The injury is easy to identify when it causes deformity. When there is less deformity, the location of pain and X-rays help the doctor make the diagnosis. Sometimes having the patient hold a weight in the hand can increase the deformity, which makes the injury more obvious on X-rays.
Treatment
Nonsurgical treatments, such as a sling, cold packs, and medications can often help manage the pain. Sometimes, a doctor may use more complicated supports to help lessen AC joint motion and lessen pain.
Most people return to near full function with this injury, even if there is a persistent, significant deformity. Some people have continued pain in the area of the AC joint, even with only a mild deformity. This may be due to:
- Abnormal contact between the bone ends when the joint is in motion
- Development of arthritis
- Injury to a disk-like piece of cushioning cartilage that is often found between the bone ends of this joint
It is often worthwhile to wait and see if reasonable function returns without surgical treatment
Surgical Treatment
Surgery can be considered if pain persists or the deformity is severe. A surgeon might recommend trimming back the end of the collarbone so that it does not rub against the acromion. Where there is significant deformity, reconstructing the ligaments that attach to the underside of the collarbone is helpful. This type of surgery works well even if it is done long after the problem started.
Whether treated conservatively or with surgery, the shoulder will require rehabilitation to restore and rebuild motion, strength, and flexibility.
ACROMIOCLAVICULAR JOINT RECONSTRUCTION SURGERY
Phase One: the first week after surgery
GOALS:
- Control pain and swelling
- Protect the AC joint repair
- Protect wound healing
- Begin early shoulder motion
ACTIVITIES:
Immediately After Surgery
- After surgery you will be taken to the recovery room room, where your family can meet you. You will have a sling on your operated arm. Rarely, an abduction pillow is needed to hold the arm up in the air away from the body.
- You should get out of bed and move around as much as you can.
- When lying in bed, elevate the head of your bed and put a small pillow under your arm to hold it away from your body.
- Apply cold packs to the operated shoulder to reduce pain and swelling.
- Move your fingers, hand and elbow to increase circulation.
- The novocaine in your shoulder wears off in about 6 hours. Ask for pain medication as needed.
- You will receive a prescription for pain medication for when you go home (it will make you constipated if you take it for a long time).
At Home
- You can remove the bandages but leave the small pieces of tape (steristrips) in place.
- You may shower and get the incision wet. To wash under the operated arm, bend over at the waist and let the arm passively come away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
- Apply cold to the shoulder for 20 minutes at a time as needed to reduce pain and swelling.
- Remove the sling several times a day: move the elbow wrist and hand. Lean over and do pendulum exercises for 3 to 5 minutes every 1 to 2 hours.
- DO NOT lift your arm at the shoulder using your muscles.
- Because of the need for your comfort and the protection of the repaired AC joint, a sling is usually necessary for 4 to 6 weeks, unless otherwise instructed by your surgeon.
OFFICE VISIT:
Please arrange to see your surgeon in the office 7-10 days after surgery for suture removal and further instructions. If you have questions or concerns regarding your surgery or the rehabilitation protocol and exercises call the office.
Rehabilitation after Acromioclavicular Joint Reconstruction
Phase One: 0 to 6 weeks after surgery
Goals:
- Protect the surgical repair
- Ensure wound healing
- Prevent shoulder stiffness
- Regain range of motion
- Control pain and swelling
Activities:
- Sling Use your sling most of the time for the first 2 weeks. The doctor will give you additional instructions on the use of the sling at your post-operative office visit. Remove the sling 4 or 5 times a day to do pendulum exercises.
- Use of the operated arm Do not let weight of arm pull on fixation device x 6 weeks Do not elevate surgical arm above 90 degrees in any plane for the first 6 weeks post-op. Do not lift any objects over 1 or 2 pounds with the surgical arm for the first 6 weeks. Avoid excsessive reaching and external/internal rotation for the first 6 weeks.
- Showering You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively come away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
Exercise program
Days per week: 7 Times per day 3-5
- pendulum exercises
- Supine external rotation
- supine assisted arm elevation limit to 90 degrees
- Isometric: Internal and external rotation at neutral
- Elbow, wrist and hand
- Scapular retraction
Phase two: 7 to 12 weeks after surgery
Goals:
- Protect the surgical repair
- Improve range of motion of the shoulder
- Begin gentle strengthening
Activities
- Sling Your sling is no longer necessary unless your doctor instructs you to continue using it (use it for comfort only).
- Use of the operated arm You can now move your arm for most daily activities, but you need to continue to be careful not to lift objects heavier than 1 or 2 pounds. You should avoid forceful pushing or pulling activities. You should continue to avoid reaching behind you or other positions with the hand behind the head.
Exercise Program
Days per week 7 Times per day 1-3
STRETCHING/ACTIVE MOTION
- Supine external rotation
- Standing external rotation
- Supine assisted arm elevation
- Arm elevation in scapular plane
- Behind the back internal rotation (limit beltline)
- Horizontal adduction (active reach only)
- Hands behind head stretch
- ER @ 90 abduction stretch
- Proprioception drills
- Side lying IR @ 90
STRENGTHENING/THERABAND
- Internal and External rotation
- Biceps curl
- Row
- Forward punch
STRENGTHENING/DYNAMIC
- Side lying ER
- Prone row
- Prone extension
- Prone ’T’s
- Prone ‘Y’s
- Standing scaption
- Isotonic biceps curl
- Rhythmic stabilization
- Scapulohumeral rhythm exercises
Phase Three: starting 13 to 18 weeks after surgery
Goals:
- Protect the surgical repair
- Regain full range of motion
- Continue strengthening progression
Activities:
Use of the operated arm You may now safely use the arm for normal daily activities involved with dressing, bathing and self- care. You may raise the arm away from the body; however, you should not raise the arm when carrying objects greater than one pound. Any forceful pushing or pulling activities could still disrupt the healing of your surgical repair. Continue to avoid lifting weighted objects overhead.
Exercise Program:
STRETCHING / RANGE OF MOTION
Days per week: 7 Times per day: 1-2
- Pendulum exercises
- Standing External Rotation / Doorway
- Wall slide Stretch
- Hands-behind-head stretch
- Standing Forward Flexion
- Behind the back internal rotation
- Supine Cross-Chest Stretch
- Sidelying internal rotation (sleeper stretch)
- External rotation at 90° Abduction stretch
STRENGTHENING / THERABAND
Days per week: 7 Times per day: 1
- External Rotation
- Internal Rotation
- Standing Forward Punch
- Shoulder Shrug
- Dynamic hug
- Seated Row
- Biceps curl
- W’s
STRENGTHENING/ DYNAMIC
Days per week: 7 Times per day: 1
- Side lying ER
- Prone horizontal ’T's
- Prone row
- Prone extension
- Prone ‘Y’s
- standing forward flexion “full can”
- Standing scaption
- Isotonic biceps curl
- Rhythmic stabilization
- Scapulohumeral rhythm exercises
- limited weight training can begin
Phase Four: starting 19 to 28 weeks after surgery
Goals:
- Progression of functional activities
- Maintain full range of motion
- Continue progressive strengthening
- Advance sports and recreational activity per surgeon
Exercise Program
STRETCHING / RANGE OF MOTION
Days per week: 5-7 Times per day: 1
Continue all exercises from phase 3
STRENGTHENING / THERABAND
Days per week: 3 Times per day: 1 Continue from phase 3
STRENGTHENING / DYNAMIC
Days per week: 3 Times per day: 1 Continue from phase 3
PLYOMETRIC PROGRAM
- ‘Rebounder’ throws with arm at side
- Wall dribbles overhead
- Rebounder throwing/weighted ball
- Deceleration drills with weighted ball
- Wall dribbles at 90°
- Wall dribble circles
WEIGHT TRAINING
See weight training precautions section
Dr. Ryan Nelson
861 Health Park Blvd. Grand Blanc, MI 48439 (810) 953-0500 www.DrRNelson.com ryan.Nelson@DrRNelson.com
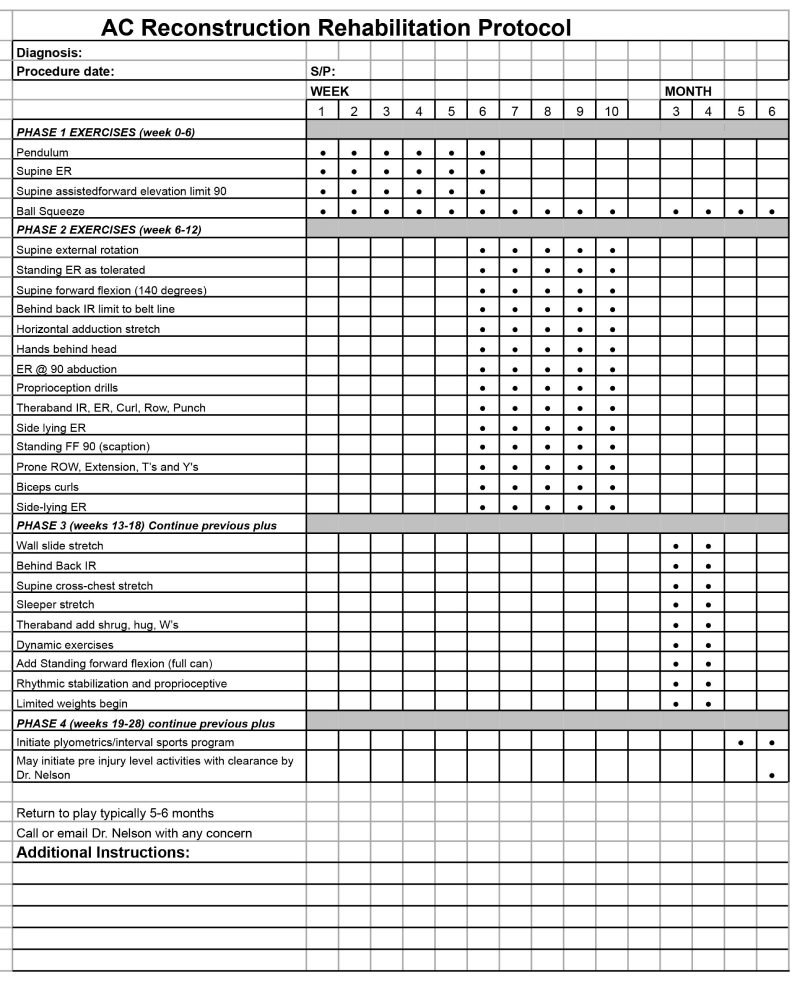
AC Reconstruction Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6

Arthroscopic Capsular Release
Shoulder Arthroscopic Capsular Release Rehabilitation
Phase one: 0 to 4 weeks after surgery
Goals:
- Improve range of motion of the shoulder and prevent adhesions from forming
- Begin gentle strengthening
Activities
Sling
Your sling is not necessary except for comfort, unless your surgeon instructs you to continue using it (use it for comfort only).
Use of the operated arm
You can move your arm for normal daily activities without restriction, unless your surgeon gives you other instructions. Avoid lifting heavy objects and avoid forceful use of the arm
Bathing and showering
There are no restrictions unless your surgeon gives you other instructions. Do not submerge the incisions in the bath, hot tub, pool or lake until the skin is healed.
Ice
- Continue to use Ice 20 minutes a time as needed. Do not place directly on skin
Exercise Program
Days per week: 7 Times per day: 2
1 set of 10-15 reps
- Pendulum exercises - Each direction for 2 minutes
- Supine External Rotation
- Standing External Rotation
- Supine passive arm elevation Seated-Standing Arm Elevation
- Behind the back internal rotation
- Supine external Rotation with Abduction Supine Cross Chest Stretch
- Side-lying Internal Rotation
- Prone Horizontal Arm Raises
Phase Two: 4 to 12 weeks after surgery
Goals:
- Regain full range of motion
- Continue gentle strengthening
Activities:
Use of the operated arm
You may now safely use the arm for most normal daily activities. Any forceful pushing, pulling or lifting activities should continue to be avoided.
Exercise Program
STRETCHING / ACTIVE MOTION
Days per week: 7 Times per day : 1-2
1-2 sets 10-15 reps
- Pendulum exercises
- Standing External Rotation / Doorway Wall Climb Stretch
- Corner Stretch
- Standing Forward Flexion
- Behind the back internal rotation
- Supine external Rotation with Abduction Supine Cross Chest Stretch
- Side-lying External Rotation / 1 lb. Prone Horizontal Arm Raises / 1 lb.
STRENGTHENING / THERABAND
1-2 sets 15-20 reps
- External Rotation
- Internal Rotation
- Standing Forward Punch
- Shoulder Shrug
- Seated or standing Row
- Biceps curl
Bankart Protocol
Shoulder Instability (Bankart)
The shoulder joint is comprised of the humerus and glenoid socket. The large head and small socket gives the shoulder joint excellent range of motion. This range of motion however comes at the cost of stability (it takes only a strong breeze to blow the golf ball off the T). A traumatic external force such as a football tackle may cause the shoulder joint to dislocate or subluxate(almost dislocate).
The labrum is a cartilaginous structure that acts as a bumper or lip to maintain the shoulder joint in place. A dislocation will tear the labrum off the glenoid surface and stretch associated ligaments. This type of labral tear is called a “Bankart tear”.
After the first dislocation the patient is at an increased risk for subsequent dislocations. The events that cause further dislocations need not be as forceful as the original. Imagine trying to balance a golf ball on a T that only had half of its top in place. Simple activities such as moving in bed or putting on a book bag may cause shoulder subluxation or dislocation. In order to return stability to the shoulder joint, the labrum should be reattached and the supporting ligaments tensioned.
Diagnosis of a Bankart Tear:
The patient with a labral tear often reports multiple shoulder dislocations from low velocity activities as described above. Patients report a feeling of apprehension with certain shoulder movements such as lifting the arm overhead or throwing a ball. Labral tears and ligament laxity are diagnosed by reviewing the shoulder history and participating in a physical examination. X-rays looking for associated trauma to the shoulder joint and MRI to examine the condition of the labrum are often utilized to aid in the diagnosis.
Conservative management may be utilized after the initial dislocation. This consists of very short term sling immobilization followed by physical therapy for shoulder joint strengthening. Surgical repair is the treatment of choice for the patient with multiple dislocations and an unstable shoulder joint. Without surgical intervention, the torn labrum and stretched ligaments are unlikely to heal properly and provide for a stable shoulder joint. The surgical repair is conducted utilizing arthroscopic equipment. This means that a small camera and small equipment will be used through tiny incisions. Anchors attached with suture material are placed in the glenoid bone. The sutures are then passed through the labral tissue. A knot is tied which brings the labrum tightly against the bone reestablishing its natural position and ligament tension
RESULTS AND RISKS OF SURGERY
The success rate of the open Bankart repair is approximately 95%. The success rate of arthroscopic Bankart repair can be similar, assuming there is little or no bone loss. If there is a fracture of the glenoid rim (Bankart fracture) and a compression fracture of the humeral head (Hill-Sachs lesion), there is an increased risk of recurrent instability following repair.
Two nerves are at risk during surgery since they are near the operative field, but they are rarely injured. As with any surgical procedure, there are potential risks: The incidence of infection is less than 0.5%. The shoulder can lose some motion after surgery, especially if the shoulder has to be significantly tightened because of excess laxity. Recurrent instability can occur.
Surgery:
The length of an arthroscopic Bankart repair will take up to 1.5 hours depending on the complexity of the tear. Your nurse will bring you into the pre-op area were you will have an IV placed and met with your anesthesiologist. General anesthesia is utilized to assure a comfortable surgery. This means that you will be “asleep” and completely unaware of the surgery until you wake up in the recovery area. Most patients will have a small tube placed in there windpipe, formal intubation may not be required. Local blocks are also available to supplement pain control. Your anesthesiologist will discuss this with you prior to surgery. Like any surgical procedure, there are risks. These risks are extremely rare and consist of nerve injury, infection and shoulder stiffness or instability.
Post-Surgery:
After the surgery is completed, you will awaken in the operating room and be moved to the recovery area. Most patients generally recover smoothly and have minimal pain due to local pain medication that is used at the completion of the surgery. Family members and guests are permitted to visit in the recovery area once the patient is fully awake and feeling comfortable; this may take up to 2 hours after the surgery is completed.
- A pain medication prescription will be provided prior to discharge. You may take the prescribed medication as directed. You should expect to experience moderate shoulder discomfort for several days and even weeks following the surgery. Patients often only need prescription narcotics for a few days following surgery and then can switch to over-the-counter medications Tylenol or Ibuprofen. Ice should be applied to the shoulder up to three times a day for 20 minutes until swelling subsides
- At the completion of surgery, you will have a sling placed on your arm. Wear the sling at all times with the exception of exercises, showering and dressing. You may also remove the sling to participate in computer work or watching TV for instance. The purpose of the sling is to protect the labral repair. Excessive arm movement during the first few weeks of recovery may put unwarranted strain on the repair. Particularly avoid external rotation or rotation away from the body for at least 6 weeks.
- Special cooling devices (called Cryo/Cuffs) are also available for patients to purchase thru our office. This can be used in the place of the ice bags.
- If the bandage is draining, reinforce it with additional dressings for the first 48 hours. After 48 hours remove the bandage and place band aids over the incision sites. Showering is acceptable at this time. Do not scrub the shoulder.
- There is an exercise sheet at the end of this packet. Conduct exercises three times daily until further directions are provided. Physical therapy will start 4-6 weeks after surgery.
- Eat a regular diet as tolerated and please drink plenty of fluids.
- You are unable to drive a car as long as you need to utilize a sling.
- Call office for Temperature >102 degrees, excessive swelling, pain or redness around the incision sites.
- Plan at least a week away from work or school. Utilize this time to decrease swelling and participate in your home exercise program. You may be able to resume work (depending on type of work and setting; very variable) once the pain and swelling resolves.
- The above are guidelines and only intended as generalities.
Rehabilitation after Bankart Shoulder Repair and Anterior Stabilizing
Phase 0: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS
GOALS:
- Control pain and swelling
- Protect the repair
- Begin early shoulder motion
ACTIVITIES WHEN YOU GO HOME:
- Apply ice to the shoulder as tolerated to reduce pain and swelling. You can change the dressing to a smaller one to allow the cold therapy to reach the shoulder.
- Remove the sling on the first day after surgery. Move your elbow, fingers and hand several times per day.
- Begin the pendulum exercise several times per day: Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion. Repeat for 2 to 3 minutes at a time.
- Remove the outer dressing on the second day after surgery and shower. Leave the little pieces of tape (steri-strips) in place. You can get the wound wet after 2 days in a shower, but do not soak in a tub. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position.
- Keep your elbow slightly in front of your body; do not reach behind your body. When putting on clothing, lean forward and pull the shirt up and over the operated arm first. Then put the other arm into the opposite sleeve. To remove the shirt, take the non-operative arm out of the sleeve first, and then slip the shirt off of the operated arm.
- Call your surgeon's office for any concerns, including, but not limited to, severe pain, fevers, chills or redness.
OFFICE VISIT:
Please arrange to come back to your surgeon's office 7-10 days after surgery for examination and further instructions.
Phase 1: 2 to 5 weeks after surgery
Goals:
- Protect the repair
- Ensure wound healing
- Prevent shoulder stiffness
Activities:
- Sling Use your sling as instructed by your surgeon. You may remove it whenever you wish if you are careful and keep the shoulder safe. Put the sling on when you are outside or in a crowd. Keep the sling on when sleeping at night for the first three or four weeks.
- Use of the operated arm You may use your hand on the operated arm as long as you do not rotate the arm externally or away from your body. You should bend your arm at the elbow and use your fingers and hand, such as to reach up and touch your face. Keep your elbow in front of you.
- Bathing and showering You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
Phase 2: 5 to 8 weeks after surgery
Goals:
- Protect the shoulder and avoid over stressing the repair
- Improve range of motion of the shoulder
- Begin strengthening exercises
Activities:
- Sling The sling is no longer necessary.
- Use of the operated arm You may now use your arm. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
- Precautions Do not lift objects overhead with the weight of the object going behind the head. In other words, keep objects in front of you where you can see them.
- Use ice or cold as necessary 15-20 minutes.
Phase 3: 8 to 12 weeks after surgery
Goals:
- Protect the shoulder repair
- Regain full range of motion
- Continue gentle strengthening
Activities:
Use of the operated arm —You may now use your arm in a more normal fashion. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
Precautions —Do not lift heavy weights overhead with the weight going behind the head. In other words, keep the weights in front of you where you can see them.
Phase Four: 12 to 24 weeks after surgery
Goals:
- Protect the ligament repair
- Regain full range of motion
- Continue strengthening
- Gradual return to full activity
Activities:
Use the arm for normal daily activities. There is no restriction on your range of motion unless exceptions are outlined in your discussions with your doctor. Weight training can gradually resume with caution being paid to exercises such as bench press, incline press, dips, pull-downs behind the neck or other exercises where the hands are repeatedly placed behind you. If you are returning to contact sports, you should wait until six months after surgery.
Dr. Ryan Nelson
861 Health Park Blvd. Grand Blanc, MI 48439 (810) 953-0500 www.DrRNelson.com ryan.Nelson@DrRNelson.com
Return to Activities
Computer After 2 weeks Golf 8 weeks (chip & putt only) Tennis 12 weeks (no overhead) Contact Sports 4 months
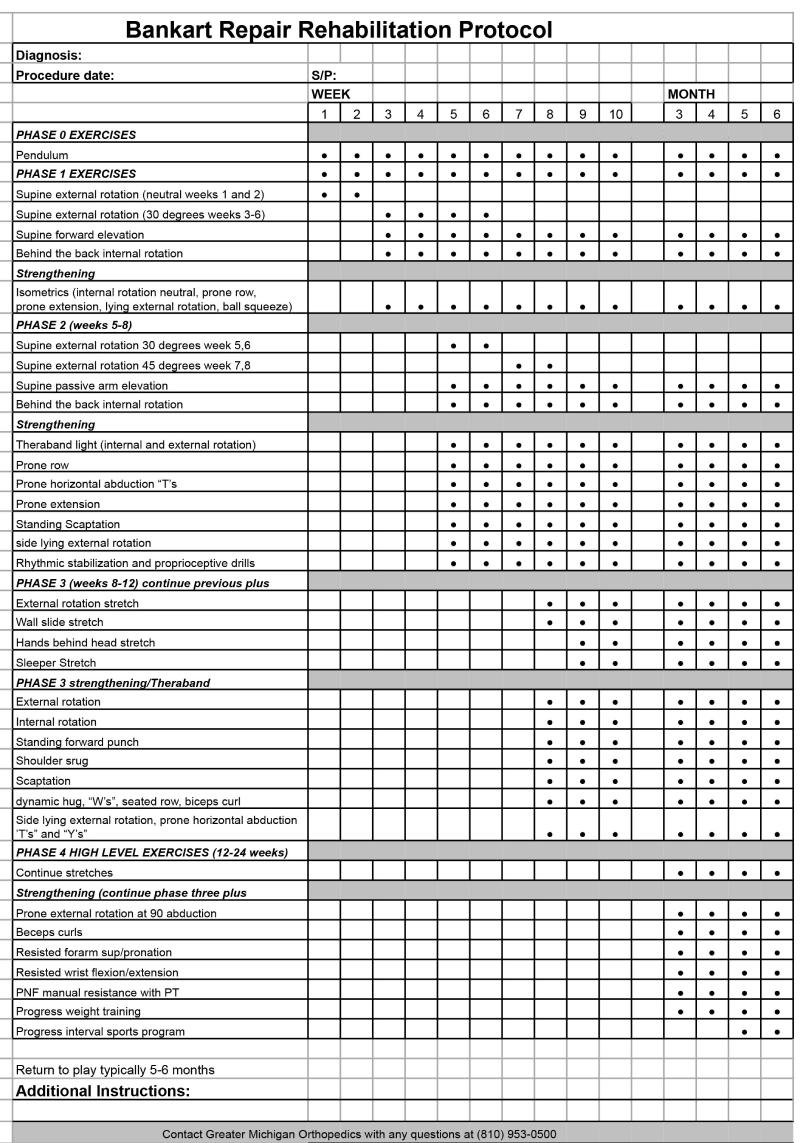
Bankart Repair Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6
Biceps Tenodesis
Biceps tenodesis
The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface. This is coupled with the humerus (shaped like a golf ball) to make up the joint. The glenoid labrum is a ”ring” of cartilage that turns the flat surface of the glenoid into a slightly deeper socket, which is similar to resting a golf ball on a golf tee instead of a table top, providing more shoulder stability. Another part of the scapula, called the acromium, articulates with the clavicle (collar bone) to make the acromioclavicular (AC) joint.
The rotator cuff is a group of four muscles: the supraspinatus, infraspinatus, teres minor, and subscapularis. The rotator cuff tendons attach around the humeral head (ball) and connects the humerus to the scapula.
The long head of the biceps originates from the top of the glenoid fossa and labrum (top of the golf tee). It then runs through a groove in the humerus (upper arm bone) to join the short head of the biceps and inserts on a bone in the forearm. Because of its position, the long head of the biceps is also considered to be a secondary stabilizer of the shoulder joint.
The long head of the biceps is at risk of injury and degenerative changes due to its proximity to the rotator cuff and the acromium. Since the long head of the biceps can act as a secondary stabilizer of the shoulder, it is also subject to injury during high speed overhead movements; repetitive overhead movements; or forceful shoulder activities when the elbow is straight. Specific injuries may include inflammation and irritation of the bicep tendon itself; a problem with the bicep tendon in conjunction with one of the rotator cuff tendons; or detachment of part of the tendon from the attachment point (SLAP tear). Bicep tendon degeneration and/or tearing can cause significant shoulder discomfort and dysfunction.
A biceps tenodesis is a surgical procedure which may be performed for treatment of severe symptoms involving the biceps tendon, including inflammation or partial tears. It may be performed in isolation or as part of a larger shoulder surgery, including surgery involving the rotator cuff. During the biceps tenodesis, the normal attachment of the biceps tendon on the shoulder socket (glenoid fossa) is cut and reattachment of the tendon is made on the humerus (upper arm bone). This takes the pressure off the biceps attachment and places the attachment below the actual shoulder joint. The goal is to eliminate the shoulder pain coming from the bicep tendon.
Biceps Tenodesis Protocol
The intent of this protocol is to provide the clinician with a guideline of the post- operative rehabilitation course of a patient that has undergone a Biceps Tenodesis for biceps dysfunction. It is no means intended to be a substitute for one’s clinical decision making regarding the progression of a patient’s post-operative course based on their physical exam/findings, individual progress, and/or the presence of post-operative complications. If a clinician requires assistance in the progression of a post-operative patient they should consult with the referring Surgeon.
Phase I – PROM Phase (starts approximately post op weeks 1- 3)
Goals:
- Minimize shoulder pain and inflammatory response
- Achieve gradual restoration of passive range of motion (PROM)
- Enhance/ensure adequate scapular function
Precautions/Patient Education:
- No active range of motion (AROM) of the elbow
- No excessive external rotation range of motion (ROM) / stretching. Stop when you feel the first end feel.
- Use of a sling to minimize activity of biceps
- Ace wrap upper forearm as needed for swelling control
- No lifting of objects with operative shoulder
- Keep incisions clean and dry
- No friction massage to the proximal biceps tendon / tenodesis site
- Patient education regarding limited use of upper extremity despite the potential lack of or minimal pain or other symptoms
Activity:
- Shoulder pendulum hang exercise
- PROM elbow flexion/extension and forearm supination/pronation
- AROM wrist/hand
- Begin shoulder PROM all planes to tolerance /do not force any painful motion
- Scapular retraction and clock exercises for scapula mobility progressed to scapular isometric exercises
- Ball squeezes
- Sleep with sling as needed supporting operative shoulder, place a towel under the elbow to prevent shoulder hyperextension
- Frequent cryotherapy for pain and inflammation
- Patient education regarding postural awareness, joint protection, positioning, hygiene, etc.
- May return to computer based work
Milestones to progress to phase II:
- Appropriate healing of the surgical incision
- Full PROM of shoulder and elbow
- Completion of phase I activities without pain or difficulty
Phase II – Active Range of Motion Phase (starts approximately post op week 4)
Goals:
- Minimize shoulder pain and inflammatory response
- Achieve gradual restoration of AROM
- Begin light waist level functional activities
- Wean out of sling by the end of the 4 postoperative week
- Return to light computer work
Precautions:
- No lifting with affected upper extremity
- No friction massage to the proximal biceps tendon / tenodesis site
Activity:
- Begin gentle scar massage and use of scar pad for anterior axillary incision
- Progress shoulder PROM to active assisted range of motion (AAROM) and AROM all planes to tolerance
- Lawn chair progression for shoulder
- Active elbow flexion/extension and forearm supination/pronation (No resistance)
- Glenohumeral, scapulothoracic, and trunk joint mobilizations as indicated (Grade I - IV) when ROM is significantly less than expected. Mobilizations should be done in directions of limited motion and only until adequate ROM is gained.
- Begin incorporating posterior capsular stretching as indicated
- Cross body adduction stretch
- Side lying internal rotation stretch (sleeper stretch)
- Continued Cryotherapy for pain and inflammation
- Continued patient education: posture, joint protection, positioning, hygiene, etc.
Milestones to progress to phase III:
- Restore full AROM of shoulder and elbow
- Appropriate scapular posture at rest and dynamic scapular control with ROM and functional activities
- Completion of phase II activities without pain or difficulty
Phase III - Strengthening Phase (starts approximately post op week 8-10)
Goals:
- Normalize strength, endurance, neuromuscular control
- Return to chest level full functional activities
Precautions:
- Do not perform strengthening or functional activities in a given plane until the patient has near full ROM and strength in that plane of movement
- Patient education regarding a gradual increase to shoulder activities
Activity:
- Continue A/PROM of shoulder and elbow as needed/indicated
- Initiate biceps curls with light resistance, progress as tolerated
- Initiate resisted supination/pronation
- Begin rhythmic stabilization drills
- External rotation (ER) / Internal Rotation (IR) in the scapular plane
- Flexion/extension and abduction/adduction at various angles of elevation
- Initiate balanced strengthening program
- Initially in low dynamic positions
- Gain muscular endurance with high repetition of 30-50, low resistance 1-3 lbs)
- Exercises should be progressive in terms of muscle demand / intensity, shoulder elevation, and stress on the anterior joint capsule
- Nearly full elevation in the scapula plane should be achieved before beginning elevation in other planes
- All activities should be pain free and without compensatory/substitution patterns
- Exercises should consist of both open and closed chain activities
- No heavy lifting should be performed at this time
- Initiate full can scapular plane raises with good mechanics
- Initiate ER strengthening using exercise tubing at 30° of abduction (use towel roll)
- Initiate sidelying ER with towel roll
- Initiate manual resistance ER supine in scapular plane (light resistance)
- Initiate prone rowing at 30/45/90 degrees of abduction to neutral arm position
- Begin subscapularis strengthening to focus on both upper and lower segments
- Push up plus (wall, counter, knees on the floor, floor)
- Cross body diagonals with resistive tubing
- IR resistive band (0, 45, 90 degrees of abduction
- Forward punch
- Continued cryotherapy for pain and inflammation as needed
Milestones to progress to phase IV:
- Appropriate rotator cuff and scapular muscular performance for chest level activities
- Completion of phase III activities without pain or difficulty
Phase IV – Advanced Strengthening Phase (starts approximately post op week 10)
Goals:
- Continue stretching and PROM as needed/indicated
- Maintain full non-painful AROM
- Return to full strenuous work activities
- Return to full recreational activities
Precautions:
- Avoid excessive anterior capsule stress
- With weight lifting, avoid military press and wide grip bench press.
Activity:
- Continue all exercises listed above
- Progress isotonic strengthening if patient demonstrates no compensatory strategies, is not painful, and has no residual soreness
- Strengthening overhead if ROM and strength below 90 degree elevation is good
- Continue shoulder stretching and strengthening at least four times per week
- Progressive return to upper extremity weight lifting program emphasizing the larger, primary upper extremity muscles (deltoid, latissimus dorsi, pectoralis major)
- Start with relatively light weight and high repetitions (15-25)
- May initiate pre injury level activities/ vigorous sports if appropriate / cleared by your surgeon
Milestones to return to overhead work and sport activities:
- Clearance from MD
- No complaints of pain
- Adequate ROM, strength and endurance of rotator cuff and scapular musculature for task completion
- Compliance with continued home exercise program
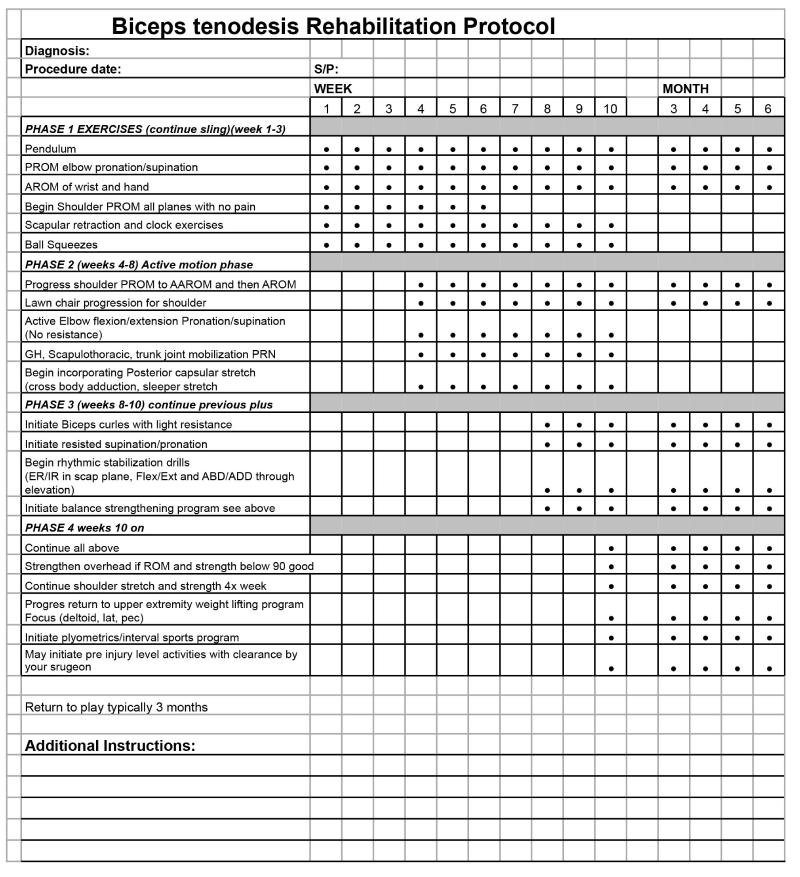
Biceps tenodesis Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6

Hip scope FAQ
What is Hip arthroscopy?
Hip arthroscopy is a minimally invasive surgery. Usually 2-3 small poke hole incisions (about 1cm) are made on the side of your hip. Special instruments and a camera are used to look inside your hip and perform the operation.
What can I do until surgery?
Most people can do activities as tolerated by pain. We do not routinely prescribe pain medicine pre-operatively.
ANATOMY
What is the hip joint?
The hip joint is a ball and socket joint made up of 2 bones. The ball is the head of the femur (part of your thigh bone) and the socket is the acetabulum (part of your pelvis).
The hip joint is lined by special smooth articular cartilage which provides a smooth lubricated surface for your hip joint to move freely without pain or grating.
Around the rim of your acetabulum (the socket), is a special type of cartilage called your labrum. It acts to effectively deepen your socket, providing more stability to your hip.
What is femoroacetabular impingement?
Femoroacetabular impingement is a term used when the bones of your hip joint are not shaped properly. There are two types of impingement.
- CAM impingement occurs when your ball (femoral head) is not perfectly round, often described as having a bone spur or bump.
- Pincer impingement occurs when your socket (acetabulum) is too deep, directed the wrong way or has excess bone around the rim.
As you move in certain directions, the bones grind on each other abnormally. This leads to tearing of your labrum and pain. It is also one of the factors that scientist believe lead to osteoarthritis.
How common is femoroacetabular impingement?
It is likely that at least 1 in 4 people have this condition. But not everyone who has this condition will develop hip pain or arthritis.
SURGERY
Do I actually need surgery?
Hip arthroscopy should be done after you have failed at least 3-6 months of conservative management. Conservative management should include physical therapy, alteration of activity, intra-articular injections, and anti-inflammatories and tylenol. Surgery should be used as a last resort.
If I don’t have surgery, can I play sports again? If it feels better, can I cause more damage if I continue activities?
Conservative care is always an option. If rest and therapy reduce the pain, you can try activity again. If you have a labral tear, it is likely that the activity will eventually cause pain again. It is possible to cause more damage if you continue activities. The pain can wax and wane.
Will surgery prevent further damage to the labrum/cartilage? What are the chances of recurrence?
Surgery is done to reshape the ball and the acetabulum and repair the labrum. We believe that it I can slow down the damage to the joint, although we cannot repair damage that has already been done to the cartilage. There is no assurance that the labrum will not tear again. Recurrent tears are unusual.
Will surgery help the pain?
Surgery can correct the mechanical issues in the hip joint. The ball and socket can be reshaped and the x-rays and MRI restored to near normal. However, this is not a guarantee that the pain will go away completely.
What kind of anesthesia do you use?
General anesthesia. A nerve block is also used sometimes to help with post-operative pain. This can be discussed with the anesthesiologist at the time of surgery.
How is the surgery done?
After you are asleep, your foot is placed into a padded boot. A traction device is then used to pull on your leg, so that the hip joint opens up. With the help of an Xray machine, the exact location of your hip joint is found and the surgical instruments are introduced. Because of the traction, your leg muscle can spasm after surgery and occasionally your feet and groin may temporarily go numb.
How long is the surgery?
This is dependent on the exact procedure. Usual time is about 2 hours.
How long am I in the hospital?
Typical patients are a day surgery, so you can come in and go home on the same day. If the pain is tolerable, you do not have to stay overnight.
What are the potential risks and complications of having hip arthroscopy?
Problems following hip arthroscopy are rare. However, you should always consider the risks before having any type of surgery.
- Risks associated with having a general anesthetic
- Infection. The chance of having an infection is about 1:5000. This ranges from a simple skin infection that is easily treated with antibiotics to a serious complication called a deep joint infection. This needs to be treated with intravenous antibiotics and further surgery to clean the joint.
- Nerve numbness (parasthesia). Sometimes the traction used during the operation can cause pressure on the nerves in the groin and lead to temporary numbness around the groin and genitalia. This is uncommon and almost all cases reported have resolved over a few days to weeks.
- There are many other theoretical risks including fracture, avascular necrosis and impotence, and they are extremely rare and we have never seen them occur.
- There is also the risk that our may not get pain relief or may not be able to get back to the activities you wish to get back to at the same level of higher.
- You can still develop arthritis and need further surgery.
- Blood clots or deep venous thrombosis can occur.
All surgery carries some risks. All efforts are made to minimize these risks. Feel free to discuss this with your surgeon.
Can surgery make me worse?
Although feeling worse after surgery is always a possibility, the incidence has been reported to be very small.
POST-OPERATION
What happens after my operation?
You will be placed in a brace and transferred to the recovery room. A nurse will look after you until the anesthesia has worn off. Once your pain is controlled you will be discharged home.
How painful is the surgery?
A lot of patients report that the pain is less than expected. Although this is minimally invasive surgery, it can still be quite painful. We give you different types of pain medications during and after the surgery to help.
What can I expect for the first 2 or 3 days after surgery?
Usually during the first 2 or 3 days, there is not a lot of moving around. We do encourage you to get about with the crutches intermittently to do your usual daily activities (i.e. use the restroom, ect.)
What do I take for pain?
Before surgery, we ask you not to take any anti-inflammatories (Iburprofen, Naproxen, Aspirin) for at least 5 days. We will give you a prescription for narcotic pain medicine on your day of surgery. We do not generally write these before that day. People vary as to how long or how much medication they need. As your pain gets better, you can switch to Tylenol.
Will I have bruising or swelling?
There is usually a large amount of swelling around the groin, thigh and buttocks and even down the knee which goes away over a couple of days. Bruising can also be fairly common.
How long will I need crutches?
Most of our patients will need crutches for 2-4 weeks. This means you can touch your foot down to the floor, but not put all of your weight on it. Occasionally this may be 6-8 weeks. We actually do not want you to be totally non-weight bearing, your foot should touch the floor when walking. Physical therapy will teach you how to be touch-down weight bearing.
When do I get my stitches out?
Most patients get dissolvable sutures, so they don’t have to come out. If you have stitches that have to be removed, we do that at about 2 weeks.
How long will I be out of school/work?
Generally, most students miss about a week of school. For work, it depends on what you do. Time out from work is also variable. This will not only depend on the procedure but what your work requirements are. If you have a job that is mostly sitting you should be able to return within a couple of weeks. If you have a physical job you should discuss this with your surgeon.
How long until I can drive?
You must be off of pain medication and crutches to drive. It may be 2-3 weeks before you are comfortable driving if it is your left hip and the car is an automatic. If surgery is on your right hip then you will not be able to drive from anywhere between 3-6 weeks.
When do I start physical therapy?
You will get a prescription for this at your first post operative visit. You can schedule your first PT visit after that appointment.
How long will it take me to recover after hip arthroscopy?
Recovery is variable and person dependent. It is generally LONGER than people anticipate. Walking can begin immediately after the operation, pain-free walking is between 2-6 weeks. Running can start at 8-12 weeks. Competitive sports usually 4-6 Months. Full recovery can be as long as ONE year.
How do I do activities of daily living?
- Sleeping. Sleeping can be difficult on the side of your operation. If possible, sleep on your back. Or, sleep on your non-operative side with a pillow between your legs.
- Prepare your home. Try to organize your home so that things are easy to get to. You will have discomfort, especially when bending over, so make things easy for yourself.
- Look after yourself. Having an operation should be considered a big thing. So take some time to really look after yourself and don’t rush around. You should be recovering, not working.
- Toilet seats. Going to the toilet can be uncomfortable. A raised toilet seat can help.
- Sitting. Sitting with your hips at 90 degrees can be painful. Try to lean back and sit with your hips less bent.
- In the car. Lean your car seat back to keep the hip less bent.
- Bending over. Try not to bend over too often the first couple weeks. Get someone to help with shoes and socks.
- Have someone look after you. Normal activities such as showering, toileting, putting on shoes and socks, getting in and out of chairs, getting in and out of bed can be difficult in the first few days.
When do I see my srugeon again?
You should have a post-operative visit at 2 weeks, 6 weeks, 3 months, 6 months and 1 year. New X-rays and MRIs may be ordered at those visits if necessary.
Always call your surgeon's office with any questions.
Shoulder Instability (Latarjet)
Shoulder Instability (Latarjet)
The shoulder joint is comprised of the humerus and glenoid socket. The large head and small socket gives the shoulder joint excellent range of motion. This range of motion however comes at the cost of stability. A traumatic external force such as a football tackle may cause the shoulder joint to dislocate or subluxate(almost dislocate).
The labrum is a cartilaginous structure that acts as a bumper or lip to maintain the shoulder joint in place. A dislocation will tear the labrum off the glenoid surface and stretch associated ligaments. This type of labral tear is called a “Bankart tear”.
After the first dislocation the patient is at an increased risk for subsequent dislocations. The events that cause further dislocations need not be as forceful as the original. Imagine trying to balance a golf ball on a T that only had half of its top in place. Simple activities such as moving in bed or putting on a book bag may cause shoulder subluxation or dislocation. In order to restore stability to the shoulder a surgical procedure is typically recommended, which can be broken down to a soft tissue procedure or a bone procedure.
Shoulder Instability – Soft Tissue:
Surgical reconstruction targeting the glenohumeral joint’s soft tissues for shoulder instability, typically involves labral repairs, the most common being the Bankart repair. A Bankart lesion typically occurs from an anterior-inferior dislocation of the humerus, tearing the labrum from it’s attachment to the glenoid, thereby detaching the inferior gleno-humeral ligament (IGHL). Surgical management of this revolves around labral repair to reattach the IGHL under appropriate tension. This may be accomplished either arthroscopically or through an open approach. Most traumatic glenohumeral dislocations may not only cause a Bankart lesion, but may create impression fractures in the postero-superior humeral head termed Hill-Sachs lesions. An adverse effect from this procedure includes suturing the capsule too tightly, causing a shortening of the capsule, and thus decreasing the external rotation allowed at the glenohumeral joint. Other complications are extremely rare, but may include axillary nerve damage, subscapularis rupture (seen only in open repairs performed with subscapularis detachment and repair), and recurrent instability. If there is bony deficiency in the glenoid, which represents 20% or more of the antero-inferior glenoid, it is biomechanically impossible to restore the same stability and is therefore more prone to recurrent instability and failure.
Shoulder Instability – Bony Deficiency:
In cases where significant bony deficiency is present (where greater than 20% of the glenoid’s surface area is missing) addressing only the soft tissue issues during the surgical procedure may lead to eventual recurrence of instability. Bony deficiency can result from congenital deformity, trauma, or recurrent dislocation. These lesions are not well visualized on plain films and are best seen on 3-dimensional CT scan. When bony lesions reach critical dimensions, reconstruction of this deficit using autograft bone yields the best surgical results. The Latarjet procedure is the most popular and highly effective, transferring the distal coracoid into the bony defect.
Results and Risks of Surgery:
There are several possible complications that could occur after a Latarjet procedure. Considering the coracoid osteotomy, there is a risk for non-union of the transferred coracoid process, which occurs typically in 3% of patients. Despite the bony union (healing), a small percentage of patients continue to experience discomfort years post-operatively and underwent another procedure to extract the screws. Screw loosening and screw breakage are other possible reasons a patient may undergo a screw removal procedure. Other complications, including musculocutaneous or axillary nerve palsy and subscapularis dysfunction, are reported but rare events.
Following a Latarjet procedure, the most functional limitation reported is a decrease in external rotation range of motion. Although some patients may return to overhead throwing sports, most do not regain full external rotation. According to Hovelius and colleagues, the mean loss of external rotation was 7.4 degrees in adduction and 8 degrees in abduction, both are minimal in every day activities. The complications of rotator cuff tendonitis and limitation in external rotation can be reduced with proper progression in rehabilitation.
Surgery:
The length of a Latarjet will take up to 2 hours depending on the complexity shoulder. Your nurse will bring you into the pre-op area were you will have an IV placed and met with your anesthesiologist. General anesthesia is utilized to assure a comfortable surgery. This means that you will be “asleep” and completely unaware of the surgery until you wake up in the recovery area. Most patients will have a small tube placed in there windpipe, formal intubation may not be required. Local blocks are also available to supplement pain control. Your anesthesiologist will discuss this with you prior to surgery. Like any surgical procedure, there are risks. These risks are extremely rare and consist of nerve injury, infection and shoulder stiffness or instability.
Post-Surgery:
After the surgery is completed, you will awaken in the operating room and be moved to the recovery area. Most patients generally recover smoothly and have minimal pain due to local pain medication that is used at the completion of the surgery. Family members and guests are permitted to visit in the recovery area once the patient is fully awake and feeling comfortable; this may take up to 2 hours after the surgery is completed.
- A pain medication prescription will be provided prior to discharge. You may take the prescribed medication as directed. You should expect to experience moderate shoulder discomfort for several days and even weeks following the surgery. Patients often only need prescription narcotics for a few days following surgery and then can switch to over-the-counter medications Tylenol or Ibuprofen. Ice should be applied to the shoulder up to three times a day for 20 minutes until swelling subsides
- At the completion of surgery, you will have a sling placed on your arm. Wear the sling at all times with the exception of exercises, showering and dressing. You may also remove the sling to participate in computer work or watching TV for instance. The purpose of the sling is to protect the repair. Excessive arm movement during the first few weeks of recovery may put unwarranted strain on the repair. Particularly avoid external rotation or rotation away from the body for at least 6 weeks.
- Special cooling devices (called Cryo/Cuffs) are also available for patients to purchase thru our office. This can be used in the place of the ice bags.
- If the bandage is draining, reinforce it with additional dressings for the first 48 hours. After 48 hours remove the bandage and place band aids over the incision sites. Showering is acceptable at this time. Do not scrub the shoulder.
- There is an exercise sheet at the end of this packet. Conduct exercises three times daily until further directions are provided. Physical therapy will start 4-6 weeks after surgery.
- Eat a regular diet as tolerated and please drink plenty of fluids.
- You are unable to drive a car as long as you need to utilize a sling.
- Call office for Temperature >102 degrees, excessive swelling, pain or redness around the incision sites.
- Plan at least a week away from work or school. Utilize this time to decrease swelling and participate in your home exercise program. You may be able to resume work (depending on type of work and setting; very variable) once the pain and swelling resolves.
- The above are guidelines and only intended as generalities.
OFFICE VISIT:
Please arrange to come back to your surgeon's office 7-14 days after surgery for examination and further instructions
Rehabilitation after Latarjet
One must recall that the purpose of the Latarjet procedure is to reinstate anterior stability to the glenohumeral joint. While this is primarily a bony procedure, specific attention must be directed towards the soft tissues which play a critical role in maintaining stability. Early post-operative therapy must protect the repair of the subscapularis as well as the developing bony union of the coracoid process.
Since it will take approximately 6-8 weeks to form an osseous union of the newly reconstructed glenoid, the biceps and coracobrachialis attachment to the coracoid needs to be protected during the initial postoperative period. Aggressive shoulder extension and combined extension and external rotation stretching is not indicated. Once strengthening commences, a gradual progressed program of biceps and coracobrachialis strengthening needs to be followed to minimize undue stress and tension on their muscular origins.
In addition, isolated external rotation range of motion needs to be gradually regained after surgery to allow the anterior capsule and subscapularis to heal appropriately.7 For that reason, external rotation range of motion is advanced in a protected fashion, with early emphasis on external rotation work being done in an open packed position (i.e. scapular plane at about 45 degrees of abduction) and then progressed to positions that gradually tension the subscapularis (i.e. full adduction and then at 90 degrees of abduction and above). Please refer to protocol below for more detail. (In the case of a subscapularis take down and repair, external rotation gains need to be progressed slower and one should avoid aggressive external rotation stretching and internal rotation strengthening until the subscapularis is well healed. In these cases it is helpful to get a ‘safe zone’ of initial external rotation range of motion from the referring surgeon, as determined from intraoperative inspection from either the operative note or discussion with surgeon.)
Due to the surgical technique and early immobilization required to promote healing, the subscapularis may not only be impacted in terms of length, but in terms of force production and proprioception. Hence, specific subscapularis proprioception and strengthening needs to be incorporated to enhance subscapularis function postoperatively. The clinician needs to tailor the rehabilitation program to address the unique structure of the subscapularis to enhance both the upper and lower subscapularis fibers. This is warranted due to the fact that the subscapularis is innervated by both the upper and lower subscapular nerves, along with the presence of two different muscular fiber alignments; hence, its action has been described as being like that of two different muscles depending upon the functional activity. The upper fibers are primarily aligned in a horizontal fashion and the lower fibers are arranged in more of an oblique alignment. One must therefore be selective in the rehabilitation protocol to maximally stimulate the appropriate portion of the subscapularis with the correct exercise.
The intent of this protocol is to provide the clinician with a guideline of the post- operative rehabilitation course of a patient that has undergone a Latarjet procedure for anterior stabilization. It is no means intended to be a substitute for one’s clinical decision making regarding the progression of a patient’s post-operative course based on their physical exam/findings, individual progress, and/or the presence of post- operative complications. If a clinician requires assistance in the progression of a post-operative patient they should consult with the referring Surgeon.
Return to Activities
Computer After 2 weeks Golf 12 weeks (chip & putt only) Tennis 16 weeks (no overhead) Contact Sports 6 months
Rehabilitation after Latarjet procedure
Phase I – Immediate Post Surgical Phase (approximately Weeks 1- 3)
Goals:
- Minimize shoulder pain and inflammatory response
- Protect the integrity of the surgical repair
- Achieve gradual restoration of passive range of motion (PROM)
- Enhance/ensure adequate scapular function
Precautions/Patient Education:
- No active range of motion (AROM) of the operative shoulder
- No excessive external rotation range of motion (ROM) / stretching. Stop at first end feel felt
- Remain in sling, only removing for showering. Shower with arm held at side
- No lifting of objects with operative shoulder
- Keep incisions clean and dry
Activity:
- Arm in sling except when performing distal upper extremity exercises
- (PROM)/Active-Assisted Range of Motion (AAROM)/ (AROM) elbow and wrist/hand
- Begin shoulder PROM (do not force any painful motion)
- Forward flexion and elevation to tolerance
- Abduction in the plane of the scapula to tolerance
- Internal rotation (IR) to 45 degrees at 30 degrees of abduction
- External rotation (ER) in the plane of the scapula from 0-25 degrees; begin at 30-40 degrees of abduction; respect anterior capsule tissue integrity with ER range of motion; (seek guidance from intraoperative measurements of external rotation ROM)
- Scapular clock exercises progressed to scapular isometric exercises
- Ball squeezes
- Sleep with sling supporting operative shoulder, place a towel under the elbow to prevent shoulder hyperextension
- Frequent cryotherapy for pain and inflammation
- Patient education regarding posture, joint protection, positioning, hygiene, etc.
Milestones to progress to phase II:
- Appropriate healing of the surgical repair
- Adherence to the precautions and immobilization guidelines
- Achieved at least 100 degrees of passive forward elevation and 30 degrees of passive external rotation at 20 degrees abduction
- Completion of phase I activities without pain or difficulty
Phase II – Intermediate Phase/ROM (approximately Week 4-9)
Goals:
- Minimize shoulder pain and inflammatory response
- Protect the integrity of the surgical repair
- Achieve gradual restoration of (AROM)
- To be weaned from the sling by the end of week 4-5
- Begin light waist level activites
Precautions:
- No active movement of shoulder till adequate PROM with good mechanics
- No lifting with affected upper extremity
- No excessive external rotation ROM / stretching
- Do not perform activities or strengthening exercises that place an excessive load on the anterior capsule of the shoulder joint (i.e. no pushups, pec flys, etc..)
- Do not perform scaption with internal rotation (empty can) during any stage of rehabilitation due to the possibility of impingement
Early Phase II (approximately week 4):
- Progress shoulder PROM (do not force any painful motion)
- Forward flexion and elevation to tolerance
- Abduction in the plane of the scapula to tolerance
- IR to 45 degrees at 30 degrees of abduction
- ER to 0-45 degrees; begin at 30-40 degrees of abduction; respect anterior capsule tissue integrity with ER range of motion; seek guidance from intraoperative measurements of external rotation ROM)
- Glenohumeral joint mobilizations as indicated (Grade I, II) when ROM is significantly less than expected. Mobilizations should be done in directions of limited motion and only until adequate ROM is gained.
- Address scapulothoracic and trunk mobility limitations. Scapulothoracic and thoracic spine joint mobilizations as indicated (Grade I, II, III) when ROM is significantly less than expected. Mobilizations should be done in directions of limited and only until adequate ROM is gained.
- Begin incorporating posterior capsular stretching as indicated
- Cross body adduction stretch
- Side lying internal rotation stretch (sleeper stretch)
- Continued Cryotherapy for pain and inflammation
- Continued patient education: posture, joint protection, positioning, hygiene, etc.
Late Phase II (approximately Week 6):
- Progress shoulder PROM (do not force any painful motion)
- Forward flexion, elevation, and abduction in the plane of the scapula to tolerance
- IR as tolerated at multiple angles of abduction
- ER to tolerance; progress to multiple angles of abduction once >/= 35 degrees at 0-40 degrees of abduction
- Glenohumeral and scapulothoracic joint mobilizations as indicated (Grade I-IV as appropriate)
- Progress to AA/AROM activities of the shoulder as tolerated with good shoulder mechanics (i.e. minimal to no scapulathoracic substitution with up to 90-110 degrees of elevation.)
- Begin rhythmic stabilization drills
- ER/IR in the scapular plane
- Flexion/extension and abduction/adduction at various angles of elevation
- Continue AROM elbow, wrist, and hand
- Strengthen scapular retractors and upward rotators
- Initiate balanced AROM / strengthening program
- Initially in low dynamic positions
- Gain muscular endurance with high repetition of 30-50, low resistance 1-3 lbs)
- Exercises should be progressive in terms of muscle demand / intensity, shoulder elevation, and stress on the anterior joint capsule
- Nearly full elevation in the scapula plane should be achieved before beginning elevation in other planes
- All activities should be pain free and without substitution patterns
- Exercises should consist of both open and closed chain activities
- No heavy lifting or plyometrics should be performed at this time
- Initiate full can scapular plane raises to 90 degrees with good mechanics
- Initiate ER/IR strengthening using exercise tubing at 0° of abduction (use towel roll)
- Initiate sidelying ER with towel roll
- Initiate manual resistance ER supine in scapular plane (light resistance)
- Initiate prone rowing at 30/45/90 degrees of abduction to neutral arm position
- Continued cryotherapy for pain and inflammation
- Continued patient education: posture, joint protection, positioning, hygiene, etc.
Milestones to progress to phase III:
- Passive forward elevation at least 155 degrees
- Passive external rotation within 8-10 degrees of contralateral side at 20 degrees abduction
- Passive external rotation at least 75 degrees at 90 degrees abduction
- Active forward elevation at least 145 degrees with good mechanics
- Appropriate scapular posture at rest and dynamic scapular control with ROM and functional activities
- Completion of phase II activities without pain or difficulty
Phase III - Strengthening Phase (approximately Week 10 – Week 15)
Goals:
- Normalize strength, endurance, neuromuscular control
- Return to chest level full functional activities
- Gradual and planned buildup of stress to anterior joint capsule
Precautions:
- Do not over stress the anterior capsule with aggressive overhead activities/strengthening
- Avoid contact sports/activities
- Do not perform strengthening or functional activities in a given plan until the patient has near full ROM and strength in that plane of movement
- Patient education regarding a gradual increase to shoulder activities
Activity:
- Continue A/PROM as needed/indicated
- Initiate biceps curls with light resistance, progress as tolerated
- Initiate gradually progressed strengthening for pectoralis major and minor; avoid positions that excessively stress the anterior capsule
- Progress subscapularis strengthening to focus on both upper and lower segments
- Push up plus (wall, counter, knees on the floor, floor)
- Cross body diagonals with resistive tubing
- IR resistive band (0, 45, 90 degrees of abduction
- Forward punch
Milestones to progress to phase IV:
- Passive forward elevation WNL
- Passive external rotation at all angles of abduction WNL
- Active forward elevation WNL with good mechanics
- Appropriate rotator cuff and scapular muscular performance for chest level activities
- Completion of phase III activities without pain or difficulty
Phase IV - Overhead Activities Phase / Return to activity phase (approximately Week 16-20)
Goals:
- Continue stretching and PROM as needed/indicated
- Maintain full non-painful AROM
- Return to full strenuous work activities
- Return to full recreational activities
Precautions:
- Avoid excessive anterior capsule stress
- With weight lifting, avoid tricep dips, wide grip bench press, and no military press or lat pulls behind the head. Be sure to “always see your elbows”
- Do not begin throwing, or overhead athletic moves until 4 months post-op or cleared by MD
Activity:
- Continue all exercises listed above
- Progress isotonic strengthening if patient demonstrates no compensatory strategies, is not painful, and has no residual soreness
- Strengthening overhead if ROM and strength below 90 degree elevation is good
- Continue shoulder stretching and strengthening at least four times per week
- Progressive return to upper extremity weight lifting program emphasizing the larger, primary upper extremity muscles (deltoid, latissimus dorsi, pectoralis major)
- Start with relatively light weight and high repetitions (15-25)
- May do pushups as long as the elbows do not flex past 90 degrees
- May initiate plyometrics/interval sports program if appropriate/cleared by PT and MD
- Can begin generalized upper extremity weight lifting with low weight, and high repetitions, being sure to follow weight lifting precautions.
- May initiate pre injury level activities/ vigorous sports if appropriate / cleared by MD
Milestones to return to overhead work and sport activities:
- Clearance from MD
- No complaints of pain or instability
- Adequate ROM for task completion
- Full strength and endurance of rotator cuff and scapular musculature for task completion
- Regular completion of continued home exercise program
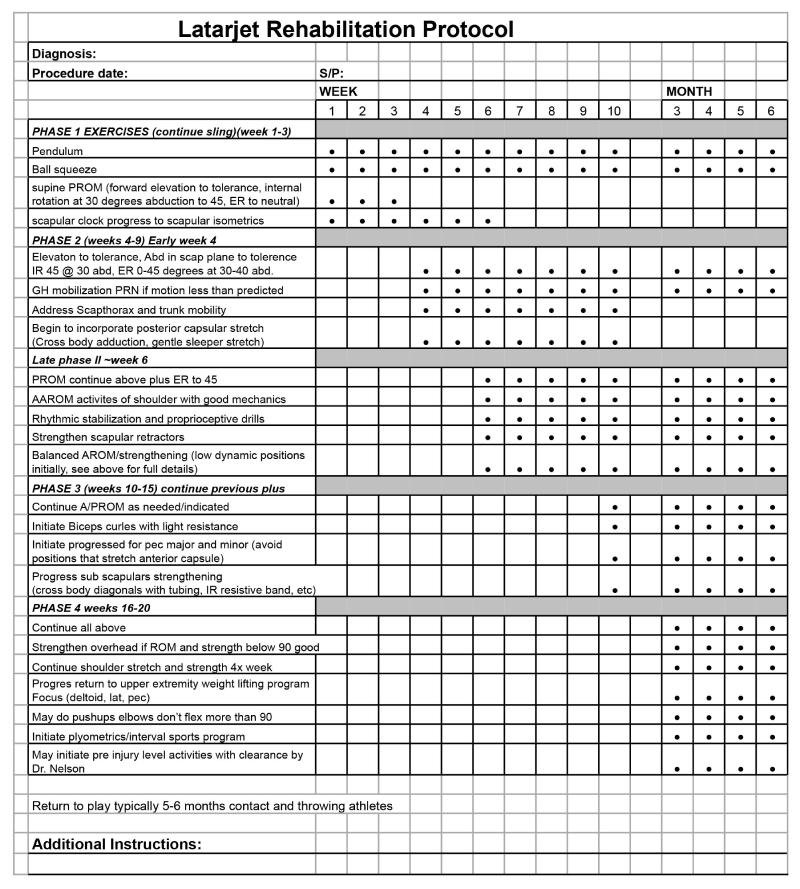
Latarjet Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6
Shoulder Instability (Bankart)
Shoulder Instability (Bankart)
The shoulder joint is comprised of the humerus and glenoid socket. The large head and small socket gives the shoulder joint excellent range of motion. This range of motion however comes at the cost of stability (it takes only a strong breeze to blow the golf ball off the T). A traumatic external force such as a football tackle may cause the shoulder joint to dislocate or subluxate(almost dislocate).
The labrum is a cartilaginous structure that acts as a bumper or lip to maintain the shoulder joint in place. A dislocation will tear the labrum off the glenoid surface and stretch associated ligaments. This type of labral tear is called a “Bankart tear”.
After the first dislocation the patient is at an increased risk for subsequent dislocations. The events that cause further dislocations need not be as forceful as the original. Imagine trying to balance a golf ball on a T that only had half of its top in place. Simple activities such as moving in bed or putting on a book bag may cause shoulder subluxation or dislocation. In order to return stability to the shoulder joint, the labrum should be reattached and the supporting ligaments tensioned. People who are high impact athletes or recurrent dislocations an open procedure may be indicated.
Diagnosis of a Bankart Tear:
The patient with a labral tear often reports multiple shoulder dislocations from low velocity activities as described above. Patients report a feeling of apprehension with certain shoulder movements such as lifting the arm overhead or throwing a ball. Labral tears and ligament laxity are diagnosed by reviewing the shoulder history and participating in a physical examination. X-rays looking for associated trauma to the shoulder joint and MRI to examine the condition of the labrum are often utilized to aid in the diagnosis.
Conservative management may be utilized after the initial dislocation. This consists of very short term sling immobilization followed by physical therapy for shoulder joint strengthening. Surgical repair is the treatment of choice for the patient with multiple dislocations and an unstable shoulder joint. Without surgical intervention, the torn labrum and stretched ligaments are unlikely to heal properly and provide for a stable shoulder joint. The surgical repair is conducted utilizing arthroscopic equipment. This means that a small camera and small equipment will be used through tiny incisions. Anchors attached with suture material are placed in the glenoid bone. The sutures are then passed through the labral tissue. A knot is tied which brings the labrum tightly against the bone reestablishing its natural position and ligament tension
RESULTS AND RISKS OF SURGERY
The success rate of the open Bankart repair is approximately 95%. The success rate of arthroscopic Bankart repair can be similar, assuming there is little or no bone loss. If there is a fracture of the glenoid rim (Bankart fracture) and a compression fracture of the humeral head (Hill-Sachs lesion), there is an increased risk of recurrent instability following repair.
Two nerves are at risk during surgery since they are near the operative field, but they are rarely injured. As with any surgical procedure, there are potential risks: The incidence of infection is less than 0.5%. The shoulder can lose some motion after surgery, especially if the shoulder has to be significantly tightened because of excess laxity. Recurrent instability can occur.
Surgery:
The length of an open capsular shift will take approximately 1.5 hours depending on the complexity of the tear. Your nurse will bring you into the pre-op area were you will have an IV placed and met with your anesthesiologist. General anesthesia is utilized to assure a comfortable surgery. This means that you will be “asleep” and completely unaware of the surgery until you wake up in the recovery area. Most patients will have a small tube placed in there windpipe, formal intubation may not be required. Local blocks are also available to supplement pain control. Your anesthesiologist will discuss this with you prior to surgery. Like any surgical procedure, there are risks. These risks are extremely rare and consist of nerve injury, infection and shoulder stiffness or instability.
Post-Surgery:
After the surgery is completed, you will awaken in the operating room and be moved to the recovery area. Most patients generally recover smoothly and have minimal pain due to local pain medication that is used at the completion of the surgery. Family members and guests are permitted to visit in the recovery area once the patient is fully awake and feeling comfortable; this may take up to 2 hours after the surgery is completed.
- A pain medication prescription will be provided prior to discharge. You may take the prescribed medication as directed. You should expect to experience moderate shoulder discomfort for several days and even weeks following the surgery. Patients often only need prescription narcotics for a few days following surgery and then can switch to over-the-counter medications Tylenol or Ibuprofen. Ice should be applied to the shoulder up to three times a day for 20 minutes until swelling subsides
- At the completion of surgery, you will have a sling placed on your arm. Wear the sling at all times with the exception of exercises, showering and dressing. You may also remove the sling to participate in computer work or watching TV for instance. The purpose of the sling is to protect the repair. Excessive arm movement during the first few weeks of recovery may put unwarranted strain on the repair. Particularly avoid external rotation or rotation away from the body for at least 6 weeks.
- Special cooling devices (called Cryo/Cuffs) are also available for patients to purchase thru our office. This can be used in the place of the ice bags.
- If the bandage is draining, reinforce it with additional dressings for the first 48 hours. After 48 hours remove the bandage and place band aids over the incision sites. Showering is acceptable at this time. Do not scrub the shoulder.
- There is an exercise sheet at the end of this packet. Conduct exercises three times daily until further directions are provided. Physical therapy will start 4-6 weeks after surgery.
- Eat a regular diet as tolerated and please drink plenty of fluids.
- You are unable to drive a car as long as you need to utilize a sling.
- Call office for Temperature >102 degrees, excessive swelling, pain or redness around the incision sites.
- Plan at least a week away from work or school. Utilize this time to decrease swelling and participate in your home exercise program. You may be able to resume work (depending on type of work and setting; very variable) once the pain and swelling resolves.
- The above are guidelines and only intended as generalities.
Rehabilitation after Open Capsular shift
Phase 0: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS
You will wake up in the operating room. A sling and an ice pack will be in place. You will go to the recovery room and generally will be discharged after 1-2 hours. You can get out of bed when you wish. Apply ice to the shoulder to reduce pain and swelling. You may remove the sling whenever you wish and gently move the elbow, wrist and fingers. Follow the instructions on your discharge paperwork or refer to Dr. Nelson’s website for further postoperative questions.
GOALS:
- Control pain and swelling
- Protect the repair
- Begin early shoulder motion
ACTIVITIES WHEN YOU GO HOME:
- Apply ice to the shoulder as tolerated to reduce pain and swelling. You can change the dressing to a smaller one to allow the cold therapy to reach the shoulder.
- Remove the sling on the first day after surgery. Move your elbow, fingers and hand several times per day.
- Begin the pendulum exercise several times per day: Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion. Repeat for 2 to 3 minutes at a time.
- Remove the outer dressing on the second day after surgery and shower. Leave the little pieces of tape (steri-strips) in place. You can get the wound wet after 2 days in a shower, but do not soak in a tub. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position.
- Keep your elbow slightly in front of your body; do not reach behind your body. When putting on clothing, lean forward and pull the shirt up and over the operated arm first. Then put the other arm into the opposite sleeve. To remove the shirt, take the non-operative arm out of the sleeve first, and then slip the shirt off of the operated arm.
- Call your surgeon's office for any concerns, including, but not limited to, severe pain, fevers, chills or redness.
OFFICE VISIT:
Please arrange to come back to Greater Michigan Orthopedics office 7-10 days after surgery for examination and further instructions.
Phase 1: 2 to 5 weeks after surgery
Goals:
- Protect the repair
- Ensure wound healing
- Prevent shoulder stiffness
Activities:
- Sling Use your sling as instructed by your surgeon. You may remove it whenever you wish if you are careful and keep the shoulder safe. Put the sling on when you are outside or in a crowd. Keep the sling on when sleeping at night for the first three or four weeks.
- Use of the operated arm You may use your hand on the operated arm as long as you do not rotate the arm externally or away from your body. You should bend your arm at the elbow and use your fingers and hand, such as to reach up and touch your face. Keep your elbow in front of you.
- Bathing and showering You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
Phase 2: 5 to 8 weeks after surgery
Goals:
- Protect the shoulder and avoid over stressing the repair
- Improve range of motion of the shoulder
- Begin strengthening exercises
Activities:
- Sling The sling is no longer necessary.
- Use of the operated arm You may now use your arm. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
- Precautions Do not lift objects overhead with the weight of the object going behind the head. In other words, keep objects in front of you where you can see them.
- Use ice or cold as necessary 15-20 minutes.
Phase 3: 8 to 12 weeks after surgery
Goals:
- Protect the shoulder repair
- Regain full range of motion
- Continue gentle strengthening
Activities:
Use of the operated arm You may now use your arm in a more normal fashion. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
Precautions Do not lift heavy weights overhead with the weight going behind the head. In other words, keep the weights in front of you where you can see them.
Phase Four: 12 to 24 weeks after surgery
Goals:
- Protect the ligament repair
- Regain full range of motion
- Continue strengthening
- Gradual return to full activity
Activities:
Use the arm for normal daily activities. There is no restriction on your range of motion unless exceptions are outlined in your discussions with your doctor. Weight training can gradually resume with caution being paid to exercises such as bench press, incline press, dips, pull-downs behind the neck or other exercises where the hands are repeatedly placed behind you. If you are returning to contact sports, you should wait until six months after surgery.
Guidelines for Returning to Weight Training After Open capsular shift Repair
You should not return to training using heavy weights or on weight machines until your surgeon determines that it is safe. In general, it is usually safe to return to heavier weight training at 3-4 months following surgery.
Before embarking on a weight-training program, you should have full range of shoulder motion and normal strength in the rotator cuff and scapular muscles. Your surgeon or a physical therapist will test your motion and strength before you start weight training.
When starting your weight-training program, you can start with 3 sets of 15-20 repetitions. Training with high repetition sets ensures that the weights that you are using are not too heavy.
NEVER perform any weight training exercise to the point of muscle failure. “Muscle failure” occurs when, in performing a weight training exercise, the muscle is no longer able to provide the energy necessary to contract and move the joint(s) involved in the particular exercise. Joint, muscle and tendon injuries are more likely to occur when muscle failure occurs.
The following weight training exercises should be avoided after Bankart repair for shoulder instability:
- Pull downs behind-the-neck (wide-grip)
- Behind-the-neck shoulder press
- Wide-grip bench press
- Standing lateral deltoid raises
- Triceps press overhead
The following exercises require special cautions:
- Pull downs should only be done in front of the head, to the chest, with a medium(not wide) grip.
- Shoulder press overhead should be done carefully, avoiding heavy weights. If doing shoulder presses, always start with the hand in front of the shoulder and end overhead where you can still see your hand. For persons using barbells, this is the “military press”.
- If bench pressing, your grip should be no wider than the wider than the width of your shoulders. Avoid any exercises using grips wider or narrower than shoulder width.
- Lateral deltoid raises should be avoided because of the impinging and wearing effect on the rotator cuff. Forward raises in the “thumb-up” position are usually safer and can be done with reasonable weights. Lateral raises from the prone or bent over position can be done as a substitute for standing lateral deltoid raises.
- When doing incline bench press with barbells, there is a danger of shoulder dislocation if the lifter loses control of the bar when returning the barbell to the rack of the incline bench. Always have a spotter for removing and replacing the barbell in this exercise.
- If you are doing any type of “chest-fly”, keep in mind the following precuations. Do not do any chest-fly exercise with straight elbows. Always allow the elbows to bend and never lower your hands (holding dumbbells) below the level of your chest.
- If you are using a “Pec-Deck” machine, never let the weight stretch the arms so that your elbows pass behind your chin. You can set the arms on this machine a few clicks forward to adjust the maximum motion allowed.
- If you a performing “dips” using a set of parallel bars, never lower yourself below the point where the elbows reach a 90-degree angle.
- For triceps exercises, triceps pushdowns on a pulley system are safe as well as bent- over triceps extensions.
- When doing the upright-rowing exercise, keep your grip at least 12 inches apart. When pulling the bar upward toward the chin, do not raise the bar higher than the point at which the elbow reaches shoulder level.
Exercises Usually Problem-Free
- Biceps Curls
- Cable and bent-over rowing
- Shoulder shrugs
Return to Activities
Computer After 2 weeks Golf 8 weeks (chip & putt only) Tennis 12 weeks (no overhead) Contact Sports 4 months
Open capsular shift Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6
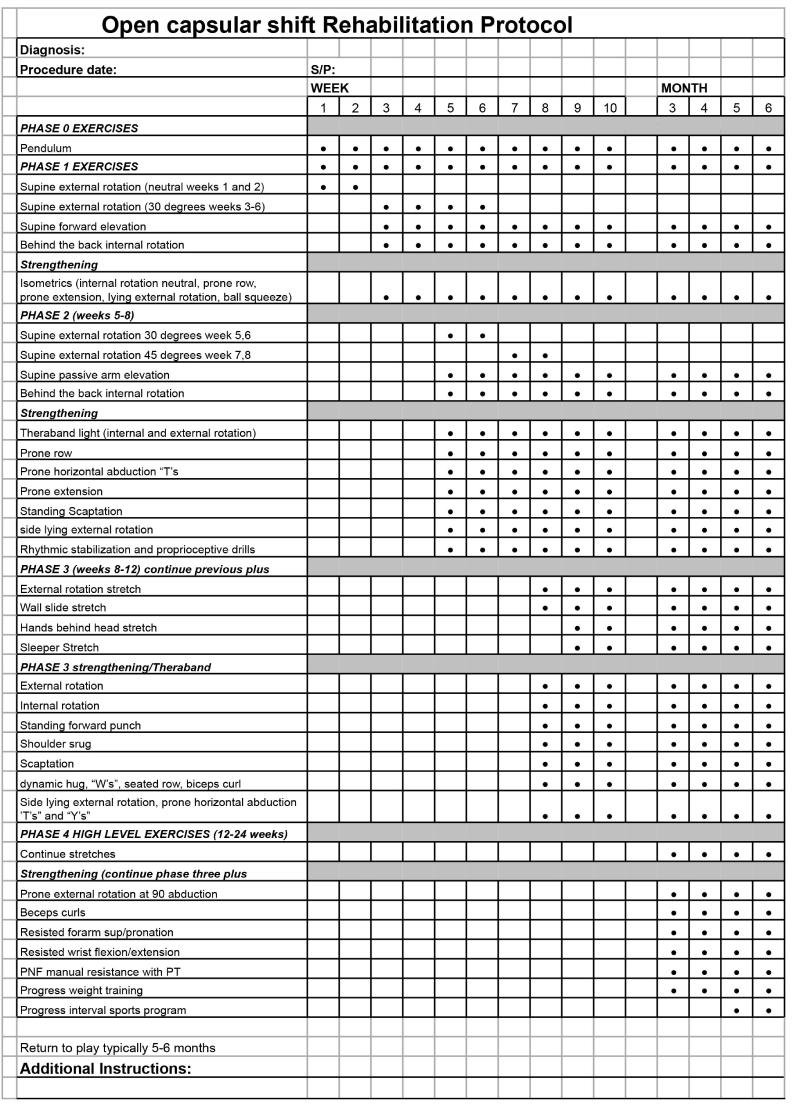
Pectoralis Major Repair
Pectoralis Major Repair
The pectoralis major muscle is the large muscle in front of the upper chest. There are two parts of the pectoralis muscle, the pectoralis major and the pectoralis minor. The pectoralis major is the larger of the two, and works to push the arms in front of the body, such as in doing a push-up or bench press exercise.
Pectoralis Major Muscle Rupture
The pectoralis major muscle, or most commonly its tendon that attaches to the arm bone (the humerus), can rupture. Athletes commonly call this a "pec rupture" but it is more accurately called a pectoralis major muscle rupture. Pectoralis major ruptures are uncommon injuries that occur almost exclusively in men between the ages of 20 to 50. While partial tears can occur, these are less common, and usually a complete rupture of the tendinous attachment of the muscle to the bone occurs.
How does a pectoralis major muscle rupture occur?
These injuries generally occur during forceful activities. A large number of pec major ruptures occur during weightlifting, particularly during a bench press exercise. Other causes of a pectoralis major rupture include football, wrestling, rugby, and other causes due to trauma.
What are the symptoms of a pectoralis major muscle rupture?
Patients who experience a pectoralis major rupture feel sudden pain, and often a tearing sensation in their chest. Symptoms include:
- Pain in the chest and upper arm
- Weakness in pushing the arms out in front of the body
- Bruising in the chest and arm
- A dimpling, or pocket, formed just above the arm pit where the rupture occurred
Treatment of Pectorals Muscle Rupture
Surgery is most often recommended for complete tears of the pectorals muscle tendon. People who have partial tears, tears within the muscle or low-demand patients may be able to avoid surgical treatment.
By repairing the torn tendon, patients have a good chance at returning to high-level sports and activities. Ideally the repair is performed in the early period following the injury. By performing the repair within several weeks of the injury, scar tissue and muscle atrophy are minimized.
The repair is performed by placing sutures in the torn tendon, and then securing these sutures to the arm bone with either holes in the bone or anchors inserted into the bone.
Rehab after Pectoralis major repair
Phase 0: 0-2 weeks after surgery.
Postoperative Instructions
You will wake up in the operating room. A sling and an ice pack will be in place. You will go to the recovery room and generally will be discharged after 1-2 hours. You can get out of bed when you wish. Apply ice to the front of the shoulder to reduce pain and swelling. You may remove the sling whenever you wish and gently move the elbow, wrist and fingers. Please follow your surgeon's post operative instructions regarding moving your shoulder after surgery.
Goals:
- Control pain and swelling
- Protect the repair
- Begin early shoulder motion
Activities When You Go Home:
1. Apply ice to the shoulder as tolerated to reduce pain and swelling. You can change the dressing to a smaller one to allow the cold therapy to reach the shoulder.
2. Remove the sling on the first day after surgery. Move your elbow, fingers and hand several times a day.
3. Begin the pendulum exercise several times a day: Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion. Repeat for 2 to 3 minutes at a time.
4. Remove the outer dressing on the second day after surgery and shower. Leave the little pieces of tape (steri-strips) in place. You can get the wound wet after 2 days in a shower, but do not soak in a tub. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position.
5. Keep your elbow slightly in front of your body; do not reach behind your body. When putting on clothing, lean forward and pull the shirt up and over the operated arm first. Then put the other arm into the opposite sleeve. To remove the shirt, take the unoperated arm out of the sleeve first, and then slip the shirt off of the operated arm.
5. Call Greater Michigan Orthopedics with any questions or concerns.
Office Visit: Please arrange to return to your surgeon's office in the office 10-14 days after surgery.
Rehab after Pectoralis major repair
Phase 1: 2-6 weeks after surgery.
Goals:
- Protect the repair
- Ensure wound healing
- Prevent shoulder stiffness
Activities:
1. Sling
Use your sling as instructed by your doctor. You may remove it whenever you wish if you are careful and keep the shoulder safe. Put the sling on when you are outside or in a crowd. Keep the sling on when sleeping at night for the first three or four weeks.
2. Use of the operated arm
You may use your hand on the operated arm as long as you do not rotate the arm externally or away from your body. You should bend your arm at the elbow and use your fingers and hand, such as to reach up and touch your face. Keep your elbow in front of you.
3. Bathing and showering
You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise. Do not submerge the incisions under water.
Ice
Ice the arm 15-20 minutes duration 4-5 times per day as needed to decrease swelling and pain.
Stretching/Passive Motion
Days per week: 7 Times per day: 4-5
Exercises:
- Pendulums
- Supine External rotation (week 2-4 limit to 0 degrees or straight up and 5-6 limit to 30 degrees)
- Supine forward elevation as tolerated start week 3
Strengthening Exercises
Days per week: 7 Times per day: 4-5
Exercises:
- Isometric External rotation at neutral
- Prone row
- Prone extension do not extend past hip
- Side-lying external rotation to above stated limits
- Rhythmic stabilization and proprioceptive training drills
- Ball squeeze exercise
Rehab after Pectoralis major repair
Phase 2: 7-12 weeks after surgery.
Goals:
- Protect the shoulder repair
- Regain full range of motion
- Continue gentle strengthening
Activities:
1. Use of the operated arm
You may now use your arm in a more normal fashion. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
2. Precautions
Do not lift heavy weights overhead with the weight going behind the head. In other words, keep the weights in front of you where you can see them.
Exercise Program:
Stretching / Motion
Days per week: 7 Times per day: 1-2
- Pendulum exercises
- Standing external rotation
- Doorway Wall slide stretch
- Hands-behind-head stretch
- (Starting the 9th week after surgery)
- Behind the back internal rotation
- Supine cross-chest stretch
- Sidelying internal rotation
Strengthening / Theraband
Days per week: 7 Times per day: 1
- Scapular stabilizer strengthening
- Biceps
- Triceps
- Rotator cuff
- Initiate closed-chain scapula exercises
- No resisted IR/ADDuction
Rehab after Pectoralis major repair
Phase 3: 12-24 weeks after surgery.
Goals:
- Protect the ligament repair
- Regain full range of motion
- Continue strengthening
- Gradual return to full activity
Activities:
Use the arm for normal daily activities. There is no restriction on your range of motion unless exceptions are outlined in your discussions with your doctor. Weight training can gradually resume with caution being paid to exercises such as bench press, incline press, dips, pull-downs behind the neck or other exercises where the hands are repeatedly placed behind you. If you are returning to contact sports, you should wait until six months after surgery.
Exercise Program
Stretching / Range of Motion
Times per day: 1 Days: 5-7
- Standing External Rotation / Doorway Wall slide Stretch
- Hands-behind-head stretch
- Behind the back internal rotation
- Supine Cross-Chest Stretch
- Sidelying internal rotation
- External rotation at 90 Abduction stretch
Strengthening / Theraband
Times per day: 1 Days per week: 3
- Continue exercises from phase 2
- Internal Rotation
- Forward Punch
- Dynamic Hug
- Diagonal down
Optional exercises:
- External rotation at 90
- Internal rotation at 90
- Standing 'T's
- Diagonal up
Strengthening / Dynamic
Times per day: 1 Days per week: 3
- Prone external rotation at 90 abduction "U's"
- Biceps curls
- Resisted forearm supination-pronation Resisted wrist flexion-extension
- PNF manual resistance with physical therapist
- Push-up progression
Return to play is approximately 6 months if strength and motion restored. Please refrain from starting sport specific exercises until 16 weeks post operative. Running may start at 12 weeks post operative.
Pectoralis Major Repair Rehabilitation Protocol
Diagnosis:
Procedure date: S/P:
| Exercise | Week | Month | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 3 | 4 | 5 | 6 | |
| PHASE 0 EXERCISES (week 0-2) | ||||||||||||||
| Pendulum | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ||||
| Continue Shoulder immobilizer | ● | ● | ● | ● | ● | ● | ||||||||
| PHASE 1 EXERCISES (week 2-6) | ||||||||||||||
| Continue immobilizer except hygiene and exercise | ● | ● | ● | ● | ● | |||||||||
| Supine external rotation (wk 2-4 0 deg 5-6 30 deg) | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Supine forward elevation as tolerated to 90 | ● | ● | ● | ● | ● | |||||||||
| Isometric External rotation at 0 | ● | ● | ● | ● | ● | |||||||||
| Prone Row, Prone extension to hip | ● | ● | ● | ● | ● | |||||||||
| Ball Squeezes | ● | ● | ● | ● | ● | ● | ● | ● | ● | |||||
| PHASE 2 (weeks 7-12) Active motion phase | ||||||||||||||
| Standing ER as tolerated to 45, behind back IR | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Doorway wall slide stretch | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Hands-behind head stretch (start week 9) | ● | ● | ● | ● | ● | ● | ||||||||
| Begin incorporating Posterior capsular stretch (cross body adduction supine, sleeper stretch) | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Initiate strengthening Biceps, Triceps, Rotator cuff | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Initiate scapula stabilization (closed chain) | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| PHASE 3 (weeks 12-24) continue previous plus | ||||||||||||||
| External rotation at 90 abduction stretch | ● | ● | ● | ● | ||||||||||
| Continue phase 2 strengthening plus | ● | ● | ● | ● | ||||||||||
| Theraband IR, Forward punch, Dynamic hug, Diag down | ● | ● | ● | ● | ||||||||||
| Optional theraband: ER, IR at 90 abd, Standing T | ● | ● | ● | ● | ||||||||||
| Dynamic strengthening Prone external rotation at 90 (U) | ● | ● | ● | ● | ||||||||||
| Biceps curls | ● | ● | ● | ● | ||||||||||
| Resisted forearm pronosupination wrist flexion/extension | ● | ● | ● | ● | ||||||||||
| Progres return to upper extremity weight lifting program Focus (deltoid, lat, pec) | ● | ● | ● | |||||||||||
| Initiate plyometrics/interval sports program | ● | ● | ● | |||||||||||
| May initiate pre injury level activities with clearance by your surgeon | ● | |||||||||||||
| Return to play typically 5-6 months | ||||||||||||||
Additional Instructions:
Posterior Shoulder Instability
Posterior Shoulder Instability
Posterior shoulder instability accounts for approximately 5% of cases of instability of the glenohumeral joint, although its incidence may be greater in population groups that routinely use their arms in ways likely to provoke injury to the shoulder joint, such as football players, weight lifters, and rock climbers. The condition can occur as a consequence of an acute event or through repeated microtranslation of the shoulder joint. Although acute injuries or dislocations of the shoulder are more readily identified than is repeated microtrauma, the latter can result from recurrent, insidious instances of instability, such as from the repeated imposition of a load posteriorly across the shoulder, as in the case of bench press or inclined press exercises in weight lifting, or in push-ups. The acute events responsible for PSI can be secondary to a forceful impact and shearing, as in blocking by a football lineman, or can result from fatigue of the structures that stabilize the shoulder, leading to laxity of the shoulder capsule, as in overhead throwing and swimming.
Non Surgical treatment
Physical therapy for patients with PSI should focus on scapulothoracic mechanics and strengthening of the rotator cuff, and specifically of the subscapularis muscle. Two thirds of patients will respond in programs for strengthening and improving proprioception. Most of these responders are patients with a history of repetitive microtrauma, as opposed to those who have had a single traumatic event or who have clear labral pathology, who will more likely require surgical stabilization. Although not a hard and fast rule, patients with GIRD and posterior instability are likely to derive greater benefit from therapy than those in whom labral pathology is the result of a forceful, shearing event, such as football linemen and weight lifters. Nevertheless, despite the tendency of GIRD to respond to therapy, labral pathology commonly requires arthroscopic treatment. The results in patients with GIRD and posterior instability are dramatic, with a 90% response to therapy, as opposed to only a 10% response in those with traumatic injuries. Notwithstanding this, patients who are identified as having PSI should have their scapular mechanics optimized and undergo strengthening before any surgical management of their condition is undertaken. Patients with a history of nontraumatic dislocation of the shoulder who do not have psychological pathology or a voluntary component of their disorder usually demonstrate stability at an average of 5 weeks with a dedicated program of scapular strengthening and conditioning. Although there is no established duration for such a program, the authors believe that it should continue for at least 3 to 6 months.
Surgical Management
Indications for arthroscopic stabilization of the unstable posterior shoulder are recurrent, posttraumatic, unidirectional posterior subluxation; multidirectional instability with symptoms accompanying motion in the posteroinferior direction; and symptomatic posterior labral tears. There are rare instances for open surgery, but complications are significantly higher and historically only successful 30-70% of the time.
Surgical Risks
- Infection <1/1000
- Recurrent instability 12-15%
- Nerve palsy <1%
- Stiffness
Outcomes
Current studies show promising results of the arthroscopic surgical repair of PSI, although not as positive as those for anterior shoulder instability. In a series of 33 patients with an average follow-up of 39.1 months found an average score of 95 on the American Shoulder and Elbow Surgeons (ASES) Standardized Shoulder Assessment Form and a value of 82% of normal on the Western Ontario Shoulder Instability (WOSI) Index. Four of the patients had recurrent instability, with the worst outcomes occurring in patients whose PSI had a voluntary positional component. Similarly, Bradley et al reported an average ASES score of 85 at an average of 27 months after the arthroscopic repair of 100 shoulders with PSI, with a failure rate of about 15%. Ninety percent of the patients returned to athletic activity, with 67% resuming such activity at the same level as before their injuries.
Posterior Shoulder Instability
Phase 0: immediately after surgery.
Postoperative Instructions
You will wake up in the operating room. A sling and an ice pack will be in place. You will go to the recovery room and generally will be discharged after 1-2 hours. You can get out of bed when you wish. Apply ice to the front of the shoulder to reduce pain and swelling. You may remove the sling whenever you wish and gently move the elbow, wrist and fingers. Please follow your surgeon's post operative instructions regarding moving your shoulder after surgery.
Goals:
- Control pain and swelling
- Protect the repair
- Begin early shoulder motion
Activities When You Go Home:
1. Apply ice to the shoulder as tolerated to reduce pain and swelling. You can change the dressing to a smaller one to allow the cold therapy to reach the shoulder.
2. Remove the sling on the first day after surgery. Move your elbow, fingers and hand several times a day.
3. Begin the pendulum exercise several times a day: Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion. Repeat for 2 to 3 minutes at a time.
4. Remove the outer dressing on the second day after surgery and shower. Leave the little pieces of tape (steri-strips) in place. You can get the wound wet after 2 days in a shower, but do not soak in a tub. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position.
5. Keep your elbow slightly in front of your body; do not reach behind your body. When putting on clothing, lean forward and pull the shirt up and over the operated arm first. Then put the other arm into the opposite sleeve. To remove the shirt, take the unoperated arm out of the sleeve first, and then slip the shirt off of the operated arm.
5. Call or email Dr. Nelson with any questions or concerns.
Office Visit: Please arrange to return to your surgeon's office in the office 10-14 days after surgery.
Rehabilitation after Arthroscopic Posterior Bankart Repair
Phase One: 0 to 4 weeks after surgery
Goals:
- Allow healing of the repaired capsule
- Initiate early protected and restricted range of motion
- Retard muscular atrophy
- Decrease pain/inflammation
Activities:
1. Sling
Use your sling until 6 weeks post operative. If you remove the sling, be careful and keep the shoulder safe. The sling must be worn at all times with the exception of exercise activity and bathing. Keep the sling on when sleeping at night for the first four weeks.
2. Use of the operated arm
You may use your hand on the operated arm as long as you do not raise the hand above your head or reach across the front of your body. Also, do not reach your hand behind you as if to tuck in your shirt or to loop your belt. You should bend your arm at the elbow and use your fingers and hand, such as to reach up and touch your face. Keep your elbow in front of you. Do not bear the weight of the body on your arm.
3. Bathing and showering
You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise. Do not submerge the incisions under water.
4. ICE
Continue to use ice as needed 15-20 minutes.
Stretches/Passive motion
Days per week: 7 Times per day: 1
- Pendulum exercises
- Supine External rotation
- Supine forward elevation limit 120
- No internal rotation
- No horizontal adduction
- Ball Squeeze
Phase Two: 4 to 6 weeks after surgery
Goals:
- Gradual increase in ROM
- Improve strength
- Decrease pain/inflammation
- Protect the labrum repair
Activities:
1. Sling
Continue sling until 6 weeks post surgery.
2. Use of the operated arm
You may now carefully use your arm. Avoid having the arm forcefully pulled behind you or across your chest in front of you. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
3. Precautions
You may use your hand on the operated arm as long as you do not raise the hand above your head or reach across the front of your body. Also, do not reach your hand behind you as if to tuck in your shirt or to loop your belt. You should bend your arm at the elbow and use your fingers and hand, such as to reach up and touch your face. Keep your elbow in front of you. Do not bear the weight of the body on your arm.
4. Ice
Use ice or cold as necessary 15-20 minutes.
Stretching/ Active motion
Times per week: 7 Times per day: 1-3
- Pendulum
- Supine External Rotation
- Hands-behind-head stretch
- Standing external rotation stretch
- Supine forward flexion: Limit 140 pain free
Strengthening/Theraband
Times per week: 7 Times per day: 1
- Theraband internal (to neutral) and external rotation
- Standing forward flexion to 90 (scaption)
- Prone row
- Prone Extension
- Biceps curl
- Side-lying External rotation
Phase Three: 7 to 12 weeks after surgery
Goals:
- Protect the shoulder repair
- Regain full range of motion
- Continue gradual strengthening
Activities:
1. Use of the operated arm
You may now use your arm in a more normal fashion. You may move the arm into all positions including behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you, pulled across the chest or bearing weight as if doing a push-up. Continue to avoid heavy weight lifting or manual labor. Follow any further instructions given to you by your doctor.
2. Precautions
Do not lift heavy objects overhead with the weight going behind the head. In other words, keep objects in front of you where you can see them.
Stretching/ROM
Times per week: 7 Times per day: 1-2
- Pendulums
- External rotation at 90 abduction stretch
- Wall slide Stretch
- Hands behind Head stretch
- Standing External rotation Stretch
- Standing forward flexion
- Behind the back internal rotation (start week 8)
- Horizontal adduction stretch (start week 8)
Strengthening/ Theraband
- External rotation
- Internal rotation
- Standing forward punch
- Shoulder Shrug
- Dynamic hug
- "W's"
- Seated row
- Biceps curl
Strengthening/ Dynamic
- Side-lying external rotation
- Prone horizontal arm raises "T's"
- Prone scaption 'Y'
- Prone row
- Prone extension
- Standing forward flexion "full-can" exercise
- Rhythmic stabilization and proprioceptive
Phase Four: 13-20 weeks after surgery
Goals:
- Protect the ligament repair
- Regain full range of motion
- Continue strengthening
- Gradual return to full activity
Activities:
Use the arm for normal daily activities but continue to cautious to avoid excessive or forceful reaching across the front of the body. Also be cautious when reaching behind your body. Continue to avoid bearing weight as if pushing open a door or doing a push-up.
Stretching / Range of Motion
- External rotation
- Wall slide
- Hands behind head
- Behind back internal rotation
- Supine Cross-Chest stretch
- Side-lying internal rotation (sleeper stretch)
- External rotation at 90 abduction stretch
Strengthening / Theraband
Continue Previous plus
- External rotation at 90
- Internal rotation at 90
- Standing 'T's'
- Diagonal up
- Diagonal down
Strengthening / Dynamic
Continue Previous
- Resisted forearm supination pronation
- Resisted wrist flexion-extension
- Machine resistance (see lifting last page)
- Closed chain program (see last page)
- PNF manual resistance with therapist
Phase Five: 21 weeks after surgery and onward
Goals:
- Progression of functional activities
- Maintain full range of motion
- Continue progressive strengthening
Exercise Program:
Stretching / Range of Motion
Days per week: 5-7 Times per day: 1
- Continue all exercises from phase 4
Strengthening / Theraband
Days per week: 3 Times per day: 1
- Continue from phase 4
Strengthening / Dynamic
Days per week: 3 Times per day: 1
- Continue from phase 4
Plyometric Program
Days per week per physical therapist
May process weight bearing program:
- Ball on wall
- Pushup on unstable surface
Weight Training
Days per week per physical therapist
See weight training precautions section Machine resistance (limited ROM):
- Latissimus dorsi pull downs
- Seated row
- Seated bench press
Guidelines for Returning to Weight Training After Arthroscopic Labrum Repair
You should not return to training using heavy weights or on weight machines until your surgeon determines that it is safe. In general, it is usually safe to return to heavier weight training at three to four months following labrum repair. Before embarking on a weight-training program, you should have full range of shoulder motion and normal strength in the rotator cuff and scapular muscles. The doctor or a physical therapist will test your motion and strength before you start weight training.
When starting your weight-training program, you can start with 3 sets of 15-20 repetitions. Training with high repetition sets ensures that the weights that you are using are not too heavy.
NEVER perform any weight training exercise to the point of muscle failure. "Muscle failure" occurs when, in performing a weight training exercise, the muscle is no longer able to provide the energy necessary to contract and move the joint(s) involved in the particular exercise. Joint, muscle and tendon injuries are more likely to occur when muscle failure occurs.
The following weight training exercises should be avoided after Bankart repair for shoulder instability:
- Pull downs behind-the-neck (wide-grip)
- Behind-the-neck shoulder press
- Wide-grip bench press
- Standing lateral deltoid raises
- Triceps press overhead
The following exercises require special cautions:
- Pull downs should only be done in front of the head, to the chest, with a medium (not wide) grip.
- Shoulder press overhead should be done carefully, avoiding heavy weights. If doing shoulder presses, always start with the hand in front of the shoulder and end overhead where you can still see your hand. For persons using barbells, this is the "military press".
- If bench pressing, your grip should be no wider than the wider than the width of your shoulders. Avoid any exercises using grips wider or narrower than shoulder width.
- Lateral deltoid raises should be avoided because of the impinging and wearing effect on the rotator cuff. Forward raises in the "thumb-up" position are usually safer and can be done with reasonable weights. Lateral raises from the prone or bent over position can be done as a substitute for standing lateral deltoid raises.
- When doing incline bench press with barbells, there is a danger of shoulder dislocation if the lifter loses control of the bar when returning the barbell to the rack of the incline bench. Always have a spotter for removing and replacing the barbell in this exercise.
- If you are doing any type of "chest-fly", keep in mind the following precautions. Do not do any chest-fly exercise with straight elbows. Always allow the elbows to bend and never lower your hands (holding dumbbells) below the level of your chest.
- If you are using a "Pec-Deck" machine, never let the weight stretch the arms so that your elbows pass behind your chin. You can set the arms on this machine a few clicks forward to adjust the maximum motion allowed.
- If you a performing "dips" using a set of parallel bars, never lower yourself below the point where the elbows reach a 90-degree angle.
- For triceps exercises, triceps pushdowns on a pulley system are safe as well as bent-over triceps extensions.
- When doing the upright-rowing exercise, keep your grip at least 12 inches apart. When pulling the bar upward toward the chin, do not raise the bar higher than the point at which the elbow reaches shoulder level.
Exercises Usually Problem-Free: 1. Biceps Curls 2. Cable and bent-over rowing 3. Shoulder shrugs
If your goal is returning to high-level weight training or weight lifting, it will take 3 to 6 months of cautious, gradual progression to return to top form. In general, avoid increasing the amount of weight lifted by more than 10-15% (at a time) of your present working weight every 10-14 days.
Remember: Weight training is beneficial to improve muscular strength and protect the joints from injury. If done improperly by using too much weight and/or improper technique, weight training can cause serious injury.
Dr. Ryan Nelson
861 Health Park Blvd.
Grand Blanc, MI 48439
(810) 953-0500
www.DrRNelson.com
ryan.Nelson@DrRNelson.com
Posterior Bankart Repair Rehabilitation Protocol
Diagnosis:
Procedure date: S/P:
| Exercise | Week | Month | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 3 | 4 | 5 | 6 | |
| PHASE 0 EXERCISES (week 0-2) | ||||||||||||||
| Pendulum | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ||||
| Continue Shoulder immobilizer | ● | ● | ● | ● | ● | ● | ||||||||
| PHASE 1 EXERCISES (week 0-4) | ||||||||||||||
| Supine ER, forward elevation limit 120 | ● | ● | ● | ● | ||||||||||
| Ball Squeeze | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● |
| PHASE 2 EXERCISES (week 4-6) | ||||||||||||||
| Continue immobilizer except hygiene and exercise | ● | ● | ● | ● | ● | ● | ||||||||
| Supine external rotation | ● | ● | ● | ● | ● | ● | ● | |||||||
| Hands-behind head stretch | ● | ● | ● | |||||||||||
| Standing ER as tolerated | ● | ● | ● | |||||||||||
| Supine forward flexion (140 degrees) | ● | ● | ● | |||||||||||
| Theraband IR (neutral), ER as tolerated | ● | ● | ● | ● | ● | |||||||||
| Standing FF 90 (scaption) | ● | ● | ● | ● | ● | |||||||||
| Prone ROW, Extension | ● | ● | ● | ● | ● | |||||||||
| Biceps curls | ● | ● | ● | ● | ● | |||||||||
| Side-lying ER | ● | ● | ● | ● | ● | |||||||||
| PHASE 3 (weeks 7-12) Continue previous plus | ||||||||||||||
| Wall slide stretch | ● | ● | ● | ● | ● | |||||||||
| Behind Back IR (start week 8) | ● | ● | ● | ● | ||||||||||
| Horizontal adduction stretch (week 8) | ● | ● | ● | |||||||||||
| Theraband, ER, IR | ● | ● | ● | ● | ● | |||||||||
| Standing forward punch | ● | ● | ● | ● | ● | |||||||||
| Shoulder shrug | ● | ● | ● | ● | ● | |||||||||
| Dynamic Hug | ● | ● | ● | ● | ● | |||||||||
| W's, T's, Y's | ● | ● | ● | ● | ● | |||||||||
| Seated row, and prone row | ● | ● | ● | ● | ● | |||||||||
| Prone extension | ● | ● | ● | ● | ● | |||||||||
| Standing forward flexion "full can" | ● | ● | ● | ● | ● | |||||||||
| Rhythmic stabilization and proprioceptive | ● | ● | ● | ● | ● | |||||||||
| PHASE 4 (weeks 12-20) continue previous plus | ||||||||||||||
| Side lying internal rotation (sleeper) | ● | ● | ● | ● | ||||||||||
| Theraband ER, IR at 90 | ● | ● | ● | ● | ||||||||||
| Diagonal up and down | ● | ● | ● | ● | ||||||||||
| Resisted forearm supination/pronation | ● | ● | ● | ● | ||||||||||
| Resisted wrist flexion-extension | ● | ● | ● | ● | ||||||||||
| Machine resistance (see handout) | ● | ● | ● | ● | ||||||||||
| PHASE 5 (weeks 20 onward) | ||||||||||||||
| Continue previous | ● | ● | ||||||||||||
| Initiate plyometrics/interval sports program | ● | ● | ||||||||||||
| May initiate pre injury level activities with clearance by your surgeon | ● | |||||||||||||
| Return to play typically 5-6 months | ||||||||||||||
Additional Instructions:
Reverse Total Shoulder Replacement Surgery
Arthritis of the shoulder
In a normal shoulder, the humeral head ("ball") at the top of the arm bone rotates smoothly inside the glenoid cavity ("socket"). Arthritis of the shoulder develops when the normally smooth, gliding surfaces of the ball and socket are damaged.
The most common form of shoulder arthritis, osteoarthritis, typically develops in patients after a lifetime of wear and tear. Less common forms of arthritis include post-traumatic arthritis (arthritis that occurs after a broken bone or other injury) and inflammatory arthritis (an autoimmune disease that destroys the joint). If the muscles surrounding the shoulder are severely damaged, the altered shoulder motion can wear out the gliding surfaces and lead to another form of arthritis called rotator cuff arthropathy.
In shoulder replacement surgery, the damaged joint is replaced with biocompatible devices that provide a smooth and painless range of motion. Your surgeon will make every effort to restore your shoulder to a condition that resembles its previous healthy status. You should discuss what realistic outcome to expect with your surgeon.
Normal shoulder
On an x-ray of a normal shoulder, a slight space can be seen between the humeral head (ball) and the glenoid cavity (socket). This indicates a smooth, gliding joint surface.
Arthritic shoulder
There is no space between this shoulder's ball and socket, indicating that the normal surfaces are likely destroyed. Also, the large bone spur (arrow) extending from the ball is probably causing additional pain and stiffness.
Total shoulder replacement
In a standard total shoulder replacement, the ball and socket of the joint are replaced by implants. Placement of the components insures that the smooth gliding surfaces are recreated and normal shoulder function
Arthritic shoulder with damaged muscles
In some cases the ball is not even located next to the socket. This x-ray shows that the humeral head (ball) has moved up and away from its normal position. It is highly likely that the muscles surrounding the shoulder joint have been destroyed.
Reverse total shoulder replacement
In this type of total shoulder replacement surgery, the ball is placed where the socket used to be and vice versa. This reverse total shoulder replacement compensates for the loss of shoulder muscles and makes it possible for the arm to be raised.
Risk factors and complications
- There are risks in any type of surgery, not just shoulder replacement surgery. The general risks of shoulder replacement surgery—such as a bad reaction to anesthesia, stroke, or heart attack—are no greater than in most other types of surgery.
- The following are among the possible complications following shoulder replacement surgery. While this list is not complete, it includes some of the more concerning complications that require your attention. The complication rate is higher than a conventional total shoulder 15-50%.
- Dislocation. (5-12%) Any shoulder replacement can dislocate ("pop out") in the first few months after the surgery. Fortunately, this is one complication that you can do much to prevent. Most surgeons recommend wearing a sling to protect the shoulder. Even in the sling, however, the shoulder can dislocate if the arm is brought backwards. Make sure to keep your operated arm either in front of you or at your side. While lying down to sleep or rest, it will help to place a pillow under the elbow of the operated arm to maintain this position.
- Acromial Fracture (unknown true incidence) This is unique to reverse total shoulder and can be managed non-operatively. Typically presents in a patient doing very well postoperative and then has a setback with worsening pain.
- Implant loosening and wear. The typical shoulder replacement has a 90-95% probability of lasting more than 10 years. Over time, however, the implant may wear out enough to require a second replacement. To slow down this wear, avoid all strenuous or repetitive overhead activities. Your surgeon will give you general guidelines of how the shoulder can be used after the surgery. Be sure to ask your surgeon for recommendations about any specific activity.
- Infection. (1%) Although infection in a shoulder replacement is relatively rare, it is a serious complication that requires immediate treatment. In some cases, the implants have to be removed in order to eradicate the infection. Many infections can be avoided. For example, most dental procedures, including routine cleaning, carry the risk of bacteria entering the bloodstream to infect the shoulder implants. Taking an oral antibiotic, prescribed by your dentist, an hour before your procedure can greatly reduce or even eliminate this risk. The same rule applies to other medical procedures, such as colonoscopy.
- Nerve or blood vessel injury. (2.4%) Similar to other surgeries, there is a risk of damage to nerves or blood vessels during shoulder replacement surgery, although this risk is extremely low. If you experience severe numbness or weakness in your hand after the block has worn off, notify your nurse or your surgeon immediately.
Driving
You may give you permission to drive within four weeks after the surgery. If your surgery was on the right side, driving permission may not be given until a month or six weeks following the surgery.
Work Activities
Determining the date you return to work will depend both on your surgeon and the type of work you do. Some individuals may require modifications of their job, while others may easily return to their previous activities. Lifting and pulling job-related activities might be delayed or discouraged. Those engaged in heavy manual labor may have to discuss the possibility of vocational counseling with their surgeon.
Leisure and Sport Activities
There are different risks associated with certain types of leisure and sport activities. Some activities may lead to damage of your artificial joint over time due to wear and tear of the joint. More vigorous the activities will increase the risk of damaging the implant. Increased the wear and tear on the implant will increase the risk of loosening of the implant.
Three major categories of activities should be avoided. These include:
- Activities causing high impact stresses on the implant
- Activities with potentially high risk of injury
- Activities that may result in falling or getting tangled with opponents risking dislocation of the joint itself or a fracture of the bone around the implant.
These types of activities include sport activities requiring a vigorous throwing motion of the arm, chopping wood, hammering, heavy lifting or pushing activities, martial arts, and rough contact sports. These activities should be avoided.
Weight lifting activities may be limited throughout your life. During your post-operative period you may be able to build up to lifting weights weighing less than five pounds. Check with your surgeon and physical therapist about lifting any heavier weights.
Lower stress activities such as hiking, walking, biking, golfing, and swimming are excellent forms of exercise for individuals with a shoulder replacement. Some patients also return to playing tennis with a shoulder replacement.
How long will I be in a sling?
Generally, 6 weeks. You should sleep in the sling as well. The sling should only be removed for hygiene and exercises. If you cannot sleep in bed due to discomfort, consider sleeping in a more upright position, such as a recliner. It is important to not externally rotate (a motion similar to reaching for the seatbelt while in a passenger seat in the car) for the first 6 weeks. A sling will prevent this motion.
How long before I am fully recovered?
By 3 months most patients are feeling about 80% and are back to daily activities. By 6 months, you should be able to return to your recreational activities (within reason) and maximal medical improvement is at one year.
Outcomes
Typically patients get 145 degrees of forward flexion or elevation and 50 degrees of external rotation. ASES scores go from an average of 35 pre-op to 77 post op (max is 100).
Reverse Total Shoulder Arthroplasty Rehab Protocol
Phase 0: 0-6 weeks after surgery
Goals:
- Protect the shoulder replacement
- Ensure wound healing
- Prevent stiffness
Activities
- Sling— Use your sling as needed. You only need it for comfort. Remove for hygiene and exercises.
- Use of the operative arm— Please move your elbow wrist and hand after surgery to prevent stiffness. When moving keep your elbow in front of your body do not reach behind your body for the first 3 weeks.
- Bathing and Showering— You may shower after surgery and wash the incision area. To wash under the arm, bend over at the waist and let the arm swing passively away from the body. It is safe to wash under the arm in this position. Do Not submerge the incision under water. Do not scrub the wound.
- Ice— 7 days a week for 4-5 times a day as needed for 15-20 minutes. Do not place directly on the skin.
Exercise Program
Passive ROM Days per week: 7 Times Per day 4-5
- Pendulum exercises 1-2 sets 20-30 rotations
- Supine External Rotation 1-2 sets 10-15 reps — Weeks 1-6: limit to neutral
- Supine forward elevation 1-2 sets 5-10 reps — Weeks 1 and 2: limit to 90 (straight up); Week 3 and on: as tolerated
- Behind the back internal rotation 1-2 sets 5-10 reps
Shoulder stretching is divided into two phases. Phase 1, or passive range of motion is always performed with the uninjured arm assisting or helping the operative arm. Phase 2, or active range of motion is a stretching is performed by the operative arm without the assistance of the uninjured arm. In most instances, wean off passive range of motion by using the uninjured arm in isolated incidents to assist the operative arm. The other major difference between passive and active stretching is the "terminal stretch." During active stretching and upon reaching your "endpoint" of pain or movement, push the operative arm with the uninjured hand another 5-10 degrees for additional movement. Maximal motion for each person remains the goal and terminal stretching will assist in achieving that goal.
All stretching exercises should be done slowly to maximize muscle and soft connective tissue involvement. When stretching, your goal is to reach the maximum range of motion for you.
Since there are more than one repetition per set, allow the first one or two repetitions to be warmup reps, with very little to no pain. Gradually work into more and more range of motion. It is also important to allow pain to be your guide. Move the arm to an "endpoint" (dictated by pain). Your goal is to increase the endpoint as often as possible until you have reached the full range of motion. As far as pain, you want to avoid excruciating pain, but "discomfort" is tolerated as long as the pain does not remain for a prolonged period of time. A basic rule, if the pain does not linger, you didn't stretch too far.
Phase 1: 6-8 weeks after surgery
Goals:
- Protect the shoulder and avoid over stressing the replacement
- Improve range of motion of the shoulder
- Begin Strengthening exercises
Activities
- Sling— None.
- Use of the operative arm— Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight.
- Precautions— Do not lift heavy weights overhead with the weight going behind the head. Keep everything where you can see it.
- Ice— 7 days a week for 4-5 times a day as needed for 15-20 minutes. Do not place directly on the skin.
Exercise Program
Stretching/Active motion Days per week 7 Times per day 2-4
- Pendulum exercises 1-2 sets 20-30 rotations
- Supine External rotation 1 set 10-15 reps
- Standing External rotation 1 set 10-15 reps — Week 6: limit to 30 degrees; Week 7-8: limit 45 degrees
- Supine passive arm elevation 1 set 5-10 reps
- Standing Arm elevation 1 set 5-10 reps
- Behind the back internal rotation 1-2 sets 5-10 reps
Phase 2: 8-12 weeks after surgery
Goals:
- Protect the shoulder
- Regain full range of motion
- Continue gentle Strengthening
Activities
- Sling— No longer necessary.
- Use of the operative arm— You may now use your arm. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight.
- Precautions— Do not lift heavy weights overhead with the weight going behind the head. Keep everything where you can see it.
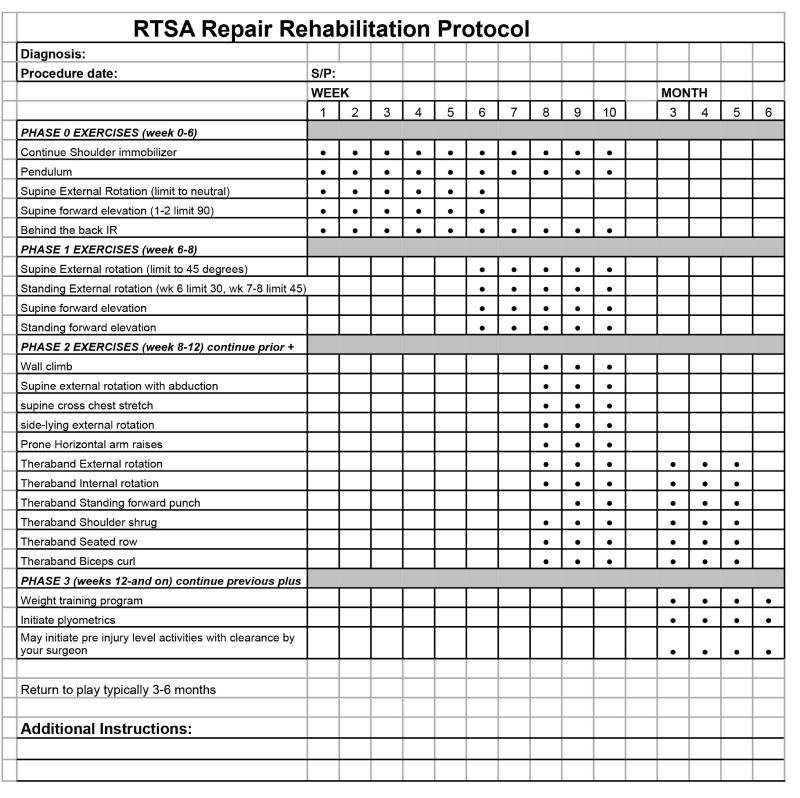

Shoulder - Torn Rotator Cuff
Anatomy and Function
The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The capsule is a broad ligament that surrounds and stabilizes the joint. The shoulder joint is moved and also stabilized by the rotator cuff. The rotator cuff is comprised of four muscles and their tendons that attach from the scapula to the humerus. The rotator cuff tendons (supraspinatus, infraspinatus, teres minor and subscapularis) are just outside the shoulder joint and its capsule. The muscles of the rotator cuff help stabilize the shoulder and allow you to lift your arm, reach overhead, and take part in activities such as throwing, swimming and tennis.
Rotator Cuff Injury and Treatment Options
The rotator cuff can tear as an acute injury such as when lifting a heavy weight or falling on the shoulder or elbow. The shoulder is immediately weak and there is pain when trying to lift the arm. A torn rotator cuff due to an injury is usually best treated by immediate surgical repair. The rotator cuff can also wear out as a result of degenerative changes. This type of rotator cuff tear can usually be repaired but sometimes the tear may not need to be repaired and sometimes cannot be repaired. However, if the tear is causing significant pain and disability, surgery may be the best treatment to relieve pain and improve shoulder function. If a torn rotator cuff is not repaired, the shoulder often develops degenerative changes and arthritis many years later. This type of arthritis is very difficult to treat in young patients and the longstanding tear in the rotator cuff may be irreparable.
Diagnosis of Torn Rotator Cuff
Symptoms of shoulder pain that awaken you at night, and weakness raising the arm are suggestive of a torn rotator cuff. Examination of the shoulder usually reveals weakness. The diagnosis can be confirmed by magnetic resonance imaging (MRI). A more sensitive test such as arthrogram MRI or arthroscopy may be needed to diagnose a small tear or a partial tear of the rotator cuff.
Rotator Cuff Repair
Most rotator cuff tears can be repaired surgically by reattaching the torn tendon(s) to the humerus. It is not a big operation to repair a torn rotator cuff, but the rehabilitation time can be long depending on the size of the tear and the quality of the tendons/muscles. The surgery is outpatient surgery, done through small poke holes. Anchors are placed into the humerus bone and the torn tendon/s are reattached to the bone with sutures. The tendons heal back to the bone, reestablishing the normal tendon-to-bone connection. It takes several months for the tendon to heal back to the bone. During this time, forceful use of the shoulder such as weight lifting and raising the arm out to the side or overhead must be avoided.
After surgery, you will probably use a sling for 4 to 6 weeks. You can remove the sling 4 to 5 times a day for gentle pendulum motion exercises. Typically a large pillow holds your arm out to the side of your body is needed for 4-6 weeks.
Results of Surgery and Risks
The success of surgery to repair the rotator cuff depends upon the size of the tear and how long ago the tear occurred.. Usually, a small tear has a good chance for full recovery. If the tear is large, the extent of recovery cannot be accurately predicted until the repair and rehabilitation is completed. If the tear occurred a long time ago (several months or longer) it can be difficult or sometimes impossible to repair. Most patients achieve good pain relief following repair regardless of the size of the tear unless the tear is massive.
Shoulder pain is usually worse than before surgery for the first 2-3 weeks, but then gradually the pain lessens. This is especially true while trying to sleep at night. It is recommended sleeping in a reclining chair during this time to help lessen the night pain. It can take up to a full year to regain motion and function in the shoulder. Shoulder stiffness and loss of motion are potential problems after rotator cuff repair. Re-rupture of the repaired rotator cuff is possible if too much force is placed on the repaired tendon before it is fully healed. Nerve and muscle injury and infection are infrequent complications.
Complications
- Persistant pain
- Stiffness 10%
- wound infection 0.16 to 1.9%
- bleeding <0.5%
- nerve injury <0.5%
Shoulder - Rotator Cuff Repair Postoperative Instructions
Phase zero: the first week after surgery
Goals:
- Control pain and swelling
- Protect the rotator cuff repair
- Protect wound healing
- Begin early shoulder motion
Activities:
Immediately After Surgery
- After surgery you will be taken to the recovery room room, where your family can meet you. You will have a sling on your operated arm with an abduction pillow.
- You should get out of bed and move around as much as you can.
- When lying in bed, elevate the head of your bed and put a small pillow under your arm to hold it away from your body.
- Apply cold packs to the operated shoulder to reduce pain and swelling.
- Move your fingers, hand and elbow to increase circulation.
- The novocaine in your shoulder wears off in about 6 hours. Use your pain medication as needed.
- You will receive a prescription for pain medication for when you go home (it will make you constipated if you take it for a long time).
The Next Day After Surgery
- You can remove the bandages but leave the small pieces of tape (steristrips) in place.
- You may shower and get the incision wet. To wash under the operated arm, bend over at the waist and let the arm passively come away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
- Apply cold to the shoulder for 20 minutes at a time as needed to reduce pain and swelling.
- Remove the sling several times a day: move the elbow wrist and hand. Lean over and do pendulum exercises for 3 to 5 minutes every 1 to 2 hours.
- DO NOT lift your arm at the shoulder using your muscles.
- Because of the need for your comfort and the protection of the repaired tendon, a sling is usually necessary for 4 to 6 weeks, unless otherwise instructed by your surgeon.
Office Visit:
Please arrange to return to your surgeon's office 7-10 days after surgery
Rehabilitation after Rotator Cuff Repair
Phase One: 0 to 6 weeks after surgery
Goals:
- Protect the rotator cuff repair (At 4 weeks post op the strength of the tendon repair is about 20% of a "normal" tendon attachment. Hence, prior to 6 weeks post op no active motion of the arm is permitted, as it may pull on the repair and disrupt the attachment of the tendon to the bone.)
- Ensure wound healing
- Prevent shoulder stiffness
- Regain range of motion
Activities:
1. Sling
Use your sling most of the time. Remove the sling 4 or 5 times a day to do pendulum exercises.
2. Use of the affected arm
You may use your hand on the affected arm in front of your body but DO NOT raise your arm or elbow away from your body. It is all right for you to flex your arm at the elbow. Also:
- No Lifting of Objects
- No Excessive Shoulder Extension
- No Excessive Stretching or Sudden Movements
- No Supporting of Body Weight by Hands
3. Showering
You may shower or bath and wash the incision area. To wash under the affected arm, bend over at the waist and let the arm passively come away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
Exercise Program
Days per week: 7 Times per day
Program:
- Pendulum exercises
- Supine Passive External rotation
- Supine passive arm elevation
- Passive scapular retraction
- Shoulder shrug
- Ball Squeeze exercises
Phase two: 6 to 12 weeks after surgery
Goals:
- Protect the rotator cuff repair
- Improve range of motion of the shoulder
- Continue strengthening
Activities
1. Sling
Your sling is no longer necessary unless your doctor instructs you to continue using it.
2. Use of the operated arm
You should continue to avoid lifting your arm away from your body, since this is the action of the tendon that was repaired. You can lift your arm forward in front of your body but not to the side. You may raise your arm to the side, if you use the good arm to assist the operated arm.
3. Bathing and showering
Continue to follow the instructions from phase one and the instructions above.
Exercise Program
The exercises listed below may be gradually integrated into the rehabilitation program under the supervision of your doctor and/or physical therapist.
Days per week: 5-7 Times per day: 1-3
Stretches
- Pendulum exercises
- Supine External rotation
- Standing External Rotation
- Supine passive elevation
- Active-Assisted elevation
- Behind the back internal rotation
- External rotation @90 degrees abduction
- Supine cross-chest stretch
- Wall slide stretch
Active Motion
- Side-lying External rotation
- Prone Horizontal arm raises "T"
- Prone Scaption "Y"
- Prone row
- Prone extension
- Prone extension
- Standing forward flexion with scapulohumeral rhythm
- Resisted forearm supination-pronation
- Resisted wrist flexion-extension
- Isometric: internal and external rotation at neutral
Phase Three: 12-18 weeks after surgery
- Protect the rotator cuff repair
- Regain full range of motion
- Continue gentle strengthening
Activities:
Use of the operated arm
You may now safely use the arm for normal daily activities involved with dressing, bathing and self-care. You may raise the arm away from the body; however, you should not raise the arm when carrying objects greater than one pound. Any forceful pushing or pulling activities could disrupt the healing of your surgical repair.
Exercise Program
The exercises below form a list that may be gradually integrated into the rehabilitation program under the supervision of your doctor and/or physical therapist. Resistance for the dynamic strengthening exercises can gradually be added starting with 1 lb and should not exceed 3 lb at this time.
Days per week: 3 Times per day: 1
Stretching / Active Motion / Strengthening
Stretching
- As above as needed
Theraband
- External Rotation
- Internal rotation
- Standing forward punch
- Shoulder shrug
- Dynamic hug
- "W's"
- Seated Rows
- Biceps curls
Dynamic strengthening
- Side-lying External Rotation
- Prone Horizontal Arm Raises "T"
- Prone Scaption "Y"
- Prone Row
- Prone Extension
- Scapulohumeral proprioception and rhythm exercises
Phase 4: 18 to 26 weeks after surgery
Goals:
- Continue to protect the repair by avoiding excessive forceful use of the arm or lifting excessively heavy weights.
- Restore full shoulder motion
- Restore full shoulder strength
- Gradually begin to return to normal activity
Activities:
- Sports that involve throwing and the use of the arm in the overhead position are the most demanding on the rotator cuff..
- For people who wish to return to training with weights, your surgeon or your therapist will give you guidelines regarding the timing and advice when returning to a weight-training program.
- The following timetable can be considered as a minimum for return to most activities:
- Ski — 6 Months
- Golf — 6 Months
- Weight Training — 6 Months
- Tennis — 6-8 months
- Swimming — 6-8 months
- Throwing — 6-8 months
Before returning safely to your activity, you must have full range of motion, full strength and no swelling or pain.
Your surgeon or your physical therapist will provide you with a specific interval-training program to follow when it is time to return the above activities.
Rotator Cuff Repair Rehabilitation Protocol
Diagnosis:
Procedure date: S/P:
| Exercise | Week | Month | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 3 | 4 | 5 | 6 | |
| PHASE 0 EXERCISES (week 0-6) | ||||||||||||||
| Continue Shoulder immobilizer | ● | ● | ● | ● | ● | ● | ||||||||
| Pendulum | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ||||
| Supine passive ER, forward elevation limit 120 shoulder shrug, scapular retraction | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ||||
| Ball Squeeze | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● | ● |
| PHASE 2 EXERCISES (week 6-12) | ||||||||||||||
| Continue stretches from prior | ● | ● | ● | ● | ● | ● | ● | ● | ||||||
| Active-assisted elevation | ● | ● | ● | ● | ● | |||||||||
| Behind Back IR | ● | ● | ● | ● | ● | |||||||||
| Supine external with abduction | ● | ● | ● | ● | ● | |||||||||
| supine cross chest stretch | ● | ● | ● | ● | ● | |||||||||
| Side-lying ER | ● | ● | ● | ● | ● | |||||||||
| Prone (T, Y, row, extension) | ● | ● | ● | ● | ● | |||||||||
| forearm supination-pronation, and wrist (F/E) | ● | ● | ● | ● | ● | |||||||||
| Isometric (IR and ER) | ● | ● | ● | ● | ● | |||||||||
| PHASE 3 (weeks 12-18) Continue previous plus | ||||||||||||||
| Theraband, ER, IR, fwd punch, shrug, dynamic hug, Ws | ● | ● | ● | |||||||||||
| seated row | ● | ● | ● | |||||||||||
| biceps curl | ● | ● | ● | |||||||||||
| Side lying ER | ● | ● | ● | |||||||||||
| Prone (T, Y, Row, Extension) | ● | ● | ● | |||||||||||
| Rhythmic stabilization and proprioceptive | ● | ● | ● | |||||||||||
| PHASE 4 (weeks 18-20) continue previous plus | ||||||||||||||
| Side lying internal rotation (sleeper) | ● | |||||||||||||
| Weight training program | ||||||||||||||
| Initiate plyometrics/interval sports program | ● | ● | ||||||||||||
| May initiate pre injury level activities with clearance by your surgeon | ● | |||||||||||||
| Return to play typically 5-6 months | ||||||||||||||
Additional Instructions:
Arthroscopic Labrum Repair of the Shoulder (SLAP)
Anatomy
The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral head rests in a shallow socket on the scapula called the glenoid. Because the head of the humerus much larger than the glenoid, a soft fibrous tissue labrum called the labrum surrounds the glenoid to help deepen and stabilize the joint. The labrum deepens the glenoid by up to 50 percent so that the head of the humerus fits better. In addition, it serves as an attachment site for several ligaments.
Injuries
Injuries to the labrum can occur from acute trauma or repetitive shoulder motion. Examples of traumatic injury include:
- Falling on an outstretched arm
- Direct blow to the shoulder
- Sudden pull, such as when trying to lift a heavy object
- Forceful overhead motions
Tears can be located either above (superior) or below (inferior) the middle of the glenoid. A SLAP lesion (superior labrum, anterior [front] to posterior [back]) is a tear of the labrum above the middle of the glenoid that may also involve the biceps tendon. A tear of the labrum below the middle of the glenoid socket that also involves the inferior glenohumeral ligament is called a Bankart lesion. Tears of the glenoid labrum often occur with other shoulder injuries, such as a dislocated shoulder (full or partial dislocation).
Signs and symptoms
It is difficult to diagnose a tear in the glenoid labrum because the symptoms are very similar to other shoulder injuries. Symptoms include:
- Pain, usually with overhead activities
- Catching, locking, popping or grinding
- Occasional night pain or pain with daily activities
- A sense of instability in the shoulder
- Decreased range of motion
- Loss of strength
Treatment
Until the final diagnosis is made, your surgeon may prescribe anti-inflammatory medication and rest to relieve symptoms. Rehabilitation exercises to strengthen the rotator cuff muscles may also be recommended. If these conservative measures are insufficient, your surgeon may recommend arthroscopic surgery.
During the surgery, your surgeon will examine the labrum and the biceps tendon. If the injury is confined to the labrum itself, without involving the tendon, the biceps tendon attachment is still stable. Your surgeon will remove the torn flap and correct any other associated problems. If the tear extends into the biceps tendon or if the tendon is detached, the result is an unstable biceps attachment. Your surgeon will need to repair and reattach the tendon, using suture anchoring devices. If there is a tear below the middle of the glenoid, your surgeon will reattach the ligament to the glenoid (Bankart repair).
Rehabilitation
After surgery, you will need to keep your shoulder in a sling for three to four weeks. Your surgeon will also prescribe gentle, passive range-of-motion exercises. When the sling is removed, you will need to do motion and flexibility exercises and eventually start strengthening. Athletes can usually begin doing sports-specific exercises after twelve weeks, although it will be about six months before the shoulder is fully healed.
Rehabilitation after Arthroscopic Labrum Repair of the Shoulder (SLAP)
Phase 0: 0 to 2 weeks after surgery
POSTOPERATIVE INSTRUCTIONS
You will wake up in the operating room. A sling and an ice pack will e in place. You will go to the recovery room and generally will be discharged after 1-2 hours. You can get out of bed when you wish. Apply ice to the shoulder to reduce pain and swelling. You may remove the sling whenever you wish and gently move the elbow, wrist and fingers. Follow your surgeon's instructions regarding moving your shoulder after surgery.
GOALS:
- Control pain and swelling
- Protect the repair
- Begin early shoulder motion
ACTIVITIES WHEN YOU GO HOME:
- Apply ice to the shoulder as tolerated to reduce pain and swelling.
- Remove the sling on the first day after surgery. Move your elbow, fingers and hand several times a day.
- Begin the pendulum exercise several times a day: Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently in small circular motions. Repeat for 2 to 3 minutes at a time.
- Remove the outer dressing on the second day after surgery and shower. Leave the little pieces of tape (steri-strips) in place. You can get the wound wet after 2 days in a shower, but do not soak in a tub. To wash under the operated arm, bend over at the waist and let the arm passively swing away from the body. It is safe to wash under the arm in this position.
- Keep your elbow slightly in front of your body; do not reach behind your body. When putting on clothing, lean forward and pull the shirt up and over the operated arm first. Then put the other arm into the opposite sleeve. To remove the shirt, take the unoperated arm out of the sleeve first, and then slip the shirt off of the operated arm.
- Call your surgeon's office for any concerns, including, but not limited to, severe pain, fevers, chills or redness. If it is an emergency go to your local emergency room and have them contact your surgeon.
OFFICE VISIT:
Please arrange to return to your surgeon's office 10 days after surgery for examination and further instructions.
Phase One: 0 to 4 weeks after surgery
Goals:
- Protect the surgical repair
- Ensure wound healing
- Prevent shoulder stiffness
- Regain range of motion
- Control pain and swelling
Activities:
- Sling Use your sling most of the time for the first 2 weeks. Your surgeon will give you additional instructions on the use of the sling at your post-operative office visit. Remove the sling 4 or 5 times a day to do pendulum exercises.
- Use of the operated arm You may use your hand on the operated arm in front of your body but DO NOT raise your arm overhead. Avoid extending the arm behind you and avoid putting your arm in a position as if your hands were behind your head. It is all right for you to flex your arm at the elbow but do not lift any objects in excess of 2 pounds or engage in activities that involve forceful use of the forearm such as using a screwdriver. Use of a computer or writing is all right as long as it is not painful.
- Showering You may shower or bath and wash the incision area. To wash under the operated arm, bend over at the waist and let the arm passively come away from the body. It is safe to wash under the arm in this position. This is the same position as the pendulum exercise.
ICE
Ice the arm 15-20 minutes duration 4-5 times per day as needed to decrease swelling and pain.
STRETCHING / PASSIVE MOTION
Days per Week: 7 Times per day: 4-5
Exercise Program:
- Pendulum exercises
- Supine External Rotation
- Supine assisted arm elevation
- Ball squeeze exercise
- Scapular retraction
- Behind the back internal rotation
- Isometric exercises: internal and external rotation at neutral
- Rhythmic stabilization and proprioceptive training drills with physical therapist
Phase two: the 5 to 7 weeks after surgery
Goals:
- Protect the surgical repair
- Improve range of motion of the shoulder
- Begin gentle strengthening
Activities
- Sling Your sling is no longer necessary unless your surgeon instructs you to continue using it (use it for comfort only).
- Use of the operated arm You can now move your arm for most daily activities, but you need to continue to be careful not to lift objects heavier than 1 or 2 pounds. You should avoid forceful pushing or pulling activities. You should avoid activities that load the biceps muscle, such as turning a screwdriver or carrying a heavy box. You should continue to avoid reaching behind you or other positions with the hand behind the head.
STRETCHING / ACTIVE MOTION
Days per week: 7 Times per day: 1 to 3
- Pendulum exercises
- Supine External Rotation
- Standing External Rotation
- Supine passive arm elevation
- Seated-Standing Arm Elevation
- Behind the back internal rotation
STRENGTHENING EXERCISES
Days per week: 7 Times per day: 1
- Theraband internal and external rotation
- Standing forward flexion (scaption)
- Prone row
- Prone horizontal abduction ‘T’s
- Prone extension
- Sidelying external rotation
Phase Three: starting 8 to 12 weeks after surgery
Goals:
- Protect the surgical repair
- Regain full range of motion
- Continue strengthening progression
Activities:
Use of the operated arm You may now safely use the arm for normal daily activities involved with dressing, bathing and self-care. You may raise the arm away from the body; however, you should not raise the arm when carrying objects greater than one pound. Any forceful pushing or pulling activities could still disrupt the healing of your surgical repair.
Exercise Program:
STRETCHING / RANGE OF MOTION Days per week: 7 Times per day: 1-2
- Pendulum exercises
- Standing External Rotation/Doorway
- Wall slide Stretch
- Hands-behind-head stretch (start week 9 post operative)
- Standing Forward Flexion
- Behind the back internal rotation
- Supine Cross-Chest Stretch
- Sidelying internal rotation (sleeper stretch)
STRENGTHENING / THERABAND Days per week: 7 Times per day: 1
- External Rotation
- Internal Rotation
- Standing Forward Punch
- Shoulder Shrug
- Dynamic hug
- “W”’s
- Biceps curl (start week 9 post operative)
- Seated Row (Start the 11th week after surgery )
STRENGTHENING / DYNAMIC Days per week: 7 Times per day: 1
- Side-lying External Rotation
- Prone Horizontal Arm Raises ’T’s
- Prone row
- Prone scaption ‘Y’s
- Prone extension
- Standing forward flexion “full-can” scaption (Add resistance 1 to 3 lb)
- Rhythmic stabilization and proprioceptive training drills with physical therapist
Phase Four: 12 to 16 weeks after surgery
Goals:
- Gradual initiation of functional activities
- Maintain full range of motion
- Continue progressive strengthening
Exercise Program
STRETCHING / RANGE OF MOTION Times per day: 1 Days per week: 5-7
- Pendulum exercises
- Standing External Rotation / Doorway Wall slide Stretch
- Hands-behind-head stretch
- Behind the back internal rotation
- Supine Cross-Chest Stretch
- Sidelying internal rotation (sleeper stretch)
- External rotation at 90° Abduction stretch
STRENGTHENING / THERABAND Times per day: 1 Days per week: 3
Continue exercises from phase 3
- Optional exercises for overhead sports:
- External rotation at 90°
- Internal rotation at 90°
- Standing ’T’s
- Diagonal up, diagonal down
STRENGTHENING / DYNAMIC Times per day: 1 Days per week: 3
- Continue exercises from phase 3
- Prone external rotation at 90° abduction
- “U’s
- Biceps curls
- Resisted forearm supination-pronation
- Resisted wrist flexion-extension
- PNF manual resistance with physical therapist Push-ups
PLYOMETRIC PROGRAM
- Times per day and days per week: per physical therapist
- ‘Rebounder’ throws with arm at side
- Wall dribbles overhead
WEIGHT TRAINING
See weight training precautions section
Guidelines and Precautions for Returning to Weight Training After Arthroscopic Labrum Repair
You should not return to training using heavy weights or on weight machines until your surgeon determines that it is safe.In general, it is usually safe to return to heavier weight training at 3-4 months following labrum repair.
Before embarking on a weight-training program, you should have full range of shoulder motion and normal strength in the rotator cuff and scapular muscles. Your surgeon or your physical therapist will test your motion and strength before you start weight training.
When starting your weight-training program, you can start with 3 sets of 15-20 repetitions. Training with high repetition sets ensures that the weights that you are using are not too heavy.
NEVER perform any weight training exercise to the point of muscle failure. “Muscle failure” occurs when, in performing a weight training exercise, the muscle is no longer able to provide the energy necessary to contract and move the joint(s) involved in the particular exercise. Joint, muscle and tendon injuries are more likely to occur when muscle failure occurs.
The following weight training exercises should be avoided after Bankart repair for shoulder instability and superior labrum repairs:
- Pull downs behind-the-neck (wide-grip)
- Behind-the-neck shoulder press
- Wide-grip bench press
- Standing lateral deltoid raises
- Triceps press overhead
The following exercises require special cautions:
- Pull downs should only be done in front of the head, to the chest, with a medium (not wide) grip.
- Shoulder press overhead should be done carefully, avoiding heavy weights. If doing shoulder presses, always start with the hand in front of the shoulder and end overhead where you can still see your hand. For persons using barbells, this is the “military press”.
- If bench pressing, your grip should be no wider than the width of your shoulders. Avoid any exercises using grips wider or narrower than shoulder width.
- Lateral deltoid raises should be avoided because of the impinging and wearing effect on the rotator cuff. Forward raises in the “thumb-up” position are usually safer and can be done with reasonable weights. Lateral raises from the prone or bent over position can be done as a substitute for standing lateral deltoid raises.
- When doing incline bench press with barbells, there is a danger of shoulder dislocation if the lifter loses control of the bar when returning the barbell to the rack of the incline bench. Always have a spotter for removing and replacing the barbell in this exercise.
- If you are doing any type of “chest-fly”, keep in mind the following precautions: Do not do any chest-fly exercise with straight elbows. Always allow the elbows to bend and never lower your hands (holding dumbbells) below the level of your chest.
- If you are using a “Pec-Deck” machine, never let the weight stretch the arms so that your elbows pass behind your chin. You can set the arms on this machine a few clicks forward to adjust the maximum motion allowed.
- If you a performing “dips” using a set of parallel bars, never lower yourself below the point where the elbows reach a 90-degree angle.
- For triceps exercises, triceps pushdowns on a pulley system are safe as well as bent-over triceps extensions.
- When doing the upright-rowing exercise, keep your grip at least 12 inches apart. When pulling the bar upward toward the chin, do not raise the bar higher than the point at which the elbow reaches shoulder level.
Exercises Usually Problem-Free
- Biceps Curls
- Cable and bent-over rowing
- Shoulder shrugs
If your goal is returning to high-level weight training or weight lifting, it will take 3 to 6 months of cautious, gradual progression to return to top form. In general, avoid increasing the amount of weight lifted by more than 10-15% (at a time) of your present working weight every 10-14 days.
Remember: Weight training is beneficial to improve muscular strength and protect the joints from injury. If done improperly by using too much weight and/or improper technique, weight training can cause serious injury.
Phase Five: 16 to 20 weeks after surgery
Goals:
- Progression of functional activities
- Maintain full range of motion
- Continue progressive strengthening
Exercise Program
STRETCHING / RANGE OF MOTION Days per week: 5-7 Times per day: 1 Continue all exercises from phase 4
STRENGTHENING / THERABAND Days per week: 3 Times per day: 1 Continue from phase 4
STRENGTHENING / DYNAMIC Days per week: 3 Times per day: 1 Continue from phase 4
PLYOMETRIC PROGRAM Days per week and times per day per physical therapist
- ‘Rebounder’ throws with arm at side Wall dribbles overhead
- Rebounder throwing/weighted ball Deceleration drills with weighted ball
- Wall dribbles at 90°
- Wall dribble circles
WEIGHT TRAINING See weight training precautions section
INTERVAL SPORT PROGRAMS See individual programs for golf, tennis, swimming and throwing.
SLAP Repair Rehabilitation Protocol
Procedure date: S/P:
WEEK MONTH 1 2 3 4 5 6 7 8 9 10 3 4 5 6
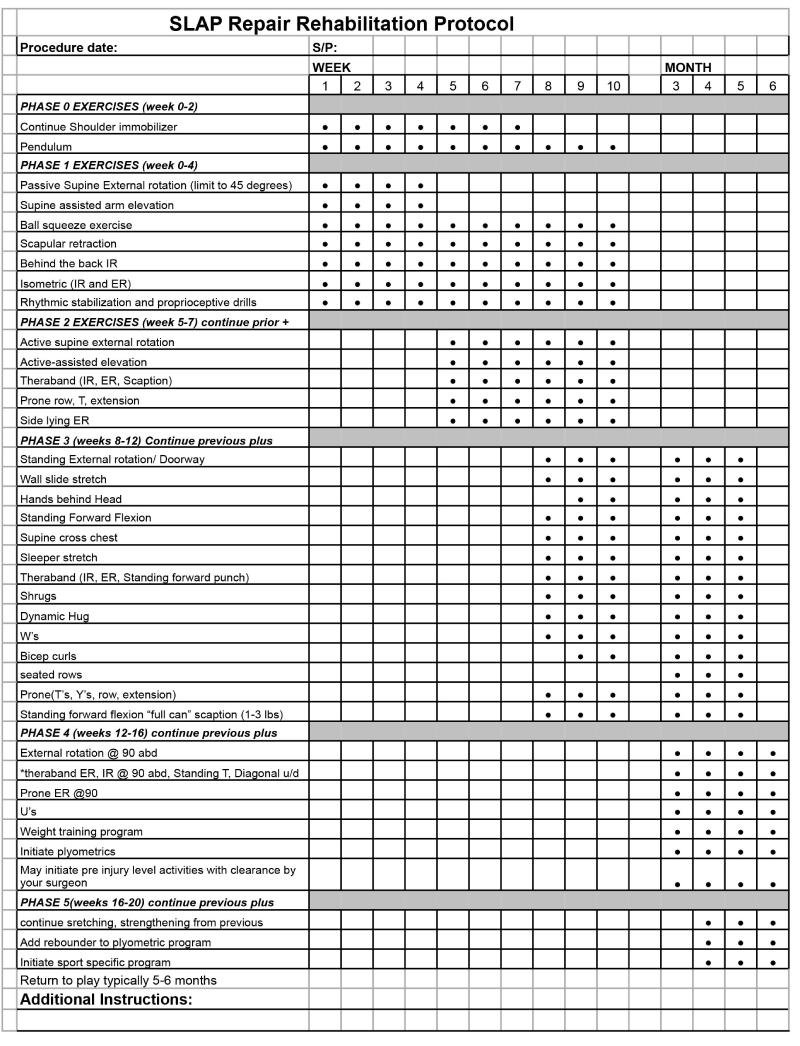
Total Shoulder Replacement Surgery
Arthritis of the shoulder
In a normal shoulder, the humeral head (“ball”) at the top of the arm bone rotates smoothly inside the glenoid cavity (“socket”). Arthritis of the shoulder develops when the normally smooth, gliding surfaces of the ball and socket are damaged.
The most common form of shoulder arthritis, osteoarthritis, typically develops in patients after a lifetime of wear and tear. Less common forms of arthritis include posttraumatic arthritis (arthritis that occurs after a broken bone or other injury) and inflammatory arthritis (an autoimmune disease that destroys the joint). If the muscles surrounding the shoulder are severely damaged, the altered shoulder motion can wear out the gliding surfaces and lead to another form of arthritis called rotator cuff arthropathy.
In shoulder replacement surgery, the damaged joint is replaced with biocompatible devices that provide a smooth and painless range of motion. Your surgeon will make every effort to restore your shoulder to a condition that resembles its previous healthy status. You should discuss what realistic outcome to expect with your surgeon.
Normal shoulder
On an x-ray of a normal shoulder, a slight space can be seen between the humeral head (ball) and the glenoid cavity (socket). This indicates a smooth, gliding joint surface.
Arthritic shoulder
There is no space between this shoulder’s ball and socket, indicating that the normal surfaces are likely destroyed. Also, the large bone spur (arrow) extending from the ball is probably causing additional pain and stiffness.
Total shoulder replacement
In a standard total shoulder replacement, the ball and socket of the joint are replaced by implants. Placement of the components insures that the smooth gliding surfaces are recreated and normal shoulder function restored.
Arthritic shoulder with damaged muscles
In some cases the ball is not even located next to the socket.This x-ray shows that the humeral head (ball) has moved up and away from its normal position. It is highly likely that the muscles surrounding the shoulder joint have been destroyed.
Reverse total shoulder replacement
In this type of total shoulder replacement surgery, the ball is placed where the socket used to be and vice versa.This reverse total shoulder replacement compensates for the loss of shoulder muscles and makes it possible for the arm to be raised.
Risk factors and complications
- There are risks in any type of surgery, not just shoulder replacement surgery. The general risks of shoulder replacement surgery—such as a bad reaction to anesthesia, stroke, or heart attack—are no greater than in most other types of surgery.
- The following are among the possible complications following shoulder replacement surgery. While this list is not complete, it includes some of the more concerning complications that require your attention.
- Dislocation. (4.9%) Any shoulder replacement can dislocate (“pop out”) in the first few months after the surgery. Fortunately, this is one complication that you can do much to prevent. Most surgeons recommend wearing a sling to protect the shoulder. Even in the sling, however, the shoulder can dislocate if the arm is brought backwards. Make sure to keep your operated arm either in front of you or at your side. While lying down to sleep or rest, it will help to place a pillow under the elbow of the operated arm to maintain this position.
- Implant loosening and wear. (5.3%) The typical shoulder replacement has a 90-95% probability of lasting more than 10 years. Over time, however, the implant may wear out enough to require a second replacement. To slow down this wear, avoid all strenuous or repetitive overhead activities.Your surgeon will give you general guidelines of how the shoulder can be used after the surgery. Be sure to ask your surgeon for recommendations about any specific activity.
- Infection. (0.7%) Although infection in a shoulder replacement is relatively rare, it is a serious complication that requires immediate treatment. In some cases, the implants have to be removed in order to eradicate the infection. Many infections can be avoided. For example, most dental procedures, including routine cleaning, carry the risk of bacteria entering the bloodstream to infect the shoulder implants. Taking an oral antibiotic,prescribed by your dentist, an hour before your procedure can greatly reduce or even eliminate this risk.The same rule applies to other medical procedures, such as colonoscopy.
- Nerve or blood vessel injury. (0.8%) Similar to other surgeries, there is a risk of damage to nerves or blood vessels during shoulder replacement surgery, although this risk is extremely low. If you experience severe numbness or weakness in your hand after the block has worn off, notify your nurse or your surgeon immediately.
- Rotator cuff failure (1.3%) Over time the rotator cuff can degenerate and tear.
- Periprosthetic fracture (1.8%)
Driving
You may give you permission to drive within four weeks after the surgery. If your surgery was on the right side, driving permission may not be given until a month or six weeks following the surgery.
Work Activities
Determining the date you return to work will depend both on your surgeon and the type of work you do. Some individuals may require modifications of their job, while others may easily return to their previous activities. Lifting and pulling job-related activities might be delayed or discouraged. Those engaged in heavy manual labor may have to discuss the possibility of vocational counseling with their surgeon.
Leisure and Sport Activities
There are different risks associated with certain types of leisure and sport activities. Some activities may lead to damage of your artificial joint over time due to wear and tear of the joint. More vigorous the activities will increase the risk of damaging the implant. Increased the wear and tear on the implant will increase the risk of loosening of the implant.
Three major categories of activities should be avoided. These include:
- Activities causing high impact stresses on the implant
- Activities with potentially high risk of injury
- Activities that may result in falling or getting tangled with opponents risking dislocation of the joint itself or a fracture of the bone around the implant.
These types of activities include sport activities requiring a vigorous throwing motion of the arm, chopping wood, hammering, heavy lifting or pushing activities, martial arts, and rough contact sports (such as, football, soccer, lacrosse, basketball, baseball, handball, and volleyball). These activities should be avoided.
Weight lifting activities may be limited throughout your life. During your post-operative period you may be able to build up to lifting weights weighing less than five pounds. Check with your surgeon and physical therapist about lifting any heavier weights.
Lower stress activities such as hiking, walking, biking, golfing, and swimming are excellent forms of exercise for individuals with a shoulder replacement. Some patients also return to playing tennis with a shoulder replacement.
How long will I be in a sling?
Generally, 6 weeks. You should sleep in the sling as well. The sling should only be removed for hygiene and exercises. If you cannot sleep in bed due to discomfort, consider sleeping in a more upright position, such as a recliner. It is important to not externally rotate (a motion similar to reaching for the seatbelt while in a passenger seat in the car) for the first 6 weeks. A sling will prevent this motion.
How long before I am fully recovered?
By 3 months most patients are feeling about 80% and are back to daily activities. By 6 months, you should be able to return to your recreational activities (within reason) and maximal medical improvement is at one year.
Total Shoulder Arthroplasty Rehab Protocol
Phase 0: 0-6 weeks after surgery
Goals:
- Protect the shoulder replacement
- Ensure wound healing
- Prevent stiffness
Activities
- Sling— Use your sling for the first 6 weeks. Remove for hygiene and exercises. Keep on for sleeping for the first 3-4 weeks.
- Use of the operative arm— Please move your elbow wrist and hand after surgery to prevent stiffness. Do not rotate the arm at the shoulder. When moving keep your elbow in front of your body do not reach behind your body.
- Bathing and Showering— You may shower after surgery and wash the incision area. To wash under the arm, bend over at the waist and let the arm swing passively away from the body. It is safe to wash under the arm in this position. Do Not submerge the incision under water. Do not scrub the wound.
- Ice— 7 days a week for 4-5 times a day as needed for 15-20 minutes. Do not place directly on the skin.
Exercise Program
Passive ROM Days per week: 7 Times Per day 4-5
- Pendulum exercises 1-2 sets 20-30 rotations
- Supine External Rotation 1-2 sets 10-15 reps Weeks 1-6: limit to neutral
- Supine forward elevation 1-2 sets 5-10 reps Weeks 1 and 2: limit to 90 (straight up) Week 3 and on: as tolerated
- Behind the back internal rotation 1-2 sets 5-10 reps
Shoulder stretching is divided into two phases. Phase 1, or passive range of motion is always performed with the uninjured arm assisting or helping the operative arm. Phase 2, or active range of motion is a stretching is performed by the operative arm without the assistance of the uninjured arm. In most instances, wean off passive range of motion by using the uninjured arm in isolated incidents to assist the operative arm. The other major difference between passive and active stretching is the “terminal stretch.” During active stretching and upon reaching your “endpoint” of pain or movement, push the operative arm with the uninjured hand another 5-10 degrees for additional movement. Maximal motion for each person remains the goal and terminal stretching will assist in achieving that goal.
All stretching exercises should be done slowly to maximize muscle and soft connective tissue involvement. When stretching, your goal is to reach the maximum range of motion for you.
Since there are more than one repetition per set, allow the first one or two repetitions to be warm-up reps, with very little to no pain. Gradually work into more and more range of motion. It is also important to allow pain to be your guide. Move the arm to an “endpoint” (dictated by pain). Your goal is to increase the endpoint as often as possible until you have reached the full range of motion. As far as pain, you want to avoid excruciating pain, but “discomfort” is tolerated as long as the pain does not remain for a prolonged period of time. A basic rule, if the pain does not linger, you didn’t stretch too far.
Phase 1: 6-8 weeks after surgery
Goals:
- Protect the shoulder and avoid over stressing the replacement
- Improve range of motion of the shoulder
- Begin Strengthening exercises
Activities
- Sling—No longer necessary.
- Use of the operative arm— You may now use your arm. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight.
- Precautions—Do not lift heavy weights overhead with the weight going behind the head. Keep everything where you can see it.
- Ice— 7 days a week for 4-5 times a day as needed for 15-20 minutes. Do not place directly on the skin.
Exercise Program
Stretching/Active motion Days per week 7 Times per day 2-4
- Pendulum exercises 1-2 sets 20-30 rotations
- Supine External rotation 1 set 10-15 reps
- Standing External rotation 1 set 10-15 reps Week 6: limit to 30 degrees Week 7-8: limit 45 degrees
- Supine passive arm elevation 1 set 5-10 reps
- Standing Arm elevation 1 set 5-10 reps
- Behind the back internal rotation 1-2 sets 5-10 reps
Phase 2: 8-12 weeks after surgery
Goals:
- Protect the shoulder
- Regain full range of motion
- Continue gentle Strengthening
Activities
- Sling—No longer necessary.
- Use of the operative arm— You may now use your arm. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight.
- Precautions—Do not lift heavy weights overhead with the weight going behind the head. Keep everything where you can see it.
Exercise Program
Stretching/Active motion Days per week 7 Times per day1-2
- Pendulum exercises 1-2 sets 20-30 rotations
- Standing External rotation 1 set 10-15 reps
- Wall climb stretch 1 set 5-10 reps
- Standing Arm elevation 1 set 5-10 reps
- Behind the back internal rotation 1-2 sets 5-10 reps
- Supine External rotation with abduction 1 set 5-10 reps
- Supine Cross Chest Stretch 1 set 5-10 reps
- Side-lying external rotation 1 set 10-20 reps
- Prone Horizontal Arm raises 1 set 10-20 reps
Strengthening/Theraband Days per week 7 Times per day1-2
- External rotation 1–2 sets 15-20 reps
- Internal rotation 1-2 sets 15-20 reps
- Standing forward punch 1-2 sets 15-20 reps
- Shoulder shrug 1-2 sets 15-20 reps
- Seated row 1-2 sets 15-20 reps
- Biceps curl 1-2 sets 15-20 reps
Phase 3: 12 weeks on after surgery
Goals:
- Protect the shoulder
- Regain full range of motion
- Strengthening to return to normal activities
Activities
- Use of the operative arm— You may now use your arm. You may move the arm into all positions including external rotation and behind the back if it is comfortable. Avoid having the arm forcefully pulled behind you. Continue to avoid heavy weight.
- Precautions—Do not lift heavy weights overhead with the weight going behind the head. Keep everything where you can see it.
Exercises
- Continue previous program
- Gradually incorporate weight training, while continuing to avoid excessive or forceful extension and external rotation
Return to sport
The rates of return to sports following total shoulder arthroplasty (75%-100%) are slightly higher than those reported for hemiarthroplasty (67%-76%) and reverse total shoulder arthroplasty (75%-85%). Take a common-sense approach and think it is reasonable to perform recreational activities like tennis, golf, fishing, swimming, light weight-lifting, but I discourage ultra-high impact activities like boxing, shotgun shooting, or heavy power-lifting. Softball has been shown to be the least favorable to return to sport (20%). Most studies demonstrate, that a return to sporting activities is possible in most patients after shoulder replacement but that general health and activity level before surgery are the strongest predictors of a successful return. In other words, patients who exercise routinely before surgery commonly return to high-level sports after shoulder replacement surgery.
TSA Repair Rehabilitation Protocol
Diagnosis: Procedure date: S/P:
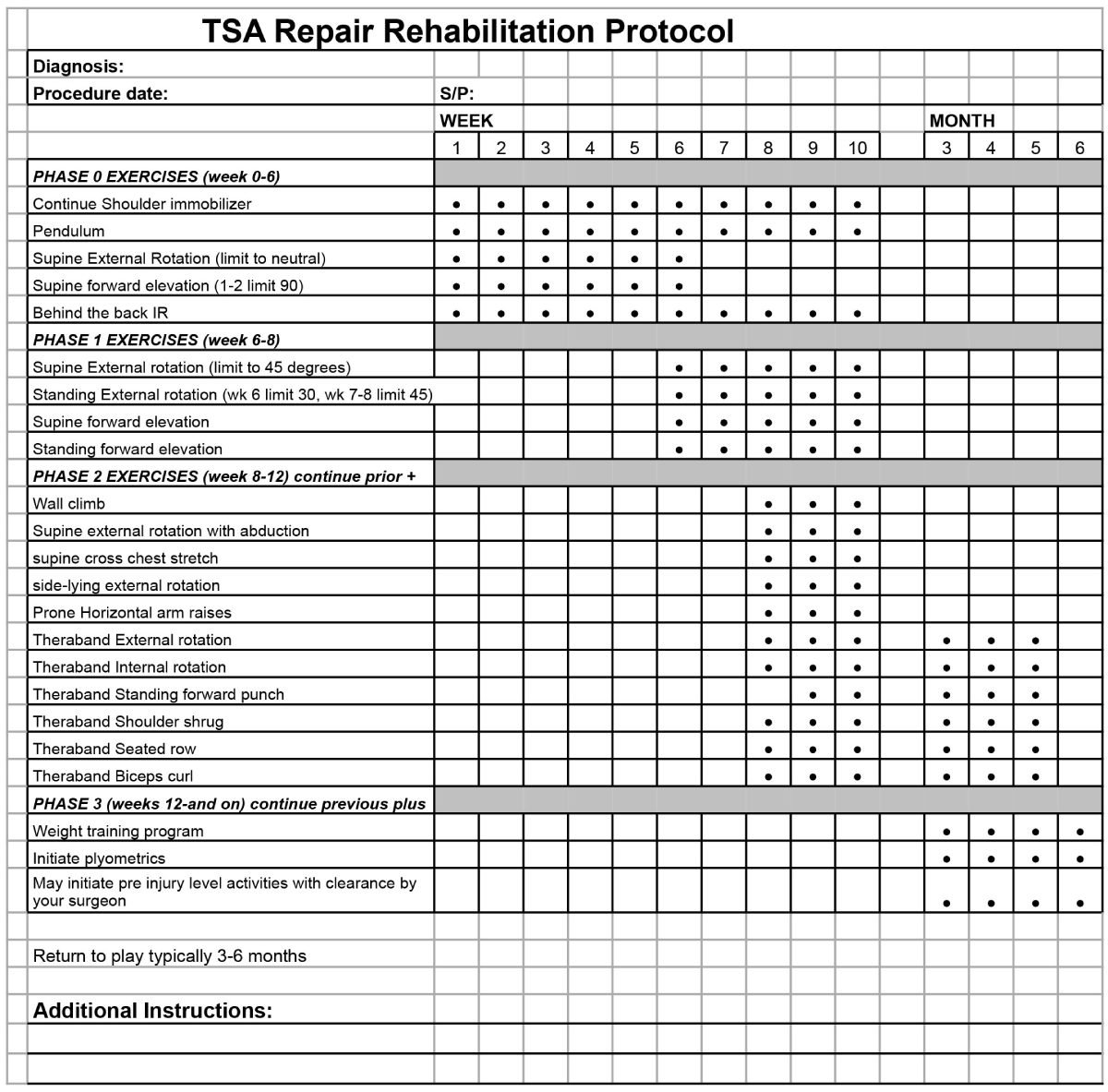
Schedule Your Consultation With Our Specialists
Schedule your next appointment quickly and conveniently with our team.

